Medically Reviewed by Dr. Tom Biernacki, DPM — Board-Certified Podiatrist, Balance Foot & Ankle Specialists, Michigan. Last updated April 2026.
PRP Injections for Foot and Ankle Pain: What Is Platelet-Rich Plasma and Does It Work?
Medically reviewed by Dr. Thomas Biernacki, DPM — Board-certified podiatric surgeon specializing in regenerative foot and ankle treatments at Balance Foot & Ankle, Southeast Michigan.
Quick Answer: What Is PRP?
Platelet-Rich Plasma (PRP) is a regenerative injection therapy that uses concentrated growth factors from your own blood to promote tissue healing and reduce inflammation. A small blood sample is drawn, processed to concentrate the platelets 3–8x above normal levels, and injected directly into the damaged tissue. For foot and ankle conditions, PRP shows the most promising results for chronic plantar fasciitis, Achilles tendinopathy, and ankle ligament injuries. PRP works best as part of a comprehensive treatment plan that includes supportive footwear with PowerStep Pinnacle Maxx insoles, topical pain management with Doctor Hoy’s Natural Pain Relief Gel, and compression with DASS compression socks.
Table of Contents
- Quick Answer
- What Is Platelet-Rich Plasma?
- How Does PRP Work?
- The PRP Procedure: What to Expect
- Foot and Ankle Conditions Treated with PRP
- PRP for Plantar Fasciitis
- PRP for Achilles Tendinopathy
- PRP for Ankle Ligament Injuries
- PRP for Foot and Ankle Arthritis
- What Does the Evidence Say?
- PRP vs Cortisone Injections
- Recovery After PRP Injection
- Complementary Treatments with PRP
- Who Is a Good Candidate for PRP?
- Most Common Mistake
- Warning Signs After PRP
- Cost and Insurance Coverage
- Complete PRP Recovery Kit
- Frequently Asked Questions
- Watch: PRP for Foot and Ankle Pain
- Sources
- Schedule Your Consultation
What Is Platelet-Rich Plasma?
If you’ve been struggling with a chronic foot or ankle condition that hasn’t responded to standard conservative treatments, platelet-rich plasma (PRP) therapy may be an option worth discussing with your podiatrist. PRP has gained significant attention in sports medicine and orthopedics as a regenerative treatment that harnesses your body’s own healing capabilities. But separating the science from the hype is important — PRP isn’t a miracle cure, but for specific conditions, the evidence supports its use as a valuable addition to a comprehensive treatment plan.
PRP is prepared from a small sample of the patient’s own blood (typically 30–60 mL). The blood is placed in a centrifuge that separates it into layers: red blood cells settle to the bottom, plasma rises to the top, and the platelet-rich layer concentrates in the middle. This concentrated platelet layer — containing 3–8 times the normal platelet concentration — is extracted and prepared for injection. Platelets contain over 300 bioactive proteins including growth factors (PDGF, TGF-β, VEGF, EGF, IGF-1) that are essential for tissue repair, collagen synthesis, angiogenesis (new blood vessel formation), and modulation of the inflammatory response.
How Does PRP Work?
When PRP is injected into damaged tissue, the concentrated platelets are activated by the tissue environment and release their stored growth factors. These growth factors initiate and amplify the body’s natural healing cascade through several mechanisms. Growth factor release stimulates local stem cells and tissue-resident progenitor cells to differentiate into the specific cell types needed for repair (tenocytes for tendon healing, fibroblasts for ligament repair, chondrocytes for cartilage support). Angiogenesis promotion creates new blood vessel formation in areas of poor blood supply — this is particularly relevant for the Achilles tendon and plantar fascia, which have notoriously poor blood supply in their mid-substance zones.
Collagen synthesis is stimulated, promoting the formation of organized, functional tissue rather than disorganized scar tissue. Inflammation modulation shifts the tissue environment from chronic, degenerative inflammation to an acute, productive healing response. This is a key distinction from cortisone injections, which suppress inflammation entirely — PRP aims to redirect the inflammatory process toward healing rather than simply turning it off. The full effect of PRP develops over 4–8 weeks as the growth factors stimulate a progressive healing response, with maximum benefit typically achieved at 3–6 months.
