Medically Reviewed | Dr. Tom Biernacki, DPM | Board-Certified Podiatric Surgeon | Balance Foot & Ankle, Michigan
Quick Answer:
Quick Answer: Osteomyelitis — bacterial infection of bone — in the foot most commonly occurs as a complication of diabetic foot ulcers that probe to bone or develop chronic non-healing wound beds. It requires combined surgical and antibiotic treatment. Dr. Biernacki performs bone debridement and resection to achieve culture-positive clean margins, coordinates intravenous antibiotic therapy with infectious disease, and reconstructs the wound to achieve healing and preserve the functional foot. Early, aggressive management prevents amputation.
What Is Osteomyelitis?
Osteomyelitis is a serious bacterial infection of bone requiring combined surgical and antibiotic treatment. In the foot, it most commonly develops as a contiguous spread from an overlying soft tissue infection or ulcer — particularly in diabetic patients where neuropathy prevents early detection of skin breakdown. The pathognomonic clinical finding is the ability to probe directly to bone through an ulcer with a sterile metal probe. When “probe to bone” is positive, osteomyelitis is present until proven otherwise, and the diagnostic specificity approaches 90%.
Diagnosis: MRI and Bone Biopsy
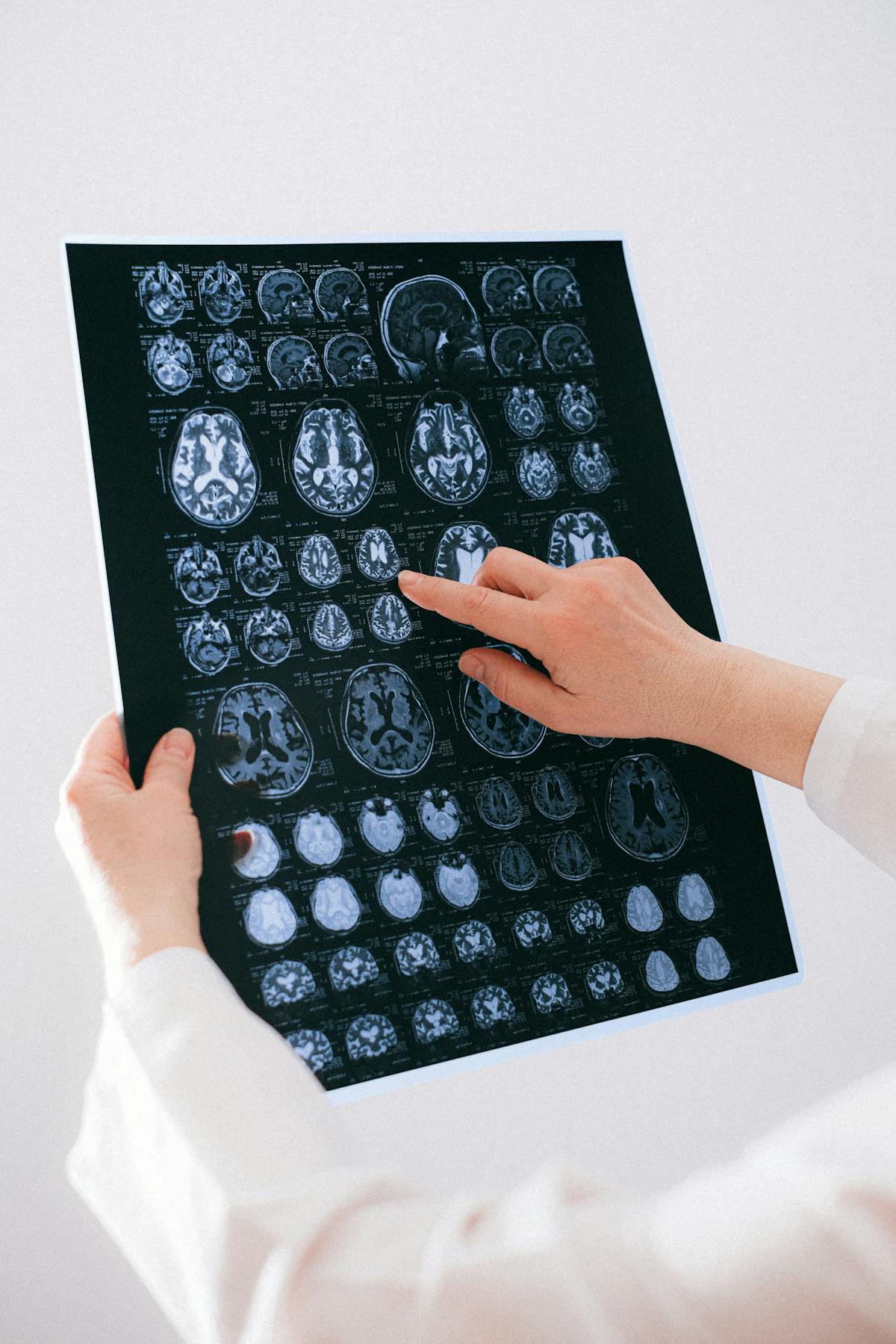
MRI with gadolinium contrast is the gold-standard imaging study for foot osteomyelitis — it demonstrates bone marrow edema and signal change with high sensitivity (90%) and specificity (83%). Plain X-rays are insensitive early — periosteal reaction and bony destruction do not appear until 40–70% of bone mineral is lost, typically 2–4 weeks after infection onset. Bone scan is sensitive but not specific. The critical step is bone biopsy — obtaining a culture from the infected bone directly (not from the wound surface, which reflects skin flora) to identify the causative organism and guide antibiotic selection.
