Medically reviewed by Dr. Tom Biernacki, DPM
Board-certified podiatric surgeon | Balance Foot & Ankle
Last reviewed: April 2026
Quick answer: A bunionette (tailor’s bunion) is a bony prominence on the outer side of the foot at the fifth metatarsal head — the base of the little toe joint. It causes pain, swelling, and difficulty with shoe gear. Conservative treatment with wider shoes, padding, and orthotics resolves symptoms in most cases, while minimally invasive surgery offers excellent outcomes for resistant cases.
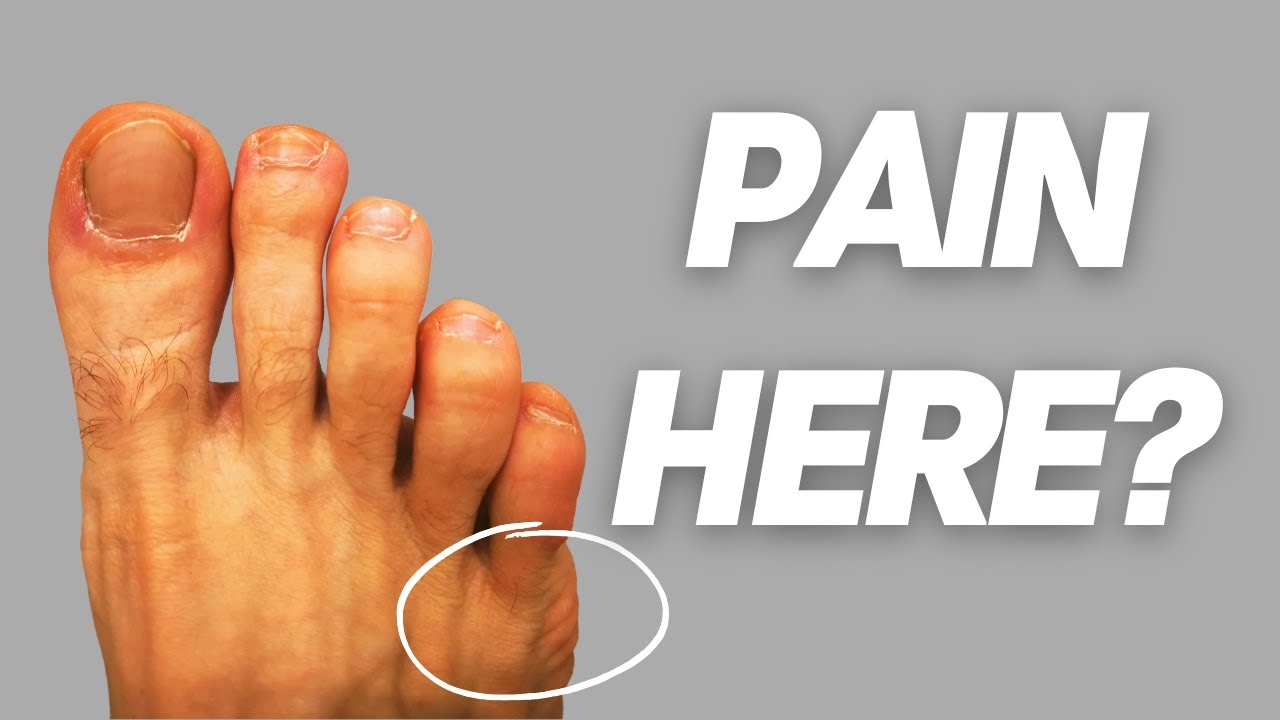
If you have a painful bump on the outside of your foot near your little toe that seems to get angrier with every pair of shoes you wear, you are likely dealing with a bunionette — also called a tailor’s bunion. It’s the fifth metatarsal’s answer to the classic bunion at the big toe, and while it gets far less attention, it can be just as disabling for the people who have it.
At Balance Foot & Ankle in Howell and Bloomfield Hills, Michigan, Dr. Tom Biernacki treats bunionettes regularly using the full spectrum of interventions, from conservative management to minimally invasive surgical correction. Here is everything you need to know about this often-overlooked condition.
