Quick answer: Frostbite Feet Toes Cold Injury Michigan Podiatrist is a common foot/ankle topic that affects many patients. The 2026 evidence-based approach combines proper diagnosis, conservative-first treatment, and escalation only when needed. We treat this regularly at our Howell and Bloomfield Township practices. Call (810) 206-1402.
Foot pain isn't resolving?
Same-week appointments at Howell & Bloomfield Hills
Medically Reviewed | Dr. Tom Biernacki, DPM | Board-Certified Podiatric Surgeon | Balance Foot & Ankle, Michigan
Quick Answer:
Quick Answer: Frostbite is a freezing thermal injury to peripheral tissue—most commonly affecting toes, feet, fingers, ears, and nose. It is classified by depth: frostnip (superficial, no ice crystal formation, fully reversible), superficial frostbite (partial thickness, ice crystal formation in epidermis/dermis, blisters with rewarming), and deep frostbite (full thickness, ice crystal formation extending into subcutaneous tissue, muscle, or bone—associated with hemorrhagic blisters, necrosis, and potential amputation). Michigan winters create significant frostbite risk, particularly for homeless individuals, outdoor workers, and winter sports enthusiasts. Acute management centers on rapid rewarming in warm water (37–39°C), ibuprofen for thromboxane inhibition, wound care, and tetanus prophylaxis. Modern advances include thrombolytic therapy (tPA) for severe frostbite within 24 hours of injury. Dr. Biernacki provides both acute assessment and long-term sequelae management including neuropathic pain, hyperhidrosis, and Raynaud’s phenomenon following frostbite.
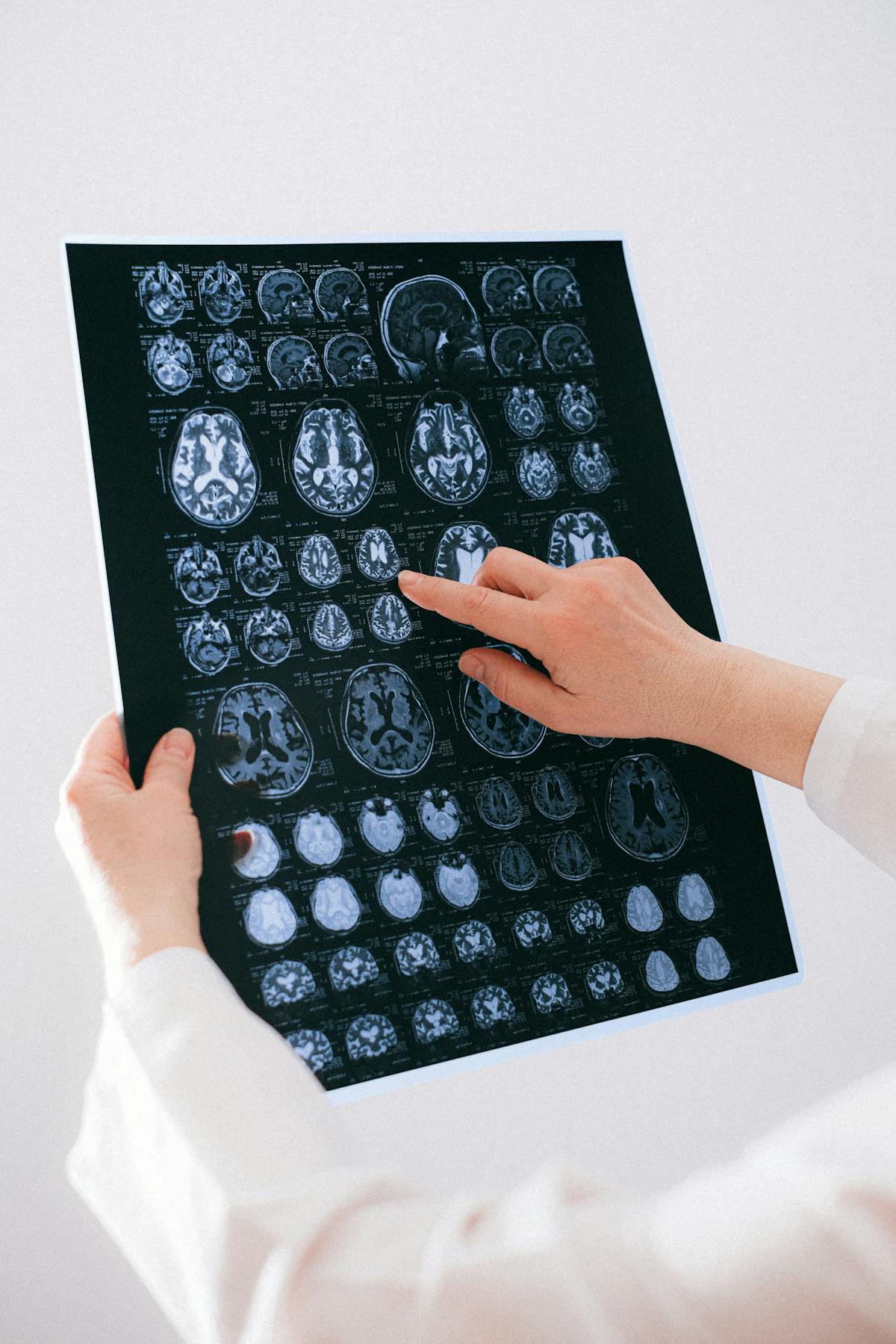
Michigan winters are serious—temperatures drop well below freezing, wind chills push conditions to dangerous extremes, and frostbite injuries to feet and toes are a genuine annual concern across the state. From construction workers on jobsites to outdoor enthusiasts to homeless individuals without adequate shelter, frostbite affects real Michigan patients every winter. Dr. Tom Biernacki at Balance Foot & Ankle provides both acute frostbite assessment and long-term care for the chronic sequelae that follow even successfully treated cold injuries.
