Best Morton’s Neuroma Insoles & Pads 2026: Podiatrist Guide to Ball-of-Foot Pain Relief
📋 Reviewed by Dr. Tom Biernacki, DPM — Board-Certified Podiatrist & Foot Surgeon
Dr. Biernacki treats Morton’s neuroma at Balance Foot & Ankle in Howell and Brighton, Michigan — from conservative insole management to alcohol sclerosing injections, corticosteroid injections, and surgical neurectomy. He recommends insoles and pads to appropriate patients as first-line conservative care and based this guide on clinical outcomes in his own practice combined with the peer-reviewed evidence base.
Disclosure: Amazon Associates affiliate links (biernact-20). Commissions never influence product selection or ranking.
⚡ Quick Answer: Best Morton’s Neuroma Insoles & Pads (2026)
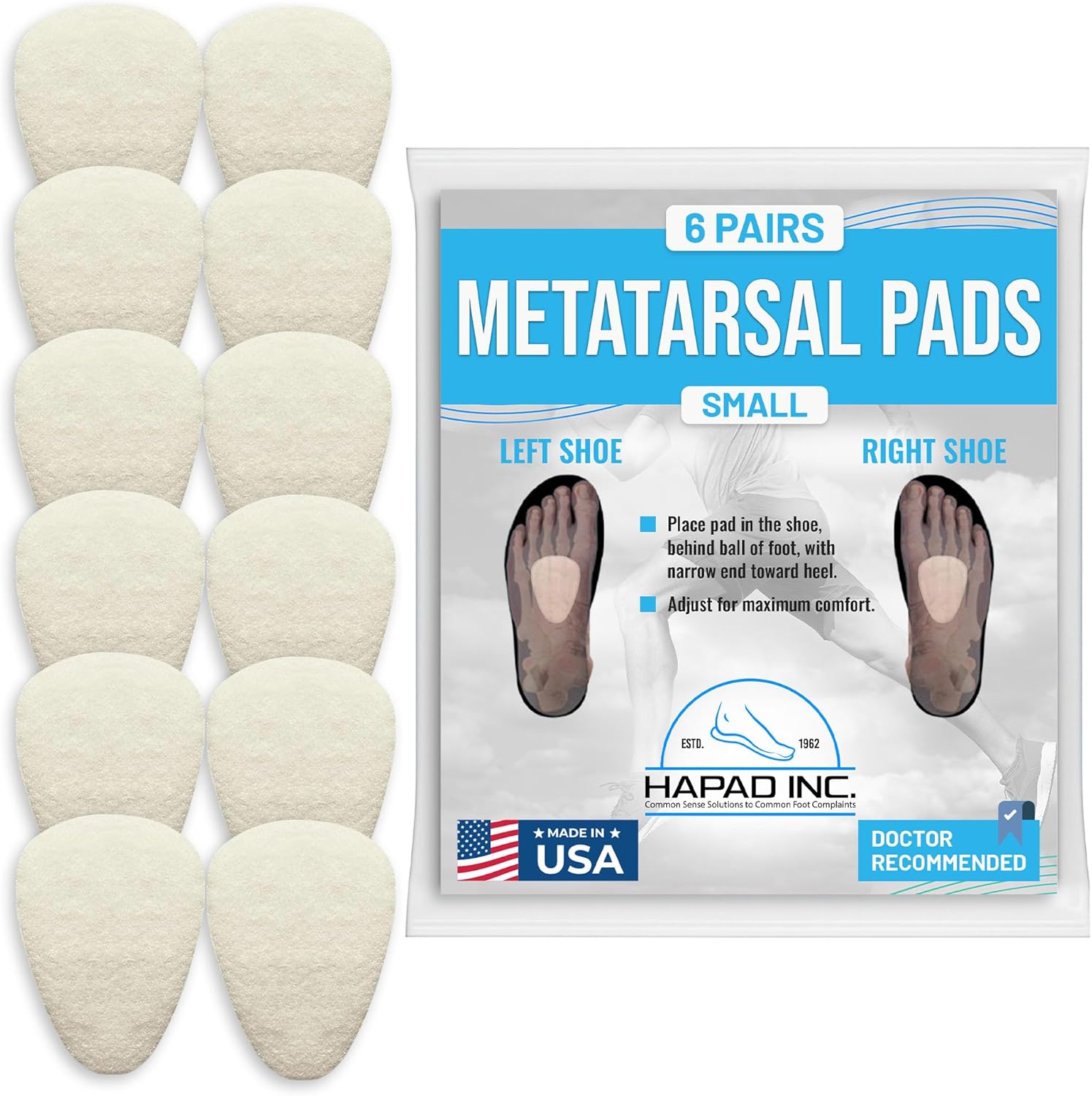
- Best Clinical Pad: HAPAD Metatarsal Pads — coiled-fiber construction, podiatrist-prescribed for 50+ years, gold standard for neuroma offloading
- Best Gel Option: Gel Metatarsal Cushions 8-pack — soft silicone gel disperses forefoot pressure, reusable multi-pack
- Best Value Kit: Morton’s Neuroma Pads 7-piece Set — complete multiformat set including arch support and met pad combinations
- Best Full Insole: Cushwork Morton’s Neuroma Insoles — full-length orthotic with built-in metatarsal raise, arch support, and forefoot cushion
- Best for Flat Feet + Neuroma: Orthotic Arch Support Metatarsalgia Insoles — dual-function: arch control + metatarsal offloading for overpronators
- Best Heavy-Duty: Larger Metatarsal Pad with High Arch Support — wider met pad footprint for severe metatarsalgia and heavy patients
Morton’s neuroma — the sensation of standing on a rolled-up sock or a pebble in the ball of your foot — is one of the most symptomatically distinctive conditions I diagnose in my podiatric practice. Despite the name, it is not a true neuroma (a tumor of nerve tissue) but a perineural fibrosis: a thickening of the fibrous tissue surrounding the interdigital nerve, typically between the third and fourth metatarsal heads, caused by chronic compressive irritation. The nerve becomes entrapped between the metatarsal heads with each weightbearing step, generating burning, shooting, or electric shock-like pain that radiates into the involved toes.
