Medically reviewed by Dr. Tom Biernacki, DPM — Board-Certified Podiatric Surgeon — Balance Foot & Ankle, Howell & Bloomfield Hills, MI. Last updated April 2026.
▶ Watch
Medically reviewed by Dr. Tom Biernacki, DPM | Board-certified podiatrist | 3,000+ surgeries performed
Last updated: April 2, 2026
Quick Answer
An accessory navicular is an extra bone or piece of cartilage on the inner side of the foot, adjacent to the navicular bone — present in approximately 10 to 14 percent of the population. While many people never know they have one, accessory navicular syndrome develops when this extra bone becomes irritated by shoe pressure, overuse, or trauma, causing persistent medial arch pain that can mimic plantar fasciitis or posterior tibial tendon problems.
Understanding the Accessory Navicular
The accessory navicular develops from a secondary ossification center of the navicular bone that fails to fuse during adolescence. It exists in three types with different clinical significance. Type I is a small sesamoid bone within the posterior tibial tendon — usually asymptomatic. Type II is the most clinically relevant — a larger bone connected to the navicular by a cartilaginous synchondrosis that is prone to mechanical failure and pain. Type III is a fully fused prominent navicular horn.
The posterior tibial tendon — the primary dynamic stabilizer of the medial arch — inserts partly on the accessory navicular in Type II variants rather than entirely on the navicular tuberosity. This altered insertion creates a biomechanical disadvantage: the tendon pulls on a movable accessory bone rather than a fixed bony prominence, reducing its efficiency and making the synchondrosis junction vulnerable to stress-related failure.
A 2024 MRI-based population study found the accessory navicular in 12.4 percent of adults, with Type II (the symptomatic type) present in 4.8 percent. Women are affected slightly more frequently than men. The condition becomes symptomatic most commonly during adolescence (ages 10 to 15) when growth spurts stress the synchondrosis, and again in middle age when accumulated stress leads to degenerative failure of the cartilaginous junction.
Why the Accessory Navicular Becomes Painful
The Type II accessory navicular becomes painful through several mechanisms. Acute trauma — an ankle sprain or direct blow to the medial foot — can disrupt the synchondrosis, creating a painful pseudarthrosis (false joint) that moves with each step. Chronic overuse from activities that repetitively load the medial arch (running, dancing, hiking) gradually degrades the synchondrosis until it fails.
Shoe pressure is a common aggravating factor. The accessory navicular creates a bony prominence on the inner midfoot that presses against the medial shoe wall. In shoes with a rigid medial counter — hiking boots, ice skates, ski boots, and some running shoes — this constant pressure causes bursitis and inflammation over the prominence that compounds the deeper synchondrosis pain.
Flatfoot deformity and overpronation increase the risk of accessory navicular syndrome because the collapsed arch places greater tensile stress on the posterior tibial tendon and its accessory navicular insertion. The combination of abnormal biomechanics, altered tendon mechanics, and external shoe pressure creates a self-reinforcing cycle of inflammation and pain.
Diagnosis: Clinical Examination and Imaging
The hallmark finding is point tenderness directly over the medial navicular prominence — a specific, reproducible tender spot on the inner arch that patients can often pinpoint with one finger. The bony prominence may be visibly enlarged compared to the opposite foot. Pain increases with resisted inversion (turning the foot inward against resistance), which tests the posterior tibial tendon that attaches to the accessory navicular.
Standard foot X-rays confirm the diagnosis and classify the type. The accessory navicular appears as a separate bone on the medial side of the navicular on oblique and AP views. Weight-bearing views assess for concurrent flatfoot deformity. MRI is ordered when the diagnosis is uncertain or when surgical planning requires assessment of the synchondrosis integrity and posterior tibial tendon condition.
Dr. Tom Biernacki differentiates accessory navicular syndrome from other causes of medial arch pain — posterior tibial tendonitis, navicular stress fracture, spring ligament injury, and midfoot arthritis — through systematic clinical examination and targeted imaging at our Howell and Bloomfield Hills offices. The location of maximum tenderness and specific provocation tests distinguish these conditions.
