Calcaneus Foot Pain
Causes, Symptoms & Best Treatment!
Say Goodbye to Painful Calcaneus Foot Pain
Calcaneus foot pain can cause severe discomfort and limit your daily activities, but the good news is there are effective solutions available. In this treatment guide, you’ll discover the 100% best way to get rid of calcaneus foot pain, with practical steps and proven methods to help you find lasting relief and get back on your feet with confidence.
Schedule Your Consultation Today
Calcaneus Stress Fracture Foot Pain Treatment Video
Calcaneus Heel Pain Causes
Most Common Calcaneus Heel Pain Causes:
The number one source of heel pain is plantar fasciitis. This is most likely felt at the bottom of the heel.
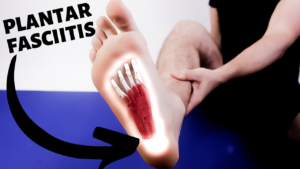
The second most common cause of heel pain is Achilles tendinitis insertional pain, this is felt most commonly at the back of the heel.
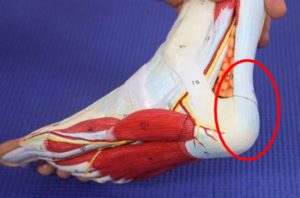
A calcaneal stress fracture is also very common, and this is most common when you squeeze the bone from side to side and there is radiating pain.

- These are three less common heel pain causes, but nonetheless they should be taken seriously!
- The treatment guide is included below.
Less common causes:
- Below are included the next most common causes of calcaneal heel pain.
- We strongly recommend looking at the three links above as these are the three most common causes.
- Nonetheless all six common causes are well treated by the guide below.
1. Calcaneus Pain due to Nerve Pain:
What to look for:
- Radiation of pain.
- Sensory problems.
- Numbness, burning or tingling.
- Pain is worst at night.
Overview:
- Neurologic heel pain is usually due to an irritated or an entrapped nerve through a region that is prone to constriction and tightness such as the ankle joint or in the back where the nerve exits the spine. This type of pain may easily mimic plantar fasciitis (painful bottom of the heel) or back of the heel pain (Achilles tendinopathy) or inside of the ankle pain.
- This type of pain usually manifests itself as numbness, tingling or burning pain rather than the aching sore pain that is experienced with muscle soreness.
- The type of nerve pain originating around the ankle joint is referred to as tarsal tunnel syndrome which is essential the equivalent of carpal tunnel syndrome that is found in the wrist.
- Nerve pain can also occur much earlier and closer to the spine and can be associated with back pain or injury. If you have recently injured your back or have had back pain, a slipped disc or anything like that, then you should suspect what is known as radiculopathy (nerve pain originating from the nerve root in the spine)
- It is also possible to have the nerve irritated in both the back and in the ankle.
- Nerves may also be irritated due to obesity, venous problems (swollen varicose veins), trauma, and space occupying masses.
- Nerve pain can also occur due to systemic disease such as diabetes, nutritional or vitamin deficiencies or alcoholism.
- Tests for neurologic nerve pain include electromyography, nerve conduction velocity, MRI and pressure specified sensory device testing which can be done by your podiatrist.
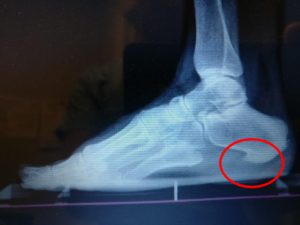
Nerve Pain Treatment:
- Release of the nerve entrapment either at the back or around the ankle and plantar fascia.
- Nerve release of the tarsal tunnel to prevent tarsal tunnel syndrome.
- Medical treatment of peripheral neuropathy through medications.
2. Inflammatory Arthritis Calcaneus Pain:
What to look for:
- History of being diagnosed with arthritis.
- Many other joints are painful and swollen.
- Obvious previous joint pain.
Overview:
- Almost all cases of heel pain are at least partially mechanically related and will respond to the following recommended therapy, even if inflammatory arthritis is present, but it is good know if any additional modifications can be made to the treatment regimen.
- Keep in mind the possibility of:
- Serognegative arthritides like psoriatic arthritis, ankylosing spondylitis, Reiter’s disease, diffuse idiopathic skeletal hyperostosis, rheumatoid arthritis, fibromyalgia and previous cases of gout.
