Achilles Tendinitis Surgery [BEST Recovery Time & Treatment]
Are you looking at Achilles Tendinitis Surgery? The average recovery time can be 6-8 weeks or more! We go over the FASTEST recovery time & best treatment.
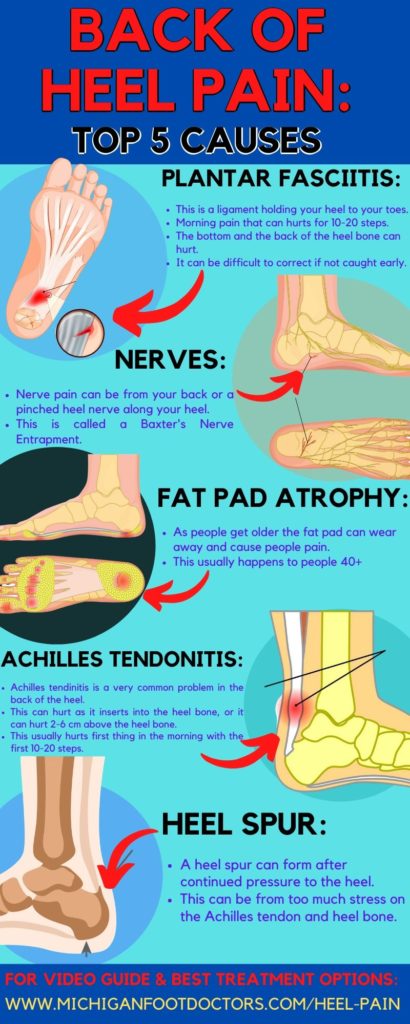
Table of Contents
Achilles Tendon & Back of Heel Pain
Back of the Heel Pain Causes:
Back of the heel pain is most commonly caused by the Achilles tendon and back of the calcaneus damage.
The most common causes of back heel pain are:
- Fat pad atrophy can lead to calcaneus bone pain.
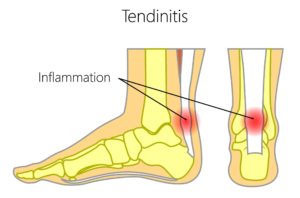
- Insertional Achilles tendinitis pain.
- Achilles tendinitis 2-6 cm above the heel bone.
- An Achilles tendon strain or rupture.
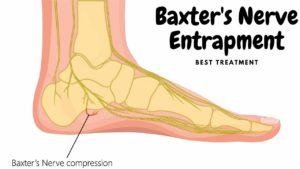
- Nerve impingement or entrapment in the heel.
- Achilles tendinosis.
- Back of the heel spur pain.
- Achilles tendon bursitis.
- Plantar fasciitis.
Achilles Tendonitis Symptoms:
- Achilles tendonitis symptoms can be a pain in the morning when you first wake up.
- Pain when trying to bend the foot up as the Achilles tendon inserts into the back of the heel.
- Worsening inflammation and tenderness while standing and walking for long periods of time.
- Improvement when wearing good shoes, good orthotics, and supportive sandals.
Make sure it is Achilles Tendinitis!
- That you have tried conservative therapy for 2-3 months before you even begin to consider surgery. Surgery comes with a great amount of risks and should not be attempted until conservative therapy is exhausted.
- Make sure that what you have been treating this entire time is actually Achilles tendinitis and not any other type of heel pain. If you are experiencing a sharp pain during your calf then you should consider following the guide for sharp pain in your Achilles Tendon.
Other possible problems are:
1) Plantar fasciitis:

2) Calcaneal stress fracture:

3) “Bump” on the back of the heel:
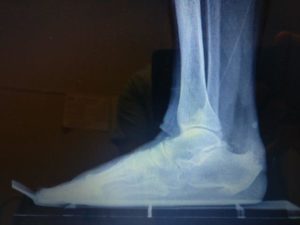
4)Re-Consider Neurologic heel Pain, Inflammatory Arthritis, Tumors or any other causes:
Surgical Treatment
- If the case of achilles tendinitis is so resistant that the first two stages of treatment were ineffective, then you should likely go seek assistance from an experienced foot and ankle surgeon. We usually find that these cases include calcification of the tendon and spurring of the back of the heel and well into the Achilles tendon.
- The surgical procedure would have to include detaching the Achilles tendon from the calcaneus, smoothing out the bone, smoothing out or resecting the calcified tissue and re-attaching the Achilles tendon to the calcaneal bone with bone and suture anchors.
- The patient will also be evaluated for gastrocnemius or tendo-achilles lengthening to ensure proper length of the Achilles tendon and if they have equinus present (improper ankle motion which likely contributed or causes the Achilles problems in the first place)
- Extracorporeal shock-wave therapy can also be tried to stimulated blood vessel growth, decrease nerve pain and attempt to break up the calcification through a “vibrations”
- Radiofrequency coblation can also be attempted to increase blood vessel proliferation.
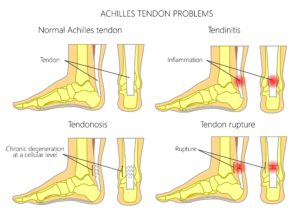
Surgical Options:
- Resection or insertional Spurring
- Tendon resection and re-attachment
- Extracorporeal shockwave therapy
- Radiofrequency coblation
Back of the heel pain treatment:
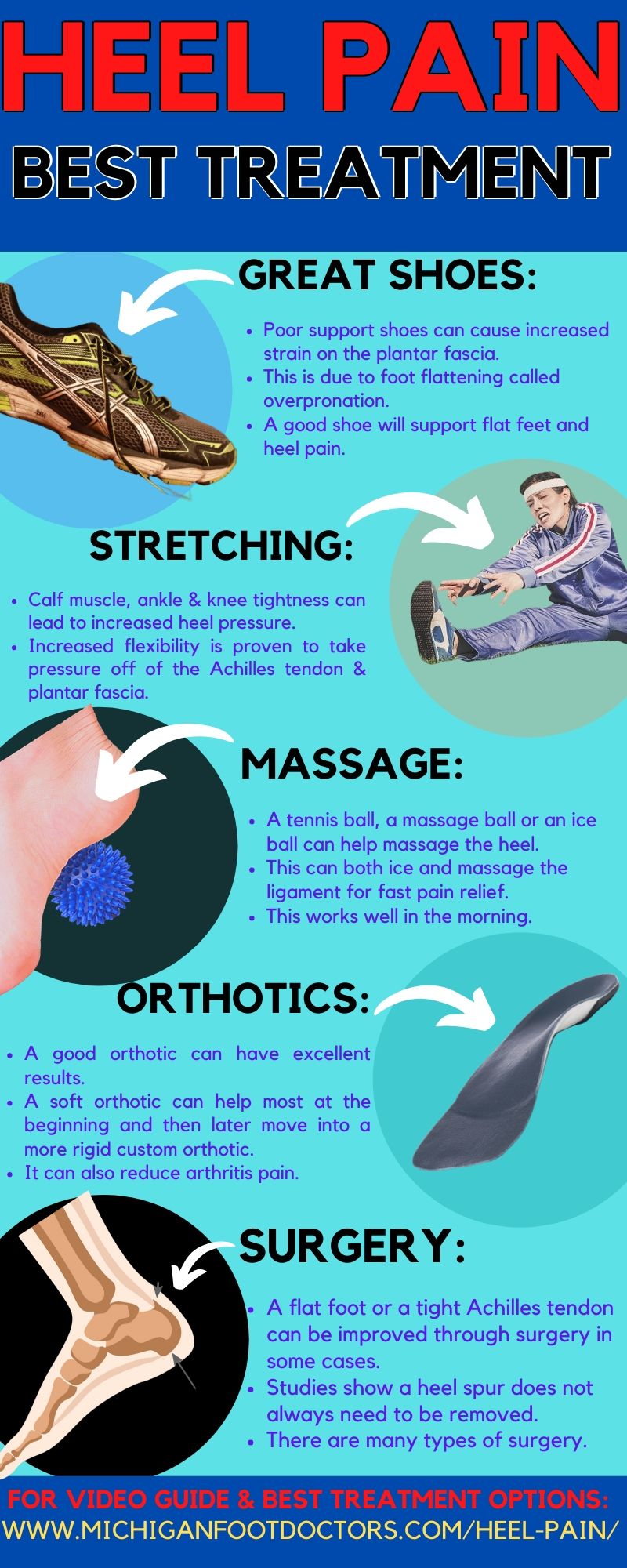
Best Back of Heel Pain Treatment:
- There are usually two phases to treating back of the heel pain.
- The two phases of treatment include controlling the acute inflammation and correcting the biomechanics, which led to the problem in the first place.
- If the tendons and ligaments are inflamed, they are almost frozen in place and cannot function properly.
- Once the inflammation is decreased, we need to correct the biomechanical causes to ensure that the Achilles tendon can never become overworked and inflamed again!
- This doesn’t matter whether it’s The back of the heel spur, fat pad atrophy, insertional Achilles tendinitis, Achilles tendinitis, or even Achilles tendinosis.
- If you do have an Achilles tendon rupture or tear, seeing podiatrist care immediately.
Achilles Tendon Natural Treatment:
Massage & Ice Products:
- Ice is an excellent option that can be safe for almost everyone.
- There is some debate about whether icing is worth doing, but this can help limit the need for medications and keep your options open for chronic pain.
- This works great for your arch, less for the ball of the foot.
- Manual massage on the Achilles tendon & calf muscle is a natural treatment that can also be considered physical therapy for your back of the heel pain.
- This works well for calf muscle pain and Achilles tendon pain.
- The more muscle and ligament tissue there is, the better ice will work there.
Best Foot & Ankle Manual Massage Devices:
Best Premium Massage Roller
Most Cost Effective Massage Roller.
Cost Effective Freezable Massage Roller.