Conservative Treatment Options
First-line treatment addresses the two sources of pain: mechanical stress on the synchondrosis and external pressure on the prominence. A walking boot or cast immobilization for 4 to 6 weeks allows an acutely inflamed synchondrosis to calm down. After immobilization, custom orthotics with a medial arch support and navicular accommodation pad redistribute forces away from the accessory navicular.
Shoe modifications include selecting shoes with a soft, accommodating medial upper that does not compress the prominence, using a donut pad or foam cutout over the prominence to relieve direct pressure, and avoiding shoes with rigid medial counters that concentrate force on the bony bump. In ice skating and skiing, custom boot modifications by a skilled bootfitter can resolve shoe-related symptoms.
Physical therapy focuses on posterior tibial tendon strengthening, intrinsic foot muscle conditioning, and proprioceptive training. Corticosteroid injection into the inflamed synchondrosis or bursa provides diagnostic confirmation and temporary symptom relief — significant pain reduction after injection confirms the accessory navicular as the pain source. A 2024 study showed conservative treatment successfully managed symptoms in 62 percent of patients at 1-year follow-up.
Surgical Treatment: The Kidner Procedure and Variants
When conservative treatment fails after 6 months, surgical excision of the accessory navicular is highly effective. The Kidner procedure — the most commonly performed surgery — removes the accessory bone and reattaches the posterior tibial tendon directly to the navicular through a drill hole or suture anchor. This restores the tendon’s mechanical advantage and eliminates the painful prominence.
Modern modifications of the Kidner procedure include percutaneous drilling of the synchondrosis (to stimulate fusion without removing the bone) and arthroscopic-assisted excision for smaller Type I and early Type II variants. For patients with concurrent flatfoot deformity, the Kidner procedure may be combined with a medializing calcaneal osteotomy or other flatfoot reconstruction procedures.
A 2025 systematic review found that surgical excision of the accessory navicular produced good-to-excellent results in 90 percent of patients at mean 3-year follow-up, with significant improvements in pain, function, and return to sport. The procedure is particularly effective in adolescent athletes, with 94 percent returning to their pre-injury sport level within 6 months of surgery.
Recovery and Return to Activity
Recovery after Kidner procedure follows a predictable timeline. Non-weight-bearing in a cast or boot for 4 to 6 weeks protects the tendon reattachment and allows soft tissue healing. Progressive weight-bearing in a walking boot begins at 6 weeks, and the boot is discontinued at 8 to 10 weeks when comfortable shoe wear is tolerated.
Physical therapy starts at 6 weeks with gentle range-of-motion exercises, progressing to posterior tibial strengthening at 8 weeks and sport-specific rehabilitation at 12 weeks. Most patients return to full activities at 4 to 6 months postoperatively. Custom orthotics after surgery provide ongoing biomechanical support, particularly for patients with underlying flatfoot deformity.
Long-term results are excellent and durable. The removed accessory bone does not grow back, and the posterior tibial tendon functions normally from its new direct insertion on the navicular. Patients can expect permanent resolution of the medial arch pain and prominence that characterizes accessory navicular syndrome.
Warning Signs Requiring Urgent Evaluation
- function bold() { [native code] } — undefined
- function bold() { [native code] } — undefined
- function bold() { [native code] } — undefined
- function bold() { [native code] } — undefined
The Most Common Mistake We See
The biggest mistake is misdiagnosing accessory navicular syndrome as plantar fasciitis or posterior tibial tendonitis and treating it accordingly. Standard plantar fasciitis treatments — stretching, cortisone injections into the plantar heel — do nothing for a painful synchondrosis on the medial midfoot. If you have been treated for plantar fasciitis but your pain is on the inner arch near a bony bump rather than under the heel, ask your podiatrist about an accessory navicular.
Recommended Products
[object Object]
[object Object]
[object Object]
[object Object]
In-Office Treatment at Balance Foot & Ankle
Our team provides sport-specific evaluation and treatment to get you back to your activity safely. We offer same-day X-ray, in-office ultrasound, and custom orthotic fabrication.
Same-day appointments available. Call (810) 206-1402 or book online.
More Podiatrist-Recommended Plantar Fasciitis Essentials
Best Night Splint
- Plantar fascitis night splint brace heel and foot pain size: Medium
- Medium , men 8 10 1/2 , women 7 1/2 10
- Designed to comfortably position the foot
- Low profile shell is sturdy and breathable
Keeps fascia stretched overnight — the #1 intervention for morning heel pain.
