Medically reviewed by Dr. Carl Jay, DPM
Board-certified podiatric surgeon | Balance Foot & Ankle
Last reviewed: April 2026
Quick answer: A ganglion cyst on the big toe joint is a noncancerous, fluid-filled sac that forms near the joint capsule or tendon sheath. These rubbery, round lumps can range from pea-sized to marble-sized and may cause pain when pressing against shoes or nerves. Many ganglion cysts resolve on their own; persistent ones can be aspirated (drained) or surgically removed. Recurrence rates are 15–20% after aspiration and 5–10% after surgical excision.
Finding a lump on your big toe joint can be frightening — your mind may jump to worst-case scenarios. The good news is that a soft, rubbery bump near the big toe joint is most likely a ganglion cyst, which is completely benign. At Balance Foot & Ankle, we evaluate foot and toe lumps regularly and can determine whether your bump is a ganglion cyst, a bunion, or something else entirely — often during a single office visit.
What Is a Ganglion Cyst?
A ganglion cyst is a noncancerous, fluid-filled sac that develops from the lining of a joint capsule or tendon sheath. The cyst is filled with thick, clear, jelly-like synovial fluid — the same fluid that lubricates your joints. Ganglion cysts are the most common soft-tissue tumors of the foot and ankle, accounting for approximately 60% of all soft-tissue masses in this region.
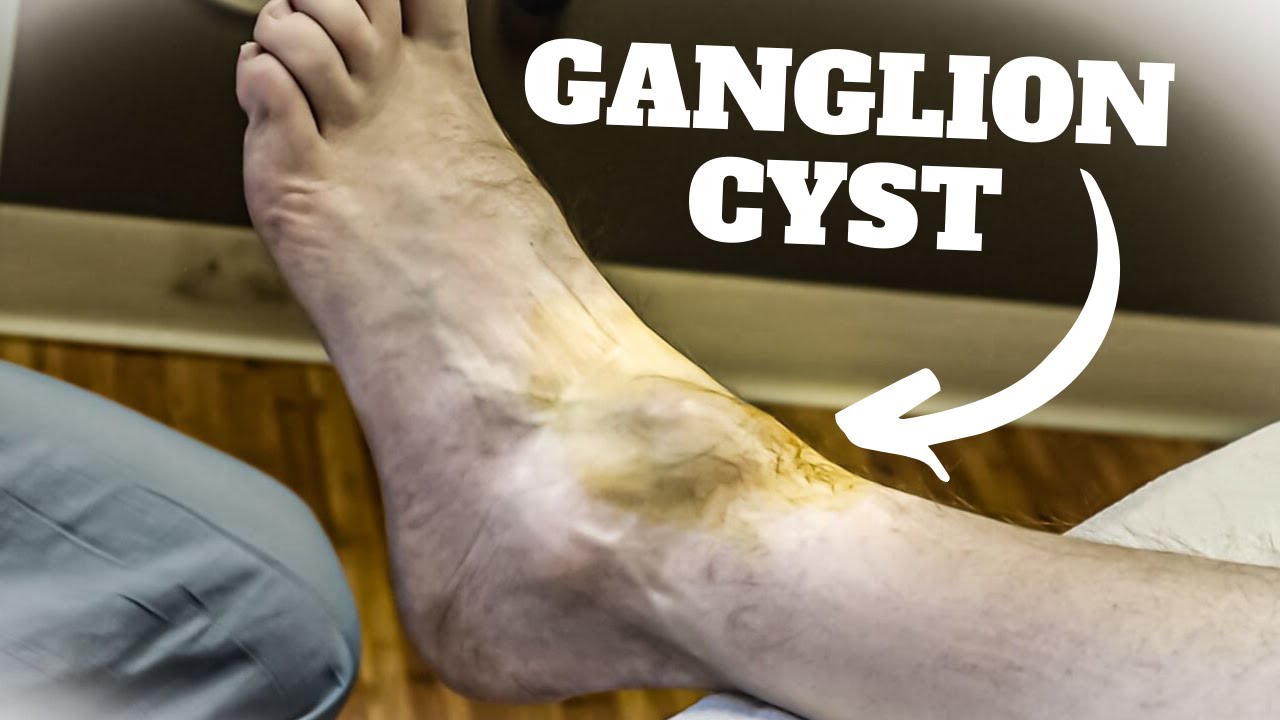
On the big toe joint (first metatarsophalangeal joint), ganglion cysts typically appear on the top (dorsal) surface as a firm, round, smooth lump. They can range from pea-sized to over 2.5 cm in diameter and may change size over time — sometimes growing larger with activity and shrinking with rest. Unlike malignant growths, ganglion cysts are mobile (they move freely under the skin) and have well-defined borders.