Price:
Price not available
$8.99
$11.99
Overview:
Premium freezable metal ball that stays cold for up to 6 hours. Great for plantar fascia, neck, shoulders and calf muscles.
Amazing Price, Great Reviews – Non-Freezable Massage Rolling Stick
Great price and it is freezable. Budget friendly freezable massage roller.
Pros:
Great reviews – near 5 star. Stays cold for a long time with deep penetrating plantar fascia massage. Used by professional athletes. Stays cold for HOURS!
Great for what it does. You roll it back and forth along your plantar fascia massaging the swelling and irritation out. Decreases pain. Thousands of 5 star reviews on Amazon.
Excellent reviews. It massages and ices, so it is a step up over the massage rollers. Near 5 star reviews with >500 reviews.
Cons:
More expensive than some of the other options, but near perfect reviews.
Is not freezable like the other two options. Massaging a sore muscle without the cold sensation can be very painful and render it useless to you if really sore.
It does a great job doing what it is supposed to do. Main downside is that it does not stay cold as long as the premium metal ball.
Important Tips:
Use it with a sock to start (could be too cold). Massaging and icing definitely loosens you up and makes you feel better, but you still have to prevent the pain in the first place. You still need stretching, orthotics and good shoes to prevent the initial damage.
Two things: Without the freezing component, it may be really painful for a very sore arch (So make sure to use ICE also). Also this only reduces pain, it does not stop the cause! You still need good orthotics, shoes and stretching to stop the pain in the first place!
Start with socks at first, especially if you have peripheral neuropathy => don’t freeze your foot! Remember that you still need good orthotics, good shoes and inserts as well as temporary activity reduction.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Manual Massage Devices:
Best Premium Massage Roller

Price:
Price not available
Overview:
Premium freezable metal ball that stays cold for up to 6 hours. Great for plantar fascia, neck, shoulders and calf muscles.
Pros:
Great reviews – near 5 star. Stays cold for a long time with deep penetrating plantar fascia massage. Used by professional athletes. Stays cold for HOURS!
Cons:
More expensive than some of the other options, but near perfect reviews.
Important Tips:
Use it with a sock to start (could be too cold). Massaging and icing definitely loosens you up and makes you feel better, but you still have to prevent the pain in the first place. You still need stretching, orthotics and good shoes to prevent the initial damage.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Manual Massage Devices:
Most Cost Effective Massage Roller.

Price:
$8.99
Overview:
Amazing Price, Great Reviews – Non-Freezable Massage Rolling Stick
Pros:
Great for what it does. You roll it back and forth along your plantar fascia massaging the swelling and irritation out. Decreases pain. Thousands of 5 star reviews on Amazon.
Cons:
Is not freezable like the other two options. Massaging a sore muscle without the cold sensation can be very painful and render it useless to you if really sore.
Important Tips:
Two things: Without the freezing component, it may be really painful for a very sore arch (So make sure to use ICE also). Also this only reduces pain, it does not stop the cause! You still need good orthotics, shoes and stretching to stop the pain in the first place!
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Manual Massage Devices:
Cost Effective Freezable Massage Roller.

Price:
$11.99
Overview:
Great price and it is freezable. Budget friendly freezable massage roller.
Pros:
Excellent reviews. It massages and ices, so it is a step up over the massage rollers. Near 5 star reviews with >500 reviews.
Cons:
It does a great job doing what it is supposed to do. Main downside is that it does not stay cold as long as the premium metal ball.
Important Tips:
Start with socks at first, especially if you have peripheral neuropathy => don’t freeze your foot! Remember that you still need good orthotics, good shoes and inserts as well as temporary activity reduction.
Affiliate Link (Buying through these links will connect you to Amazon):
Menthol Based Gels:
- Biofreeze is one of our favorites.
- These gels have been studied to work 2x as long as ice.
- This works great for the ball of the foot.
- This can be very effective for pain relief, but this can decrease inflammation in the calf muscle and Achilles tendon.
Best Foot & Ankle Muscle/Ligament Pain Relief Products
Best & Proven Pain Relieving Gel.
Roll On Version of Biofreeze Gel.
A giant container of value size biofreeze.
Menthol Based Ointment with Hemp Extract