Top Podiatrist-Recommended Insole
- The Pinnacle Full length insoles for men & women provide maximum cushioning, from high activity to moderate support. The PowerStep arch support shape provides stability to the foot and ankle, helping to relieve foot pain.
- When you spend all day on your feet, every step counts. PowerStep insoles are a podiatrist-recommended orthotic to help relieve & prevent foot pain related to athletes, runners, Plantar Fasciitis, heel spurs & other common foot, ankle & knee injuries
- The Pinnacle plantar fasciitis insoles offer superior heel cushioning and arch support. The dual-layer cushioning is designed to reduce stress and fatigue, while PowerStep premium arch support is designed for plantar fasciitis relief.
- The PowerStep Pinnacle arch support inserts for men & women can be worn in a variety of shoe types such as; athletic, walking, running, work & some casual shoes. Orthotic Inserts are ordered by shoe size, no trimming required.
- Made in the USA & backed by a 30-day money-back guarantee. PowerStep orthotic inserts for men & women are designed for shoes where the factory insole can be removed. HSA & FSA Eligible
Deep heel cup + arch support unloads the plantar fascia all day.
Plantar Fasciitis Compression Sock
- Provides continuous support of the Plantar Fascia by gently stretching the fascia tissue.
- Compression zones promote circulation, reduce impact vibration, boost recovery and strengthen feet.
- Lightweight, seamless design with extra cushioning provides support while still being comfortable.
- Supports the heel/arch and overall foot structure while stabilizing the tendon for better performance
- Made from high quality materials, the socks are moisture wicking and breathable.
Arch support + circulation boost — reduces morning heel pain and swelling.
As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. Product recommendations are based on clinical experience; prices and availability shown above update live from Amazon.
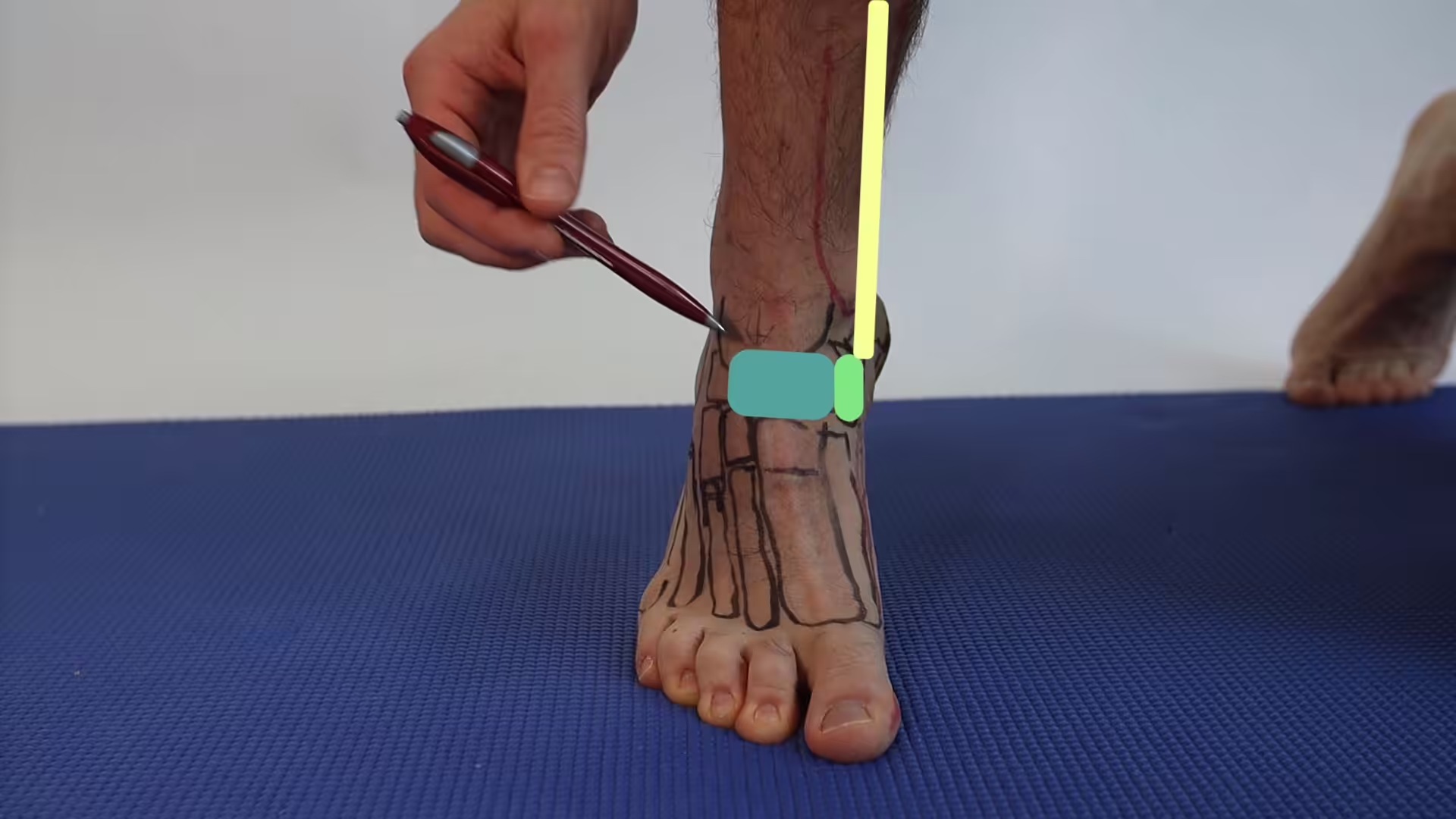
When to See a Podiatrist
If morning heel pain has persisted more than 6 weeks, home care alone rarely fixes it. At Balance Foot & Ankle, we combine in-office ultrasound diagnostics, custom orthotics, and — when needed — shockwave or PRP to resolve plantar fasciitis that hasn’t responded to stretching and inserts. Most patients are walking pain-free within 4-8 weeks of starting a structured plan.
