✅ Medically Reviewed by Dr. Tom Biernacki, DPM
Board-certified podiatric physician & surgeon | Balance Foot & Ankle | Updated April 2026
⚡ Quick Answer: What Is Peroneus Longus Tendonitis?
Peroneus longus tendonitis is inflammation of the tendon running along the outer ankle, causing lateral pain that worsens with activity. Common in runners and athletes. Treatment: rest, ice, NSAIDs, ankle bracing, physical therapy, and custom orthotics. A podiatrist can confirm with ultrasound and rule out a tendon tear.
✅ Medically reviewed by Dr. Thomas Biernacki, DPM — Board-Certified Podiatrist · Last updated April 7, 2026

Medically reviewed by Dr. Carl Jay, DPM
Board-Certified Podiatric Surgeon · Balance Foot & Ankle
Last reviewed: April 2026
Quick Answer: What Is Peroneus Longus Tendonitis?
Peroneus longus tendonitis is inflammation of the peroneus (fibularis) longus tendon — the longer of the two peroneal tendons that runs along the outer ankle, under the foot, and attaches to the base of the first metatarsal. It causes pain on the outside of the ankle and lateral foot, worsening with activity, walking on uneven surfaces, and push-off. Treatment starts with ankle bracing, supportive shoes, and targeted strengthening — most cases resolve in 4–8 weeks with proper conservative care.
Table of Contents
- Peroneus Longus Anatomy — Why This Tendon Matters
- Peroneus Longus vs. Peroneus Brevis
- What Causes Peroneus Longus Tendonitis?
- Symptoms — How to Recognize It
- How We Diagnose It
- Home Treatment Protocol
- Best Products for Peroneal Tendonitis
- Rehabilitation Exercises
- Professional Treatment Options
- Warning Signs — When to See a Podiatrist
- Frequently Asked Questions
- The Bottom Line
Every time you push off your foot or walk on uneven ground, a dull ache flares along the outer side of your ankle. Maybe it started after a long hike, a trail run, or an ankle sprain that never quite healed. The pain runs behind the outer ankle bone and may extend underneath the foot. It’s not the classic “rolled ankle” pain — it’s deeper, more persistent, and gets worse with activity.
Peroneal tendonitis is one of the most common causes of chronic outer ankle pain — and the peroneus longus is frequently the culprit because of its unique course under the foot. At Balance Foot & Ankle, we see this condition regularly in runners, hikers, and patients recovering from lateral ankle sprains. Here’s everything you need to know about diagnosis and treatment.
Peroneus Longus Anatomy — Why This Tendon Matters
The peroneus longus (also called fibularis longus) is one of two peroneal muscles in the outer lower leg. It originates from the upper fibula bone, runs down the lateral leg, passes behind the outer ankle bone (lateral malleolus), then takes a unique path: it courses under the foot through a groove in the cuboid bone and crosses the entire sole to attach at the base of the first metatarsal and medial cuneiform on the inner side of the foot.
This cross-foot path gives the peroneus longus two critical functions: it everts the foot (turns the sole outward) for ankle stability, and it plantarflexes the first ray (pushes the big toe side of the foot down), which stabilizes the medial arch during push-off. Without a functioning peroneus longus, the arch collapses at push-off and the ankle becomes laterally unstable.
The tendon is vulnerable at several points: behind the lateral malleolus (where it passes through a tight fibrous tunnel), at the peroneal tubercle of the calcaneus (where longus and brevis separate), and at the cuboid groove (where it makes a sharp turn under the foot). Inflammation can develop at any of these friction points.
Peroneus Longus vs. Peroneus Brevis — Key Differences
| Feature | Peroneus Longus | Peroneus Brevis |
|---|---|---|
| Course | Behind ankle → under the foot → inner foot | Behind ankle → outer side of foot (5th metatarsal base) |
| Primary function | Stabilizes arch during push-off; everts foot | Everts foot; primary lateral ankle stabilizer |
| Pain location | Behind outer ankle AND under the foot | Behind outer ankle AND at 5th metatarsal base |
| Injury pattern | Overuse; cuboid groove friction; chronic tendinosis | More prone to tears and subluxation |
| Unique test | Pain with resisted first ray plantarflexion | Pain with resisted eversion at midfoot |
What Causes Peroneus Longus Tendonitis?