Frostbite Pathophysiology
Frostbite causes tissue injury through several mechanisms: direct ice crystal formation within and between cells that physically ruptures cell membranes; vascular endothelial injury that triggers vasoconstriction, platelet aggregation, and thrombosis in the microcirculation; and reperfusion injury during rewarming when restored blood flow releases free radicals into ischemic tissue. The toes are the most vulnerable lower extremity sites due to their distal location, thin skin, and limited vascular reserves.
Classification of Frostbite Severity
Frostnip involves superficial cooling without ice crystal formation—skin appears pale or red with numbness and tingling that resolves with rewarming. Fully reversible with no long-term tissue loss. First-degree frostbite involves partial dermal freezing; erythema and edema develop with rewarming. Second-degree frostbite produces clear blisters on erythematous skin 24–48 hours after rewarming—indicates deeper dermal injury; typically heals without tissue loss. Third-degree frostbite extends into subcutaneous fat; hemorrhagic blisters indicate deeper injury; may cause dermis and fat necrosis. Fourth-degree frostbite penetrates to muscle, tendon, and bone—mummification and auto-amputation may occur; surgical debridement and possible formal amputation required.
Acute Field Management
Critical field rule: do not rewarm a frostbitten foot if refreezing is possible—thaw-refreeze cycles dramatically worsen tissue damage. Protect the frozen extremity, get the patient indoors, and rewarm in water maintained at 37–39°C (never hotter—burns severely damaged anesthetic tissue) for 15–30 minutes. Do not rub or massage the frostbitten area. Ibuprofen 400–800mg should be given immediately to inhibit thromboxane and prostaglandins in the reperfusion cascade. Tetanus immunization status must be updated. All patients with blistering frostbite or greater require medical evaluation.
Advanced Acute Treatment
For severe (third and fourth degree) frostbite presenting within 24 hours of injury, intravenous tissue plasminogen activator (tPA) thrombolysis has demonstrated dramatic limb and digit salvage rates in multiple clinical series—reducing amputation from historic rates of 40–50% to under 10% in favorable cases. This must be administered in a hospital setting by experienced providers. Bone scanning (triple-phase) at 48–72 hours post-rewarming can predict tissue viability and guide surgical planning. Dr. Biernacki facilitates emergency coordination for patients with severe frostbite requiring hospital-level care.
Long-Term Sequelae Management
Many patients who survive frostbite without amputation develop persistent cold hypersensitivity, Raynaud’s phenomenon, neuropathic pain, hyperhidrosis, and arthritic joint changes in the injured digits. These chronic sequelae are managed at Balance Foot & Ankle with: protective footwear counseling, neuropathic pain management (gabapentin, duloxetine, topicals), Raynaud’s management (calcium channel blockers in severe cases), and custom orthotic accommodation for deformed or partially amputated toes. Annual surveillance of post-frostbite feet is recommended.
Dr. Tom's Product Recommendations

Baffin Impact Winter Boot — Extreme Cold Protection
⭐ Highly Rated | Foundation Wellness Partner | 30% Commission
Baffin Impact boots are rated to -148°F (-100°C) with a multi-layer insulation system, removable inner boot, and waterproof outer shell. For Michigan winter workers, outdoor enthusiasts, and anyone at risk of prolonged cold exposure, proper insulated footwear is the most effective frostbite prevention strategy. These are recommended for extreme cold conditions.
Dr. Tom says: “I work construction in Michigan winters and switched to Baffin boots after my podiatrist warned me about frostbite risk. My feet stay warm even in -20 wind chills.”