What Causes Ganglion Cysts on the Foot?
The exact cause of ganglion cysts isn’t fully understood, but they’re believed to develop from micro-tears or degeneration in the joint capsule or tendon sheath. Joint irritation from repetitive stress, previous injury, or underlying arthritis may trigger the formation. The body produces excess synovial fluid in response to joint irritation, and this fluid collects in a balloon-like sac adjacent to the joint.
Ganglion cysts are more common in women (3:1 ratio) and most frequently affect adults aged 20–50. Conditions that stress the big toe joint — including hallux rigidus (big toe arthritis), bunion deformity, and repetitive athletic activities — may increase the risk. There’s also evidence suggesting a genetic predisposition, as ganglion cysts tend to run in families.
Symptoms
- Visible or palpable lump: A round, smooth, firm-but-slightly-compressible bump, typically on the top of the big toe joint
- Pain with shoe pressure: The cyst may rub against the inside of your shoe, causing irritation, redness, and pain
- Aching or dull pain: Larger cysts can press on nearby nerves or joint structures, causing localized discomfort
- Size fluctuation: The cyst may enlarge with activity and shrink with rest — this size change is characteristic of ganglion cysts
- Joint stiffness: Large cysts near the joint line can limit range of motion
- Tingling or numbness: If the cyst compresses a digital nerve, you may experience numbness in the big toe
Some ganglion cysts are completely asymptomatic — discovered only because you notice the bump visually. If the cyst isn’t causing pain, numbness, or functional limitation, treatment may not be necessary.
⚠️ See a Podiatrist If:
- The lump is hard, fixed (doesn’t move), or irregularly shaped
- The mass is growing rapidly
- There’s associated skin discoloration or ulceration
- You experience persistent numbness or weakness in the toe
- Pain is worsening or isn’t explained by the visible bump
- You’re unsure if the lump is a ganglion cyst, bunion, or something else
How We Diagnose Ganglion Cysts
At Balance Foot & Ankle, diagnosis typically begins with physical examination. Ganglion cysts have classic features: they transilluminate (light passes through them because they’re fluid-filled), are mobile and smooth, and occur in typical locations near joints or tendons. We press, prod, and transilluminate the mass to assess its characteristics.
In-office diagnostic ultrasound confirms the diagnosis by visualizing the cyst as a well-defined, fluid-filled structure adjacent to the joint. Ultrasound can also determine the cyst’s exact size, whether it has a stalk connecting it to the joint, and its relationship to nearby nerves and tendons. In rare cases where the diagnosis is uncertain or a solid mass is suspected, MRI provides detailed soft-tissue evaluation. X-rays may be ordered to evaluate the underlying joint for arthritis or bone spurs that may be contributing to cyst formation.
Watch and Wait
If the ganglion cyst is small, painless, and not interfering with shoe wear or daily activities, observation is a perfectly reasonable approach. Studies show that up to 40–58% of ganglion cysts resolve spontaneously without treatment. Your podiatrist may recommend protective padding over the cyst to prevent shoe friction, wider footwear, and periodic monitoring to ensure the mass remains stable.
Important: Never attempt to “pop” or smash a ganglion cyst yourself (the old “Bible bump” treatment of hitting it with a heavy book). This can damage surrounding structures, doesn’t address the cyst stalk, and risks infection and recurrence. Leave treatment to your podiatrist.
Aspiration (Needle Drainage)
Aspiration is a minimally invasive in-office procedure where your podiatrist inserts a needle into the cyst and drains the fluid. The procedure takes about 10 minutes, is performed under local anesthesia, and provides immediate relief. The thick, jelly-like fluid is sent for pathology if there’s any diagnostic uncertainty.
After aspiration, a corticosteroid injection into the cyst cavity may reduce the inflammatory response and lower recurrence rates. The main limitation of aspiration is recurrence — the cyst stalk remains intact, and the sac can refill with fluid. Recurrence rates after aspiration are approximately 15–50%, with some studies showing lower rates when combined with corticosteroid injection. Multiple aspiration attempts are reasonable before considering surgery.
