Ball of the Foot Pain
Mortons Neuroma [Causes, Symptoms & Best HOME Treatment]
Mortons Neuroma is sharp shooting pain between your 3rd and 4th toes. It can also happen between the 2nd and 3rd toes, 95% we can AVOID surgery!
Ball of the Foot Pain Pictures & Photo Gallery:
Look:
- Metatarsalgia: which means generalized foot pain without a specific cause.
- Second toe capsulitis: this is the inflammation of the second toe joint capsule.
- Capsulitis is related to hammertoe formation, and can lead to a plantar plate tear. There is some overlap between these three disorders. As they get worse tearing and ligament damage can occur.
- Morton’s neuroma: this is the damage and inflammation to the nerves between and underneath the metatarsal joints.
- Fat pad atrophy of the ball of the foot: this is the loss of cushioning in the ball the foot.
- Plantar Plate Tear: A plantar plate tear is ripping of the ligaments holding the toe together.
So, click on the photo gallery to see the specific causes of your ball of the foot pain!
Morton’s Neuroma Overview:
- The Morton’s Neuroma (aka Interdigital Neuroma or Morton’s Neuroma) is a benign(non-cancerous) enlargement of the third common digital branch of the medial plantar nerve.
- Mortons Neuroma is also know by it’s more common name of an interdigital neuroma or Morton’s neuroma.
- This is a very common disorder in that is more of a nuisance than a life threatening problem. Luckily it is very well researched and it is very treatable!
Symptoms of Mortons Neuroma:
- -shooting pain
- -numbness and/or tingling in the third and fourth digits
- -burning sensation
- -cramping
- -feeling of “walking on a lump” in the ball of the foot.
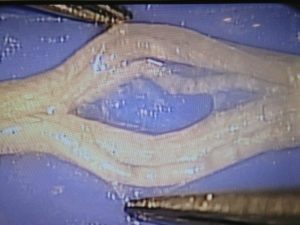
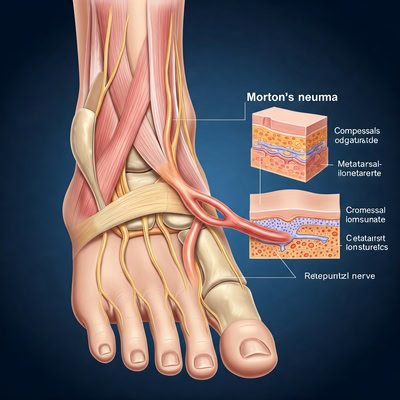
Anatomy of Mortons Neuroma:
- -The interdigital neuroma is a benign(non-cancerous) enlargement of the third common digital branch of the medial plantar nerve.
- -This nerve passes deep to the deep transverse metatarsal ligament.
- -The enlargement or neuroma is usually located at the level of the third and fourth metatarsal heads but often can be found just distal to the metatarsal heads.
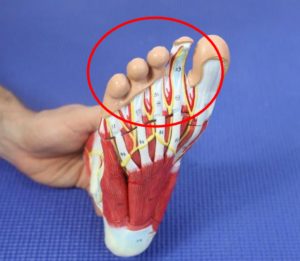
Causes:
- -ischemia (poor blood flow)
- -presence of an intermetatarsal bursa (due to chronic irritation)
- -pronation (flat foot)
- -Equinus (tight hamstring)
- -trauma
- -anatomic thickness of the nerve in the third interspace (genetic)
-Bottom line- the nerve gets impinged somehow and causes swelling & irritation
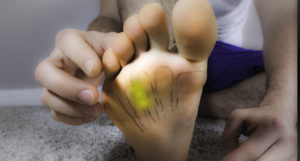
Diagnosis:
- -Mulder Test- Squeeze the foot from side to side & move fingers in the 3rd interspace to feel a click
- -You should be able to feel a big ball between the 3rd and 4th toe joints
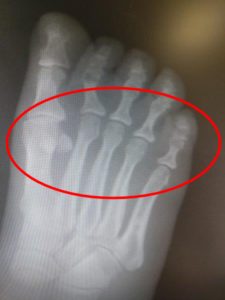
- -MRI, X-ray & Ultrasound confirm it
Non-Surgical Treatment
Goal- Decrease pressure & irritation on nerve
- 1)Metatarsal pads & orthotics can help alleviate pressure and assist in spreading the metatarsal heads ***This has a 41% cure rate according to studies***
- 2)Corticosteroid and local anesthetic combination injection is commonly used. Typically, 1 to 3 injections are given.
- ***80% initial success for 1-3 months, but after 4 years only 11% had permanent relief**
- ***Another Study shows that 60-80% of corticosteroid & lidocaine combinations had relief on a 2 year followup**
- ***Best results came with an Ultrasound guided injection needle – 82% relief on 12 month checkup***
This is most common in people who have very tight hamstrings calf muscles are putting much more pressure on the ball the foot. This can lead to neuroma, metatarsal or even stress fracture pain.
Bottomline:
- About 40% cure with orthotics/Pads
- About 60% with steroids/lidocaine injection
- About 80-85% with a combination of both
- About 15% of people will need the nerve killed with injections or surgery.
Alcohol Sclerosing injection:
- -Injection of a 4% alcohol sclerosing solution has shown complete relief of their symptoms. This injection was given in a series of 3 to 7 injections at 5- to 10-day intervals.
- ***a success rate of 89%, with 82% of patients relaying complete relief of symptoms***
- -Corticosteroid and alcohol sclerosing injections have been used under ultrasound guidance.
- ***partial or total pain relief in 94% of patients, with 84% totally pain free after 10 months***
Surgical management:
-Surgical excision remains the most common procedure for Morton neuroma. It is most commonly performed through a dorsal or plantar longitudinal incision approach. these procedures are essentially the same, with the same goal of neurectomy (to simply cut out the nerve), differences exist in the dissection. You will lose feeling in the area after this surgery.
- Dorsal Approach (from the top)- The dissection is more difficult and more inter-operative complications may occur.
- Plantar Approach (from the bottom)- The dissection is very easy with little complications, but you must be in a surgical boot for 2-3 weeks so a scar or keloid doesn’t develop at the bottom of your boot.
Unique Surgical Options for Mortons Neuroma:
- Nerve decompression- is performed by releasing the deep transverse metatarsal ligament. – this requires a small cut from inbetween the webspace of the 3rd and 4th digits. The ligament above the nerve is cut to allow the nerve to expand. Although this has little complications and feeling remains in your foot – the pain may not go away. Usually if the surgeon observes the nerve as very thick they will just cut it out.
- *** The nerve was excised in 46 of the 69 cases; the nerve was preserved in 23 cases with release of the deep transverse metatarsal ligament. Total relief of symptoms was appreciated in all but one from each group. Thus results were almost 100% successful after surgery***