Overuse and repetitive stress: Running (especially on uneven terrain or cambered roads), hiking, and sports involving lateral movements (basketball, tennis, soccer) repeatedly load the peroneal tendons. Training errors — too much mileage increase, inadequate rest — are the most common trigger.
Prior ankle sprains: Lateral ankle sprains stretch the peroneal tendons and can leave subtle instability that chronically overloads the peroneals as they work harder to stabilize the ankle. Studies show that up to 40% of patients with chronic lateral ankle instability develop secondary peroneal tendonitis.
High-arched (cavus) foot: A high arch increases the inversion moment of the foot, forcing the peroneals to work harder to prevent the ankle from rolling outward. People with cavovarus foot posture have significantly higher rates of peroneal tendon pathology.
Improper footwear: Shoes without adequate lateral support, worn-out shoes with broken-down midsoles, and shoes that allow excessive ankle movement all increase peroneal tendon loading.
Os peroneum (accessory bone): Approximately 20% of people have an accessory bone (os peroneum) within the peroneus longus tendon near the cuboid. This bone can fracture, dislocate, or create a friction point that leads to tendinitis.
Symptoms — How to Recognize Peroneus Longus Tendonitis
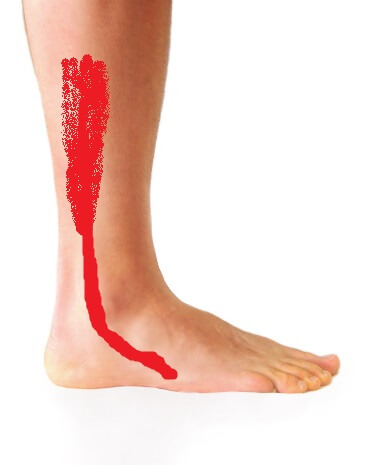
Pain behind and below the outer ankle bone that worsens with walking, running, or standing on tiptoes. The pain may radiate along the outside of the foot or under the foot toward the arch. It’s typically worse when walking on uneven surfaces, during lateral movements, and during push-off.
Swelling and warmth along the peroneal tendon course behind the lateral malleolus. You may be able to feel the tendon as a thick, tender cord when you palpate behind the ankle bone.
Weakness with eversion: Turning the sole of your foot outward against resistance feels weak and painful. This is the diagnostic test we use in our clinic — resisted eversion reproduces the peroneal tendon pain.
Ankle instability or “giving way”: The peroneals are the primary dynamic stabilizers of the lateral ankle. When they’re inflamed and weakened, the ankle may feel unstable — especially on uneven ground or when walking on slopes.
How We Diagnose It
Physical examination: We palpate the peroneal tendons along their entire course — behind the lateral malleolus, at the peroneal tubercle, and under the foot. We test resisted eversion and resisted first ray plantarflexion. We assess ankle stability with anterior drawer and talar tilt tests. We examine foot posture (cavus vs. planus).
X-rays: Weight-bearing X-rays evaluate ankle alignment, check for an os peroneum (accessory bone), and rule out fractures. A calcified or fractured os peroneum is a specific finding that changes the treatment approach.
MRI or ultrasound: For persistent cases, MRI shows the tendon detail — thickening, partial tears, tendinosis (chronic degeneration), or fluid around the tendon (tenosynovitis). Ultrasound can be performed dynamically, showing the tendon sliding in real-time and detecting subluxation that MRI may miss.
Home Treatment Protocol
Most peroneus longus tendonitis responds well to conservative treatment. Here’s the protocol we use at Balance Foot & Ankle:
Phase 1 (Weeks 1–2): Relative rest and protection. Reduce activity that aggravates symptoms. Wear a lace-up ankle brace to support the lateral ankle and reduce peroneal tendon demand. Ice for 15 minutes after activity. NSAIDs (ibuprofen 400mg 3x daily with food) for 7–10 days to reduce inflammation. Switch to supportive shoes with good lateral stability.