Price:
$34.95
$29.95
$175.00
$19.99
Overview:
The Proven and Scientifically Published Menthol Based Gel
Same as biofreeze gel, but the roll-on is prefered by some people for their feet, less messy.
8.1 lbs(3.67 kg) of Value Sized Biofreeze!
This is an alternative cream: Basically Biofreeze + hemp extract.
Pros:
Scientifically proven to loosen up and relief pain up to 2x longer than Ice. Less effort than ice and great reviews. 900+ 5 star reviews on Amazon.
The roll-on application of this biofreeze can be easier to apply. Less overall mess.
If you know you already love it and trust the reviews. This is a great value that lasts a long time.
It has great reviews, loved by the all natural crowd. 100s of 5 star reviews with a near perfect rating.
Cons:
Don’t put this on open sores or mucous membranes, it will burn! It can run out quick and doesn’t prevent pain, just helps it.
Not as easy to spread in other areas, main difference is the roll on applicator, same solution.
A gigantic bottle that could fall over and injure you! Seriously this could be too big in some situations.
Basically looks like menthol(active Biofreeze ingredient), but with hemp extract SKYROCKETING the price.
Important Tips:
Menthol is the active ingredient in this and other hemp based creams. It works similar to ice, but once you apply it you can just move on rather than waiting 20 minutes. **Works great to get your through the night if you have pain sleeping**
Roll-on method is best for the bottom of the feet. No other real advantage. Most patients like it prior to bed for easy sleeping without foot pain.
If you know you love it, this stuff works all over the sore areas in your body not just your foot. I have had many people get me to order this for them in the past and LOVED IT!
The hemp extract is almost nothing and likely a marketing gimmick. It’s basically Biofreeze with some hemp extract raising the price.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Muscle/Ligament Pain Relief Products
Best & Proven Pain Relieving Gel.

Price:
$34.95
Overview:
The Proven and Scientifically Published Menthol Based Gel
Pros:
Scientifically proven to loosen up and relief pain up to 2x longer than Ice. Less effort than ice and great reviews. 900+ 5 star reviews on Amazon.
Cons:
Don’t put this on open sores or mucous membranes, it will burn! It can run out quick and doesn’t prevent pain, just helps it.
Important Tips:
Menthol is the active ingredient in this and other hemp based creams. It works similar to ice, but once you apply it you can just move on rather than waiting 20 minutes. **Works great to get your through the night if you have pain sleeping**
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Muscle/Ligament Pain Relief Products
Roll On Version of Biofreeze Gel.

Price:
$29.95
Overview:
Same as biofreeze gel, but the roll-on is prefered by some people for their feet, less messy.
Pros:
The roll-on application of this biofreeze can be easier to apply. Less overall mess.
Cons:
Not as easy to spread in other areas, main difference is the roll on applicator, same solution.
Important Tips:
Roll-on method is best for the bottom of the feet. No other real advantage. Most patients like it prior to bed for easy sleeping without foot pain.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Muscle/Ligament Pain Relief Products
A giant container of value size biofreeze.

Price:
$175.00
Overview:
8.1 lbs(3.67 kg) of Value Sized Biofreeze!
Pros:
If you know you already love it and trust the reviews. This is a great value that lasts a long time.
Cons:
A gigantic bottle that could fall over and injure you! Seriously this could be too big in some situations.
Important Tips:
If you know you love it, this stuff works all over the sore areas in your body not just your foot. I have had many people get me to order this for them in the past and LOVED IT!
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Muscle/Ligament Pain Relief Products
Menthol Based Ointment with Hemp Extract

Price:
$19.99
Overview:
This is an alternative cream: Basically Biofreeze + hemp extract.
Pros:
It has great reviews, loved by the all natural crowd. 100s of 5 star reviews with a near perfect rating.
Cons:
Basically looks like menthol(active Biofreeze ingredient), but with hemp extract SKYROCKETING the price.
Important Tips:
The hemp extract is almost nothing and likely a marketing gimmick. It’s basically Biofreeze with some hemp extract raising the price.
Affiliate Link (Buying through these links will connect you to Amazon):
Massage Sticks:
- These can work great for loosening your muscles.
- This allows less tightness and pressure onto the plantar fascia and heel.
- This is very effective for the arch, the gastrocnemius, calf muscle, and the hamstring and thigh muscles.
- This also works very well for the gluteus muscles if you are having butt cheek or hip pain.
- The massage stick can break up lumps in your Achilles tendon and heel pain.
Leg & Calf Muscle Massage Roller Sticks:
Best Overall Muscle Massage Stick
Best Cost Effective Massage Roller.
Best & Most Affordable Foot Massage Unit



Price:
$39.95
Price not available
Price not available
Overview:
This is a great option because hair or skin never gets pinched between the wheels. Softer interface.
Great option for an amazing cost. Not as sturdy and comfortable as the tiger tail.
A well reviewed foot massage unit.
Pros:
Best reviews. Hair and skin cannot get pinched. Almost instantly makes you less tender and more flexible. This is a professional grade massage roller.
Amazing reviews for the price point. It essentially does the same job. Muscles feel great afterward. Same overall benefit.
Amazing reviews averaging almost 5 stars. Reasonable price compared to most other units. Relieves swelling and inflammation in your feet naturally.
Cons:
If truly injured (break or tear) this won’t fix your pain. But no real downsides as far as what a massage roller does. Reviews are near perfect.
Wheels and handles can come loose. As a result it can gap and pinch skin and leg hairs. Not as durable as the other roller recommended here.
A more expensive version of manual and ice massage. The extra $ is basically to remove the manual labor yourself if you are OK with that!
Important Tips:
Studies show how effective massage rollers are: Use for 30-60 seconds to loosen up tight muscles, and then you can stretch further short term(1-2 hrs). Great for calf, hamstring, thight and IT band muscle stretching.
Same as for the more expensive one. Studies show the real benefits appear in 30-60 seconds per muscle => less sore and more flexible. That is the time to take advantage and play sports/stay loose. Very proven results.
This can actually help loosen up your calf muscles and foot muscles for a better stretch. So take advantage! You will be less sore and more flexible, but the results disappear after 1-2 hours or so!
Affiliate Link (Buying through these links will connect you to Amazon):
Leg & Calf Muscle Massage Roller Sticks:
Best Overall Muscle Massage Stick

Price:
$39.95
Overview:
This is a great option because hair or skin never gets pinched between the wheels. Softer interface.
Pros:
Best reviews. Hair and skin cannot get pinched. Almost instantly makes you less tender and more flexible. This is a professional grade massage roller.
Cons:
If truly injured (break or tear) this won’t fix your pain. But no real downsides as far as what a massage roller does. Reviews are near perfect.
Important Tips:
Studies show how effective massage rollers are: Use for 30-60 seconds to loosen up tight muscles, and then you can stretch further short term(1-2 hrs). Great for calf, hamstring, thight and IT band muscle stretching.
Affiliate Link (Buying through these links will connect you to Amazon):
Leg & Calf Muscle Massage Roller Sticks:
Best Cost Effective Massage Roller.