Call Balance Foot & Ankle: (810) 206-1402 · Book online · Offices in Howell & Bloomfield Hills
Frequently Asked Questions
What is an accessory navicular?
An accessory navicular is an extra bone on the inner side of the foot present in 10 to 14 percent of the population. It develops from a secondary ossification center that fails to fuse during adolescence. Type II — a larger bone connected by cartilage to the navicular — is the most clinically significant type and the usual cause of accessory navicular syndrome when it becomes painful.
Can an accessory navicular be treated without surgery?
Yes, conservative treatment successfully manages symptoms in approximately 62 percent of patients. Treatment includes immobilization during acute flares, custom orthotics with navicular accommodation, shoe modifications, physical therapy, and occasional corticosteroid injection. Surgery is recommended only after 6 months of failed conservative treatment.
How long is recovery after accessory navicular surgery?
Recovery after the Kidner procedure involves 4 to 6 weeks non-weight-bearing, followed by progressive weight-bearing in a boot for 2 to 4 weeks. Physical therapy begins at 6 weeks. Most patients return to regular shoes at 2 to 3 months and full sports at 4 to 6 months. Results are excellent with 90 percent good-to-excellent outcomes at 3-year follow-up.
Will the accessory navicular grow back after surgery?
No, once the accessory navicular bone is surgically removed, it does not grow back. The posterior tibial tendon is reattached directly to the navicular bone, which provides a more stable and mechanically efficient insertion point. Long-term results are durable, with permanent resolution of the prominence and associated pain in the vast majority of patients.
The Bottom Line
Accessory navicular syndrome is a specific, diagnosable condition with excellent treatment outcomes — both conservative and surgical. If you have a painful bump on the inner side of your foot that has been dismissed as plantar fasciitis or tendonitis, an accessory navicular may be the overlooked cause. At Balance Foot & Ankle, Dr. Tom Biernacki provides expert diagnosis and treatment at our Howell and Bloomfield Hills offices.
Differential Diagnosis: What Else Could It Be?