The PRP Procedure: What to Expect
The PRP procedure is performed in the office and takes approximately 30–45 minutes total. Here’s what to expect. First, a small blood sample (30–60 mL, roughly 2–4 tablespoons) is drawn from a vein in your arm — similar to a routine blood draw. The blood is placed in a specialized centrifuge and processed for 10–15 minutes to separate and concentrate the platelet-rich fraction. While the blood is processing, the injection site is prepared with ultrasound imaging to precisely identify the damaged tissue.
The injection itself is performed under ultrasound guidance for maximum accuracy. A local anesthetic may or may not be used — some protocols avoid anesthetic because lidocaine can theoretically reduce platelet function, while others use a small amount for patient comfort. The concentrated PRP is injected directly into the damaged tissue using a technique called “peppering” — multiple small deposits throughout the damaged area to ensure broad coverage. Mild discomfort during injection is normal and reflects the PRP activating within the tissue. The entire injection takes about 5 minutes.
After the injection, expect increased pain and swelling for 3–5 days — this is actually the desired response, as it represents the initiated healing cascade. Important: avoid NSAIDs (ibuprofen, naproxen, aspirin) for at least 2 weeks before and 4–6 weeks after PRP injection, as these medications inhibit the platelet function that PRP depends upon. Use Doctor Hoy’s Natural Pain Relief Gel and acetaminophen for pain management instead. Apply DASS compression socks to manage post-injection swelling.
Foot and Ankle Conditions Treated with PRP
PRP has been studied and used for a variety of foot and ankle conditions with varying levels of evidence. The strongest evidence supports its use in chronic plantar fasciitis and Achilles tendinopathy. Moderate evidence exists for ankle ligament injuries, peroneal tendinopathy, posterior tibial tendinopathy, and spring ligament injuries. Emerging evidence is being gathered for foot and ankle arthritis, osteochondral lesions of the talus, surgical augmentation (enhancing healing after tendon repair or fusion), and chronic wound healing in diabetic patients.
PRP for Plantar Fasciitis
Chronic plantar fasciitis is perhaps the strongest indication for PRP in the foot and ankle. Multiple randomized controlled trials have demonstrated that PRP provides superior long-term pain relief compared to cortisone injections for plantar fasciitis that has failed conservative treatment for more than 3 months. While cortisone provides faster initial relief (within 1–2 weeks), PRP provides more durable improvement — studies show sustained pain reduction at 6, 12, and even 24 months after a single PRP injection, whereas cortisone effects typically wear off by 3–6 months.
The mechanism makes biological sense: chronic plantar fasciitis is primarily a degenerative condition (plantar fasciosis) rather than an inflammatory one. The fascia shows disorganized collagen, neovascularization, and mucoid degeneration — tissue changes that don’t respond to anti-inflammatory treatment but do respond to the regenerative stimulus of PRP growth factors. PRP for plantar fasciitis should always be combined with biomechanical optimization — wearing PowerStep Pinnacle Maxx orthotic insoles in all shoes, proper stretching, and gradual return to activity after the injection.
PRP for Achilles Tendinopathy
Achilles tendinopathy — chronic degeneration of the Achilles tendon — is another condition where PRP shows meaningful benefit. Like plantar fasciosis, chronic Achilles tendinopathy involves degenerative tissue changes rather than true inflammation, making PRP’s regenerative mechanism particularly appropriate. Studies have shown improvement in pain scores, tendon thickness, and imaging appearance (reduced areas of degeneration on ultrasound) after PRP injection.
PRP for Achilles tendinopathy is typically performed under ultrasound guidance to precisely target areas of tendon degeneration. The injection is combined with a structured eccentric loading program (the gold standard rehabilitation for Achilles tendinopathy) that begins after the initial 1–2 week rest period. Continue wearing supportive shoes with PowerStep Pinnacle Maxx insoles to reduce tendon strain during recovery, and use Doctor Hoy’s Natural Pain Relief Gel along the tendon for topical pain management (remember: no NSAIDs for 4–6 weeks after PRP).