Price:
Price not available
Overview:
Great option for an amazing cost. Not as sturdy and comfortable as the tiger tail.
Pros:
Amazing reviews for the price point. It essentially does the same job. Muscles feel great afterward. Same overall benefit.
Cons:
Wheels and handles can come loose. As a result it can gap and pinch skin and leg hairs. Not as durable as the other roller recommended here.
Important Tips:
Same as for the more expensive one. Studies show the real benefits appear in 30-60 seconds per muscle => less sore and more flexible. That is the time to take advantage and play sports/stay loose. Very proven results.
Affiliate Link (Buying through these links will connect you to Amazon):
Leg & Calf Muscle Massage Roller Sticks:
Best & Most Affordable Foot Massage Unit

Price:
Price not available
Overview:
A well reviewed foot massage unit.
Pros:
Amazing reviews averaging almost 5 stars. Reasonable price compared to most other units. Relieves swelling and inflammation in your feet naturally.
Cons:
A more expensive version of manual and ice massage. The extra $ is basically to remove the manual labor yourself if you are OK with that!
Important Tips:
This can actually help loosen up your calf muscles and foot muscles for a better stretch. So take advantage! You will be less sore and more flexible, but the results disappear after 1-2 hours or so!
Affiliate Link (Buying through these links will connect you to Amazon):
Remove the Achilles tendon tightness.
- The key is to prevent future pain stress and trauma to the Achilles tendon muscle.
- This means keeping you active while keeping stress off of your Achilles tendon. This will prevent future re-injury and the development of plantar fasciitis.
- If you can get rid of the pain and swelling, this will let you start walking normally.
- If you can walk normally, the vast majority of your pain should gradually start to go away.
- The best way to ensure that your plantar fascia, foot, and ankle ligaments are not overworked is to support them.
- The best way to support them is to use great orthotics and great shoes.
- Some people may also need to rely on supportive ankle braces and other supportive modalities.
Best Shoes for Back of Heel Pain:
- Getting a great supportive pair of Achilles tendonitis shoes will ensure that there is pressure removed from the heel and plantar fascia region.
- This is especially important if you have plantar fasciitis, heel spur pain, or Achilles tendonitis as well.
- Consider Achilles tendonitis shoes combined with a good supportive orthotic for best pain relief!
- The following link will show you what our favorites are.
Best Achilles Tendonitis Insoles:
- These are our recommended orthotics for Achilles tendonitis.
- Custom orthotics can work very well, but they should not be the first line of treatment due to the cost.
- There are different types of different shoes.
- Women’s shoes usually need a less bulky orthotic but allow for less correction.
- A full-length orthotic requires a running shoe, boot, or comfortable walking/dress shoe.
- We recommend doing everything you can to get a good supportive shoe that can fit a full-length orthotic.
- A further home remedy tip for Achilles tendonitis pain is cutting out a hole where the nodule uses scissors or a knife. Be careful and start with a very low-cost orthotic.

Best Full Length Achilles tendonitis Orthotics:
- These will only work in wider shoes or a good supportive running shoe.
- This will not work in sandals, flats, or most women’s dress shoes.
Best Medium to Heavy Duty Heel Pain Orthotics:
Best Overall Orthotic For Everything (Medium Thick Fit)
Best Heavy Duty Orthotic (Thickest Fit)
Best SOFTER Choice For Sensitive Feet (Medium Thick Fit)
Best Women’s Orthotics




Price:
$44.95
$40.91
Price not available
$59.95
Overview:
These work best in shoes with laces and running shoes. Not good for dress shoes or women’s cute shoes.
Biggest and most corrective option. Only use for running shoes or work boots. Not cute shoes.
These are full length inserts, but softer. Great if you can’t tolerate the firmer ones. Best for very sore and sensitive feet.
Great Support & Better Fit
Pros:
Pretty much guaranteed to help you if it fits in your shoes and you give it 2 weeks to get used to. 5,000+ amazon reviews, great track record.
My personal favorite, but not for everyone. Amazing reviews over 3,500. But not for everyone. Only for bigger shoes that can fit them
They are softer and the initial break in time is AMAZING. But longer term benefits are less. >500 Almost 5 star amazon rating.
Sleek, supportive and have a better fit than the orthotics above.
Cons:
Do not wear these in cute or dress shoes!
Bigger and bulkier than all the other ones. You will be dissappointed if you have a cute women’s shoe or dress shoe. This is meant for running shoes and boots.
Great to start with, but don’t correct long term as much as the other ones.
A little bit more expensive.
Crucial Tips:
Ease in to these, 1-2hrs a day. They are like braces for your teeth, they suck at the beginning! But they will make your feet pain free as 1-2 weeks go by. Don’t give up on them after 1 or 2 days. Everyone feels off at the beginning!
This has the most correction, but hardest break in time! IF SENSITIVE, USE A SOFTER PAIR FIRST! But if you get these, you must break them in. Give it 1-2 hours a day, but then you will start to have excellent results. The bad reviews are all people who couldn’t fit it into their shoes and gave up too quickly. You have been WARNED!
If you are very sore, TRY THESE FIRST! These are easiest to break in with initially. If you are very sore and rigid, don’t use the heavy duty ones to start with.
These will have a harder time fitting in flats and pointed shoes.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Medium to Heavy Duty Heel Pain Orthotics:
Best Overall Orthotic For Everything (Medium Thick Fit)

Price:
$44.95
Overview:
These work best in shoes with laces and running shoes. Not good for dress shoes or women’s cute shoes.
Pros:
Pretty much guaranteed to help you if it fits in your shoes and you give it 2 weeks to get used to. 5,000+ amazon reviews, great track record.
Cons:
Do not wear these in cute or dress shoes!
Crucial Tips:
Ease in to these, 1-2hrs a day. They are like braces for your teeth, they suck at the beginning! But they will make your feet pain free as 1-2 weeks go by. Don’t give up on them after 1 or 2 days. Everyone feels off at the beginning!
Affiliate Link (Buying through these links will connect you to Amazon):
Best Medium to Heavy Duty Heel Pain Orthotics:
Best Heavy Duty Orthotic (Thickest Fit)

Price:
$40.91
Overview:
Biggest and most corrective option. Only use for running shoes or work boots. Not cute shoes.
Pros:
My personal favorite, but not for everyone. Amazing reviews over 3,500. But not for everyone. Only for bigger shoes that can fit them
Cons:
Bigger and bulkier than all the other ones. You will be dissappointed if you have a cute women’s shoe or dress shoe. This is meant for running shoes and boots.
Crucial Tips:
This has the most correction, but hardest break in time! IF SENSITIVE, USE A SOFTER PAIR FIRST! But if you get these, you must break them in. Give it 1-2 hours a day, but then you will start to have excellent results. The bad reviews are all people who couldn’t fit it into their shoes and gave up too quickly. You have been WARNED!
Affiliate Link (Buying through these links will connect you to Amazon):
Best Medium to Heavy Duty Heel Pain Orthotics:
Best SOFTER Choice For Sensitive Feet (Medium Thick Fit)

Price:
Price not available
Overview:
These are full length inserts, but softer. Great if you can’t tolerate the firmer ones. Best for very sore and sensitive feet.
Pros:
They are softer and the initial break in time is AMAZING. But longer term benefits are less. >500 Almost 5 star amazon rating.
Cons:
Great to start with, but don’t correct long term as much as the other ones.
Crucial Tips:
If you are very sore, TRY THESE FIRST! These are easiest to break in with initially. If you are very sore and rigid, don’t use the heavy duty ones to start with.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Medium to Heavy Duty Heel Pain Orthotics:
Best Women’s Orthotics