Phase 2 (Weeks 2–4): Gentle strengthening begins. Start peroneal strengthening exercises (see below) at a pain-free intensity. Continue ankle brace use during activity. Begin single-leg balance exercises on flat ground. Avoid uneven terrain and lateral sports.
Phase 3 (Weeks 4–8): Progressive loading. Gradually increase activity intensity. Progress balance exercises to unstable surfaces (wobble board, BOSU ball). Begin sport-specific movements. The ankle brace can be weaned when strength and balance are restored — typically 6–8 weeks.
Best Products for Peroneal Tendonitis
🏆 #1 Pick: ASICS Gel-Kayano (Lateral Stability)
Best for: Daily shoe providing maximum lateral ankle support
Why we recommend it: Peroneal tendonitis requires shoes with excellent lateral stability to reduce the tendon’s workload as an ankle stabilizer. The ASICS Gel-Kayano has structured medial and lateral support, a firm heel counter, and a wide base that prevents excessive ankle motion. The GEL cushioning absorbs landing forces. For patients with peroneal tendonitis from ankle instability, this shoe provides external support that lets the tendon heal while you stay active.
PowerStep Orthotic Insoles
Best for: Arch support to reduce peroneal tendon overload
Why we recommend it: In patients with high arches (cavus foot), the peroneals are chronically overloaded because the foot tends to roll outward. PowerStep insoles with structured arch support help control this inversion tendency, reducing the demand on the peroneal tendons. They also provide a stable platform that complements the ankle brace and supportive shoe.
Brooks Ghost
Best for: Neutral daily shoe with reliable lateral support
Why we recommend it: For patients who don’t need the aggressive stability features of the Kayano, the Brooks Ghost provides a well-balanced combination of cushioning, lateral support, and comfort. The wide platform and secure heel counter support the lateral ankle without feeling restrictive. A versatile everyday option during peroneal tendonitis recovery.
Disclosure: Some links above are affiliate links. We only recommend products we use in our practice or have vetted for our patients. Affiliate commissions help support our free educational content. Your price is not affected.
Rehabilitation Exercises
Resistance band eversion: Sit with legs extended. Loop a resistance band around the ball of the affected foot, anchored to a table leg on the inner side. Turn the sole of your foot outward against the band’s resistance. Hold 3 seconds, slowly return. 3 sets of 15 repetitions. This is the primary peroneal strengthening exercise.
Single-leg balance: Stand on the affected foot with eyes open, holding for 30 seconds. Progress to eyes closed, then to standing on an unstable surface (pillow, foam pad, wobble board). This trains the proprioceptive reflex loop that the peroneals are part of — ankle stability depends on this system. 3 sets of 30 seconds, twice daily.
Heel raises with eversion bias: Stand on a step with the ball of your foot on the edge. Rise onto your toes, then slowly lower. At the top of the raise, subtly roll to the outside of the foot (eversion) to load the peroneus longus through its full range. 3 sets of 12 repetitions.
Lateral step-downs: Stand on a step on the affected leg. Slowly lower the opposite foot to the ground by bending the standing knee and controlling the lateral ankle position. This functional exercise trains the peroneals in a weight-bearing, real-world context. 3 sets of 10, twice daily.
Professional Treatment Options
Physical therapy: For cases that don’t respond to home exercises, formal PT provides manual therapy (soft tissue mobilization, instrument-assisted techniques), supervised progressive loading, and sport-specific rehabilitation. A therapist can also identify biomechanical contributors that home exercises can’t address.
Custom orthotics with lateral wedge: For patients with cavus (high-arch) foot posture driving the peroneal overload, custom orthotics with a lateral forefoot wedge reduce the inversion moment of the foot, decreasing peroneal demand. This is a long-term biomechanical solution for recurrent peroneal tendonitis.
