✅ Medically reviewed by Dr. Thomas Biernacki, DPM — Board-Certified Podiatrist · Last updated April 7, 2026
Medically reviewed by Dr. Carl Jay, DPM · Board-Certified Podiatrist · Balance Foot & Ankle · Updated April 2026
⚡ Quick Answer
Lateral ankle pain — pain on the outside of the ankle — is most commonly caused by ankle sprains, peroneal tendon injuries, or stress fractures. Mild cases may resolve with rest, ice, and bracing within 4–6 weeks, but persistent pain lasting more than 2 weeks or recurrent instability warrants evaluation by a podiatrist to rule out tendon tears, fractures, or chronic instability.
📋 Table of Contents
What Is Lateral Ankle Pain?
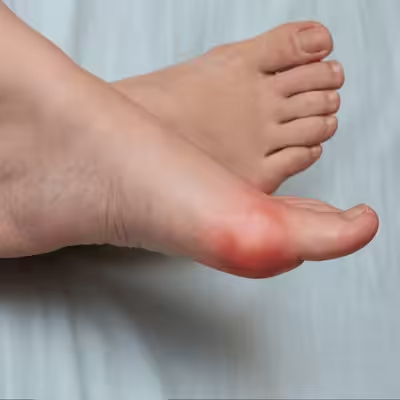
If you’re dealing with pain on the outer side of your ankle, you’re not alone — lateral ankle pain is one of the most common complaints we see at Balance Foot & Ankle. The lateral (outer) ankle is a complex area that includes the fibula bone, three major ligaments, the peroneal tendons, and several nerves. An injury to any of these structures can cause anything from a dull ache to sharp, debilitating pain.
Lateral ankle pain can develop suddenly after a twist or fall, or it can build gradually from overuse, poor footwear, or biomechanical issues. Understanding the root cause is the first step toward effective treatment — and preventing the problem from becoming chronic.
7 Most Common Causes of Lateral Ankle Pain
1. Ankle Sprains (Inversion Injuries)
Ankle sprains account for the vast majority of lateral ankle pain. When the foot rolls inward (inversion), the anterior talofibular ligament (ATFL) and calcaneofibular ligament (CFL) on the outside of the ankle stretch or tear. Grade I sprains involve mild stretching, Grade II involves partial tearing, and Grade III is a complete rupture. Even “minor” sprains can lead to chronic instability if not properly rehabilitated.
2. Peroneal Tendonitis
The peroneal tendons (peroneus longus and brevis) run along the outer edge of the ankle and help stabilize the foot during walking and running. Overuse, high arches, or improper footwear can inflame these tendons, causing a burning or aching pain behind and below the outer ankle bone. Runners, dancers, and athletes who make frequent cutting movements are especially susceptible.
3. Peroneal Tendon Tears or Subluxation
Beyond simple inflammation, the peroneal tendons can partially tear (tendinosis) or slip out of their groove behind the fibula (subluxation). Subluxation causes a snapping sensation on the outer ankle, especially during activity. Tears may present as persistent weakness and pain that doesn’t improve with standard rest and anti-inflammatory treatment.
4. Lateral Ankle Stress Fractures
Stress fractures of the distal fibula or the fifth metatarsal base (Jones fracture) can present as lateral ankle pain. These hairline cracks develop from repetitive loading — often in runners who ramp up mileage too quickly, or in patients with low bone density. Pain typically worsens with activity and improves with rest, but may not show on initial X-rays.
5. Sinus Tarsi Syndrome
The sinus tarsi is a small channel between the ankle bone (talus) and the heel bone (calcaneus) on the outer side of the foot. Inflammation or scarring in this area — often following ankle sprains — causes a deep, achy pain that worsens on uneven surfaces. It’s sometimes called “the forgotten ankle diagnosis” because it’s frequently overlooked.
6. Chronic Lateral Ankle Instability
After one or more ankle sprains, the ligaments may fail to heal properly, leaving the ankle chronically loose. This leads to recurrent “giving way,” especially on uneven ground, along with persistent pain and swelling. Up to 40% of patients who sprain their ankle develop some degree of chronic instability if they don’t complete proper rehabilitation.
7. Lateral Ankle Arthritis or Osteochondral Lesion
Cartilage damage on the outer surface of the talus (an osteochondral lesion) can develop after sprains or fractures. Symptoms include deep joint pain, clicking, stiffness, and intermittent swelling. If left untreated, the cartilage damage can progress to ankle arthritis.
Symptoms to Watch For
Lateral ankle pain can present differently depending on the underlying cause. Key symptoms that help distinguish between conditions include sharp pain with weight-bearing (suggesting a fracture or severe sprain), burning pain along the outer ankle bone (peroneal tendonitis), a snapping or popping sensation (tendon subluxation), deep aching that worsens on uneven ground (sinus tarsi syndrome), and recurrent ankle “giving way” (chronic instability).