Price:
$59.95
Overview:
Great Support & Better Fit
Pros:
Sleek, supportive and have a better fit than the orthotics above.
Cons:
A little bit more expensive.
Crucial Tips:
These will have a harder time fitting in flats and pointed shoes.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Dress Shoe Achilles tendonitisOrthotics:
- These are a great choice for dress orthotics.
Best Dress Shoe Orthotics:
Best Fitting Dress Shoe Orthotic (3/4″)
Best Full Length Dress Orthotic.
Great Heavy Duty Insole for Men



Price:
Price not available
Price not available
$34.95
Overview:
This is my top choice due to best fit. It is a little less supportive than full length, but fit is the key in dress shoes!
Best option if you can fit a full length orthotic. This does give you most control.
Great price and heavy duty insole for Oxford shoes.
Pros:
Excellent overall fit. This will fit in almost every dress shoe. Excellent reviews and reasonable cost overall. Can’t go wrong in most cases.
Great color dress option. Not the most corrective, but very color and dress appropriate. Great Reviews. Better correction and relief than the 3/4″ length.
These fit in most shoes and have really good predictable results
Cons:
Less correction than full length and heavy duty orthotics.
These can have a poor fit in in some shoes. If you have tight shoes, DO NOT BUY the full length orthotic! You have been warned.
They are not full length and thus do not provide as much support
Crucial Tips:
If you haven’t used dress orthotics before, get this one and avoid poor fit. If you wear dress shoes every day with room, the full length might give you more support.
This is will work great in most men’s shoes that are not pointy. If you have a rounded toe box, this will probably work well. If a tight shoe go with the 3/4″ length.
Get these for Oxford and pointed shoes. This will provide best results.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Dress Shoe Orthotics:
Best Fitting Dress Shoe Orthotic (3/4″)

Price:
Price not available
Overview:
This is my top choice due to best fit. It is a little less supportive than full length, but fit is the key in dress shoes!
Pros:
Excellent overall fit. This will fit in almost every dress shoe. Excellent reviews and reasonable cost overall. Can’t go wrong in most cases.
Cons:
Less correction than full length and heavy duty orthotics.
Crucial Tips:
If you haven’t used dress orthotics before, get this one and avoid poor fit. If you wear dress shoes every day with room, the full length might give you more support.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Dress Shoe Orthotics:
Best Full Length Dress Orthotic.

Price:
Price not available
Overview:
Best option if you can fit a full length orthotic. This does give you most control.
Pros:
Great color dress option. Not the most corrective, but very color and dress appropriate. Great Reviews. Better correction and relief than the 3/4″ length.
Cons:
These can have a poor fit in in some shoes. If you have tight shoes, DO NOT BUY the full length orthotic! You have been warned.
Crucial Tips:
This is will work great in most men’s shoes that are not pointy. If you have a rounded toe box, this will probably work well. If a tight shoe go with the 3/4″ length.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Dress Shoe Orthotics:
Great Heavy Duty Insole for Men

Price:
$34.95
Overview:
Great price and heavy duty insole for Oxford shoes.
Pros:
These fit in most shoes and have really good predictable results
Cons:
They are not full length and thus do not provide as much support
Crucial Tips:
Get these for Oxford and pointed shoes. This will provide best results.
Affiliate Link (Buying through these links will connect you to Amazon):
Best 3/4 Length Achilles tendonitis Orthotics:
- These are great options for women’s dress shoes and thinner shoes.
- These are not the most supportive pair of orthotics.
Best Flat Shoe (Non-Lace Up) Orthotics:
Best Choice For Tight Women’s Shoes or High Heels..

Price:
Price not available
Overview:
These are the best fitting for the most narrow shoes. Some but not great correction.
Pros:
They will fit in even the tightest shoes! Guaranteed to make you feel better, but you know what you are getting in a tight shoes. Great reviews and price.
Cons:
At the end of the day high heels and slender orthotics help, but never cure all your pain. Make the best of a painful shoe!
Crucial Tips:
**WARNING***: If your shoe almost just barely fits onto your foot, this WILL NOT FIT! Be aware, it still needs a small amount of space to fit.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Flat Shoe (Non-Lace Up) Orthotics:
Best Choice For Tight Women’s Shoes or High Heels..

Price:
Price not available
Overview:
These are the best fitting for the most narrow shoes. Some but not great correction.
Pros:
They will fit in even the tightest shoes! Guaranteed to make you feel better, but you know what you are getting in a tight shoes. Great reviews and price.
Cons:
At the end of the day high heels and slender orthotics help, but never cure all your pain. Make the best of a painful shoe!
Crucial Tips:
**WARNING***: If your shoe almost just barely fits onto your foot, this WILL NOT FIT! Be aware, it still needs a small amount of space to fit.
Affiliate Link (Buying through these links will connect you to Amazon):
Get A Great Dynamic Stretch:
- It is possible to stretch on your own, but these products can also really help!
- This will take pressure off of the ball of your foot.
- This form of the back of the heel pain physical therapy breaks up the scar tissue.
- We personally prefer this method of stretching.
Best Standing Foot & Ankle Stretching Devices:
Best Premium Plantar Fascia Stretching Device.
Best Budget Plantar Fascia Stretching Stretch Device.
Best Stationary Calf Stretching Device.
Best Hamstring Stretching Device




Price:
Price not available
$20.06
$39.99
$67.95
Overview:
Great Stretching Device While Standing. (4.9 Amazon Rating)
Plastic and Lighter Plantar Fascia & Achilles Stretching Device.
Premium Best Rated Wood Ankle Stretch Device.
Uses gravity to stretch your hamstring for you. Great reviews and track record.
Pros:
Very sturdy and durable. Great bottom grip and weight so it won’t slide on you. Perfect 5 star review on Amazon.
Amazing cost, still works and 1,300+ 5 star reviews. Works great overall and gives you the same stretch.
Near perfect 4.8 star review on Amazon. Great sturdy device that stretches your calf and hamstring. All you have to do is lean forward. Can be very effective.
Reviews on Amazon are >4.5 overall with hundreds of reviews. It uses gravity to stretch for you, allows you to also use your hips. Gets great results.
Cons:
More expensive and built like a tank = more weight. If you can’t balance well or support yourself it could be dangerous.
The plastic and less bulk/grip makes it more dangerous to slip. Less premium feel to it.
Nothing wrong with the product, as the reviews suggest, but at the end of the day you can do this stuff yourself (just a little bit harder).
These are stretches that you realistically can do on your own. If budget is tight, this is not worth it. If you need help with hamstring stretching, it can make all the difference.
Important Tips:
Make sure you can balance yourself well against a counter/railing. Do only one foot at a time to prevent falling. Uses your body weight to stretch for you.
Even more important to balance yourself well with this device, make sure you don’t injure yourself with this thing! Still gives you a great stretch to the area.
Make sure you balance yourself on a counter/railing. You need to keep up with this daily at least 15-30 second x 3 or so per morning. It doesn’t stretch for you!
Need to do 3-5 stretches per day 15-30 seconds. You should notice a massive difference to knee and hamstring tightness. You can massage roll ahead to time for better results for 30-60 seconds.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Standing Foot & Ankle Stretching Devices:
Best Premium Plantar Fascia Stretching Device.

