Quick answer: Toe Amputation Surgery Digit Removal Diabetic Wound Care is a common foot/ankle topic that affects many patients. The 2026 evidence-based approach combines proper diagnosis, conservative-first treatment, and escalation only when needed. We treat this regularly at our Howell and Bloomfield Township practices. Call (810) 206-1402.
Medically reviewed by Dr. Tom Biernacki, DPM — Board-Certified Podiatric Surgeon — Balance Foot & Ankle, Howell & Bloomfield Hills, MI. Last updated April 2026.
▶ Watch
Medically Reviewed by Dr. Tom Biernacki, DPM — Board-Certified Podiatrist, Balance Foot & Ankle Specialists, Michigan. Last updated April 2026.
When Toe Amputation Becomes Necessary
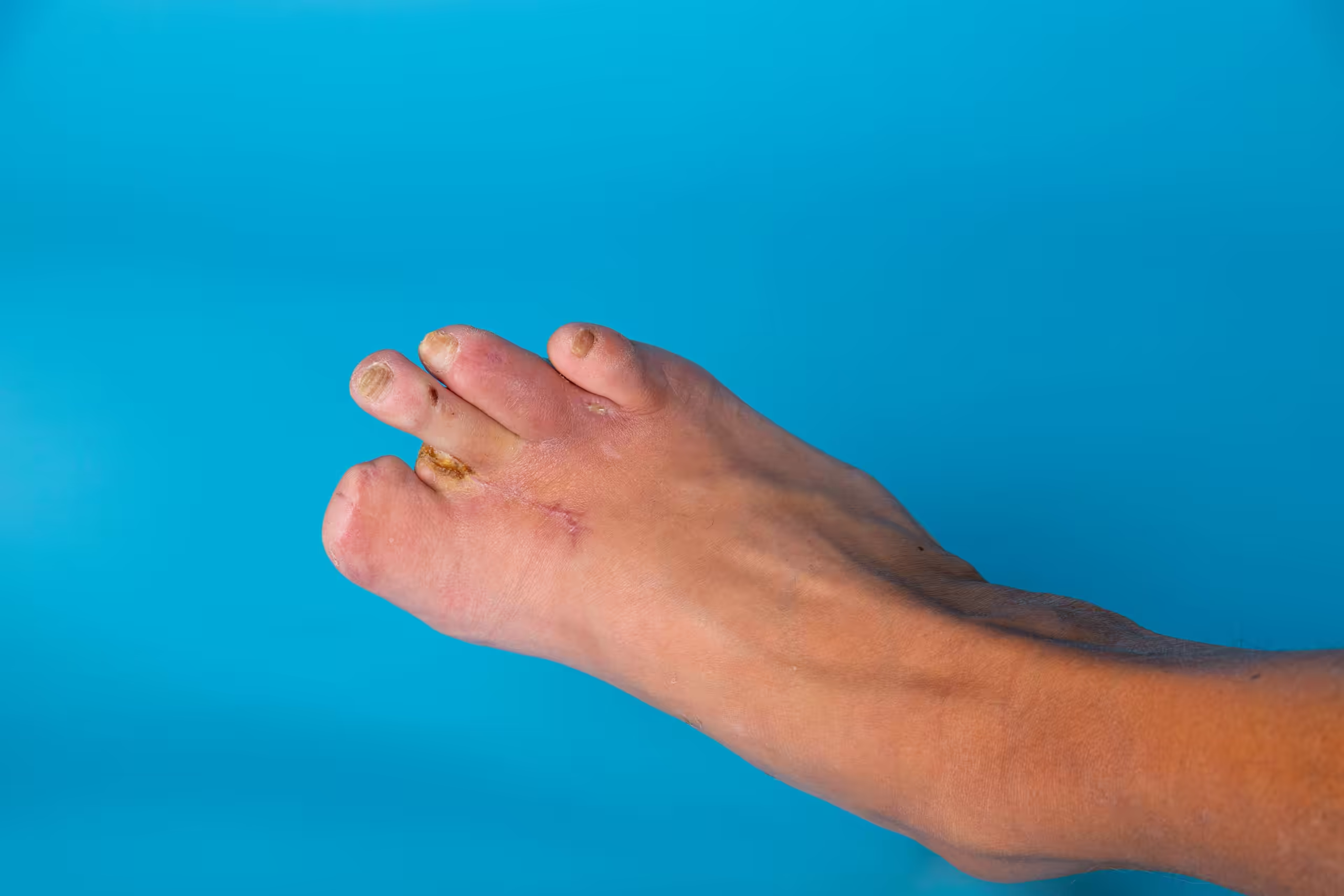
Toe amputation is one of the most difficult conversations in foot and ankle medicine. The goal of podiatric care is always preservation — preventing wounds, treating infections aggressively, and restoring tissue when possible. But circumstances exist in which removing a toe is the most effective way to save the rest of the foot and the patient life: uncontrolled infection spreading to bone, gangrene from severely compromised blood supply, and cancer involving the digit are the most common indications.