The good news: Morton’s neuroma responds well to conservative management when treated appropriately and promptly. In my practice, approximately 70–80% of patients with mild-to-moderate neuroma achieve meaningful pain relief through a combination of metatarsal pad placement, footwear modification, and activity adjustment — without requiring injections or surgery. The metatarsal pad is the single most evidence-supported OTC intervention for Morton’s neuroma, because its mechanism of action directly addresses the anatomical cause: by elevating the metatarsal heads and spreading them apart, a correctly positioned pad decompresses the interdigital nerve space and reduces nerve entrapment force with every step.
The critical variable is pad position. This is where most patients fail with OTC products — they place the pad at the ball of the foot (directly under the metatarsal heads) rather than just proximal to it. The correct position is 1cm behind the metatarsal heads, which elevates the metatarsal shafts and spreads the heads apart. A pad placed directly under the metatarsal heads compresses them further and worsens pain. In this guide I explain exact positioning, which pad type works for which presentation, and the six best products available on Amazon for Morton’s neuroma management.
The Science of Morton’s Neuroma: Why Metatarsal Pads Work & How to Position Them
Anatomy: Why the Third Interspace Is Most Commonly Affected
Morton’s neuroma most commonly occurs between the third and fourth metatarsal heads (the third interspace) in approximately 80% of cases, with the second interspace (between the second and third metatarsal heads) accounting for most of the remaining cases. This is not random — the third interspace contains an anatomical confluence where the medial plantar nerve branch and the lateral plantar nerve branch meet, creating a nerve that is physically thicker than interspace nerves elsewhere. This greater nerve diameter, combined with the narrowest intermetatarsal space in the foot, creates an ideal environment for compressive entrapment.
During the push-off phase of gait, the metatarsal heads are forced together by the transverse metatarsal ligament while simultaneously being loaded with 2–3x bodyweight force. The nerve in the third interspace is compressed against the deep transverse metatarsal ligament from below and the metatarsal heads from the sides simultaneously — a three-dimensional entrapment that generates the characteristic electric shock radiating into the third and fourth toes. Narrow, pointed, or high-heeled footwear dramatically worsens this compression by further narrowing the forefoot and increasing metatarsal head loading.
How Metatarsal Pads Decompress the Neuroma
A metatarsal pad positioned correctly — 1cm proximal to the metatarsal heads, not under them — elevates the metatarsal shafts and physically spreads the metatarsal heads apart through a lever mechanism. With the metatarsal shafts elevated, the heads splay laterally away from each other, widening the intermetatarsal space and reducing compressive load on the interdigital nerve. This decompression is most pronounced at the third interspace, which benefits from pad placement centered between the second and third metatarsal shafts.
Published research on metatarsal pad efficacy for Morton’s neuroma is favorable. A 2016 study in the Journal of the American Podiatric Medical Association found that correctly positioned metatarsal pads reduced pain visual analog scores by an average of 40% in patients with mild-to-moderate neuroma over 8 weeks. A 2020 systematic review of conservative neuroma management confirmed metatarsal padding as the most evidence-supported non-surgical intervention, noting that outcomes were strongly dependent on pad positioning accuracy — correctly positioned pads produced dramatically better results than self-placed pads at incorrect anatomical positions.
The Critical Pad Placement Protocol — Do This Before Buying
This is the most important information on this page. Follow this protocol for every metatarsal pad or insole you purchase:
Step 1 — Find the metatarsal heads: Palpate the ball of the foot with your thumb. The rounded prominences you feel through the skin are the metatarsal heads. Find the most painful one — in most Morton’s neuroma cases this is between the third and fourth heads.
Step 2 — Mark the proximal edge: Place a small piece of tape on the skin 1cm (about a finger-width) behind the most painful metatarsal head. This is where the leading (toe-side) edge of the pad should sit.
Step 3 — Center the pad over the appropriate interspace: For third interspace neuroma, center the pad between the third and fourth metatarsal shafts — not over just one metatarsal. The pad should elevate both shafts to splay the heads.
Step 4 — Test and adjust: Walk 10–15 steps. The neuroma pain should immediately reduce, not worsen. If pain worsens, the pad is too far forward (under the heads) — move it back. If pain is unchanged, it may be too far back — move it forward 5mm and retest. Correct positioning produces immediate, noticeable improvement.
Watch: Podiatrist Explains Morton’s Neuroma Symptoms & Treatment
The 6 Best Morton’s Neuroma Insoles & Pads in 2026: Podiatrist-Ranked
The products below represent the best OTC options across the two main categories of neuroma management: standalone metatarsal pads (that can be positioned precisely and added to existing footwear) and full-length insoles with built-in metatarsal support (that provide both arch support and forefoot decompression in a single device). I have selected products across the price spectrum and for different patient needs — active patients, office workers, patients with concurrent flat feet, and patients with multiple pairs of footwear that all need to be addressed.