Price:
Price not available
Overview:
Great Stretching Device While Standing. (4.9 Amazon Rating)
Pros:
Very sturdy and durable. Great bottom grip and weight so it won’t slide on you. Perfect 5 star review on Amazon.
Cons:
More expensive and built like a tank = more weight. If you can’t balance well or support yourself it could be dangerous.
Important Tips:
Make sure you can balance yourself well against a counter/railing. Do only one foot at a time to prevent falling. Uses your body weight to stretch for you.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Standing Foot & Ankle Stretching Devices:
Best Budget Plantar Fascia Stretching Stretch Device.

Price:
$20.06
Overview:
Plastic and Lighter Plantar Fascia & Achilles Stretching Device.
Pros:
Amazing cost, still works and 1,300+ 5 star reviews. Works great overall and gives you the same stretch.
Cons:
The plastic and less bulk/grip makes it more dangerous to slip. Less premium feel to it.
Important Tips:
Even more important to balance yourself well with this device, make sure you don’t injure yourself with this thing! Still gives you a great stretch to the area.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Standing Foot & Ankle Stretching Devices:
Best Stationary Calf Stretching Device.

Price:
$39.99
Overview:
Premium Best Rated Wood Ankle Stretch Device.
Pros:
Near perfect 4.8 star review on Amazon. Great sturdy device that stretches your calf and hamstring. All you have to do is lean forward. Can be very effective.
Cons:
Nothing wrong with the product, as the reviews suggest, but at the end of the day you can do this stuff yourself (just a little bit harder).
Important Tips:
Make sure you balance yourself on a counter/railing. You need to keep up with this daily at least 15-30 second x 3 or so per morning. It doesn’t stretch for you!
Affiliate Link (Buying through these links will connect you to Amazon):
Best Standing Foot & Ankle Stretching Devices:
Best Hamstring Stretching Device

Price:
$67.95
Overview:
Uses gravity to stretch your hamstring for you. Great reviews and track record.
Pros:
Reviews on Amazon are >4.5 overall with hundreds of reviews. It uses gravity to stretch for you, allows you to also use your hips. Gets great results.
Cons:
These are stretches that you realistically can do on your own. If budget is tight, this is not worth it. If you need help with hamstring stretching, it can make all the difference.
Important Tips:
Need to do 3-5 stretches per day 15-30 seconds. You should notice a massive difference to knee and hamstring tightness. You can massage roll ahead to time for better results for 30-60 seconds.
Affiliate Link (Buying through these links will connect you to Amazon):
Get A Great Static Stretch:
- These devices are great for stretching while you are resting.
- This is an excellent Achilles tendonitis physical therapy that you can do at home.
- This will also help take pressure off of the ball of your foot.
- This works great for plantar fasciitis.
- The static night splint can use it while watching TV or at night time.
Best Night & Stretch Splint Products:
Most Cost Effective Night Splint (Not Best for Sleeping).
Best Actual Night Splint (For Night Time Use)
Best Price & Light Support Night Splint



Price:
$39.99
$58.14
Price not available
Overview:
Hard Night Splint -** Use it before going to bed for 20-30 minutes**
Best & most comfortable splint for actual night time use.
Top of the foot softer & more gentle splint.
Pros:
This is an amazing device with the highest amazon rating. Has 2 great foot wedges that bend your big toe up and lock your foot in. Great at what it does.
This has excellent reviews(better than the hard splint), less foot numbness and soreness in the ball of your foot. Very soft and comfortable.
Most people can tolerate this one during the night, but only because it stretches you less! That might be a good thing if you can set it and forget it for 6-8 hours at night.
Cons:
Hard to use at while sleeping, so don’t use it that way! Easy to use it incorrectly if you don’t use the foot wedges correctly. Your big toe should be angled up to lock your foot in.
It actually stretches you less (that’s why you are able to wear it all night). It is more expensive.
Basically it is more tolerable because it is weaker. This less results in more time.
Important Tips:
**Must use the foot wedge in the front to angle your toes up. This locks your foot from twisting out rather than stretching through the Achilles tendon – This is the KEY!**
If you prefer to actually wear it at night then this is the BEST option. It does work, but this is for those with very little time and can fall asleep in it!
This is meant only for sleeping because to get results you need to wear it a lot longer than the other braces. Use it only if you are very sensitive.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Night & Stretch Splint Products:
Most Cost Effective Night Splint (Not Best for Sleeping).

Price:
$39.99
Overview:
Hard Night Splint -** Use it before going to bed for 20-30 minutes**
Pros:
This is an amazing device with the highest amazon rating. Has 2 great foot wedges that bend your big toe up and lock your foot in. Great at what it does.
Cons:
Hard to use at while sleeping, so don’t use it that way! Easy to use it incorrectly if you don’t use the foot wedges correctly. Your big toe should be angled up to lock your foot in.
Important Tips:
**Must use the foot wedge in the front to angle your toes up. This locks your foot from twisting out rather than stretching through the Achilles tendon – This is the KEY!**
Affiliate Link (Buying through these links will connect you to Amazon):
Best Night & Stretch Splint Products:
Best Actual Night Splint (For Night Time Use)

Price:
$58.14
Overview:
Best & most comfortable splint for actual night time use.
Pros:
This has excellent reviews(better than the hard splint), less foot numbness and soreness in the ball of your foot. Very soft and comfortable.
Cons:
It actually stretches you less (that’s why you are able to wear it all night). It is more expensive.
Important Tips:
If you prefer to actually wear it at night then this is the BEST option. It does work, but this is for those with very little time and can fall asleep in it!
Affiliate Link (Buying through these links will connect you to Amazon):
Best Night & Stretch Splint Products:
Best Price & Light Support Night Splint

Price:
Price not available
Overview:
Top of the foot softer & more gentle splint.
Pros:
Most people can tolerate this one during the night, but only because it stretches you less! That might be a good thing if you can set it and forget it for 6-8 hours at night.
Cons:
Basically it is more tolerable because it is weaker. This less results in more time.
Important Tips:
This is meant only for sleeping because to get results you need to wear it a lot longer than the other braces. Use it only if you are very sensitive.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Heel Compression Brace:
- A good compression brace can stabilize your foot from turning outward.
- This prevents your foot from pronation.
- The pronated foot will turn your foot outward, in your foot will rub on the outside of the shoe.
- This has solved their pain for many of her patients and is very comfortable to wear inside your shoe.
- This solves both pain and outward pronation for a relatively low cost.
Best Heel & Ankle Compression Braces:
Best Premium Brace (Support & Compression)
Budget Brace With Some Compression & Some Support.