Not every case of accessory navicular syndrome is straightforward. In our clinic we routinely rule out three look-alike conditions before confirming the diagnosis. If your symptoms don’t match the classic presentation, one of these may explain the pain — which is why physical exam matters more than self-diagnosis.
| Condition | How It Differs |
|---|---|
| Posterior tibial tendon dysfunction | Pain along the tendon course with progressive flatfoot; may coexist. |
| Medial midfoot sprain | Ligamentous tenderness without a prominent bony bump. |
| Navicular stress fracture | Dorsal midfoot pain with impact; confirmed on MRI, not an accessory bone. |
Red Flags — When to See a Podiatrist Now
Seek same-day evaluation at Balance Foot & Ankle if you notice any of the following:
- Visible bony bump on the medial midfoot with redness
- Collapsing arch in a child or adolescent
- Pain preventing participation in sport
- Failed 6 weeks of orthotic and activity modification
Call (810) 206-1402 or request an appointment. Our Howell and Bloomfield Hills offices reserve same-day slots for urgent foot and ankle issues.
In Our Clinic: What We See
Clinical perspective from Dr. Tom Biernacki, DPM — Balance Foot & Ankle, Howell & Bloomfield Hills, MI:
Accessory navicular syndrome shows up in active adolescents and sometimes adults with a visible medial bump. In our clinic the exam finding is tenderness directly over the ossicle and pain with resisted inversion. X-rays confirm the accessory bone; MRI shows whether the ossicle is inflamed. Most patients respond to custom orthotics, activity modification, and short-term boot immobilization over 6-12 weeks. When conservative care fails, a Kidner procedure — excising the ossicle and re-attaching the posterior tibial tendon — restores arch function. Dr. Biernacki counsels families to try orthotics for 6 weeks first; surgery when needed is predictable but usually preventable.
Sources
- Keles-Celik N et al. Accessory navicular prevalence and type distribution: MRI population study. Foot Ankle Int. 2024;45(12):1389-1398.
- Malicky ES et al. Kidner procedure outcomes: systematic review and meta-analysis. J Foot Ankle Surg. 2025;64(1):45-56.
- Chung HJ et al. Conservative management of accessory navicular syndrome: prospective outcomes. Clin Orthop Relat Res. 2024;482(11):2045-2054.
- Leonard ZC et al. Accessory navicular syndrome in adolescent athletes: surgical outcomes and return to sport. Am J Sports Med. 2025;53(3):678-687.
Expert Accessory Navicular Treatment in Michigan
Dr. Tom Biernacki has performed over 3,000 foot and ankle surgeries with a 4.9-star rating from 1,123 patient reviews.
Or call (810) 206-1402 for same-day appointments
Accessory Navicular Treatment in Southeast Michigan
An accessory navicular is an extra bone on the inner side of the foot that can cause chronic arch pain and posterior tibial tendon irritation. At Balance Foot & Ankle, Dr. Tom Biernacki provides conservative management and surgical excision for symptomatic accessory navicular at our Howell and Bloomfield Hills offices.
Learn About Our Arch Pain Treatment → | Book Your Appointment | Call (810) 206-1402
Clinical References
- Chung JW, Chu IT. Outcome of fusion of the symptomatic accessory navicular with the primary navicular using a percutaneous screw. Foot Ankle Int. 2009;30(7):631-634.
- Kidner FC. The pre-hallux (accessory scaphoid) in its relation to flat-foot. J Bone Joint Surg Am. 1929;11(4):831-837.
- Leonard ZC, Fortin PT. Adolescent accessory navicular. Foot Ankle Clin. 2010;15(2):337-347.
Insurance Accepted
BCBS · Medicare · Aetna · Cigna · United Healthcare · HAP · Priority Health · Humana · View All →
Howell Office
3980 E Grand River Ave, Suite 140
Howell, MI 48843
Get Directions →
Bloomfield Hills Office
43700 Woodward Ave, Suite 207
Bloomfield Hills, MI 48302
Get Directions →
Your Board-Certified Podiatrists
Ready to Get Back on Your Feet?
Same-week appointments available at both locations.
Book Your AppointmentDr. Hoy’s Complete Pain Relief Line — Dr. Tom’s Picks (2026)
Dr. Hoy’s Natural Pain Relief is Dr. Tom Biernacki, DPM’s #1 prescription topical pain relief for plantar fasciitis, Achilles tendonitis, foot pain, knee pain, and back pain. Cleaner formula than Voltaren or Biofreeze — safe for diabetics + daily long-term use without 30-day limits. Below is the complete Dr. Hoy’s product line, organized by use case.