PRP injection: Platelet-rich plasma injected around the peroneal tendon provides concentrated growth factors that promote healing in chronic tendinosis. We consider PRP for patients with 3+ months of symptoms who haven’t responded to bracing, exercises, and physical therapy.
Surgery: Reserved for tears, chronic subluxation (tendon popping out of the groove), or os peroneum pathology. Surgical options include tendon debridement, repair, groove deepening (for subluxation), and os peroneum excision. Success rates for peroneal tendon surgery are 85–90%.
Warning Signs — When to See a Podiatrist
⚠️ See a Podiatrist If:
- You feel a snapping or popping sensation behind the ankle bone — this suggests peroneal tendon subluxation (the tendon is slipping out of its groove), which may require surgical stabilization.
- Outer ankle pain hasn’t improved after 4–6 weeks of bracing and home exercises — persistent symptoms may indicate a partial tendon tear or chronic tendinosis requiring imaging.
- Sudden sharp pain followed by weakness in pushing off or turning the foot — acute peroneal tendon rupture needs urgent evaluation.
- Recurrent ankle sprains with ongoing outer ankle pain — chronic lateral ankle instability commonly coexists with peroneal pathology and both need to be addressed.
- Swelling behind the ankle that worsens or doesn’t resolve — persistent tenosynovitis may indicate an underlying tear or structural issue.
More Podiatrist-Recommended Foot Health Essentials
Hoka Clifton 10
Max-cushion everyday shoe — podiatrist favorite for walking and running.
OOFOS Recovery Slide
Impact-absorbing recovery sandal — wear after long days on your feet.
As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. Product recommendations are based on clinical experience; prices and availability shown above update live from Amazon.
When to See a Podiatrist
If foot or ankle pain has been bothering you for more than a few weeks, home care alone may not be enough. Balance Foot & Ankle offers same-week appointments at our Howell and Bloomfield Hills clinics — no referral needed in most cases. Bring your current shoes and a short list of symptoms and we’ll build you a treatment plan in one visit.
Call Balance Foot & Ankle: (810) 206-1402 · Book online · Offices in Howell & Bloomfield Hills
Frequently Asked Questions
How long does peroneal tendonitis take to heal?
Mild cases resolve in 2–4 weeks with rest, bracing, and supportive shoes. Moderate cases take 4–8 weeks with structured rehabilitation. Chronic cases with tendinosis may take 3–6 months of progressive loading to fully resolve. The key factor is whether you address the underlying cause (ankle instability, foot posture, training error) — without correcting the root cause, symptoms tend to recur.
Can I run with peroneal tendonitis?
Not during the acute phase (first 2–4 weeks). Running loads the peroneals heavily, especially on uneven terrain. Once pain subsides with daily activities, you can begin a graduated return-to-running program: walk → walk-jog → continuous jog → running, progressing only if pain-free. Wear supportive shoes and avoid trails until fully recovered. Cross-train with cycling or swimming during the rest period.
What’s the difference between peroneal tendonitis and a lateral ankle sprain?
A lateral ankle sprain damages the ligaments on the outside of the ankle (ATFL, CFL). Peroneal tendonitis is inflammation of the tendons on the outside of the ankle. They often coexist — an ankle sprain can trigger peroneal tendonitis as the tendons compensate for damaged ligaments. The key difference: ligament injuries feel unstable and are tender over the ligaments (in front of and below the ankle bone); peroneal tendonitis is tender behind and above the ankle bone along the tendon course.
The Bottom Line
Peroneus longus tendonitis causes pain along the outer ankle and under the foot, typically from overuse, prior ankle sprains, or high-arched foot posture. It responds well to conservative treatment — ankle bracing, supportive shoes, and progressive peroneal strengthening exercises resolve most cases within 4–8 weeks. If you notice snapping behind the ankle, symptoms lasting beyond 6 weeks, or weakness with push-off, professional evaluation ensures you don’t have a tendon tear or subluxation that needs targeted treatment.