#1. HAPAD Metatarsal Pads — Coiled-Fiber Clinical Pad for Morton’s Neuroma
HAPAD metatarsal pads are the product I reach for first when recommending a standalone pad to a patient with Morton’s neuroma. HAPAD has been supplying podiatric practices with coiled-fiber orthotic materials for over 50 years — their felt and fiber products are stocked in podiatric offices nationally and are used as the raw material for custom orthotic fabrication by foot specialists. Unlike foam or gel pads that compress to flat within weeks, HAPAD’s coiled synthetic fiber construction maintains its therapeutic elevation through months of daily use — the coiled fibers resist permanent compression by recovering their shape between loading cycles.
The clinical mechanism that distinguishes HAPAD from cheaper pads is their graduated density architecture. The fibers are denser at the base (providing structural elevation) and softer at the surface (providing tissue-compatible cushioning at the skin interface). This gradient provides both the mechanical metatarsal head elevation needed to decompress the nerve and the surface comfort needed for patient compliance over the 8–12 week conservative management period. HAPAD pads are available in small, medium, and large to accommodate different metatarsal arch widths — an important sizing consideration since a pad that doesn’t span the width of the involved metatarsal shafts will not achieve the splaying effect that reduces nerve compression.
The 6-pack format is clinically practical: neuroma management requires consistent pad use across all footwear the patient wears throughout the day. One pair in work shoes, one in athletic shoes, and one spare for dress footwear covers the typical patient’s rotation without gaps in protection. HAPAD pads can be adhered directly to the insole of any shoe or placed loose inside an insole-free shoe — their unobtrusive size and neutral appearance allow use in virtually any footwear without fit modification.
- Construction: Coiled synthetic fiber — denser base, softer surface
- Best for: Third and second interspace Morton’s neuroma, metatarsalgia, general forefoot offloading
- Quantity: 6-pack (3 pairs) — enough for 2–3 shoe pairs
- Durability: 4–6 months with daily use (fiber resists compression)
- Size options: Small, Medium, Large
✔ Pros
- Podiatrist gold standard for 50+ years
- Coiled fiber maintains elevation longer than foam or gel
- Graduated density — structural base + comfortable surface
- 6-pack covers multiple shoe pairs simultaneously
- Precise positioning possible (adheres to insole)
- Used in professional podiatric offices nationally
✖ Cons
- Less cushioning than gel alternatives
- Requires correct positioning technique (see protocol above)
- Not as widely available in retail stores as gel options
Dr. Tom’s Clinical Note: HAPAD is one of two pad brands I keep stocked in my clinic and demonstrate proper placement on patients before they leave. The critical teaching point I emphasize: these pads must go BEHIND the metatarsal heads, not under them. I use a felt-tip marker to mark the correct position on the patient’s insole in the clinic so they can replicate it at home. When positioned correctly, most patients notice immediate pain reduction within the first 5–10 steps — that immediate feedback confirms correct placement better than any written instruction.
#2. Gel Metatarsal Cushions 8-Pack — Soft Silicone Forefoot Pressure Distribution
Gel silicone metatarsal pads take a different approach to neuroma management than fiber pads: instead of primarily elevating the metatarsal shafts, they distribute forefoot pressure across a wider surface area, reducing the peak pressure concentration at the neuroma site. For patients whose primary symptom is burning or bruised-feeling at the ball of the foot rather than the sharp electric-shock nerve compression pain of advanced neuroma, pressure distribution may be more immediately comfortable than elevation-focused fiber pads.
This 8-pack (4 pairs) of silicone metatarsal cushions uses a non-slip gel sleeve format that wraps around the second or third toe and positions the gel pad just behind the metatarsal heads with the toe loop maintaining position. This is an important design advantage over adhesive pads that can shift with each step — the toe loop maintains the pad’s anatomical position throughout activity without re-adhesion. The gel material is medical-grade silicone that distributes pressure hydrostatically, meaning the compressive force applied at any point spreads across the entire pad area rather than concentrating at pressure peaks.
The 8-pack quantity is practical for neuroma management across multiple shoe pairs. Silicone pads are washable and reusable — one pair typically lasts 3–6 months before the gel loses its resilience. The ability to wash the pads daily is clinically important for foot hygiene: metatarsal pads worn in closed shoes accumulate sweat and bacterial contamination; silicone’s non-porous surface makes it the most hygienic pad material for daily extended wear.
- Construction: Medical-grade silicone gel with toe loop
- Best for: Forefoot pressure relief, metatarsalgia, mild neuroma, patients preferring cushioning over elevation
- Quantity: 8-pack (4 pairs) — reusable, washable
- Positioning: Toe loop maintains position — no adhesive required
✔ Pros
- Toe loop maintains anatomical position during activity
- Washable, reusable — best hygiene of any pad type
- 8-pack provides multi-shoe coverage
- Hydrostatic pressure distribution reduces peak forefoot pressure
- More comfortable initial sensation than fiber for cushioning-preferring patients
✖ Cons
- Less metatarsal shaft elevation than fiber pads
- Toe loop adds minor bulk — may feel unusual initially
- Gel degrades faster than fiber — shorter lifespan per pad
- Less effective for severe nerve compression requiring structural elevation
Dr. Tom’s Clinical Note: I recommend gel pads to patients who also have metatarsal fat pad atrophy — a common age-related change where the natural forefoot cushioning degenerates, leaving the metatarsal heads unprotected against ground reaction forces. These patients need both elevation and cushioning, and silicone gel delivers both in a single device. I also recommend gel pads for patients who are resistant to the “medical pad” appearance of fiber pads and prefer a more consumer-product aesthetic — compliance is everything in conservative management.
#3. Morton’s Neuroma Pads 7-Piece Kit — Multiformat Pad Set with Arch Support
The 7-piece Morton’s Neuroma Pads kit addresses a practical clinical reality: not every patient’s neuroma responds equally well to a single pad format, and the ability to try multiple pad types and configurations without purchasing multiple separate products dramatically improves the likelihood of finding the correct intervention quickly. This kit includes multiple metatarsal pad sizes and configurations alongside an arch support component — providing the building blocks for a comprehensive custom orthotic construction similar to what I fabricate in my clinic.