Far from being a sign of treatment failure, timely toe amputation — when genuinely indicated — is a life-preserving and limb-preserving procedure that allows the patient to heal, ambulate, and avoid a more proximal amputation.
Common Indications for Toe Amputation
Diabetic Osteomyelitis
Osteomyelitis — bone infection — develops when bacteria from a diabetic foot ulcer breach the soft tissue and penetrate to the bone. The infected bone cannot be sterilized with antibiotics alone — the necrotic bone serves as a sequestrum that perpetuates infection despite systemic antibiotic therapy. When osteomyelitis involves a toe or metatarsal head, surgical resection of the infected bone — which typically means removing the affected digit — is required for infection control. Post-operative antibiotic therapy addresses residual soft tissue infection after surgical debridement.
Wet Gangrene from Infection
Wet gangrene — soft tissue death with active bacterial infection — in a toe represents a surgical emergency. The necrotic, infected tissue must be removed urgently to prevent sepsis (life-threatening bloodstream infection) and proximal spread of the necrosis. Toe amputation in this setting is performed emergently, often before complete vascular evaluation, because the immediate life threat from systemic sepsis outweighs the benefit of delaying surgery.
Dry Gangrene from Arterial Occlusion
Dry gangrene — tissue death from complete arterial occlusion without active infection — presents as a black, mummified toe. Unlike wet gangrene, dry gangrene is not an emergency. If the demarcation between viable and non-viable tissue is clear and there is no infection, the gangrene may be allowed to autoamputate (separate spontaneously) or be surgically removed after vascular workup confirms that blood flow to the remaining foot is adequate to support healing.
Surgical Technique: Digital and Ray Amputation
Toe Amputation (Digital Amputation)
A digital amputation removes the toe at the metatarsophalangeal joint level. The skin is incised in a fish-mouth pattern to create viable flaps for closure. The extensor and flexor tendons are cut proximal to the metatarsal head, and the joint is disarticulated. The wound is irrigated thoroughly and closed with sutures or left open for delayed closure depending on infection status. A simple digital amputation creates a small deformity that is well accommodated by standard or extra-depth footwear.
Ray Amputation
A ray amputation removes a toe and its corresponding metatarsal — typically necessary when osteomyelitis or gangrene involves the metatarsal head or shaft rather than just the toe. Fifth ray amputation (removal of the fifth toe and metatarsal) heals well with minimal functional consequence. Central ray amputations (second, third, fourth) create a gap in the forefoot that requires footwear modification and custom orthotic accommodation for optimal gait mechanics.
Post-Amputation Care and Rehabilitation
The wound requires careful postoperative management — daily dressing changes, suture removal at two to three weeks when appropriate, and protection from pressure while healing progresses. The goal is primary wound closure over two to four weeks for simple digital amputations in patients with adequate circulation. Patients with significant PAD may experience delayed healing and require vascular surgery consultation.
After healing, custom-molded shoes or extra-depth therapeutic footwear with toe filler prosthetics accommodate the amputation and maintain foot function. Gait training with a physical therapist helps patients adapt their weight distribution and stride mechanics after forefoot amputation. The majority of patients with isolated digital or ray amputations walk comfortably and maintain independence with appropriate footwear.