PRP for Ankle Ligament Injuries
PRP is increasingly used to augment healing of ankle ligament injuries, particularly the anterior talofibular ligament (ATFL) after lateral ankle sprains. Emerging evidence suggests that PRP injection at the site of ligament damage can accelerate healing, improve ligament quality, and potentially reduce the rate of chronic ankle instability that develops after severe sprains. PRP may be particularly valuable for grade II sprains (partial tears) where the ligament has healing potential but the natural repair process needs biological support.
For recurrent ankle sprains suggesting chronic ligament insufficiency, PRP can be considered as an intermediate step between failed conservative treatment and surgical ligament repair (modified Broström procedure). The injection is combined with intensive proprioceptive rehabilitation and ankle bracing during the healing period. Compression with DASS compression socks helps manage swelling while the ligament heals.
PRP for Foot and Ankle Arthritis
PRP for arthritic joints is more controversial than for tendon conditions. The evidence is mixed — some studies show modest improvement in pain and function for early-to-moderate arthritis, while severe arthritis with significant joint space loss typically shows minimal benefit. PRP for arthritis likely works through its anti-inflammatory properties rather than true tissue regeneration — it modulates the inflammatory joint environment, reducing pain and potentially slowing cartilage degeneration.
In our practice, we consider PRP for foot and ankle arthritis in patients with mild-to-moderate joint degeneration who want to delay surgical intervention. It can be particularly useful for ankle, subtalar, and first MTP joint arthritis. Multiple injections (typically a series of 2–3 spaced 4–6 weeks apart) may provide more sustained benefit than a single injection for arthritic joints. Concurrent use of PowerStep Pinnacle Maxx insoles for biomechanical support and Doctor Hoy’s Pain Relief Gel for topical pain management optimizes outcomes.
What Does the Evidence Say?
The scientific evidence for PRP in foot and ankle conditions has grown substantially over the past decade. For plantar fasciitis, level I evidence (randomized controlled trials) supports PRP over cortisone for long-term pain relief, with multiple meta-analyses confirming superiority at 6 and 12 months. For Achilles tendinopathy, the evidence is moderately positive, with several RCTs showing improvement over placebo, though results are somewhat variable depending on PRP preparation method and injection technique. For ankle ligament healing and arthritis, the evidence is still emerging with smaller studies and less robust methodology.
It’s important to understand that PRP preparation varies significantly between systems — the platelet concentration, white blood cell content (leukocyte-rich vs leukocyte-poor), and activation method all influence the biological activity of the final product. This variability contributes to inconsistent results in the literature. At our practice, we use a standardized preparation protocol that has been validated in published clinical trials to ensure consistent, high-quality PRP for every injection.
PRP vs Cortisone Injections
The PRP vs cortisone debate is common, and understanding the differences helps patients make informed decisions. Cortisone is a powerful anti-inflammatory that provides rapid pain relief (often within days) by suppressing the inflammatory response. However, cortisone does not promote tissue healing — in fact, repeated cortisone injections can weaken tendons and fascia, potentially leading to rupture. Cortisone effects are typically temporary (weeks to months), and there are limits on how many injections a structure can safely receive.
PRP takes longer to work (4–8 weeks for initial improvement, 3–6 months for maximum benefit) but aims to promote actual tissue healing rather than just suppressing symptoms. PRP carries no risk of tissue weakening (unlike cortisone) and can theoretically be repeated without cumulative damage. The disadvantage is that PRP is more expensive, requires a blood draw and centrifuge processing, and the initial post-injection period involves increased pain rather than the immediate relief cortisone provides. For most chronic conditions that have failed initial conservative treatment, PRP represents a better biological strategy — treat the underlying tissue degeneration rather than repeatedly masking symptoms with cortisone.
Recovery After PRP Injection
Days 1–5: Expect increased pain and swelling at the injection site — this is normal and represents the desired healing response. Manage with acetaminophen (NOT ibuprofen or naproxen), Doctor Hoy’s Natural Pain Relief Gel applied around the injection area, ice for 15–20 minutes every 2–3 hours, and DASS compression socks for swelling control. Limit activity to gentle walking with supportive shoes and PowerStep Pinnacle Maxx insoles.
