Medically reviewed by Dr. Tom Biernacki, DPM · Board-Certified Podiatric Surgeon · Last reviewed: April 2026 · Editorial Policy
Quick Answer
Metatarsalgia Differential Diagnosis: Morton’s Neuroma relates to plantar fasciitis — typically caused by tight calves and arch overload. Most patients improve in 6-12 weeks with conservative care. Same-week appointments in Howell + Bloomfield Twp: (810) 206-1402.
Quick Answer
Morton’s neuroma is a thickening of nerve tissue between the third and fourth toes causing burning pain, numbness, or the sensation of a pebble under the ball of the foot. Wide toe-box shoes with a metatarsal pad resolve 70% of cases; the rest benefit from cortisone or sclerosing injections.
Treatment at Balance Foot & Ankle: EPAT Shockwave for Heel Pain →
Medically Reviewed by Dr. Tom Biernacki, DPM — Board-Certified Podiatrist, Balance Foot & Ankle Specialists, Michigan. Last updated April 2026.
Metatarsalgia — pain localized to the plantar forefoot at or near the metatarsal heads — is a symptom, not a diagnosis, and encompasses at least seven distinct clinical entities, each requiring a specific treatment approach. Accurately differentiating Morton’s neuroma, plantar plate tear, MTP joint synovitis, metatarsal stress fracture, Freiberg’s disease, intermetatarsal bursitis, and sesamoid pathology based on history, physical examination, and targeted imaging prevents the repeated ineffective treatments that characterize misdiagnosed metatarsalgia.
Watch: Dr. Tom Biernacki, DPM
Clinical Differentiation of Common Causes
Morton’s neuroma: burning, electric, or shooting pain radiating into the toes (classic third web space, between 3rd and 4th metatarsal heads); Mulder’s click — a palpable and audible click with lateral compression of the metatarsals combined with direct web space pressure; pain with narrow shoes that resolves with shoe removal; no joint swelling or positive drawer test; MRI confirms an ovoid lesion >5mm in the web space. Plantar plate tear (second MTP instability): plantar pain at the second metatarsal head; positive drawer test (dorsal subluxation of the proximal phalanx on the metatarsal head with 2mm dorsal translation); second toe ‘V sign’ (medial deviation); history of progressive toe deviation rather than shoe-related symptoms; MRI confirms the tear. MTP joint synovitis: diffuse dorsal and plantar joint swelling; pain with passive MTP joint dorsiflexion AND plantarflexion; no specific shoe-type correlation; synovitis secondary to inflammatory arthropathy (RA, psoriatic, gout) — ESR, CRP, urate level; MRI shows synovial thickening and joint effusion. Metatarsal stress fracture: dorsal metatarsal shaft tenderness (not plantar head pain); focal tenderness with axial compression along the metatarsal; history of increased walking/running; MRI confirms bone marrow edema along the shaft; first and fifth metatarsal stress fractures require more aggressive management than central shaft fractures. Freiberg’s infraction: second or third MTP joint pain; younger patients (adolescent females most common); X-ray shows flattening and sclerosis of the metatarsal head; MRI shows osteonecrosis and subchondral collapse.
Systematic Examination Protocol
The examination protocol for metatarsalgia should include: (1) plantar palpation of each metatarsal head individually to localize the pain; (2) web space palpation for neuroma; (3) Mulder’s test; (4) drawer test at each MTP joint; (5) axial compression of each metatarsal shaft; (6) passive MTP joint range of motion; (7) V sign assessment for lateral toe deviation. Imaging algorithm: weight-bearing AP foot X-ray first (stress fracture, Freiberg’s, joint space); MRI for soft tissue differentiation (neuroma vs. plantar plate vs. synovitis) when examination is unclear. Targeted injection: fluoroscopic or ultrasound-guided injection of 1% lidocaine into the suspected structure (web space vs. MTP joint) provides diagnostic confirmation. Dr. Biernacki at Balance Foot & Ankle performs comprehensive forefoot examination and provides targeted treatment for all causes of metatarsalgia at our Bloomfield Hills and Howell offices. Call (810) 206-1402.
📧 Get Dr. Tom’s Free Lab Test Guide
Discover the 5 lab tests every person over 35 should ask their doctor about — explained in plain English by a board-certified physician.
📍 Located in Michigan?
Our board-certified podiatrists treat this condition at two convenient locations. Same-day appointments often available.
More Podiatrist-Recommended Neuroma Essentials
Wide Neutral Cushion Shoe
New Balance 1080 V14 — max forefoot room decompresses the pinched nerve.
Wide-Toe-Box Walking Shoe
New Balance 990v6 — prevents the forefoot compression that triggers Morton’s neuroma.