Prevention Is the Goal
Every toe amputation represents a preventable event in most cases. Regular diabetic foot monitoring, early wound evaluation, aggressive treatment of infections before bone involvement occurs, and optimization of vascular supply prevent the progression that makes amputation necessary. If you have diabetes, contact Balance Foot & Ankle to establish regular preventive care. If you have an active wound, contact us immediately for evaluation — early intervention saves toes, feet, and lives.
Ready to Relieve Your Foot Pain?
Board-certified podiatrists serving Southeast Michigan. Same-week appointments available.
Book Your AppointmentToe Amputation & Diabetic Wound Care at Balance Foot & Ankle
When conservative wound care is insufficient, toe amputation may be necessary to prevent life-threatening infection. Dr. Tom Biernacki at Balance Foot & Ankle provides compassionate surgical care and rehabilitation at our Howell and Bloomfield Hills offices.
Learn About Our Diabetic Wound Care Services | Book Your Appointment | Call (810) 206-1402
Clinical References
- Izumi Y, et al. “Risk of reamputation in diabetic patients stratified by limb and level of amputation.” Diabetes Care. 2006;29(3):566-570.
- Thorud JC, et al. “Mortality after nontraumatic major amputation among patients with diabetes and peripheral vascular disease.” Journal of Foot and Ankle Surgery. 2016;55(6):1218-1226.
- Armstrong DG, et al. “Off-loading the diabetic foot wound: a randomized clinical trial.” Diabetes Care. 2001;24(6):1019-1022.
Insurance Accepted
BCBS · Medicare · Aetna · Cigna · United Healthcare · HAP · Priority Health · Humana · View All →
Howell Office
3980 E Grand River Ave, Suite 140
Howell, MI 48843
Get Directions →
Bloomfield Hills Office
43700 Woodward Ave, Suite 207
Bloomfield Hills, MI 48302
Get Directions →
Your Board-Certified Podiatrists
Ready to Get Back on Your Feet?
Same-week appointments available at both locations.
Book Your AppointmentWatch Dr. Tom on Toe Amputation
Dr. Tom on toe amputation surgery — when it’s life-saving in diabetes, wound healing, offloading, prevention of further loss.
Post-Amputation Foot Kit
Toe amputation changes foot biomechanics. These four items protect the remaining foot and prevent further loss:
Eucerin Advanced Repair Foot Cream
Daily skin preservation becomes critical after amputation — increased risk of further skin breakdown.
Check Amazon Price →Extra-Depth Diabetic Shoe
Prescriptive footwear with toe filler — restores biomechanical balance and prevents pressure on remaining toes.
Check Amazon Price →Custom-Fit Pressure-Redistribution Insole
Multi-density foam — essential pressure redistribution to prevent new ulcers on the altered foot.
Check Amazon Price →Antimicrobial Foot Spray
Daily prevention of bacterial/fungal overgrowth on the compromised foot.
Check Amazon Price →Affiliate disclosure: Amazon links are affiliate links — we earn a small commission if you buy through them. We only recommend products we actually prescribe to patients at Balance Foot & Ankle.
Related from Balance Foot & Ankle
In Our Clinic
Diabetic neuropathy patients in our clinic often don’t realize they have it until we put a 10-gram Semmes-Weinstein monofilament to the plantar foot and they can’t feel it. Many arrive for an unrelated concern — an ingrown toenail, a callus — and we catch the neuropathy on screening. The conversation then shifts: we need to discuss daily foot inspections, appropriate footwear, the urgency of any blister or open area, and the timing of vascular referral if pulses are diminished. Comprehensive diabetic foot exams are covered by Medicare annually. If you have diabetes, we want to see you once a year even if nothing hurts.
More Podiatrist-Recommended Diabetic Essentials
Diabetic-Approved Walking Shoe
- Tie-Less Lacing System eliminates the need to tie laces. Heel strap enables to adjust the grip around the heel. Cushioning sole with a mild Rocker adds spring to your step. Soft, padded fabric interior with no overlays eliminates irritation.