Weeks 1–4: Pain gradually decreases but may fluctuate. Begin gentle stretching and range-of-motion exercises at 1–2 weeks. Avoid high-impact activity. Continue avoiding NSAIDs. Maintain compression and topical pain management. Weeks 4–8: Many patients begin to notice improvement. Gradually resume activity. Physical therapy can be initiated to optimize the healing response. Months 2–6: Progressive improvement continues. Most patients achieve maximum benefit at 3–6 months. If insufficient improvement at 3 months, a second injection may be considered.
Complementary Treatments with PRP
PRP works best as part of a comprehensive treatment plan, not as a standalone treatment. Essential complementary treatments include orthotic support with PowerStep Pinnacle Maxx insoles to address biomechanical factors that caused the tissue damage, physical therapy with eccentric loading exercises (for tendon conditions) or stretching protocols (for plantar fasciitis), topical pain management with Doctor Hoy’s Natural Pain Relief Gel as an NSAID-safe alternative, compression therapy with DASS compression socks for swelling control, and activity modification during the healing window.
Who Is a Good Candidate for PRP?
The ideal PRP candidate has a chronic (>3 months) foot or ankle condition that has failed standard conservative treatment, has a condition with established evidence for PRP benefit (plantar fasciitis, Achilles tendinopathy), is willing to comply with post-injection restrictions (no NSAIDs, modified activity), has realistic expectations about the timeline (weeks to months, not days), and doesn’t have conditions that impair platelet function (certain blood disorders, active cancer treatment, certain medications). PRP may be less effective in patients who smoke, have uncontrolled diabetes, or have severe tissue degeneration with complete tears rather than partial damage.
Most Common Mistake
🔑 Most Common Mistake: Taking NSAIDs after a PRP injection. This is the single most common error that undermines PRP effectiveness. Ibuprofen, naproxen, aspirin, and other NSAIDs directly inhibit platelet function — the very mechanism PRP depends on for healing. Taking NSAIDs after PRP is like paying for expensive car repairs and then pouring sugar in the gas tank. Use Doctor Hoy’s Natural Pain Relief Gel for topical pain relief and acetaminophen (Tylenol) for systemic pain control. Avoid all NSAIDs for at least 4–6 weeks before and after PRP.
Warning Signs After PRP
🚨 Warning Signs — Contact Your Doctor If You Experience: Severe pain that worsens progressively beyond 5–7 days (some pain increase is expected for 3–5 days, but it should begin improving). Signs of infection: increasing redness, warmth, swelling, or drainage from the injection site, or fever above 100.4°F. Allergic reaction (rare with autologous PRP): hives, difficulty breathing, facial swelling. Sudden sharp pain or “pop” at the injection site (very rare — possible tendon rupture if the tissue was severely compromised). Numbness or tingling that develops after the injection and persists beyond 24 hours. These are uncommon but require prompt evaluation.
Cost and Insurance Coverage
PRP injections are generally not covered by most insurance plans, including Medicare, as they are still considered “investigational” by many payers despite growing clinical evidence. The out-of-pocket cost typically ranges from $400–$800 per injection depending on the PRP preparation system used, number of injection sites, and geographic location. While this represents a significant investment, many patients find the cost justified when compared to the cumulative cost of repeated cortisone injections, ongoing physical therapy, and the potential cost of surgical intervention that PRP may help avoid.
Some insurance plans are beginning to cover PRP for specific indications (particularly plantar fasciitis) as the evidence base strengthens. We recommend checking with your insurance provider before scheduling PRP treatment. For patients considering PRP, the investment includes not just the injection but the complete treatment protocol — orthotic support, rehabilitation, and follow-up — that maximizes the chance of a successful outcome.
Complete PRP Recovery Kit
✅ Complete PRP Recovery Kit — Recommended by Dr. Biernacki:
🦶 PowerStep Pinnacle Maxx Orthotic Insoles — Essential biomechanical support during PRP recovery. Addresses the structural factors that caused tissue damage, preventing re-injury while PRP promotes healing. Use in every pair of shoes from the day of injection onward.
🧴 Doctor Hoy’s Natural Pain Relief Gel — The NSAID-safe pain management solution for PRP patients. Since ibuprofen and naproxen must be avoided for 4–6 weeks after PRP, Doctor Hoy’s topical gel becomes your primary pain relief tool. Apply 2–3 times daily to the treatment area.