Sources
- Heckman DS, Reddy S, Pedowitz D, et al. “Operative treatment for peroneal tendon disorders.” J Bone Joint Surg Am. 2008;90(2):404-418.
- Dombek MF, Lamm BM, Saltrick K, et al. “Peroneal tendon tears: a retrospective review.” J Foot Ankle Surg. 2003;42(5):250-258.
- Redfern D, Myerson M. “The management of concomitant tears of the peroneus longus and brevis tendons.” Foot Ankle Int. 2004;25(10):695-707.
- van Dijk PA, Lubberts B, Verheul C, et al. “Rehabilitation after surgical treatment of peroneal tendon tears and instability.” Knee Surg Sports Traumatol Arthrosc. 2016;24(4):1165-1174.
Outer Ankle Pain That Won’t Quit? We Can Help.
Board-certified podiatrists · In-office ultrasound · Howell & Bloomfield Hills, MI
⭐ 4.9 Stars · 1,123 Reviews · 3,000+ Surgeries
Dealing With Peroneus Longus Tendonitis?
Peroneus longus tendonitis causes pain along the outer ankle and under the foot. Our podiatrists provide targeted treatment to heal the tendon and restore normal function.
📞 Or call us directly: (810) 206-1402
Clinical References
- Petersen W, Bobka T, Stein V, Tillmann B. Blood supply of the peroneal tendons. Injection and immunohistochemical studies of cadaver tendons. Acta Orthopaedica Scandinavica. 2000;71(2):168-174.
- Davda K, Malhotra K, O’Donnell P, et al. Peroneal tendon disorders. EFORT Open Reviews. 2017;2(6):281-292.
- van Dijk PAD, Kerkhoffs GM, Chiodo C, DiGiovanni CW. Chronic disorders of the peroneal tendons: current concepts review of the literature. Journal of the American Academy of Orthopaedic Surgeons. 2019;27(16):590-598.
Insurance Accepted
BCBS · Medicare · Aetna · Cigna · United Healthcare · HAP · Priority Health · Humana · View All →
👟 Dr. Tom Also Recommends
Podiatrist Recommended Shoes 2026: Dr. Tom’s Top Picks for Every Condition
The right footwear can make or break your recovery. Dr. Tom’s complete guide to the best shoes for plantar fasciitis, flat feet, neuropathy, bunions & more — with clinical picks for every foot type.
See Dr. Tom’s Top Shoe Picks →Howell Office
3980 E Grand River Ave, Suite 140
Howell, MI 48843
Get Directions →
Bloomfield Hills Office
43700 Woodward Ave, Suite 207
Bloomfield Hills, MI 48302
Get Directions →
Your Board-Certified Podiatrists
Ready to Get Back on Your Feet?
Same-week appointments available at both locations.
Book Your AppointmentDr. Hoy’s Complete Pain Relief Line — Dr. Tom’s Picks (2026)
Dr. Hoy’s Natural Pain Relief is Dr. Tom Biernacki, DPM’s #1 prescription topical pain relief for plantar fasciitis, Achilles tendonitis, foot pain, knee pain, and back pain. Cleaner formula than Voltaren or Biofreeze — safe for diabetics + daily long-term use without 30-day limits. Below is the complete Dr. Hoy’s product line, organized by use case.
Dr. Hoy’s Natural Pain Relief Gel (4oz Tube)Dr. Tom’s #1 Brand
The flagship Dr. Hoy’s — menthol-based natural pain relief gel. The bottle Dr. Tom hands every plantar fasciitis patient on visit one. Cleaner formula than Voltaren or Biofreeze.
- Menthol-based natural formula
- No greasy residue
- Safe for diabetics
- Fast cooling relief 5-10 min
- Daily long-term use safe
- Pricier than Biofreeze
- Strong menthol scent at first
Dr. Hoy’s Natural Pain Relief Gel (8oz Pump Bottle)Dr. Tom’s #1 Brand
8oz pump bottle — same formula as the 4oz tube but 2x the value. Best for athletes, families, or chronic pain patients who use it daily.