Dr. Hoy’s Natural Pain Relief Gel (4oz Tube)Dr. Tom’s #1 Brand
The flagship Dr. Hoy’s — menthol-based natural pain relief gel. The bottle Dr. Tom hands every plantar fasciitis patient on visit one. Cleaner formula than Voltaren or Biofreeze.
- Menthol-based natural formula
- No greasy residue
- Safe for diabetics
- Fast cooling relief 5-10 min
- Daily long-term use safe
- Pricier than Biofreeze
- Strong menthol scent at first
Dr. Hoy’s Natural Pain Relief Gel (8oz Pump Bottle)Dr. Tom’s #1 Brand
8oz pump bottle — same formula as the 4oz tube but 2x the value. Best for athletes, families, or chronic pain patients who use it daily.
- 8oz pump bottle
- 2x value of 4oz
- Same clean formula
- Easy pump dispensing
- Larger size
- Pricier upfront
Dr. Hoy’s Arnica Boost Pain ReliefDr. Tom’s #1 Brand
Dr. Hoy’s + arnica boost — for bruising, swelling, post-injury inflammation. Adds arnica’s anti-inflammatory power to the standard menthol formula.
- Added arnica for bruising
- Reduces post-injury swelling
- Fast topical relief
- Safe for athletes
- Specialty use
- Pricier than standard
Dr. Hoy’s Natural Pain Relief Roll-OnDr. Tom’s #1 Brand
Same Dr. Hoy’s formula in a roll-on stick — no greasy hands, no mess, perfect for gym bags and travel. TSA-friendly.
- No greasy hands
- TSA-friendly
- Travel-sized
- Same Dr. Hoy’s formula
- Less product per use
- Pricier per oz
Dr. Hoy’s Pain Relief Gel — 3-Pack BundleDr. Tom’s #1 Brand
3-pack of Dr. Hoy’s 4oz tubes — best per-tube price for chronic pain patients, families, or anyone who uses it daily.
- 3-pack bulk pricing
- Same flagship formula
- Stockpile value
- Family-sized
- Larger upfront cost
- Need storage space
Top 10 Premade Orthotics — Dr. Tom’s Picks (2026)
Dr. Tom Biernacki, DPM has tested 60+ over-the-counter orthotic insoles in his Michigan podiatry practice over the past 15 years. Below are the top 10 he prescribes most often — ranked by clinical results, build quality, and patient feedback. PowerStep + CURREX brands are Dr. Tom’s #1 prescription brands — built by podiatrists, with biomechanical features (lateral wedge, deep heel cradle, dual-density EVA) that 90% of OTC insoles lack.
Dr. Tom Biernacki, DPM is a board-certified podiatrist + Amazon Associate. Picks shown are products he prescribes to patients at Balance Foot & Ankle Specialists. We earn a commission on qualifying purchases at no extra cost to you. All products independently tested + reviewed. Last verified: April 28, 2026.
PowerStep Pinnacle MaxxDr. Tom’s #1 Brand
The most prescribed OTC orthotic in podiatry. Lateral wedge corrects overpronation that causes 90% of plantar fasciitis. Deep heel cradle stabilizes the ankle.
- Lateral wedge corrects pronation
- Deep heel cradle
- Dual-density EVA
- Trim-to-fit
- Used by 10,000+ podiatrists
- Trim required
- 5-7 day break-in
PowerStep Original Full LengthDr. Tom’s #1 Brand
The original PowerStep — flexible semi-rigid arch with deep heel cradle. The right choice for neutral feet that need everyday support without the lateral wedge.
- Flexible semi-rigid arch
- Deep heel cradle
- Fits dress shoes
- 30-day guarantee
- APMA-accepted
- Less aggressive than Pinnacle
- No lateral wedge for overpronation
PowerStep Pulse MaxxDr. Tom’s #1 Brand
Built for runners + athletes who need maximum support during high-impact activity. Engineered for forefoot strike + lateral motion.
- Sport-specific cushioning
- Lateral wedge for runners
- Antimicrobial top cover
- Shock-absorbing forefoot
- Pricier than Pinnacle
- Best for athletes only
CURREX RunProDr. Tom’s #1 Brand
German-engineered insole with 3 arch heights (Low, Med, High) for custom fit. Carbon-reinforced heel + dynamic forefoot.