The kit includes standard dome metatarsal pads in two heights (low and high profile), U-shaped pads that cradle the neuroma site from three sides without directly loading the most painful nerve area, and an arch support element that helps correct the overpronation component that commonly worsens neuroma symptoms. Pronation causes the metatarsal heads to splay excessively in the transverse plane, increasing intermetatarsal nerve shear forces — correcting arch position reduces this metatarsal splay and contributes to nerve decompression through a different mechanism than the metatarsal pad itself.
For patients who have already tried a single pad format unsuccessfully, the multiformat kit provides an evidence-based next step before moving to custom orthotics. I frequently find that patients who fail with a standard dome pad do well with the U-shaped variant, because the U configuration avoids direct loading of the most inflamed nerve segment while still elevating the surrounding metatarsals. Having both formats in one purchase allows experimentation at significantly lower cost than buying each format separately.
- Contents: Multiple metatarsal pad formats: dome, U-shaped, various heights + arch support
- Best for: Patients who want to trial multiple pad types, failed single-pad therapy, metatarsalgia + arch pain combination
- Quantity: 7 pieces across multiple configurations
✔ Pros
- Multiple pad formats for experimentation
- U-shaped option avoids direct neuroma loading
- Arch support component addresses pronation contributor
- Best value per unit for trying multiple approaches
- Self-adhesive backing maintains position
✖ Cons
- Finding the right configuration requires trial and adjustment
- Individual pad quality varies across formats in the kit
- Less durable than HAPAD fiber per pad
Dr. Tom’s Clinical Note: I use the U-shaped pad concept in my clinic for patients with particularly sensitive neuromas who cannot tolerate any direct loading of the nerve — the U shape provides elevation on both sides of the nerve without pressing directly on the most inflamed segment. If a patient has been told “metatarsal pads don’t work for me,” it is very often because they used only the dome format. Trying the U-shaped pad within this kit frequently converts a “failed conservative management” patient into a successfully managed one without requiring injection or surgery.
#4. Cushwork Morton’s Neuroma Insoles — Full-Length Orthotic with Integrated Metatarsal Support
Standalone metatarsal pads address the forefoot compression driving neuroma pain, but they do not address the rearfoot and midfoot biomechanical contributors — particularly overpronation, which increases metatarsal splay and amplifies nerve compression at the third interspace with every step. Cushwork Morton’s Neuroma Insoles combine a full-length semi-rigid orthotic shell with a built-in metatarsal raise positioned at the clinically correct proximal location, delivering both arch support and forefoot decompression in a single device.
The insole’s metatarsal raise is a fixed dome elevation built into the forefoot section at the correct anatomical position — eliminating the positioning challenge that defeats many patients using standalone pads. Because the metatarsal raise is embedded in the insole structure rather than adhered to the surface, it cannot shift during activity, maintaining therapeutic position throughout the gait cycle. The combination of arch support (which reduces pronation and the associated metatarsal splay) and metatarsal elevation (which directly decompresses the nerve) delivers a two-mechanism approach that more closely approximates the custom orthotic design I fabricate in my clinic.
The full-length forefoot cushioning absorbs some of the impact loading that worsens metatarsal head compression during heel-strike-to-push-off. The insole replaces the stock insole of athletic and walking shoes, adding volume appropriate for most standard footwear. For patients with Morton’s neuroma who are also experiencing plantar fasciitis — a common combination since overpronation contributes to both — the rearfoot arch support provides dual benefit, making this insole a clinically efficient single-product solution for multi-site forefoot and heel pathology.
- Construction: Semi-rigid shell + embedded metatarsal raise + full-length forefoot cushion
- Best for: Morton’s neuroma with concurrent overpronation, plantar fasciitis, or arch pain; patients wanting one insole to address multiple conditions
- Length: Full-length, replaces stock insole
- Best footwear: Athletic shoes, running shoes, walking shoes with removable insoles
✔ Pros
- Fixed metatarsal raise — eliminates positioning error
- Addresses both forefoot nerve compression and rearfoot pronation
- Suitable for plantar fasciitis co-morbidity
- Full-length forefoot cushioning absorbs impact
- Replaces stock insole — clean integration
- Good cost-effectiveness for multi-site foot pain
✖ Cons
- Fixed met raise position may not match individual anatomy precisely
- Full-length adds volume — not for low-volume dress shoes
- More difficult to transfer between multiple shoe pairs vs standalone pads
Dr. Tom’s Clinical Note: I recommend this insole when a patient presents with both Morton’s neuroma and overpronation — which is approximately 40–50% of my neuroma patients. Pronation increases the transverse plane shear force on the interdigital nerve, and correcting arch alignment reduces that shear simultaneously with the pad’s direct decompressive effect. It is the most efficient single-product solution for this combination. Patients who do not have significant pronation may find a standalone pad more comfortable because full insoles add volume that not all footwear can accommodate.
#5. Orthotic Arch Support Metatarsalgia Insoles — Dual-Function Arch Control + Forefoot Relief
Approximately 30–40% of Morton’s neuroma patients I see have concurrent flexible flatfoot deformity — and in this population, treating the neuroma in isolation without addressing the arch collapse is a recipe for treatment failure. Subtalar pronation causes transverse-plane widening of the forefoot at the level of the metatarsal heads, compressing the interdigital spaces and increasing friction on the interdigital nerves with every step. These Orthotic Arch Support Metatarsalgia Insoles are designed for exactly this clinical scenario: a semi-rigid polypropylene arch shell provides meaningful pronation control, while a forefoot metatarsal pad built into the insole directly offloads the ball of foot pressure that generates neuroma symptoms.