Surgical Excision
Surgical excision is recommended for ganglion cysts that recur after aspiration, cause significant pain, or compress nerves. The procedure involves removing the entire cyst, including its stalk and a small cuff of the joint capsule from which it originates. This addresses the root cause and has the lowest recurrence rate — approximately 5–10%.
Surgery is typically performed under local anesthesia as an outpatient procedure. Recovery involves 1–2 weeks of limited activity, suture removal at 10–14 days, and return to regular footwear within 3–4 weeks. Complications are uncommon but can include surgical site infection, nerve damage (temporary numbness), and recurrence. Our surgeons at Balance Foot & Ankle use meticulous dissection techniques to minimize these risks.
Preventing Recurrence
While no method guarantees prevention, addressing the underlying joint irritation that triggered cyst formation reduces recurrence risk. This includes treating associated conditions (arthritis, bone spurs), wearing properly fitted shoes that don’t compress the big toe joint, using custom orthotics to optimize foot mechanics, and avoiding repetitive trauma to the area. If you have underlying hallux rigidus contributing to cyst formation, treating the arthritis helps prevent future cysts.
Frequently Asked Questions
Is a ganglion cyst on the big toe dangerous?
No — ganglion cysts are benign (noncancerous) and pose no danger to your health. They’re simply collections of joint fluid in a sac. The main concerns are cosmetic appearance, shoe friction, and pain from nerve compression. However, any new lump should be evaluated to confirm it’s a ganglion cyst and not a different type of mass.
Can a ganglion cyst go away on its own?
Yes — studies show that 40–58% of ganglion cysts resolve spontaneously without any treatment. They may fluctuate in size for months or even years before eventually disappearing. However, some cysts persist indefinitely or continue to grow. If yours is painful or interfering with daily activities, waiting may not be the best strategy.
How do I know if my lump is a ganglion cyst or a bunion?
A ganglion cyst is soft-to-firm, round, mobile under the skin, and typically on the top of the joint. A bunion is a bony prominence on the inner (medial) side of the big toe joint, is hard and fixed, and is associated with the big toe angling toward the second toe. Your podiatrist can easily distinguish between the two with a physical exam and X-rays.
Does ganglion cyst aspiration hurt?
Most patients describe mild discomfort — a brief sting from the local anesthetic injection, then pressure during fluid drainage. The entire procedure takes about 10 minutes and is well-tolerated. Afterward, mild soreness for 1–2 days is common and manageable with ice and over-the-counter pain relief.
The Bottom Line
A ganglion cyst on the big toe joint is a benign, treatable condition. Many cysts resolve on their own, but those that persist can be effectively managed with aspiration or surgical excision. The key is getting a proper diagnosis to rule out other conditions and choosing the right treatment approach for your specific situation. At Balance Foot & Ankle, we provide in-office ultrasound evaluation, aspiration, and surgical excision — giving you a clear path from diagnosis to resolution.
Concerned About a Lump on Your Foot?
Same-week appointments in Howell & Bloomfield Hills, MI. Three board-certified podiatrists.
4.9★ | 1,100+ Reviews | 3,000+ Surgeries
Or call: (810) 206-1402
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon serving Southeast Michigan at Balance Foot & Ankle Specialists. With over a decade of clinical experience and thousands of surgeries and procedures performed, Dr. Biernacki brings exceptional expertise to every patient interaction.
A Michigan native, Dr. Biernacki earned his undergraduate degree from the University of Memphis and his Doctor of Podiatric Medicine (DPM) from Kent State University College of Podiatric Medicine. He completed a three-year advanced surgical residency in foot and ankle surgery in the Detroit metro area, followed by additional fellowship training in podiatric surgery.
Dr. Biernacki specializes in the treatment of heel pain, bunions, hammertoes, diabetic foot care, sports injuries, flatfoot correction, and minimally invasive foot surgery. He is dedicated to providing evidence-based, patient-centered care that helps people of all ages stay active and pain-free.
Outside the office, Dr. Biernacki is a devoted family man — married for over 15 years and a proud father of four children. He is committed to community education through the MichiganFootDoctors.com resource library and his YouTube channel, which has reached over one million views. Dr. Biernacki is a member of the American Podiatric Medical Association (APMA) and the American College of Foot and Ankle Surgeons (ACFAS).