🧦 DASS Medical-Grade Compression Socks — Controls the post-injection swelling that naturally occurs as PRP initiates the healing response. Wear daily for the first 2–4 weeks post-injection. Enhances topical gel absorption when worn over Doctor Hoy’s application.
This kit is specifically designed for PRP recovery — every component is NSAID-free and supports the biological healing process that PRP initiates.
Affiliate Disclosure: Some links above are affiliate links, meaning we may earn a small commission at no extra cost to you. We only recommend products we personally use with our patients at Balance Foot & Ankle.
More Podiatrist-Recommended Cortisone Essentials
Hoka Clifton 10
Max-cushion everyday shoe — podiatrist favorite for walking and running.
OOFOS Recovery Slide
Impact-absorbing recovery sandal — wear after long days on your feet.
As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. Product recommendations are based on clinical experience; prices and availability shown above update live from Amazon.
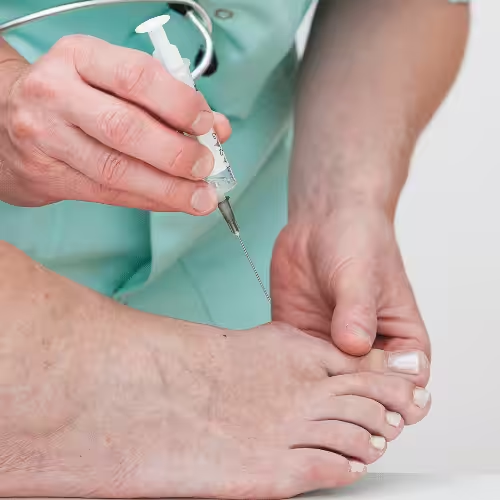
When to See a Podiatrist
Cortisone injections are most effective when paired with a root-cause fix — orthotic, shoe change, or physical therapy. At Balance Foot & Ankle, we use ultrasound guidance to place every injection exactly in the inflamed space, maximizing relief. And we always discuss the treatment plan that follows, so the pain stays gone.
Call Balance Foot & Ankle: (810) 206-1402 · Book online · Offices in Howell & Bloomfield Hills
Frequently Asked Questions About PRP Injections
Does PRP injection hurt?
The blood draw is similar to a routine lab test. The injection itself causes moderate discomfort — patients typically describe it as a deep pressure or aching sensation that lasts 1–2 minutes during the injection and increases over the first 24–48 hours. Pain management with acetaminophen and Doctor Hoy’s Pain Relief Gel keeps discomfort manageable. Most patients say it’s tolerable and worth it for the long-term results.
How many PRP injections do I need?
For tendon conditions (plantar fasciitis, Achilles tendinopathy), a single injection is often sufficient, with reassessment at 3 months to determine if a second injection would be beneficial. For arthritic joints, a series of 2–3 injections spaced 4–6 weeks apart typically provides better results than a single injection. Your doctor will recommend a treatment plan based on your specific condition and response.
How long does it take for PRP to work?
Unlike cortisone which provides rapid relief, PRP works gradually. Most patients notice initial improvement at 4–6 weeks with progressive improvement over 3–6 months. The delayed onset reflects the biological healing process — PRP stimulates tissue remodeling that takes weeks to months to mature. This is why combining PRP with supportive treatments like PowerStep Pinnacle Maxx insoles is essential during the waiting period.
Can I walk after a PRP injection in my foot?
Yes, gentle walking in supportive shoes is encouraged after PRP injection. Avoid high-impact activities (running, jumping, heavy lifting) for 2–4 weeks, but normal daily walking is safe and actually beneficial for promoting blood flow to the treatment area. Wear PowerStep Pinnacle Maxx insoles in supportive shoes and DASS compression socks to manage swelling.
Is PRP better than cortisone for plantar fasciitis?
For chronic plantar fasciitis (>3 months), multiple studies show PRP provides superior long-term results compared to cortisone. Cortisone works faster initially (days vs weeks) but effects wear off by 3–6 months, while PRP improvements are sustained at 12–24 months. PRP also avoids the risk of plantar fascia weakening or rupture that repeated cortisone injections carry.