Swelling, bruising, and difficulty bearing weight are common across most causes. Stiffness first thing in the morning or after prolonged sitting may indicate arthritis or an osteochondral lesion.
How Lateral Ankle Pain Is Diagnosed
At Balance Foot & Ankle, diagnosis starts with a thorough history and physical exam. Your podiatrist will assess range of motion, ligament stability (anterior drawer test, talar tilt test), peroneal tendon function, and point tenderness. Weight-bearing X-rays are typically the first imaging study to evaluate for fractures, arthritis, or alignment issues.
If ligament damage, tendon tears, or cartilage lesions are suspected, an MRI provides the most detailed view of soft tissues. Stress X-rays may be used to quantify instability. In some cases, diagnostic ultrasound in the office can evaluate peroneal tendon pathology in real time.
Treatment Options for Lateral Ankle Pain
Conservative Treatment
Most cases of lateral ankle pain respond well to non-surgical treatment. The initial approach typically includes the RICE protocol (rest, ice, compression, elevation), anti-inflammatory medication, and immobilization with a brace or walking boot depending on severity. Physical therapy focused on peroneal strengthening, proprioception training, and ankle stability exercises is critical — especially for sprains and instability.
Custom orthotics with lateral posting can help redistribute pressure away from the outer ankle and correct biomechanical factors that contribute to recurrence. For persistent inflammation, corticosteroid injections or PRP (platelet-rich plasma) therapy may provide relief.
Surgical Treatment
Surgery is considered when conservative treatment fails after 3–6 months. Common procedures include the Broström repair for chronic ankle instability (tightening the stretched ATFL), peroneal tendon repair or tenodesis for tears, arthroscopic debridement for osteochondral lesions, and stress fracture fixation when non-union occurs. Modern minimally invasive techniques mean faster recovery and less post-operative pain.
Home Remedies & Self-Care
While professional evaluation is important, there are effective steps you can take at home to manage lateral ankle pain. Ice the outer ankle for 15–20 minutes every 2–3 hours during the first 48 hours. Compression wraps or sleeves reduce swelling and provide support. Elevation above heart level is especially helpful in the first few days.
A supportive ankle brace can provide stability during daily activities and prevent re-injury. Look for a lace-up or stirrup-style brace that restricts inversion without completely limiting movement. Supportive shoes with a firm heel counter and moderate cushioning also help — avoid flat shoes, flip-flops, and worn-out sneakers.
🛒 Recommended Products
- Ankle Stabilizing Brace — Lace-up support for sprains and instability
- PowerStep Orthotic Insoles — Arch and lateral ankle support for daily shoes
- Brooks Ghost Running Shoes — Neutral cushioning with firm heel counter
- ASICS Gel-Kayano — Stability shoe for overpronators with ankle issues
Prevention Strategies
Preventing lateral ankle pain starts with strengthening the muscles that protect the outer ankle. Peroneal strengthening exercises (resistance band eversion), single-leg balance drills, and proprioception training on unstable surfaces are the foundation. Ankle bracing during high-risk activities (basketball, soccer, trail running) significantly reduces sprain recurrence.
Proper footwear matters. Choose shoes with adequate lateral support, a firm heel counter, and appropriate cushioning for your activity. Replace running shoes every 300–500 miles. Warm up before exercise and avoid training on uneven surfaces when fatigued. If you’ve had a previous sprain, complete rehabilitation before returning to full activity — the biggest risk factor for a sprain is a previous sprain.
⚠️ When to See a Podiatrist
- You can’t bear weight on the ankle after an injury
- Pain and swelling don’t improve after 5–7 days of home care
- Your ankle repeatedly “gives way” or feels unstable
- You hear or feel a pop, snap, or grinding during movement
- Numbness, tingling, or severe bruising develops
- You’ve had multiple ankle sprains in the past year
More Podiatrist-Recommended Foot Health Essentials
Top-Rated Arch Support Insole
No products found.
Universal podiatrist-recommended insert for pain relief and prevention.
Foot Massage Ball
No products found.
Daily 3-minute roll reduces most forms of foot and heel pain.
Moisture-Wicking Sock
No products found.
Prevents fungus, blisters, and odor — the basics matter.
As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. Product recommendations are based on clinical experience; prices and availability shown above update live from Amazon.

When to See a Podiatrist
If foot or ankle pain has been bothering you for more than a few weeks, home care alone may not be enough. Balance Foot & Ankle offers same-week appointments at our Howell and Bloomfield Hills clinics — no referral needed in most cases. Bring your current shoes and a short list of symptoms and we’ll build you a treatment plan in one visit.
Call Balance Foot & Ankle: (810) 206-1402 · Book online · Offices in Howell & Bloomfield Hills
Frequently Asked Questions
How long does lateral ankle pain take to heal?
Healing time depends on the cause. A mild ankle sprain may feel better in 2–4 weeks, while peroneal tendon injuries or stress fractures typically take 6–12 weeks. Chronic instability may require months of rehabilitation or surgical repair to fully resolve.