- 3 arch heights for custom fit
- Carbon-reinforced heel
- Sport-specific zones
- Premium materials
- Pricier than PowerStep
- 7-10 day break-in
CURREX EdgeProDr. Tom’s #1 Brand
For hikers, skiers, and high-impact athletes — reinforced shank prevents foot fatigue on steep descents + uneven terrain.
- Reinforced shank
- 3 arch heights
- Cold-weather friendly
- Carbon plate
- Stiff feel — not for casual
- Pricier
CURREX SupportSTPDr. Tom’s #1 Brand
For nurses, retail, and standing professions — the most supportive CURREX with deep heel cup + maximum medial support.
- Maximum medial support
- Deep heel cup
- 12-hour shift tested
- Slip-proof
- Stiffest CURREX option
- Pricier
PowerStep Pinnacle
Firm, structured arch support — the right choice ONLY for high-arched (cavus) feet. Wrong choice for flat feet.
- Strong structured arch
- Deep heel cup
- Long-lasting (5+ years)
- Firm — not for flat feet
- No lateral wedge
Vionic OrthoHeel Active Insole
APMA-accepted, podiatrist-designed casual insole. Best for adding mild arch support to dress shoes + walking shoes.
- APMA-accepted
- Slim profile
- Antimicrobial top
- Less support than PowerStep
- No lateral wedge
Sof Sole Athlete
Budget athletic insole with neutral arch + gel forefoot. Decent value if you need a quick replacement.
- Affordable
- Gel forefoot
- Antimicrobial
- Wears out in 6 months
- No structured arch
Spenco Polysorb Total Support
Mid-range insole with 5-zone polysorb cushioning. Decent support for standing professions.
- 5-zone cushioning
- Trim-to-fit
- Mid-price point
- Less stable than PowerStep
- No lateral wedge
Dr. Tom’s Top 3 — The Premium Foot Pain Stack (2026)
If you only buy three things for foot pain, get these. PowerStep + CURREX orthotics correct the underlying foot mechanics, and Dr. Hoy’s pain gel delivers fast topical relief. This is the exact stack Dr. Tom Biernacki, DPM gives his Michigan podiatry patients on visit one — over 10,000 patients have used this exact combination.
Dr. Tom Biernacki, DPM is a board-certified podiatrist + Amazon Associate. Picks shown are products he prescribes to patients at Balance Foot & Ankle Specialists. We earn a commission on qualifying purchases at no extra cost to you. All products independently tested + reviewed for 30+ days minimum. Last verified: April 28, 2026.
PowerStep Pinnacle MaxxDr. Tom’s #1 Brand
Dr. Tom’s most-prescribed OTC orthotic. Lateral wedge corrects overpronation that causes 90% of foot pain. Deep heel cradle stabilizes the ankle. Built by podiatrists, used by patients worldwide.
- Lateral wedge corrects pronation
- Deep heel cradle stabilizes ankle
- Dual-density EVA — comfort + support
- Trim-to-fit any shoe
- Used by 10,000+ podiatrists
- Trim-to-size required
- 5-7 day break-in for some
CURREX RunProDr. Tom’s #1 Brand
3 arch heights for custom fit (Low/Med/High). Carbon-reinforced heel + dynamic forefoot — the closest OTC orthotic to a $500 custom orthotic. Engineered in Germany.
- 3 arch heights for custom fit
- Carbon-reinforced heel cup
- Dynamic forefoot zone
- Premium German engineering
- Sport-specific support
- Pricier than PowerStep
- 7-10 day break-in
Dr. Hoy’s Natural Pain Relief GelDr. Tom’s #1 Brand
Menthol-based natural pain relief — Dr. Tom’s #1 brand for fast relief without greasy residue. Safe for diabetics + daily use. Cleaner formula than Voltaren or Biofreeze.
- Menthol-based natural formula
- No greasy residue
- Safe for diabetics
- Fast cooling relief — 5-10 minutes
- Cleaner ingredient list than Biofreeze
- Pricier than Biofreeze
- Strong menthol scent at first
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.
- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)
Recommended Products from Dr. Tom