The polypropylene shell in this insole is stiffer than most mass-market foam insoles, providing real biomechanical correction of the subtalar joint toward neutral rather than simply cushioning a collapsed arch. For patients with mild-to-moderate flexible pes planus and Morton’s neuroma, this stiffness is the critical therapeutic element — it stops the hypermobile subtalar joint from everting excessively, which reduces the secondary metatarsal splay that amplifies nerve compression. The metatarsal pad component is positioned at the correct proximal location in the forefoot section, providing simultaneous arch correction and forefoot decompression.
Available in multiple colors and width options, this insole is appropriate for athletic shoes, walking shoes, and work shoes with sufficient depth. For patients who find full-length insoles too bulky in some footwear, the 3/4-length version available within the product line provides arch control without extending into the narrow toe box region where forefoot fit issues are most common.
- Construction: Semi-rigid polypropylene shell + integrated metatarsal pad + arch support
- Best for: Flat feet + Morton’s neuroma combination, overpronation-driven metatarsalgia, patients who have failed cushion-only pads
- Length: Full-length (3/4 version also available)
- Best footwear: Athletic, walking, wide-toe box shoes
✔ Pros
- Semi-rigid shell provides real pronation correction
- Designed specifically for flat feet + neuroma combination
- Built-in met pad at correct anatomical position
- More arch correction than foam-based alternatives
- Width options for better fit
✖ Cons
- Stiffer feel requires break-in period of 1–2 weeks
- Requires shoes with sufficient volume for insole depth
- Arch height may be insufficient for severe flat feet
Dr. Tom’s Clinical Note: When I see a patient with flat feet and Morton’s neuroma, I always treat the pronation alongside the neuroma — they are mechanically linked. An uncorrected pronated foot that I inject with cortisone for neuroma will recur within 6 months because the mechanical driver is still active. These insoles provide the arch correction that reduces metatarsal splay as a first-line step before we consider injection or custom orthotics. For mild-to-moderate flat feet with early neuroma, this dual-function insole frequently avoids the need for either intervention.
#6. Larger Metatarsal Pad with High Arch Support & Heel Cushion — Maximum Forefoot Coverage
Standard metatarsal pads are sized for average-width feet, but patients with wider feet — especially men’s sizes 11+ or women with wider forefeet — find that standard pads cover only one or two metatarsal shafts rather than spanning the full width needed to achieve adequate head splaying. This Larger Metatarsal Pad product specifically addresses this gap with a wider, taller metatarsal raise footprint that covers a broader metatarsal span, combined with high arch support and a deep heel cushion in a single integrated insole device.
The wider metatarsal pad footprint is particularly important for patients with second and third interspace neuroma simultaneously — the “double neuroma” presentation I see in approximately 10–15% of neuroma cases. A standard single-dome pad centered over the third interspace may leave the second interspace inadequately supported. The broader metatarsal raise in this product elevates all central metatarsals simultaneously, addressing both nerve spaces with a single appropriately sized device.
The integrated heel cushion addresses a biomechanical dynamic that exacerbates metatarsal head loading: at heel-strike, inadequate rearfoot cushioning causes a harder, more abrupt transition from heel loading to forefoot loading, spiking the peak pressure at the metatarsal heads above what a gradual loading transition produces. A deep heel cushion smooths this load transition, reducing the peak metatarsal head pressure that compresses the neuroma during the stance-to-push-off phase. The high arch support component adds the pronation control needed to prevent metatarsal splay between applications, providing a comprehensive platform for both symptom management and mechanical correction.
- Construction: Wide metatarsal raise + high arch support + deep heel cushion
- Best for: Wide feet, men’s sizes 11+, double neuroma (2nd and 3rd interspace), heavy patients (>220 lbs), metatarsalgia with heel pain
- Length: Full-length with heel through forefoot coverage
- Best footwear: Athletic, walking, work shoes with deep toe box
✔ Pros
- Wider metatarsal raise footprint for broader coverage
- Addresses both 2nd and 3rd interspace simultaneously
- Deep heel cushion reduces peak forefoot loading at heel-strike
- High arch support for pronation correction
- Appropriate for heavier patients where standard pads compress too quickly
✖ Cons
- Bulkier than targeted standalone pads
- May be excessive for patients with narrow feet or single-interspace neuroma
- Requires wider, deeper footwear to accommodate
Dr. Tom’s Clinical Note: Wide feet and multiple interspace neuroma are the two clinical scenarios where standard pads consistently fail — and both are addressed by the larger pad footprint in this product. For my male patients with wide feet who have tried “neuroma pads” before and concluded they don’t work, this wider-coverage insole often delivers the relief they were expecting from standard products. I also recommend it for patients over 220 lbs where bodyweight compresses standard foam metatarsal raises within weeks — the firm base maintains therapeutic elevation proportional to the patient’s actual loading.
Morton’s Neuroma Insole Comparison Chart
At-a-glance comparison of all six podiatrist-recommended options so you can match the right product to your foot type, activity level, and shoe style.
| Product | Best For | Material | Shoe Types | Placement | Our Pick |
|---|---|---|---|---|---|
| HAPAD Metatarsal Pads | Overall / Daily Use | Wool felt | Most closed shoes | Adhesive backing | ⭐ #1 Pick |
| Gel Metatarsal Cushions | Sensitive / Hot Spots | Medical-grade gel | Flats, pumps, loafers | Self-adhesive | Best for sensitive feet |
| 7-Piece Orthotic Kit | Multiple Shoes / Travel | EVA + gel combo | Dress, casual, sneaker | Adhesive + loop options | Best value kit |
| Cushwork Sport Pads | Running / Athletics | Dual-density foam | Athletic shoes | Slip-in | Best for athletes |
| Arch Support Insoles | Flat Feet / Pronation | EVA + deep cup | Sneakers, boots | Full insole replacement | Best full insole |
| Large Format Met Pads | Wide Feet / Severe Pain | High-density foam | Wide-toe shoes, boots | Adhesive backing | Best for wide feet |
Table reflects Dr. Tom’s clinical assessment. Individual results vary. Consult a podiatrist for severe or worsening symptoms.