Price:
$114.00
$22.49
Overview:
This is The Top Level Brace – Does Compression, Support & Great Fit.
This brace attempts mild compression and mild support.
Pros:
Excellent brace: Best overall mix of compression & support, and it still fits in most shoes! If you have a chronic injury and need to wear normal shoes => This is the BEST CHOICE.
Good rating at 4.3 with 2,000 reviews. It is cost effective and gives some support with some compression. Does both ok, but excellent when price is factored in.
Cons:
Expensive. It doesn’t do any single thing the best. There are cheaper and more supportive braces, there are cheaper and more compressive braces. But no braces combine the two and still fit in a shoe.
Does not really do anything well. Weak support and not the best compression. Meant as an assist for chronic pain and low activity. Not for an acute injury.
Important Tips:
This is a high durability brace for everyday use. If you have chronic arthritis or pain with a high need for activity, this is your brace to use! **Gel inside seems to deteriorate after daily washing at about 1 year old**
This is mean for lower activity and better fit than a true supportive brace. Don’t use this for an acute sprain or injury.
Best Heel & Ankle Compression Braces:
Best Premium Brace (Support & Compression)

Price:
$114.00
Overview:
This is The Top Level Brace – Does Compression, Support & Great Fit.
Pros:
Excellent brace: Best overall mix of compression & support, and it still fits in most shoes! If you have a chronic injury and need to wear normal shoes => This is the BEST CHOICE.
Cons:
Expensive. It doesn’t do any single thing the best. There are cheaper and more supportive braces, there are cheaper and more compressive braces. But no braces combine the two and still fit in a shoe.
Important Tips:
This is a high durability brace for everyday use. If you have chronic arthritis or pain with a high need for activity, this is your brace to use! **Gel inside seems to deteriorate after daily washing at about 1 year old**
Affiliate Link (Buying through these links will connect you to Amazon):
Best Heel & Ankle Compression Braces:
Budget Brace With Some Compression & Some Support.

Price:
$22.49
Overview:
This brace attempts mild compression and mild support.
Pros:
Good rating at 4.3 with 2,000 reviews. It is cost effective and gives some support with some compression. Does both ok, but excellent when price is factored in.
Cons:
Does not really do anything well. Weak support and not the best compression. Meant as an assist for chronic pain and low activity. Not for an acute injury.
Important Tips:
This is mean for lower activity and better fit than a true supportive brace. Don’t use this for an acute sprain or injury.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Heel Stability Brace:
- The stability brace goes a little bit further than the compression brace to stop your foot from turning out.
- This takes the pressure off of your heel and plantar fascia.
- At the same time, this is a little bit bulkier and does not affect every shoe.
- We find people are a little bit happier trying the compression brace before the stability brace.
Best Ankle Stability Braces (Not for Compression):
The Best Overall Brace For Fit & Support.
Most Supportive Premium Brace.
Best Budge Supportive Brace.


Price:
Price not available
$112.88
$31.97
Overview:
Amazing brace, best fit and support combination: If you can afford it.
This is the best brace for pure support, but it can’t fit in more snug shoes.
Outstanding brace for the price point. This is a figure 8 strap with laces, soft interface.
Pros:
Amazing brace. Best reviews and best fit. This is the Ferrari of braces if you can afford it.
This is a very highly rated, great reviewed brace. The support and stability is top notch for athletics. Very durable and does it’s job.
Amazing reviews with proven track record. This is very soft and supportive in your shoe.
Cons:
The only downside besides cost, is complexity. This brace must be left or right. Not interchangeable. It is also for post-injury situations and good support. Not for compression!
The brace may be a little too big for a more snug shoe. This requires some room to fit and would be the main complaint. Hard interface along the padding.
The main downside is the durability and the ability for the material to give out. Great at first but maybe 3-4 months of continuous use prior to failure.
Important Tips:
Make sure to choose left vs. right. This is a high level brace mean specifically for injury support. This is not for compression or non-injury situations. It will be too tight.
This is a fantastic and supportive brace. Just make sure that your shoe will have some room for it to fit. Most good running shoes should let it fit.
This is an excellent starter brace if you have never had a brace before. It is a little longer to put with the straps and laces.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Ankle Stability Braces (Not for Compression):
The Best Overall Brace For Fit & Support.

Price:
Price not available
Overview:
Amazing brace, best fit and support combination: If you can afford it.
Pros:
Amazing brace. Best reviews and best fit. This is the Ferrari of braces if you can afford it.
Cons:
The only downside besides cost, is complexity. This brace must be left or right. Not interchangeable. It is also for post-injury situations and good support. Not for compression!
Important Tips:
Make sure to choose left vs. right. This is a high level brace mean specifically for injury support. This is not for compression or non-injury situations. It will be too tight.
Affiliate Link (Buying through these links will connect you to Amazon):
Compare Stores:
Best Ankle Stability Braces (Not for Compression):
Most Supportive Premium Brace.

Price:
$112.88
Overview:
This is the best brace for pure support, but it can’t fit in more snug shoes.
Pros:
This is a very highly rated, great reviewed brace. The support and stability is top notch for athletics. Very durable and does it’s job.
Cons:
The brace may be a little too big for a more snug shoe. This requires some room to fit and would be the main complaint. Hard interface along the padding.
Important Tips:
This is a fantastic and supportive brace. Just make sure that your shoe will have some room for it to fit. Most good running shoes should let it fit.
Affiliate Link (Buying through these links will connect you to Amazon):
Compare Stores:
Best Ankle Stability Braces (Not for Compression):
Best Budge Supportive Brace.

Price:
$31.97
Overview:
Outstanding brace for the price point. This is a figure 8 strap with laces, soft interface.
Pros:
Amazing reviews with proven track record. This is very soft and supportive in your shoe.
Cons:
The main downside is the durability and the ability for the material to give out. Great at first but maybe 3-4 months of continuous use prior to failure.
Important Tips:
This is an excellent starter brace if you have never had a brace before. It is a little longer to put with the straps and laces.
Affiliate Link (Buying through these links will connect you to Amazon):
Compare Stores:
Severe Achilles tendonitis Pain:
- If you think you might have a broken heel, a calcaneal stress fracture, or something of similar severity, these products might help!
- Always remember to see a foot and ankle specialist like a podiatrist if you have plantar fasciitis or more severe pain!
Plantar Fascia Tear, Broken Heel Bone, Achilles Tendon Tear:
- If you have a traumatic injury such as a torn plantar fascia ligament, calcaneus stress fracture, heel fracture, or insertional Achilles tendon injury: consider protecting your foot!
- The best way to do this is, of course, to see your podiatrist and get evaluated with an x-ray, ultrasound, and potentially even an MRI or CT scan.
- If you cannot do so, it may benefit you to be in a cast, fractured boot, or even keep the weight off of it with a rolling knee scooter or other protective devices.
- We as podiatrists frequently take patients off work for very long periods of time when they suffer a traumatic injury. Unfortunately, there is no other way around us in labor jobs.
- If you have a sit-down job, there are ways to get people back to work quicker, but this can be not easy otherwise.
Heel Injury Boot Treatment:
- There are pros and cons to using a boot to treat your heel injury. The Pros are that your injured heel will hopefully have a chance to heal gradually! If you are immobilized too long, the cons are that you will gradually become stiff and overworked to your other leg.
- Our favorite fracture boots and their supplies:
Best Fracture Boots & Covers
Best Tall Boot
Best Short Boot
Best Fracture Boot Balance Device
Best Cast Shower Cover