Surgical Treatment: Debridement and Resection
Surgical debridement is the cornerstone of osteomyelitis treatment — removing all infected bone until viable bleeding bone margins are obtained. For forefoot osteomyelitis (metatarsal heads, toes), partial ray resection — removing the infected bone segment with the associated toe — provides definitive treatment and allows reliable wound closure over a smaller tissue defect. For more proximal or complex cases, staged debridement with antibiotic spacer (PMMA beads with antibiotic impregnation) followed by reconstruction may be required. The goal is achieving a viable, plantar-flat foot that can be protected with therapeutic footwear.
Antibiotic Management
Osteomyelitis traditionally required 6 weeks of intravenous antibiotics — a significant burden requiring a PICC line and home infusion service. Recent high-quality evidence (OVIVA trial) demonstrates that oral antibiotic therapy with highly bioavailable agents (fluoroquinolones, linezolid, doxycycline) achieves equivalent outcomes to IV therapy for most cases in compliant patients. Dr. Biernacki coordinates with infectious disease specialists to select the optimal antibiotic duration and route based on the infecting organism, surgical adequacy of debridement, and patient factors.
Vascular Assessment and Optimization
Osteomyelitis in the context of peripheral arterial disease is a limb-threatening emergency — bone infection in an ischemic foot will not respond to antibiotics without restoration of blood flow. Ankle-brachial index, toe pressure, and CTA angiography are obtained when vascular compromise is suspected. Vascular surgical consultation for angioplasty or bypass precedes or accompanies osteomyelitis management in ischemic patients. Dr. Biernacki’s practice coordinates closely with vascular surgery to provide integrated limb salvage care for the most complex diabetic foot cases.
Dr. Tom's Product Recommendations
Silverts Adaptive Diabetic Slippers
⭐ Highly Rated | Foundation Wellness Partner | 30% Commission
Extra-wide adaptive slippers with Velcro closure for post-surgical diabetic feet — designed for patients recovering from foot osteomyelitis debridement with bandaged or modified foot anatomy.
Dr. Tom says: “Fully adjustable Velcro closure accommodates dressings, casts, and post-surgical swelling — essential footwear for the wound care phase after osteomyelitis treatment.”
Post-surgical foot accommodation for osteomyelitis recovery and wound care
Indoor use only — not for outdoor walking on uneven surfaces
Disclosure: We earn a commission at no extra cost to you.
✅ Pros / Benefits
- Probe-to-bone test provides rapid clinical diagnosis at the bedside.
- Bone biopsy guides targeted antibiotic therapy — avoids empirical broadspectrum treatment.
- OVIVA trial supports oral antibiotic therapy — eliminates IV line requirement for many patients.
- Vascular coordination ensures adequate perfusion for wound healing.
❌ Cons / Risks
- Osteomyelitis requires prolonged antibiotic treatment (4–6 weeks) even with adequate debridement.
- Partial ray resection alters foot biomechanics — custom orthotics required post-healing.
- Recurrence rate is significant without complete debridement to viable bone margins.
Dr. Tom Biernacki’s Recommendation
Osteomyelitis is a true foot emergency. Diabetic patients with non-healing ulcers need a probe-to-bone test at every visit — if I can touch bone through that ulcer, the infection is already in the bone and we need to act. The OVIVA trial changed our antibiotic management completely — most of my patients now complete treatment with oral antibiotics at home instead of 6 weeks with an IV line. Game changer.
— Dr. Tom Biernacki, DPM | Board-Certified Podiatric Surgeon | Balance Foot & Ankle
Frequently Asked Questions
How do I know if my diabetic foot ulcer has gone into the bone?
The probe-to-bone test is the most reliable bedside indicator — a sterile metal probe inserted into the ulcer that contacts hard, gritty bone indicates osteomyelitis with ~90% specificity. MRI confirms the diagnosis and defines extent. Never ignore a diabetic foot ulcer that won’t heal despite offloading.
Can osteomyelitis be cured without surgery?
In very limited circumstances — minimal bone involvement, no adjacent abscess, and compliant patient — antibiotic-only treatment may be attempted. However, surgical debridement to clean bone margins significantly improves cure rates and should be performed in virtually all cases with clinical signs of bone infection.
How long are antibiotics needed for foot osteomyelitis?
Typically 4–6 weeks of targeted antibiotic therapy is required. The OVIVA trial showed oral antibiotics equivalent to IV for most cases — most patients can complete treatment at home with twice-daily oral medication rather than a PICC line.
What happens if foot osteomyelitis is not treated?
Untreated osteomyelitis leads to progressive bone destruction, adjacent joint septic arthritis, soft tissue gas (necrotizing fasciitis), septicemia, and ultimately amputation or death from systemic sepsis. Early aggressive treatment — debridement and antibiotics — is life and limb-saving.
Michigan Foot Pain? See Dr. Biernacki In Person
4.9★ rated | 1,123 Reviews | 3,000+ Surgeries
Same-week appointments · Howell & Bloomfield Hills
📞 (810) 206-1402 Book Online →Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.
- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)