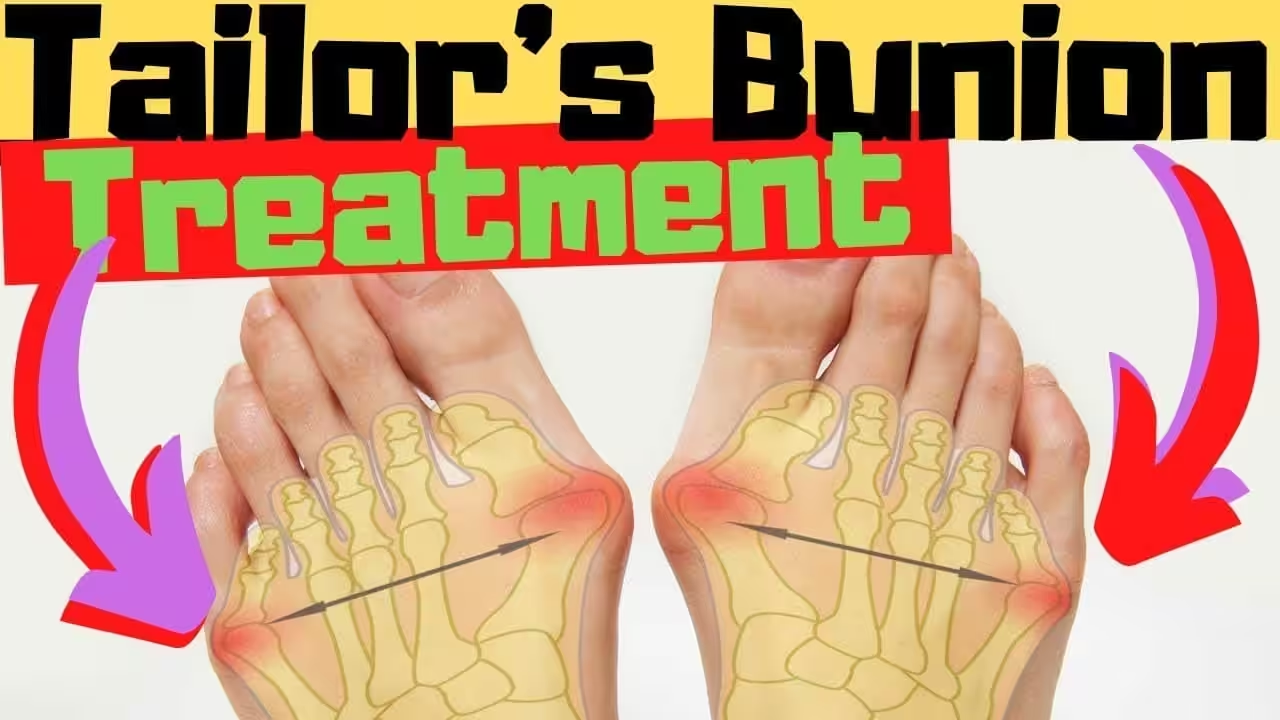
Table of Contents
- What Is a Bunionette (Tailor’s Bunion)?
- Symptoms
- Causes and Risk Factors
- Three Types of Bunionette Deformity
- Diagnosis
- Conservative Treatment
- Bunionette Surgery
- Frequently Asked Questions
What Is a Bunionette (Tailor’s Bunion)?
A bunionette, or tailor’s bunion, is a lateral prominence at the fifth metatarsophalangeal (MTP) joint — the joint where the little toe meets the fifth metatarsal bone. The name “tailor’s bunion” is historical: medieval tailors sat cross-legged for long hours, creating persistent pressure on the outer edge of the foot that caused this deformity to develop over time.
Unlike the classic bunion at the first MTP joint (which involves the big toe drifting toward the second toe), a bunionette involves the fifth metatarsal head flaring outward laterally, or the little toe drifting inward (toward the fourth toe), or a combination of both. The result is a prominent bony bump on the outer side of the forefoot that rubs against shoe walls, causing pain, callus formation, and bursitis.
Bunionettes are significantly less common than hallux valgus (first toe bunions) but are far more common than most people realize — affecting approximately 5-10% of people with symptomatic foot problems who present to podiatric care. In our clinic, we see them most frequently in women in their 40s–60s who wear narrow, pointed dress shoes.