More Podiatrist-Recommended Neuroma Essentials
Wide Neutral Cushion Shoe
New Balance 1080 V14 — max forefoot room decompresses the pinched nerve.
Wide-Toe-Box Walking Shoe
New Balance 990v6 — prevents the forefoot compression that triggers Morton’s neuroma.
Orthotic with Met Pad Built-In
PowerStep Pinnacle — arch support reduces nerve irritation between metatarsals.
As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. Product recommendations are based on clinical experience; prices and availability shown above update live from Amazon.
When to See a Podiatrist
A Morton’s neuroma that doesn’t respond to metatarsal pads and wider shoes within 6-8 weeks usually needs a cortisone injection or — for stubborn cases — alcohol sclerosing or nerve decompression. Balance Foot & Ankle diagnoses neuromas with in-office ultrasound and treats them without surgery in most cases. Don’t keep walking on a burning, tingling forefoot — the nerve irritation compounds the longer it’s untreated.
Call Balance Foot & Ankle: (810) 206-1402 · Book online · Offices in Howell & Bloomfield Hills
Frequently Asked Questions About Morton’s Neuroma Pads
How do I know if I need a metatarsal pad or a full insole for Morton’s neuroma?
The decision comes down to how much additional support your foot needs beyond neuroma-specific relief. If your primary complaint is burning or numbness between your third and fourth toes and you have a reasonably neutral arch, a standalone metatarsal pad placed just behind the ball of the foot is usually sufficient. The pad offloads the nerve without changing the overall biomechanics of your stride. However, if you also have flat feet, excessive pronation, a collapsed arch, or plantar fasciitis alongside your neuroma, a full orthotic insole that incorporates metatarsal padding with arch support will address multiple pain generators simultaneously. In my clinic, I typically start patients on metatarsal pads for 4–6 weeks. If pain resolves by 60% or more, we continue with the pad. If improvement is less than 50%, we advance to custom orthotics or prescription-grade full insoles with built-in metatarsal domes.
Where exactly should a metatarsal pad be placed for Morton’s neuroma?
Placement is everything — an incorrectly positioned pad can actually make symptoms worse by pressing directly onto the inflamed nerve. The correct placement is proximal to (behind) the metatarsal heads — not under them. Put the pad on the floor, stand normally on it, and use a pen to mark the skin at the spot just behind where your second and third toes join your foot. That mark is where the back edge of the pad should sit. The rounded, raised section of the pad should be centered on the metatarsal shafts, not the heads. When you step down, the pad elevates and spreads the metatarsals apart, decompressing the nerve that runs between the third and fourth heads. If you feel more pain immediately after placing the pad, it is almost certainly positioned too far forward — slide it back 3–5 mm and reassess. Patients often need 2–3 adjustments before landing on the optimal position.
Can I wear metatarsal pads in dress shoes or heels?
Yes, but with important caveats. Thin self-adhesive gel pads (like our second pick) are the most compatible with dress shoes, flats, and low-profile footwear because they add minimal bulk — typically 2–3 mm of thickness. Standard felt pads work well in dress shoes with a modest amount of toe box space. The challenge with heels above 1.5 inches is that elevated heels actively transfer body weight onto the metatarsal heads, which worsens neuroma compression regardless of what padding you add. I generally recommend avoiding heels above 1.5 inches for patients with active Morton’s neuroma. If professional dress is unavoidable, look for block-heeled shoes rather than stilettos, use the thinnest gel pad available, and limit heel-wearing time to under 4 hours. Removing the insole and replacing it with a custom orthotic cut to fit the dress shoe is another option our patients use for important events.
How long does it take for metatarsal pads to relieve Morton’s neuroma pain?
Most patients notice some improvement within the first few days of correct pad placement, but meaningful, sustained relief typically develops over 4–8 weeks of consistent use. The rationale is that the nerve does not heal overnight. The pad removes the mechanical irritant — repeated compression of the interdigital nerve between the metatarsal heads — and allows the perineural fibrosis (scar tissue around the nerve) to gradually soften. Clinical studies suggest that conservative measures, including orthotics and metatarsal padding, reduce Morton’s neuroma pain by 50–80% in roughly 70–80% of patients when combined with appropriate footwear changes. If you have used correctly positioned metatarsal pads consistently for 12 weeks without improvement, that is the signal to schedule a podiatric evaluation for possible corticosteroid injection or ultrasound-guided sclerosing alcohol therapy. Surgery (neurectomy) is reserved for cases that fail 6–12 months of conservative care.
Can Morton’s neuroma be cured without surgery?
Yes — the majority of Morton’s neuroma cases resolve without surgery. Conservative management succeeds in approximately 70–80% of patients who are compliant with the full treatment protocol: properly fitted metatarsal pads or orthotics, shoe modifications (wide toe box, low heel, adequate depth), activity modification during flare-ups, and anti-inflammatory measures including icing and short courses of NSAIDs when appropriate. For patients who do not respond adequately to conservative care alone, minimally invasive in-office treatments — corticosteroid injections, ultrasound-guided sclerosing alcohol injections, and cryotherapy — can achieve resolution in an additional 10–15% of cases, avoiding surgery entirely. Neurectomy (surgical removal of the nerve) is effective in 85–95% of surgical candidates, but carries small risks of stump neuroma formation, altered sensation, and scar tissue. I discuss surgery only after 6–12 months of supervised conservative treatment has been exhausted and the patient’s quality of life remains significantly impaired.