- Evaluation for these arthritides would require x-ray and laboratory testing by your podiatrist.
Inflammatory Arthritis Treatment:
-Consult with a rheumatological specialist
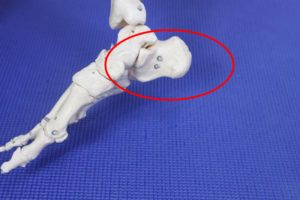
3. Traumatic Calcaneus Pain:
What to look for:
- History of trauma
- Severe pain with compression
- Pain that gets worse with activity
- Rather than better with activity
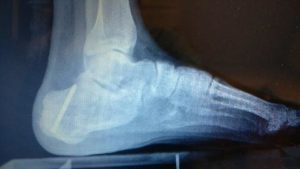
Overview:
- While biomechanical damage over time is the most common form of soft tissue injury to the plantar fascia and the Achilles tendon around the heel, a traumatic injury to the heel bone itself is the most common cause of a bone injury in the heel region.
- The main thing is recognizing that a high impact fall can translate into the ankle or the mid-foot as spread out pain that is not localized, or it could even have injured your back and compressed nerves that are leading down to your foot and ankle.
- It is important to diagnose this type of pain because over time as you think that it will get better, the small little fragments will develop into arthritis and inhibit joint motion permanently.
Traumatic Calcaneus Pain Treatment.
- Get it diagnosed properly with history and X-rays
- Immobilization will likely be needed to prevent the development of arthritis
- Surgery may be necessary to excise broken bone fragments or re-attach pieces if they are large enough or serious enough
Consult Balance Foot & Ankle Specialist in Howell and Bloomfield.
Our skilled podiatric surgeons use advanced techniques, precision, and compassionate care to successfully treat calcaneus foot pain. With state-of-the-art facilities, personalized patient education, and innovative treatment options, Balance Foot & Ankle Specialist has become a trusted choice for foot and ankle care in Southeast Michigan. Our commitment is to relieve your pain, restore function, and help you walk comfortably and confidently again.
Book Your Podiatrist Visit Now

Frequently Asked Questions About Calcaneus (Heel Bone) Foot Pain
Calcaneus foot pain refers to discomfort or aching in the heel bone, often caused by overuse, injury, or conditions like plantar fasciitis or heel spurs.
What causes pain in the calcaneus bone?
Common causes include plantar fasciitis, Achilles tendonitis, heel spurs, fractures, and bursitis.
How do I know if I have a calcaneus fracture?
Symptoms of a calcaneus fracture include sudden heel pain after trauma, swelling, bruising, and difficulty bearing weight.
Is heel pain worse in the morning a sign of something serious?
Yes, if your heel pain is worst when you first step out of bed, it may be a sign of plantar fasciitis or another inflammatory condition.
How is calcaneus pain treated?
Treatment options may include rest, ice, stretching, orthotics, anti-inflammatory medications, physical therapy, and in severe cases, surgery.
When should I see a podiatrist for heel pain?
If heel pain lasts more than a few days, worsens, or interferes with walking, it’s important to see a podiatrist for proper diagnosis and treatment.
Related Treatment Guides
- Plantar Fasciitis & Heel Pain Treatment
- Custom 3D Orthotics
- Sports Foot & Ankle Injury Treatment
- Bunion Treatment
Dr. Tom Biernacki, DPM is a board-qualified podiatrist and foot & ankle surgeon serving Southeast Michigan at Balance Foot & Ankle Specialists. A Michigan native, Dr. Biernacki earned his undergraduate degree from Michigan State University and his Doctor of Podiatric Medicine (DPM) from Kent State University College of Podiatric Medicine. He completed a three-year comprehensive surgical residency in foot and ankle surgery in the Detroit metro area.
Dr. Biernacki specializes in the treatment of heel pain, bunions, hammertoes, diabetic foot care, sports injuries, flatfoot correction, and minimally invasive foot surgery. He is dedicated to providing evidence-based, patient-centered care that helps people of all ages stay active and pain-free.
He sees patients at multiple convenient Metro Detroit locations and is committed to community education through the MichiganFootDoctors.com resource library. Dr. Biernacki is a member of the American Podiatric Medical Association (APMA) and the Michigan Podiatric Medical Association (MPMA).