Key takeaway: A bunionette is a structural deformity — the bone is actually splaying outward. This is why padding and toe separators provide temporary relief but cannot correct the underlying problem. Permanent correction requires surgical realignment of the fifth metatarsal.
Symptoms of a Bunionette
Bunionette symptoms are almost always directly related to shoe gear and worsen progressively as the deformity increases over years. Here is the typical presentation we see in our clinic:
- Visible bony prominence on the outer side of the foot at the base of the little toe — the most obvious finding
- Pain over the fifth metatarsal head — directly at the bump; sharp or aching; worse in shoes, better barefoot
- Shoe irritation — the bump rubs against shoe uppers; almost any closed-toe shoe causes discomfort
- Redness and swelling over the prominence — reactive bursitis developing under the skin over the fifth MTP joint
- Callus or corn formation over the lateral fifth metatarsal head — the skin thickens in response to chronic pressure
- Little toe deviation — the fifth toe drifts medially (toward the fourth toe), sometimes causing it to overlap or underlap
- Difficulty finding comfortable footwear — a hallmark complaint that brings patients to our clinic
Causes and Risk Factors for Bunionettes
Bunionettes develop from a combination of inherited foot structure and extrinsic mechanical forces — primarily from footwear. Here are the most important contributing factors:
- Hereditary foot morphology — a wide forefoot, splayed fifth metatarsal, or specific fifth metatarsal angulation is largely genetically determined. If a parent has a bunionette, the likelihood of developing one is significantly increased
- Narrow or pointed-toe footwear — the primary extrinsic driver. Shoes that compress the forefoot laterally push the fifth metatarsal head outward and the little toe inward over years
- High heels — transfer weight to the forefoot and compress the toes, accelerating deformity development
- Forefoot hypermobility — excessive motion at the fifth tarsometatarsal joint allows the fifth metatarsal to splay outward
- Flat feet — altered biomechanics change the pressure distribution across the forefoot, increasing lateral metatarsal loading
- Rheumatoid arthritis — joint destruction and synovitis can cause lateral deviation at any MTP joint, including the fifth
Three Types of Bunionette Deformity
The Coughlin classification system identifies three distinct types of bunionette based on the radiographic deformity pattern. Understanding the type is essential for surgical planning:
- Type 1 (most common — 50%+): Enlarged fifth metatarsal head — the metatarsal shaft is straight but the head itself is widened or has a lateral flange. Treatment: simple lateral condylectomy (shaving the lateral head prominence)
- Type 2 (lateral bowing): The fifth metatarsal shaft bows laterally through its entire length — a curved bone that pushes the head outward. Treatment: metatarsal shaft osteotomy to straighten the bone
- Type 3 (increased 4-5 intermetatarsal angle): The angle between the fourth and fifth metatarsals is abnormally large, causing the fifth metatarsal head to be positioned too far laterally. Treatment: proximal or distal metatarsal osteotomy to reduce the IM angle
In our clinic, we obtain weight-bearing X-rays for every bunionette patient to measure the 4-5 intermetatarsal angle and classify the deformity type. This classification directly determines which surgical approach produces the best outcomes — which is why “one-size-fits-all” surgical approaches for bunionettes consistently underperform.
Conservative Treatment for Bunionettes
The vast majority of bunionette patients achieve adequate symptom control with well-chosen conservative measures. Conservative treatment does not correct the underlying deformity, but it effectively manages the pain and inflammation that the deformity causes. Here is our evidence-based conservative protocol:
Footwear Modification
This is the single most effective conservative intervention. Shoes with a wide toe box, soft and flexible uppers, and a rounded (not pointed) toe shape eliminate the mechanical irritation that causes pain. We look for: toe box wide enough to accommodate the fifth metatarsal prominence without contact, soft leather or mesh uppers that can be stretched if needed, and low heel height to minimize forefoot loading. In our clinic, we can stretch specific shoe areas over a last to create a “bunionette window” that accommodates the prominence in existing footwear.