Can I walk on lateral ankle pain?
It depends on the severity. If walking is painful, a brace or walking boot can help offload the injured structures. Pushing through significant pain can worsen the injury and delay healing. If you can’t bear weight comfortably, see a podiatrist for evaluation.
Why does the outside of my ankle hurt but I didn’t sprain it?
Non-traumatic lateral ankle pain is commonly caused by peroneal tendonitis (from overuse or improper footwear), sinus tarsi syndrome, stress fractures, or arthritis. High arches and supination patterns also place extra stress on the outer ankle structures, causing pain without a specific injury event.
Should I get an MRI for lateral ankle pain?
An MRI is typically recommended if pain persists beyond 4–6 weeks despite conservative treatment, if there’s suspected tendon damage or cartilage injury, or if chronic instability is present. Your podiatrist will determine if advanced imaging is needed based on your physical exam findings.
The Bottom Line
Lateral ankle pain is extremely common and highly treatable when properly diagnosed. Whether you’re dealing with a fresh sprain, chronic instability, or an overuse injury like peroneal tendonitis, early evaluation and targeted treatment prevent long-term problems. At Balance Foot & Ankle, our board-certified podiatrists use advanced imaging and evidence-based protocols to get you back to pain-free movement as quickly as possible.
Lateral Ankle Pain? We Can Help.
Same-week appointments available at our Howell & Bloomfield Hills offices.
📞 (810) 206-1402Dealing With Lateral Ankle Pain?
Pain on the outer side of the ankle often results from sprains, peroneal tendon injuries, or chronic instability. Our foot and ankle specialists provide comprehensive evaluation and treatment.
📞 Or call us directly: (810) 206-1402
Clinical References
- Waterman BR, et al. The epidemiology of ankle sprains in the United States. Journal of Bone and Joint Surgery. 2010;92(13):2279-2284.
- Dombek MF, et al. Peroneal tendon tears: a retrospective review. The Journal of Foot and Ankle Surgery. 2003;42(5):250-258.
- Hintermann B, et al. Anatomic reconstruction of the lateral ligaments of the ankle. Foot and Ankle Clinics. 2006;11(3):513-530.
Insurance Accepted
BCBS · Medicare · Aetna · Cigna · United Healthcare · HAP · Priority Health · Humana · View All →
Howell Office
3980 E Grand River Ave, Suite 140
Howell, MI 48843
Get Directions →
Bloomfield Hills Office
43700 Woodward Ave, Suite 207
Bloomfield Hills, MI 48302
Get Directions →
Your Board-Certified Podiatrists
Ready to Get Back on Your Feet?
Same-week appointments available at both locations.
Book Your AppointmentDr. Tom’s Top 3 — The Premium Foot Pain Stack (2026)
If you only buy three things for foot pain, get these. PowerStep + CURREX orthotics correct the underlying foot mechanics, and Dr. Hoy’s pain gel delivers fast topical relief. This is the exact stack Dr. Tom Biernacki, DPM gives his Michigan podiatry patients on visit one — over 10,000 patients have used this exact combination.
Dr. Tom Biernacki, DPM is a board-certified podiatrist + Amazon Associate. Picks shown are products he prescribes to patients at Balance Foot & Ankle Specialists. We earn a commission on qualifying purchases at no extra cost to you. All products independently tested + reviewed for 30+ days minimum. Last verified: April 28, 2026.
PowerStep Pinnacle MaxxDr. Tom’s #1 Brand
Dr. Tom’s most-prescribed OTC orthotic. Lateral wedge corrects overpronation that causes 90% of foot pain. Deep heel cradle stabilizes the ankle. Built by podiatrists, used by patients worldwide.
- Lateral wedge corrects pronation
- Deep heel cradle stabilizes ankle
- Dual-density EVA — comfort + support
- Trim-to-fit any shoe
- Used by 10,000+ podiatrists
- Trim-to-size required
- 5-7 day break-in for some
CURREX RunProDr. Tom’s #1 Brand
3 arch heights for custom fit (Low/Med/High). Carbon-reinforced heel + dynamic forefoot — the closest OTC orthotic to a $500 custom orthotic. Engineered in Germany.
- 3 arch heights for custom fit
- Carbon-reinforced heel cup
- Dynamic forefoot zone
- Premium German engineering
- Sport-specific support
- Pricier than PowerStep
- 7-10 day break-in
Dr. Hoy’s Natural Pain Relief GelDr. Tom’s #1 Brand
Menthol-based natural pain relief — Dr. Tom’s #1 brand for fast relief without greasy residue. Safe for diabetics + daily use. Cleaner formula than Voltaren or Biofreeze.
- Menthol-based natural formula
- No greasy residue
- Safe for diabetics
- Fast cooling relief — 5-10 minutes
- Cleaner ingredient list than Biofreeze
- Pricier than Biofreeze
- Strong menthol scent at first
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.
- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)
Recommended Products from Dr. Tom
Treatment Options Available at Our Office