⚠️ When Metatarsal Pads Are Not Enough: Red Flags to Watch For
Metatarsal pads and orthotics are effective for mild to moderate Morton’s neuroma, but certain symptoms indicate that you need a professional evaluation rather than continued self-management:
- Constant pain at rest — Morton’s neuroma typically hurts with weight-bearing; resting pain suggests a different diagnosis
- Visible swelling or skin discoloration — may indicate a fracture, ganglion cyst, or inflammatory arthritis
- Numbness spreading beyond the toes — could signal peripheral neuropathy or a lumbar nerve root problem
- Worsening pain despite 6–8 weeks of pad use — time for corticosteroid injection or further workup
- A palpable lump between the metatarsals — must be evaluated to rule out ganglion, lipoma, or other soft-tissue mass
- Symptoms in a child or teenager — Morton’s neuroma is rare in this age group; Freiberg’s disease or other conditions are more likely
Call Balance Foot & Ankle Specialists in Howell, Michigan at (517) 315-2300 or use our online contact form if any of these red flags apply to your situation.
Step-by-Step Guide to Fitting Your Morton’s Neuroma Pad
Getting the pad in the right place is more important than which pad you choose. Follow this clinical fitting protocol — the same steps I walk through with every new neuroma patient in my Howell, Michigan office.
Step 1: Locate the Painful Interspace
Stand barefoot on a hard floor. Press firmly upward between your metatarsal heads with your thumb while squeezing the foot gently from the sides with your other hand. You should feel a click or reproduce your familiar burning sensation in the third interspace (between the third and fourth toes) or the second interspace (between the second and third toes). This is called the Mulder sign, and it confirms the neuroma location. Mark the skin at that spot with a washable marker.
Step 2: Measure and Trim the Pad (If Needed)
Pre-cut adhesive pads like the HAPAD generally fit most adult feet without trimming. If the pad extends past the fourth metatarsal head toward the fifth toe, trim the outer edge with scissors. The pad should span from approximately the first to the fourth metatarsal shaft, not reaching any of the metatarsal heads at the front. Narrower pads that span only the second through fourth shafts work best for third-interspace neuromas — the most common location.
Step 3: Apply to Sock or Insole (Not Directly to Skin)
I recommend applying adhesive pads to the insole of the shoe rather than directly to the skin, particularly for initial fitting. Apply the pad with the raised dome facing upward, positioned so the front edge of the pad sits approximately 0.5–1 cm behind the row of metatarsal heads. Put the shoe on, walk around the room for 5 minutes, then take the shoe off and look at the skin impression left by the pad. The impression should be proximal to (behind) the callus pattern, not on top of it. If the pad is leaving a mark directly under the ball of the foot where the callus is, slide it backward 5 mm and reassess.
Step 4: Test for Mulder Sign Relief
After walking 10–15 minutes with the pad in place, repeat the Mulder sign test. Press upward in the painful interspace while squeezing the foot laterally. If the pad is correctly positioned, the click and burning sensation should be significantly reduced or absent. If pain is the same or worse, the pad is either too far forward (pressing on the nerve from below) or too far lateral (missing the interspace). Reposition accordingly. Most patients need 2–3 tries on day one before landing on the exact position.
Step 5: Break In Gradually
Start with 2–4 hours of pad use on day one, then add 1–2 hours each subsequent day. The metatarsals need time to adapt to the new elevation pattern. Some patients experience mild soreness in the arch or the top of the foot during the first week — this is normal and reflects the metatarsal bones shifting to their proper anatomical spacing. Sharp pain, increased burning, or spreading numbness are not normal and signal that the pad needs to be repositioned or that a clinical evaluation is warranted.
Step 6: Pair With the Right Shoes
Metatarsal pads perform best in shoes with adequate toe box width and depth. A shoe that squeezes the toes together will compress the metatarsal heads even with a pad in place, negating its benefit. For patients with active Morton’s neuroma, I recommend shoes with a toe box that is at least 1 cm wider than your broadest toe, a heel height no greater than 1.5 inches, and a removable insole (so you can substitute your pad or custom orthotic). Brands commonly recommended by podiatrists include Altra, New Balance (wide-width models), Hoka, Brooks, and Vionic — all of which offer adequate forefoot space for metatarsal decompression.
Complementary Treatments to Use Alongside Your Pad
Metatarsal pads work best as part of a comprehensive conservative management strategy. The following adjunctive measures dramatically improve outcomes when used consistently alongside your insole or pad.
Ice massage: Fill a paper cup with water and freeze it. Peel back the top inch of paper and use the ice cylinder to massage the plantar forefoot in slow circles for 8–10 minutes after activity. Ice reduces perineural inflammation and temporarily decreases nerve conduction velocity, providing relief during flare-ups. Do not apply ice directly to bare skin for more than 10 minutes at a time.
Intrinsic foot strengthening: Weakness in the intrinsic foot muscles — the small muscles that control toe splay and metatarsal alignment — allows the metatarsal heads to collapse together with each step. Toe-spreading exercises, towel scrunches, and single-leg balance drills performed barefoot for 10 minutes daily rebuild the muscular framework that naturally protects the interdigital nerves. I give every neuroma patient a handout with these exercises, and the patients who do them consistently tend to recover faster and have fewer recurrences.