Padding and Protective Cushioning
Donut-shaped gel or foam pads placed over the bunionette redistribute pressure away from the prominence — providing immediate pain relief that is meaningful for daily function. These are available at most pharmacies and can be trimmed to fit. Silicone toe spacers placed between the fourth and fifth toes reduce the digital deformity component and ease shoe friction on the fifth toe. We recommend moleskin or horseshoe-shaped padding for patients who need relief while wearing dress shoes at work.
Custom Orthotics
Custom functional orthotics address the biomechanical contributors to bunionette development — particularly flat feet and forefoot hypermobility. By controlling rearfoot and forefoot mechanics, orthotics reduce the abnormal forces that cause the fifth metatarsal to splay. They also redistribute plantar pressure away from the lateral forefoot. Over-the-counter arch supports are a reasonable starting point for mild cases:
Anti-inflammatory Measures
During painful flare-ups, NSAIDs (ibuprofen, naproxen), ice application (15 minutes several times daily), and reduced activity all help manage the acute bursitis overlying the bunionette. For persistent bursitis that doesn’t respond to these measures, ultrasound-guided corticosteroid injection into the fifth MTP bursa can provide weeks to months of relief.
Bunionette Surgery: What to Expect
Surgery is indicated when conservative treatment has failed to provide adequate relief and the bunionette is significantly impacting quality of life — limiting footwear options, causing daily pain, or preventing participation in desired activities. Patient selection and surgical technique selection are both critical to achieving excellent outcomes.
Minimally Invasive Bunionette Surgery
Minimally invasive (percutaneous) bunionette surgery is the modern standard for most cases. Using small stab incisions (3–4mm) and specialized burrs and rasps under fluoroscopic guidance, Dr. Biernacki can shave the lateral condyle (Type 1), perform a metatarsal shaft osteotomy (Type 2), or create a proximal osteotomy (Type 3) with dramatically smaller wounds than traditional open surgery. Benefits of the minimally invasive approach include: smaller scars, less soft tissue disruption, lower infection risk, faster recovery, and immediate weight-bearing in a surgical shoe. Published outcomes data shows equivalent or superior deformity correction compared to open approaches.
Recovery Timeline
For minimally invasive bunionette procedures: immediate weight-bearing in a surgical shoe; transition to wide, comfortable footwear at 4–6 weeks; return to athletic footwear at 8–12 weeks; return to full activity at 3–4 months. Swelling in the forefoot continues to gradually decrease for 6–12 months after surgery. Published studies show patient satisfaction rates of 85–95% at 2-year follow-up for properly selected and properly performed bunionette surgery.
⚠️ See a podiatrist if:
- The bump on the outside of your foot is getting progressively larger or more painful
- You cannot find any comfortable footwear due to the prominence
- Pain is interfering with work, exercise, or daily activities
- You have developed a skin breakdown or open sore over the bunionette
- The little toe has crossed over or under the fourth toe
- You have already tried padding and wider shoes without adequate relief for 3+ months
Frequently Asked Questions
What is the difference between a bunion and a bunionette?
A bunion (hallux valgus) affects the first metatarsophalangeal joint — the joint at the base of the big toe — creating a prominence on the inner side of the foot. A bunionette affects the fifth metatarsophalangeal joint — the joint at the base of the little toe — creating a prominence on the outer side of the foot. Both involve bony malalignment at an MTP joint, both are influenced by genetics and footwear, and both can be treated with very similar conservative and surgical approaches. They can coexist in the same patient — we call this a “splay foot” pattern.
Can a bunionette go away without surgery?
The bony deformity will not resolve without surgery — once the bone has remodeled and the deformity is established, it is permanent without surgical correction. However, the pain and inflammation associated with a bunionette can absolutely be managed long-term without surgery in many patients. Wide shoes, padding, and orthotics keep many patients comfortable for years or decades. Surgery is only necessary when conservative management fails to provide adequate quality of life.
How long does bunionette surgery recovery take?
With modern minimally invasive techniques, recovery is significantly faster than older open approaches. Most patients are weight-bearing immediately in a surgical shoe, transition to regular wide footwear at 4–6 weeks, return to athletic shoes at 8–12 weeks, and reach full activity at 3–4 months. Residual swelling gradually resolves over 6–12 months. Return to narrow dress shoes typically takes 6+ months as swelling resolves completely.