Price:
$81.07
$46.95
Price not available
$12.99
Overview:
Excellent reviews at 4.6/5 with over 800+ Reviews:
Very good reviews. This is 4.3/5 ratings on over 3,000+ reviews.
Outstanding reviews: 4.3/5 for 1,000+ reviews! Prevents hip, knee and back pain.
Amazing Reviews at 4.6/5 at 500+ reviews. Best reviewed and cost effective bag.
Pros:
It has an air bladder for extra cushion. It is tall for extra support, as well as air bladder.
Excellent lower cost walking boot. With a orthotic and cushion, it really keeps pressure off of your ankle.
This works great to balance the opposite foot. This prevents the back, hip and knees from having any pain.
It is very effective but not perfect. The price is really good and it has excellent reviews.
Cons:
The inner sleeve can ride lower and the plastic around the rim can irritate the boot.
Less support with the less than full length boot. It is more comfortable but less supportive.
Does not work that great for slippers and less supportive shoes.
It can still leak, so be careful!
Crucial Tips:
Make sure your lift the cushioning material along the hard plastic rim. Make sure to keep it pumped up. Use an orthotic and a lift on the other side.
Use a lift for the other foot to prevent back and hip problems. Also use an orthotic for the flat foot bed.
This is very cost effective and well worth it. Just make sure both shoes have good supportive orthotics.
Just be careful with this is not perfect. It can still get wet underneath.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Fracture Boots & Covers
Best Tall Boot

Price:
$81.07
Overview:
Excellent reviews at 4.6/5 with over 800+ Reviews:
Pros:
It has an air bladder for extra cushion. It is tall for extra support, as well as air bladder.
Cons:
The inner sleeve can ride lower and the plastic around the rim can irritate the boot.
Crucial Tips:
Make sure your lift the cushioning material along the hard plastic rim. Make sure to keep it pumped up. Use an orthotic and a lift on the other side.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Fracture Boots & Covers
Best Short Boot

Price:
$46.95
Overview:
Very good reviews. This is 4.3/5 ratings on over 3,000+ reviews.
Pros:
Excellent lower cost walking boot. With a orthotic and cushion, it really keeps pressure off of your ankle.
Cons:
Less support with the less than full length boot. It is more comfortable but less supportive.
Crucial Tips:
Use a lift for the other foot to prevent back and hip problems. Also use an orthotic for the flat foot bed.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Fracture Boots & Covers
Best Fracture Boot Balance Device

Price:
Price not available
Overview:
Outstanding reviews: 4.3/5 for 1,000+ reviews! Prevents hip, knee and back pain.
Pros:
This works great to balance the opposite foot. This prevents the back, hip and knees from having any pain.
Cons:
Does not work that great for slippers and less supportive shoes.
Crucial Tips:
This is very cost effective and well worth it. Just make sure both shoes have good supportive orthotics.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Fracture Boots & Covers
Best Cast Shower Cover

Price:
$12.99
Overview:
Amazing Reviews at 4.6/5 at 500+ reviews. Best reviewed and cost effective bag.
Pros:
It is very effective but not perfect. The price is really good and it has excellent reviews.
Cons:
It can still leak, so be careful!
Crucial Tips:
Just be careful with this is not perfect. It can still get wet underneath.
Affiliate Link (Buying through these links will connect you to Amazon):
Offloading and Scooter treatment:
- These are favorite knee scooters and walking devices.
- If your Achilles tendonitis pain is severe, offloading can be very effective until the pain calms down.
Best Fracture Scooters
Best Value & Best Seller Knee Rolling Scooter.
Best All Terrain Heavy Duty Scooter.
Best Crutch Free Walking Device.
Best Elevating Specific Postop or Swelling Pillow




Price:
$113.99
$254.99
Price not available
$34.99
Overview:
Very good reviews at 4.5/5 with 3,000+ reviews. Great Price.
Excellent overall reviews at 4.4/5 with 1,300+ reviews. Great heavy duty all terrain.
Decent reviews at 3.9/5 with 4,000+ reviews. NOT for everyone!
Very good reviews at 4.7/5 with almost 2,000 Reviews. Simple job but does it well.
Pros:
Great reviews, great price overall, what more can you ask for?
Good for offroad, grass and dirt. This is the better choice for heavy and tall patients over 6 foot and heavy.
This is great for athletic and mobile people. We have found success for younger and more physically capable people.
Great pillow for the first 1-2 weeks after foot or ankle fracture and surgery. Decreased pain and swelling.
Cons:
Least durable and no real off-road capabilities.
It is more costly than the economy version.
DO NOT get this if you are older, have poor balance and poor mobility. Higher fall risk.
Basically it is a pillow that costs $50, if you are tight on money, don’t get it.
Crucial Tips:
These can be tough on the knee and the lower back. Combine with physical therapy.
If you are a bigger person at over 6ft tall, consider this. If you need to be at work or outside, this is great option.
This is better for very mobile and physically capable people. Do not get this if you have poor weight control or poor balance.
It can be very effective and does a great job, but if you are tight on cash, use it on a better boot or scooter.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Fracture Scooters
Best Value & Best Seller Knee Rolling Scooter.

Price:
$113.99
Overview:
Very good reviews at 4.5/5 with 3,000+ reviews. Great Price.
Pros:
Great reviews, great price overall, what more can you ask for?
Cons:
Least durable and no real off-road capabilities.
Crucial Tips:
These can be tough on the knee and the lower back. Combine with physical therapy.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Fracture Scooters
Best All Terrain Heavy Duty Scooter.

Price:
$254.99
Overview:
Excellent overall reviews at 4.4/5 with 1,300+ reviews. Great heavy duty all terrain.
Pros:
Good for offroad, grass and dirt. This is the better choice for heavy and tall patients over 6 foot and heavy.
Cons:
It is more costly than the economy version.
Crucial Tips:
If you are a bigger person at over 6ft tall, consider this. If you need to be at work or outside, this is great option.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Fracture Scooters
Best Crutch Free Walking Device.

Price:
Price not available
Overview:
Decent reviews at 3.9/5 with 4,000+ reviews. NOT for everyone!
Pros:
This is great for athletic and mobile people. We have found success for younger and more physically capable people.
Cons:
DO NOT get this if you are older, have poor balance and poor mobility. Higher fall risk.
Crucial Tips:
This is better for very mobile and physically capable people. Do not get this if you have poor weight control or poor balance.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Fracture Scooters
Best Elevating Specific Postop or Swelling Pillow

Price:
$34.99
Overview:
Very good reviews at 4.7/5 with almost 2,000 Reviews. Simple job but does it well.
Pros:
Great pillow for the first 1-2 weeks after foot or ankle fracture and surgery. Decreased pain and swelling.
Cons:
Basically it is a pillow that costs $50, if you are tight on money, don’t get it.
Crucial Tips:
It can be very effective and does a great job, but if you are tight on cash, use it on a better boot or scooter.
Affiliate Link (Buying through these links will connect you to Amazon):