Watch: PRP for Foot and Ankle Pain
Sources
- Peerbooms JC, van Laar W, Faber F, Schuller HM, van der Hoeven H, Gosens T. “Use of Platelet Rich Plasma to Treat Plantar Fasciitis: Design of a Multi Centre Randomized Controlled Trial.” BMC Musculoskeletal Disorders. 2010;11:69.
- Monto RR. “Platelet-Rich Plasma Efficacy Versus Corticosteroid Injection Treatment for Chronic Severe Plantar Fasciitis.” Foot & Ankle International. 2014;35(4):313-318.
- de Vos RJ, Weir A, van Schie HT, et al. “Platelet-Rich Plasma Injection for Chronic Achilles Tendinopathy.” JAMA. 2010;303(2):144-149.
- Franceschi F, Papalia R, Franceschetti E, Paciotti M, Maffulli N, Denaro V. “Platelet-Rich Plasma Injections for Chronic Plantar Fasciitis: A Systematic Review.” British Medical Bulletin. 2014;112(1):83-95.
- Filardo G, Di Matteo B, Kon E, Merli G, Marcacci M. “Platelet-Rich Plasma in Tendon-Related Disorders: Results and Indications.” Knee Surgery, Sports Traumatology, Arthroscopy. 2018;26(7):1984-1999.
Schedule Your PRP Consultation
If you have a chronic foot or ankle condition that hasn’t responded to standard treatments, PRP therapy may provide the regenerative stimulus your body needs to heal. Dr. Biernacki offers PRP injections with ultrasound guidance for plantar fasciitis, Achilles tendinopathy, and other foot and ankle conditions at Balance Foot & Ankle in Southeast Michigan.
👉 Schedule Your PRP Consultation Today
Related Articles: Podiatrist-Recommended Foot Care Products · Plantar Fasciitis Treatment · Achilles Tendinitis Treatment
Insurance Accepted
BCBS · Medicare · Aetna · Cigna · United Healthcare · HAP · Priority Health · Humana · View All →
Howell Office
3980 E Grand River Ave, Suite 140
Howell, MI 48843
Get Directions →
Bloomfield Hills Office
43700 Woodward Ave, Suite 207
Bloomfield Hills, MI 48302
Get Directions →
Your Board-Certified Podiatrists
Ready to Get Back on Your Feet?
Same-week appointments available at both locations.
Book Your AppointmentWhen Shoes Aren’t Enough — Dr. Tom’s Top 9 Orthotics
About 30% of patients I see for foot pain need MORE than a great shoe — they need a structured insole. Below: my complete 2026 orthotic ranking with pros, cons, and the specific patient I’d give each one to.
★ DR. TOM’S COMPLETE 2026 ORTHOTIC RANKING
9 Best Prefab Orthotics by Use Case
PowerStep, Currex, Spenco, Vionic, and PowerStep Pinnacle — every orthotic I’ve fitted to thousands of patients across both Michigan offices. Each card includes pros, cons, and the specific patient I’d give it to. Real Amazon ratings, review counts, and prices below.
Best All-Purpose Orthotic for Most Patients
Semi-rigid arch shell + dual-layer cushion + deep heel cup. The orthotic I’ve fitted to more patients than any other for 15 years. APMA-accepted. Trim-to-fit design works in athletic shoes, casual shoes, and most work boots.
✓ Pros
- Semi-rigid arch shell provides true biomechanical correction
- Deep heel cup centers the heel and reduces lateral instability
- Dual-layer cushion (top + bottom) lasts 9-12 months daily wear
- Available in 8 sizes for precise fit
- APMA-accepted and clinically validated
- Lower price than PowerStep Pinnacle for equivalent function
✗ Cons
- Too thick for most dress shoes (use ProTech Slim instead)
- Some break-in period required (3-7 days for arch tolerance)
- Not enough correction for severe pes planus or rigid pes cavus
Dr. Tom’s Recommendation: If a patient has run-of-the-mill plantar fasciitis, mild flat feet, or arch fatigue, this is the first orthotic I try. Better value than PowerStep Pinnacle for 90% of patients, which is why I swapped it into our clinic kits three years ago. Sub-$50 typically.