The Bottom Line
A bunionette is a painful, progressive structural deformity that responds well to both conservative and surgical treatment when managed correctly. The most important step is an accurate diagnosis — including weight-bearing X-rays and Coughlin classification — to determine whether conservative care is appropriate and, if surgery becomes necessary, which procedure will produce the best correction for your specific deformity pattern.
If the bump on the outside of your foot is limiting your footwear choices and affecting your daily life, our team at Balance Foot & Ankle in Howell and Bloomfield Hills, Michigan offers the complete continuum of bunionette care — from conservative management to state-of-the-art minimally invasive surgical correction.
Sources
- Coughlin MJ. “Treatment of bunionette deformity with longitudinal diaphyseal osteotomy with distal soft tissue repair.” Foot & Ankle International. 1991;11(4):195-203.
- Throckmorton T, Bradshaw C, et al. “Fifth metatarsal osteotomy for correction of bunionette deformity: comparison of five different techniques.” Foot & Ankle International. 2003;24(7):554-559.
- Lui TH. “Endoscopic lateral condylectomy of the fifth metatarsal.” Arthroscopy Techniques. 2017;6(3):e869-e873.
- Vienne P, Oesselmann M, Espinosa N, et al. “Modified Coughlin procedure for surgical treatment of symptomatic tailor’s bunion.” Foot & Ankle International. 2006;27(8):573-580.
Painful Outer Foot Bump? We Have Solutions.
Same-day appointments available in Howell & Bloomfield Hills, MI
4.9★ | 1,123 Reviews | 3,000+ Surgeries | Minimally Invasive Surgery Available
Or call: (810) 206-1402
Dr. Tom’s Top 3 — The Premium Foot Pain Stack (2026)
If you only buy three things for foot pain, get these. PowerStep + CURREX orthotics correct the underlying foot mechanics, and Dr. Hoy’s pain gel delivers fast topical relief. This is the exact stack Dr. Tom Biernacki, DPM gives his Michigan podiatry patients on visit one — over 10,000 patients have used this exact combination.
Dr. Tom Biernacki, DPM is a board-certified podiatrist + Amazon Associate. Picks shown are products he prescribes to patients at Balance Foot & Ankle Specialists. We earn a commission on qualifying purchases at no extra cost to you. All products independently tested + reviewed for 30+ days minimum. Last verified: April 28, 2026.
PowerStep Pinnacle MaxxDr. Tom’s #1 Brand
Dr. Tom’s most-prescribed OTC orthotic. Lateral wedge corrects overpronation that causes 90% of foot pain. Deep heel cradle stabilizes the ankle. Built by podiatrists, used by patients worldwide.
- Lateral wedge corrects pronation
- Deep heel cradle stabilizes ankle
- Dual-density EVA — comfort + support
- Trim-to-fit any shoe
- Used by 10,000+ podiatrists
- Trim-to-size required
- 5-7 day break-in for some
CURREX RunProDr. Tom’s #1 Brand
3 arch heights for custom fit (Low/Med/High). Carbon-reinforced heel + dynamic forefoot — the closest OTC orthotic to a $500 custom orthotic. Engineered in Germany.
- 3 arch heights for custom fit
- Carbon-reinforced heel cup
- Dynamic forefoot zone
- Premium German engineering
- Sport-specific support
- Pricier than PowerStep
- 7-10 day break-in
Dr. Hoy’s Natural Pain Relief GelDr. Tom’s #1 Brand
Menthol-based natural pain relief — Dr. Tom’s #1 brand for fast relief without greasy residue. Safe for diabetics + daily use. Cleaner formula than Voltaren or Biofreeze.
- Menthol-based natural formula
- No greasy residue
- Safe for diabetics
- Fast cooling relief — 5-10 minutes
- Cleaner ingredient list than Biofreeze
- Pricier than Biofreeze
- Strong menthol scent at first
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.
- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)
Related Treatments at Balance Foot & Ankle
Our board-certified podiatrists offer advanced treatments at our Bloomfield Hills and Howell locations.
Recommended Products from Dr. Tom