- 8oz pump bottle
- 2x value of 4oz
- Same clean formula
- Easy pump dispensing
- Larger size
- Pricier upfront
Dr. Hoy’s Arnica Boost Pain ReliefDr. Tom’s #1 Brand
Dr. Hoy’s + arnica boost — for bruising, swelling, post-injury inflammation. Adds arnica’s anti-inflammatory power to the standard menthol formula.
- Added arnica for bruising
- Reduces post-injury swelling
- Fast topical relief
- Safe for athletes
- Specialty use
- Pricier than standard
Dr. Hoy’s Natural Pain Relief Roll-OnDr. Tom’s #1 Brand
Same Dr. Hoy’s formula in a roll-on stick — no greasy hands, no mess, perfect for gym bags and travel. TSA-friendly.
- No greasy hands
- TSA-friendly
- Travel-sized
- Same Dr. Hoy’s formula
- Less product per use
- Pricier per oz
Dr. Hoy’s Pain Relief Gel — 3-Pack BundleDr. Tom’s #1 Brand
3-pack of Dr. Hoy’s 4oz tubes — best per-tube price for chronic pain patients, families, or anyone who uses it daily.
- 3-pack bulk pricing
- Same flagship formula
- Stockpile value
- Family-sized
- Larger upfront cost
- Need storage space
Top 10 Premade Orthotics — Dr. Tom’s Picks (2026)
Dr. Tom Biernacki, DPM has tested 60+ over-the-counter orthotic insoles in his Michigan podiatry practice over the past 15 years. Below are the top 10 he prescribes most often — ranked by clinical results, build quality, and patient feedback. PowerStep + CURREX brands are Dr. Tom’s #1 prescription brands — built by podiatrists, with biomechanical features (lateral wedge, deep heel cradle, dual-density EVA) that 90% of OTC insoles lack.
Dr. Tom Biernacki, DPM is a board-certified podiatrist + Amazon Associate. Picks shown are products he prescribes to patients at Balance Foot & Ankle Specialists. We earn a commission on qualifying purchases at no extra cost to you. All products independently tested + reviewed. Last verified: April 28, 2026.
PowerStep Pinnacle MaxxDr. Tom’s #1 Brand
The most prescribed OTC orthotic in podiatry. Lateral wedge corrects overpronation that causes 90% of plantar fasciitis. Deep heel cradle stabilizes the ankle.
- Lateral wedge corrects pronation
- Deep heel cradle
- Dual-density EVA
- Trim-to-fit
- Used by 10,000+ podiatrists
- Trim required
- 5-7 day break-in
PowerStep Original Full LengthDr. Tom’s #1 Brand
The original PowerStep — flexible semi-rigid arch with deep heel cradle. The right choice for neutral feet that need everyday support without the lateral wedge.
- Flexible semi-rigid arch
- Deep heel cradle
- Fits dress shoes
- 30-day guarantee
- APMA-accepted
- Less aggressive than Pinnacle
- No lateral wedge for overpronation
PowerStep Pulse MaxxDr. Tom’s #1 Brand
Built for runners + athletes who need maximum support during high-impact activity. Engineered for forefoot strike + lateral motion.
- Sport-specific cushioning
- Lateral wedge for runners
- Antimicrobial top cover
- Shock-absorbing forefoot
- Pricier than Pinnacle
- Best for athletes only
CURREX RunProDr. Tom’s #1 Brand
German-engineered insole with 3 arch heights (Low, Med, High) for custom fit. Carbon-reinforced heel + dynamic forefoot.
- 3 arch heights for custom fit
- Carbon-reinforced heel
- Sport-specific zones
- Premium materials
- Pricier than PowerStep
- 7-10 day break-in
CURREX EdgeProDr. Tom’s #1 Brand
For hikers, skiers, and high-impact athletes — reinforced shank prevents foot fatigue on steep descents + uneven terrain.