Maximum Motion Control · Flat Feet & Severe Over-Pronation
PowerStep’s most aggressive stability orthotic. Adds a 2°-7° medial heel post on top of the standard PowerStep platform — designed specifically for flat-footed patients and severe pronators who need real corrective force.
✓ Pros
- 2°-7° medial heel post adds aggressive pronation control
- Same trusted PowerStep arch shell, more correction
- Built specifically for flat-foot biomechanics
- Excellent for posterior tibial tendon dysfunction (PTTD)
- Removable top cover for cleaning
✗ Cons
- Too aggressive for neutral-arch patients
- Needs longer break-in (10-14 days) due to stronger correction
- Adds 2-3 mm of stack height — won’t fit slim dress shoes
Dr. Tom’s Recommendation: When a patient comes in with significant flat feet AND symptoms (heel pain, arch pain, knee pain), the Original PowerStep isn’t aggressive enough. The Maxx is what gets prescribed. About 25% of my flat-footed patients end up here.
Low-Profile · Fits Dress Shoes & Narrow Casuals
3 mm slim profile with podiatrist-designed tri-planar arch technology. Engineered specifically to fit inside dress shoes, oxfords, loafers, and women’s flats without crowding the toe box. Vionic was founded by an Australian podiatrist.
✓ Pros
- 3 mm slim profile (vs 7-10 mm for standard orthotics)
- Tri-planar arch technology adds support without bulk
- Built-in deep heel cup despite slim design
- Fits dress shoes WITHOUT having to remove the factory insole
- Trim-to-fit · APMA-accepted
✗ Cons
- Less arch support than full-volume orthotics
- Top cover wears faster than thicker alternatives
- Not enough correction for severe foot deformities
Dr. Tom’s Recommendation: My default when a patient says ‘I need orthotics but I have to wear dress shoes for work.’ Slim enough to fit in oxfords and pumps without the heel sliding out. The single highest-impact change you can make for office workers with foot pain.
Built-In Metatarsal Pad · Morton’s Neuroma · Ball-of-Foot Pain
Standard Pinnacle orthotic with a built-in metatarsal pad positioned proximal to the metatarsal heads — the exact location that offloads neuromas and metatarsalgia. No need for separate met pads or pad placement guesswork.
✓ Pros
- Built-in met pad eliminates DIY pad placement errors
- Specifically designed for Morton’s neuroma + metatarsalgia
- Same trusted PowerStep arch + heel cup platform
- Top cover protects sensitive forefoot skin
- Faster relief than orthotics + add-on met pads
✗ Cons
- Met pad position is fixed (can’t fine-tune individual placement)
- Some patients with very small or very large feet need custom
- Slightly thicker than the standard Pinnacle
Dr. Tom’s Recommendation: If a patient has Morton’s neuroma, sesamoiditis, or generalized ball-of-foot pain (metatarsalgia), this saves a clinic visit and a prescription. The built-in pad placement is anatomically correct for 80% of feet. Way better than DIY met pads.
Adaptive Dynamic Arch · Athletic & Daily Wear
Currex’s flagship adaptive arch technology — the orthotic flexes with your gait instead of fighting it. Different stiffness zones along the length give you targeted support at the heel, midfoot, and forefoot. Available in three arch heights (low/medium/high).
✓ Pros
- Dynamic flex zones adapt to natural gait cycle
- Three arch heights ensure precise fit
- Lighter than rigid orthotics (no ‘heavy foot’ feel)
- Excellent for runners and athletic walkers
- European podiatric design (German engineering)
✗ Cons
- More expensive than PowerStep Original ($55-65 typically)
- Less aggressive correction than Pinnacle Maxx for severe cases
- Three arch heights means you must self-select correctly
Dr. Tom’s Recommendation: I started recommending Currex three years ago for runners who said PowerStep felt ‘too rigid.’ The dynamic flex zones respect natural gait. Best for active patients who walk 8K+ steps daily and don’t need maximum motion control.
Running-Specific · Heel Strike + Forefoot Strike Compatible
Currex’s purpose-built running orthotic. The midfoot flex zone is positioned for runner’s gait mechanics, with a flared heel cushion for heel strikers and a forefoot rocker for midfoot/forefoot strikers. Tested on 1000+ runners during product development.