Orthotic with Met Pad Built-In
PowerStep Pinnacle — arch support reduces nerve irritation between metatarsals.
As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. Product recommendations are based on clinical experience; prices and availability shown above update live from Amazon.
When to See a Podiatrist
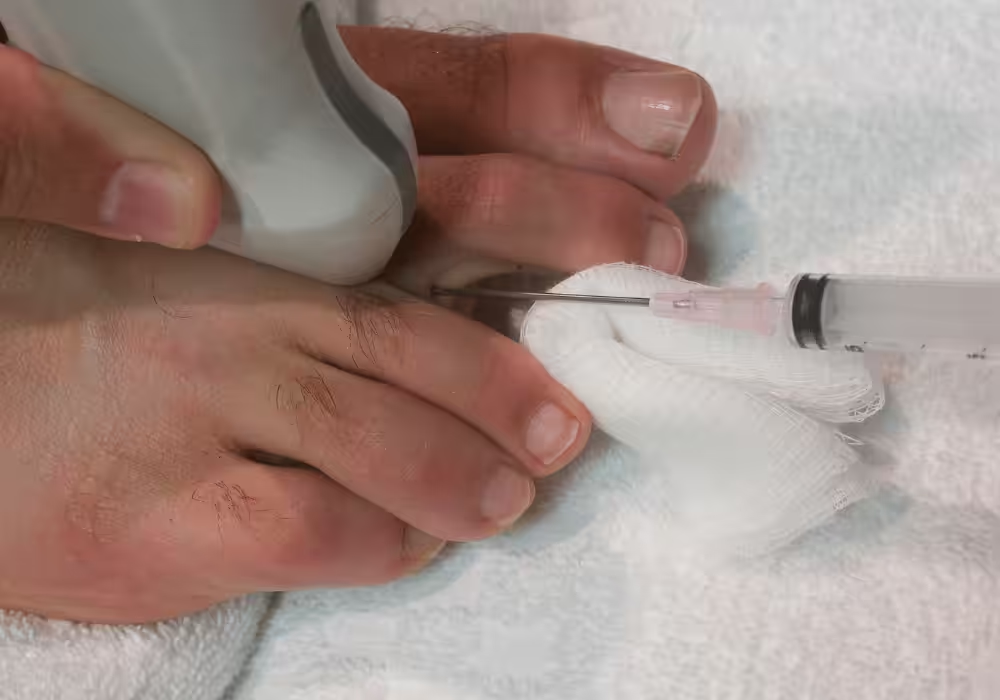
A Morton’s neuroma that doesn’t respond to metatarsal pads and wider shoes within 6-8 weeks usually needs a cortisone injection or — for stubborn cases — alcohol sclerosing or nerve decompression. Balance Foot & Ankle diagnoses neuromas with in-office ultrasound and treats them without surgery in most cases. Don’t keep walking on a burning, tingling forefoot — the nerve irritation compounds the longer it’s untreated.
Call Balance Foot & Ankle: (810) 206-1402 · Book online · Offices in Howell & Bloomfield Hills
Frequently Asked Questions
How long does a foot stress fracture take to heal?
Most foot stress fractures heal within 6–8 weeks with proper offloading. High-risk fractures (Jones fracture, navicular stress fracture) can take 3–6 months and sometimes require surgery. Premature return to activity is the most common cause of delayed healing.
How do I know if I have a stress fracture?
Stress fractures cause localized pain that worsens with activity and improves with rest, often with point tenderness over a specific bone. X-rays may be negative for 2–3 weeks after onset — MRI provides definitive diagnosis earlier.
Can you walk on a stress fracture?
This depends on the fracture location and severity. Many foot stress fractures allow limited walking in a protective boot. High-risk fractures (Jones, navicular) typically require non-weight-bearing. Walking on an unprotected stress fracture risks complete fracture.
Need Treatment at Balance Foot & Ankle?
Dr. Tom Biernacki, Dr. Carl Jay, and Dr. Daria Gutkin see patients at our Howell and Bloomfield Township offices.
Book Online or call (810) 206-1402
Insurance Accepted
BCBS · Medicare · Aetna · Cigna · United Healthcare · HAP · Priority Health · Humana · View All →
Howell Office
3980 E Grand River Ave, Suite 140
Howell, MI 48843
Get Directions →
Bloomfield Hills Office
43700 Woodward Ave, Suite 207
Bloomfield Hills, MI 48302
Get Directions →
Your Board-Certified Podiatrists
Ready to Get Back on Your Feet?
Same-week appointments available at both locations.
Book Your Appointment- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)
Recommended Products from Dr. Tom