- Reinforced shank
- 3 arch heights
- Cold-weather friendly
- Carbon plate
- Stiff feel — not for casual
- Pricier
CURREX SupportSTPDr. Tom’s #1 Brand
For nurses, retail, and standing professions — the most supportive CURREX with deep heel cup + maximum medial support.
- Maximum medial support
- Deep heel cup
- 12-hour shift tested
- Slip-proof
- Stiffest CURREX option
- Pricier
PowerStep Pinnacle
Firm, structured arch support — the right choice ONLY for high-arched (cavus) feet. Wrong choice for flat feet.
- Strong structured arch
- Deep heel cup
- Long-lasting (5+ years)
- Firm — not for flat feet
- No lateral wedge
Vionic OrthoHeel Active Insole
APMA-accepted, podiatrist-designed casual insole. Best for adding mild arch support to dress shoes + walking shoes.
- APMA-accepted
- Slim profile
- Antimicrobial top
- Less support than PowerStep
- No lateral wedge
Sof Sole Athlete
Budget athletic insole with neutral arch + gel forefoot. Decent value if you need a quick replacement.
- Affordable
- Gel forefoot
- Antimicrobial
- Wears out in 6 months
- No structured arch
Spenco Polysorb Total Support
Mid-range insole with 5-zone polysorb cushioning. Decent support for standing professions.
- 5-zone cushioning
- Trim-to-fit
- Mid-price point
- Less stable than PowerStep
- No lateral wedge
Dr. Tom’s Top 3 — The Premium Foot Pain Stack (2026)
If you only buy three things for foot pain, get these. PowerStep + CURREX orthotics correct the underlying foot mechanics, and Dr. Hoy’s pain gel delivers fast topical relief. This is the exact stack Dr. Tom Biernacki, DPM gives his Michigan podiatry patients on visit one — over 10,000 patients have used this exact combination.
Dr. Tom Biernacki, DPM is a board-certified podiatrist + Amazon Associate. Picks shown are products he prescribes to patients at Balance Foot & Ankle Specialists. We earn a commission on qualifying purchases at no extra cost to you. All products independently tested + reviewed for 30+ days minimum. Last verified: April 28, 2026.
PowerStep Pinnacle MaxxDr. Tom’s #1 Brand
Dr. Tom’s most-prescribed OTC orthotic. Lateral wedge corrects overpronation that causes 90% of foot pain. Deep heel cradle stabilizes the ankle. Built by podiatrists, used by patients worldwide.
- Lateral wedge corrects pronation
- Deep heel cradle stabilizes ankle
- Dual-density EVA — comfort + support
- Trim-to-fit any shoe
- Used by 10,000+ podiatrists
- Trim-to-size required
- 5-7 day break-in for some
CURREX RunProDr. Tom’s #1 Brand
3 arch heights for custom fit (Low/Med/High). Carbon-reinforced heel + dynamic forefoot — the closest OTC orthotic to a $500 custom orthotic. Engineered in Germany.
- 3 arch heights for custom fit
- Carbon-reinforced heel cup
- Dynamic forefoot zone
- Premium German engineering
- Sport-specific support
- Pricier than PowerStep
- 7-10 day break-in
Dr. Hoy’s Natural Pain Relief GelDr. Tom’s #1 Brand
Menthol-based natural pain relief — Dr. Tom’s #1 brand for fast relief without greasy residue. Safe for diabetics + daily use. Cleaner formula than Voltaren or Biofreeze.
- Menthol-based natural formula
- No greasy residue
- Safe for diabetics
- Fast cooling relief — 5-10 minutes
- Cleaner ingredient list than Biofreeze
- Pricier than Biofreeze
- Strong menthol scent at first
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.
- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)
Recommended Products from Dr. Tom
Treatment Options Available at Our Office

![Flexor Hallucis Longus PAIN [FHL Tendonitis BEST Treatment!]](https://www.michiganfootdoctors.com/wp-content/cache/flying-press/f76e796729e23971056c8809b96b8803.jpg)