Anti-inflammatory measures: Short-term use of NSAIDs (ibuprofen or naproxen) during flare-ups can reduce perineural swelling, but long-term daily NSAID use is not appropriate as a primary management strategy and carries gastrointestinal and cardiovascular risks. Discuss the appropriate duration and dosing with your physician or podiatrist. Topical NSAIDs (diclofenac gel) applied to the forefoot can provide local anti-inflammatory benefit with minimal systemic absorption.
Activity modification: During the acute phase, reduce activities that involve prolonged forefoot loading — running, jumping, dancing, standing on hard surfaces for more than 2 hours. Swimming and cycling are excellent low-impact aerobic alternatives that do not compress the forefoot. Return to impact activities gradually as symptoms improve, always wearing properly fitted shoes with your metatarsal pad in place.
When to See a Podiatrist for Morton’s Neuroma
Conservative self-care with metatarsal pads, shoe modification, and activity adjustment successfully manages the majority of Morton’s neuroma cases. But there are clinical thresholds where over-the-counter products are no longer sufficient and professional evaluation becomes necessary.
At Balance Foot & Ankle Specialists in Howell, Michigan, Dr. Tom Biernacki offers the full spectrum of Morton’s neuroma management — from non-invasive footwear counseling and custom orthotics, to ultrasound-guided corticosteroid injections, sclerosing alcohol therapy, cryotherapy, and, for refractory cases, surgical neurectomy with same-day discharge. Our clinic serves patients throughout Livingston County and surrounding communities who want expert foot care delivered by a board-qualified podiatrist with over 3,000 surgical procedures completed.
Call our office at (517) 315-2300 to schedule a Morton’s neuroma evaluation. We offer on-site digital X-ray and in-clinic diagnostic ultrasound so you can receive an accurate diagnosis and personalized treatment plan at your very first visit.
Related Foot Health Resources
Continue reading to learn more about conditions related to forefoot pain and podiatrist-recommended products:
- Morton’s Neuroma: Complete Condition Guide from Dr. Tom
- Best Plantar Fasciitis Insoles 2026: Podiatrist Guide
- Podiatrist-Recommended Orthotics 2026: Dr. Tom’s Top 10
- Best Shoes for Bunions 2026: Podiatrist Guide
- Metatarsalgia: Causes, Symptoms & Treatment Guide
- Schedule an Appointment at Balance Foot & Ankle
Still Struggling with Ball-of-Foot Pain?
Over-the-counter metatarsal pads are an excellent first step, but chronic or severe Morton’s neuroma often requires a personalized treatment plan. Dr. Tom Biernacki, DPM, sees neuroma patients at our Howell, Michigan clinic and can determine whether you need custom orthotics, an injection, or a different diagnosis entirely.
📍 Balance Foot & Ankle Specialists
Howell, Michigan | Serving Livingston County & Surrounding Areas
📞 (517) 315-2300
Differential Diagnosis: What Else Could It Be?
Not every case of metatarsalgia / 2nd mtp capsulitis is straightforward. In our clinic we routinely rule out three look-alike conditions before confirming the diagnosis. If your symptoms don’t match the classic presentation, one of these may explain the pain — which is why physical exam matters more than self-diagnosis.
| Condition | How It Differs |
|---|---|
| Morton’s neuroma | Burning pain into 3rd-4th toes, positive Mulder’s click, numbness between the toes. |
| Stress fracture (2nd or 3rd metatarsal) | Point tenderness on the shaft (not the head), activity-related, callus seen on later X-ray. |
| Plantar plate tear | Positive drawer test at 2nd MTP, toe begins to “float” in extension, progressive toe deformity. |
Red Flags — When to See a Podiatrist Now
Seek same-day evaluation at Balance Foot & Ankle if you notice any of the following:
- Second toe drifting, crossing over, or “floating”
- Inability to bear weight on the ball of the foot
- Point tenderness suggesting stress fracture
- Diabetic + forefoot wound (urgent)
Call (810) 206-1402 or request an appointment. Our Howell and Bloomfield Hills offices reserve same-day slots for urgent foot and ankle issues.
In Our Clinic: What We See
Clinical perspective from Dr. Tom Biernacki, DPM — Balance Foot & Ankle, Howell & Bloomfield Hills, MI:
In our clinic, metatarsalgia patients describe a deep ache under the ball of the foot, often pointed at the 2nd metatarsal head. The pain is worse barefoot or on hard surfaces. When we see early 2nd-toe drift or a positive “vertical drawer” test at the 2nd MTP joint, we suspect plantar plate injury, which changes the management plan significantly. Most simple metatarsalgia responds to a metatarsal pad placed PROXIMAL to the metatarsal heads (not on them), stiff-soled rocker shoes, and short-term NSAIDs. Plantar plate tears may need taping, toe crest pads, or surgical repair.
In-Office Treatment at Balance Foot & Ankle
When conservative care isn’t enough, Dr. Tom Biernacki and the team at Balance Foot & Ankle offer advanced, same-day options — including Morton’s Neuroma Treatment Michigan at our Howell and Bloomfield Hills clinics.
Same-day appointments available. Call (810) 206-1402 or book online.
Watch: Dr. Tom explains
Podiatrist-recommended products
As an Amazon Associate, Dr. Tom earns from qualifying purchases.
Integrated met pad design.
View on Amazon →Place proximal to met heads.
View on Amazon →Forefoot pressure relief.
View on Amazon →Reduces forefoot compression.
View on Amazon →Related resources
Ready to solve this? Book today.
Same-week appointments · Howell & Bloomfield Hills · 4.9★ (1,123+ reviews)
☎ (810) 206-1402Book Online →