✓ Pros
- Designed by German biomechanics lab specifically for runners
- Dynamic arch flexes with running gait (not static like PowerStep)
- Three arch heights (low/medium/high)
- Reduces overuse injury risk in mid-distance runners
- Lightweight (no impact on cadence)
✗ Cons
- Premium price ($60-75)
- Not aggressive enough for severe over-pronators (use Pinnacle Maxx)
- Runner-specific design = less ideal for daily walking shoes
Dr. Tom’s Recommendation: If a patient runs 20+ miles per week and has plantar fasciitis or shin splints, this is the orthotic I prescribe. The dynamic flex zones respect running biomechanics in a way that no rigid PowerStep can match. Pricier but worth it for serious runners.
Cavus Foot & High-Arch Patients
Polyurethane base with a deeper heel cup and higher arch profile than PowerStep — built for cavus (high-arched) feet that need maximum cushion and support. The 5-zone cushioning system addresses the unique pressure points of high-arch feet.
✓ Pros
- Deeper heel cup centers the heel for cavus foot stability
- Higher arch profile fills the void under high arches
- 5-zone cushioning addresses cavus foot pressure points
- Polyurethane base lasts 12+ months
- Available in Wide width
✗ Cons
- Too tall/aggressive for normal or low arches
- Won’t fit slim dress shoes
- Pricier than PowerStep Original
- Some patients find the arch height uncomfortable initially
Dr. Tom’s Recommendation: Cavus foot patients are often misdiagnosed and given low-arch orthotics — that makes everything worse. Spenco’s Total Support has the arch profile that high-arch feet actually need. About 15% of my patients have cavus feet; this is what they wear.
Cushion Layer · Standing All Day · Gel Pressure Relief
NOT a true biomechanical orthotic — this is a cushion insole. But for patients who want gel pressure relief instead of arch correction (or to add ON TOP of factory insoles in work boots), this is the best gel option on Amazon.
✓ Pros
- Genuine gel cushioning (not foam pretending to be gel)
- Targeted gel waves under heel and ball of foot
- Trim-to-fit · works in most shoe types
- Sub-$15 price (most affordable option in this list)
- Massaging texture is genuinely soothing
✗ Cons
- ZERO arch support — this is cushion only
- Won’t fix plantar fasciitis or flat-foot issues
- Compresses faster than PowerStep (4-6 months)
- Top cover wears through in high-mileage applications
Dr. Tom’s Recommendation: I recommend these to patients who tell me ‘I just want my feet to stop hurting at the end of my shift’ and who don’t have a biomechanical issue. Construction workers, factory workers, retail. Pure cushion does the job for them.
Tight-Fitting Shoes · Cycling Shoes · Hockey Skates
PowerStep Pinnacle’s slim version of their famous Green insole. The trademark stabilizer cap is preserved but the overall thickness is reduced — works in cycling shoes, hockey skates, ski boots, and other tight-fitting footwear that the standard PowerStep Pinnacle can’t fit into.
✓ Pros
- Stabilizer cap centers the heel (PowerStep Pinnacle’s signature feature)
- Slim profile fits tight athletic footwear
- Lasts 12+ months daily wear
- Excellent for cycling shoes specifically
- Built-in odor-control treatment
✗ Cons
- Premium price ($45-55)
- Less cushion than PowerStep equivalents
- Not as aggressive correction as Pinnacle Maxx for flat feet
- The signature ‘heel cup feel’ takes 1-2 weeks to adapt to
Dr. Tom’s Recommendation: If you’re a cyclist with foot numbness, hot spots, or knee pain — this is the orthotic. The stabilizer cap solves cycling-specific biomechanical issues that no other orthotic addresses. Worth the premium for athletes.
None of these solving your foot pain?
Some patients (about 30%) need custom-molded prescription orthotics. We make 3D-scanned custom orthotics in our Howell and Bloomfield Hills offices — specifically built for your foot mechanics.
Schedule a Custom Orthotic Fitting →FSA/HSA eligible · Most insurance accepted · (810) 206-1402
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.
- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)
Recommended Products from Dr. Tom
Treatment Options Available at Our Office