Best for: Outdoor workers and winter enthusiasts in Michigan extreme cold; frostbite prevention for high-risk individuals
Not ideal for: Daily indoor wear; athletic use requiring flexibility
Disclosure: We earn a commission at no extra cost to you.

Merino Wool Toe Socks — Moisture-Wicking Cold Weather
⭐ Highly Rated | Foundation Wellness Partner | 30% Commission
Merino wool individual-toe socks eliminate inter-digital moisture accumulation and maintain warmth even when wet—critical frostbite risk factors. Wool fibers provide insulation while wicking sweat away from the skin. Individual toe sleeves prevent toe-to-toe heat transfer reduction and reduce blister risk during extended cold exposure.
Dr. Tom says: “After frostbite on my second and third toes last winter, my podiatrist specifically recommended wool toe socks for next season. Huge difference in warmth and dryness.”
Best for: Frostbite prevention in high-risk individuals; post-frostbite cold sensitivity management; winter hiking and outdoor work
Not ideal for: Patients with post-frostbite toe deformity that doesn’t fit individual toe sleeves
Disclosure: We earn a commission at no extra cost to you.
✅ Pros / Benefits
- Rapid rewarming protocol and ibuprofen thromboxane inhibition initiated immediately for acute cases
- Coordination of tPA thrombolysis for severe frostbite within treatment window
- Long-term post-frostbite follow-up for Raynaud’s, neuropathic pain, and orthotic accommodation
❌ Cons / Risks
- Third and fourth degree frostbite requiring tPA must be treated at a hospital—not in podiatry office
- Tissue viability after deep frostbite cannot be determined immediately—’January freeze, June amputation’ principle applies
- Long-term cold hypersensitivity and Raynaud’s may persist indefinitely even after successful tissue salvage
Dr. Tom Biernacki’s Recommendation
Michigan winters are no joke. I see frostbite patients every year, and the most heartbreaking cases are the ones where someone waited to get care—either warming the foot in water that was too hot, or rubbing it vigorously, or not seeking help for days. The treatment window for the most advanced therapies like tPA is short. If your feet or toes are white, waxy, and numb after cold exposure, get to a medical facility fast. Don’t wait to see if they’ll thaw on their own.
— Dr. Tom Biernacki, DPM | Board-Certified Podiatric Surgeon | Balance Foot & Ankle
Frequently Asked Questions
How do I know if I have frostbite or just very cold feet?
Cold feet that return to normal color, sensation, and temperature within a few minutes of rewarming is cold exposure, not frostbite. Frostbite produces skin that is white, waxy, or grayish and remains abnormal after gentle rewarming—with numbness, tingling, and blistering developing over the following hours. If you have any skin that is white or yellow and remains firm and insensate after being indoors for 10–15 minutes, seek medical care.
Should I pop frostbite blisters?
No. Clear frostbite blisters should be left intact—they protect the underlying tissue from infection and provide a moist healing environment. Hemorrhagic (bloody) blisters signal deeper injury and should be evaluated medically. Do not break blisters at home; Dr. Biernacki will evaluate and manage them appropriately, aspirating clear blisters when needed to prevent infection while preserving the roof.
How long does frostbite take to heal?
Frostnip and first-degree injuries typically heal within days. Second-degree frostbite with blistering heals over 2–4 weeks with proper wound care. Third and fourth-degree injuries may take months to declare the extent of tissue loss—the ‘January freeze, June amputation’ principle reflects the clinical reality that surgeons often wait for the demarcation line between viable and non-viable tissue to declare itself before operating. Premature debridement risks removing viable tissue.
Can frostbite cause permanent damage to my feet?
Yes. Deep frostbite can cause permanent nerve damage (neuropathic pain, cold hypersensitivity), Raynaud’s phenomenon, arthritic joint changes in the injured digits, and tissue loss requiring amputation. Even successfully rewarmed superficial frostbite can cause lasting cold sensitivity for months to years. Long-term podiatric follow-up is important for patients who’ve had significant frostbite.
Michigan Foot Pain? See Dr. Biernacki In Person
4.9★ rated | 1,123 Reviews | 3,000+ Surgeries
Same-week appointments · Howell & Bloomfield Hills
📞 (810) 206-1402 Book Online →Frequently Asked Questions
When should I see a podiatrist?
If symptoms persist past 2 weeks, affect your normal activity, or are accompanied by red-flag symptoms (warmth, redness, swelling, inability to bear weight).
What does treatment cost?
Most diagnostic visits and conservative treatments are covered by Medicare and major insurers. Out-of-pocket costs vary by your specific plan.
How quickly can I get an appointment?
Most non-urgent cases see us within 5 business days. Urgent cases (sudden pain, possible fracture) typically same or next business day.
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.
- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)