Unproven Surgical Options:
- Cryogenic Neuroablation- this is a minimally invasive procedure that freezes the nerve at -50 to -70 degrees celsius- the results are not permanent and the procedure is unproven with research.
Complications of Surgery for Mortons Neuroma:
Most Common in descending order:
- 1)Stump neuroma – caused by not resecting the nerve proximal enough, incomplete excision, or tethering of the nerve to the plantar aspect of the metatarsophalangeal joint or other structures.
- 2)One study found that 54% of the time there is a tarsal tunnel irritation at the proximal tibial nerve as well & this is why the surgery did not work.
Less Common
- 3)Damage to the digital arteries- This occurs almost 30% of the time according to some studies- although this almost always leads to no ill effects due to formation of collateral vessels to compensate.
- 4)Hammertoe formation- the toes can splay if the deep transverse inter tarsal ligament required resection.
Very Rare
- Keloid formation, complex regional pain syndrome.
References:
http://en.wikipedia.org/wiki/Morton’s_neuroma
Clinics in Podiatric Medicine and Surgery
Volume 27, Issue 4, October 2010, Pages 535–545
Ball of the Foot Pain Treatment Infographic

Ball of the Foot Home Treatment:
- Consider taping, orthotics, and great shoes as a combination to fix your foot problem.
- Products are not always necessary to fix your problem.
- The key is correcting the biomechanical problems that are leading to forefoot overload.
- Foot overload means too much pressure in the ball of the foot.
- Generally, something called ankle joint equinus can lead to too much pressure in the ball of your foot. This means your ankle is not flexible enough to move up and down.
- Ball of the foot pain treatment consists of two phases, first is control inflammation, next is to control bio-mechanics.
Remove Control Inflammation:
Massage & Ice Products:
- The metal ball is one of my personal favorites.
- This works great for your arch, less for the ball of the foot.
- These can help relax the arch or heel ligaments, leading to less pressure in the ball of the foot.
- Pills, creams, and ice will never completely fix your problem alone. What they will do is reduce the pressure on the area.






Menthol Based Gels:
- Biofreeze is one of our favorites.
- These gels have been studied to work 2x as long as ice.
- This works great for the ball of the foot.
- Consider using these as options when resting on the couch or going to sleep at night.








Massage Sticks:
- These can work great for loosening your muscles.
- This is means for your hamstring and calf muscles. This can loosen the ankle tightness, putting pressure on the ball of your foot.
- This allows less tightness and pressure on the ball of your foot.






Ball of the Foot Stress Relief.
- The key is to prevent future pain.
- If you can get rid of the pain and swelling, this will let you start walking normally.
- If you can walk normally, the vast majority of your pain should gradually start to go away.
- This means proper cushion, proper stability, and pressure relief from the front of your foot.
- This will relieve pressure from your big toe, your 2nd toe, your Morton’s neuroma, your plantar plate, hammertoes and joint capsules.
Best Metatarsalgia Shoes:
- Getting a great supportive pair of shoes will make sure that there is pressure removed from the ball of your foot.
- This is especially important if you have metatarsalgia, Morton’s neuroma, 2nd metatarsal overload syndrome, and capsulitis!
- Consider shoes combined with a good supportive orthotic for the best pain relief!
- The following link will show you what our favorites are.
Best Ball of the Foot Insoles:
- These are our recommended orthotics & insoles.
- There are different types of different shoes.
- Women’s shoes usually need a less bulky orthotic but allow for less correction.
- A full-length orthotic requires a running shoe, boot, or comfortable walking/dress shoe.
Best Full-Length Orthotics:
- Full-length orthotics are the most recommended type for the ball of the foot pain.
- Be aware that if they are too uncomfortable, it might be worth starting with a less corrective pair.
- Eventually, you can then work your way up to these.








Best Dress Shoe Orthotics:
- These are a stronger option for shoes with tight dress shoes.
- Just be aware that less corrective orthotics & tight shoes are usually not a good combination.






Best 3/4 Length Orthotics:
- These may be a good option for the ball of the foot if the full-length orthotics are too tight or too uncomfortable.


Get A Great Dynamic Stretch:
- It is possible to stretch on your own, but these products can also really help!
- Personally, I have the stationary block set up in my kitchen to stretch every day multiple times while getting my coffee!
- This will take pressure off of the ball of your foot.








Ball of the Foot Pain