Orthofeet Sprint — seamless, extra-depth, designed for neuropathic feet.
Seamless Diabetic Sock
- Provides continuous support of the Plantar Fascia by gently stretching the fascia tissue.
- Compression zones promote circulation, reduce impact vibration, boost recovery and strengthen feet.
- Lightweight, seamless design with extra cushioning provides support while still being comfortable.
- Supports the heel/arch and overall foot structure while stabilizing the tendon for better performance
- Made from high quality materials, the socks are moisture wicking and breathable.
OS1st FS4 — non-binding, moisture-wicking, protects fragile diabetic skin.
Recovery Slide for Indoor Wear
- Model ID: 1135061-BTRT
HOKA Ora 3 — protects diabetic feet from barefoot injury at home.
As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. Product recommendations are based on clinical experience; prices and availability shown above update live from Amazon.
Watch: Diabetes Peripheral Neuropathy Treatment [Diabetic Nerve Pain Remedy] — MichiganFootDoctors YouTube
When to See a Podiatrist
One unnoticed blister on a neuropathic foot can become a limb-threatening ulcer in under 14 days. Medicare covers diabetic shoes (A5500) and comprehensive foot exams annually for most diabetic patients with neuropathy or circulation concerns. Balance Foot & Ankle runs a dedicated diabetic limb-preservation program — vascular screening, offloading, ulcer care, and shoe fitting — all in one visit. Schedule your annual diabetic foot exam today.
Call Balance Foot & Ankle: (810) 206-1402 · Book online · Offices in Howell & Bloomfield Hills
In-Office Treatment at Balance Foot & Ankle
If home treatment isn’t providing relief for your diabetic foot conditions, our podiatry team at Balance Foot & Ankle can help with same-day evaluations and advanced in-office care.
Same-day appointments available. (810) 206-1402
Doctor Hoy’s Natural Pain Relief Gel
Natural topical pain relief I use in our clinic. Arnica + camphor formula — apply directly to the area 3–4x daily. ($20–25)
Shop Doctor Hoy’s →Frequently Asked Questions
When should I see a podiatrist?
If symptoms persist past 2 weeks, affect your normal activity, or are accompanied by red-flag symptoms (warmth, redness, swelling, inability to bear weight).
What does treatment cost?
Most diagnostic visits and conservative treatments are covered by Medicare and major insurers. Out-of-pocket costs vary by your specific plan.
How quickly can I get an appointment?
Most non-urgent cases see us within 5 business days. Urgent cases (sudden pain, possible fracture) typically same or next business day.
What is Diabetic foot?
Diabetic foot is a common foot/ankle condition that affects mobility and quality of life. Understanding the underlying cause is the first step in successful treatment. Our podiatrists at Balance Foot & Ankle perform a hands-on biomechanical exam, review your activity history, and use diagnostic imaging when appropriate to identify the root cause—not just treat the symptom. Many patients have been told to “rest and ice” without a deeper diagnostic workup; our approach is different.
Symptoms and warning signs
Common signs of diabetic foot include pain that worsens with activity, morning stiffness, swelling, tenderness when palpated, and difficulty bearing weight. If you experience sudden severe pain, inability to walk, visible deformity, numbness or color change, contact our office the same day or visit urgent care—these can signal a more serious injury such as a fracture, tendon rupture, or vascular compromise. Diabetics with any foot wound should seek same-day care.
Conservative treatment options
Most cases of diabetic foot respond to non-surgical care: structured rest, supportive footwear changes, custom orthotics, targeted stretching and strengthening protocols, anti-inflammatory medications when medically appropriate, and in-office procedures such as ultrasound-guided injections. We also offer advanced therapies including MLS laser therapy, EPAT/shockwave, regenerative injections, and image-guided procedures. Treatment is sequenced from least invasive to most invasive, and we explain the rationale at every step.
When is surgery considered?
Surgery is reserved for cases that fail 3-6 months of well-structured conservative care, when there is structural pathology (severe deformity, complete tear, advanced arthritis), or when imaging shows damage that will not heal without intervention. Our surgeons have performed 3,000+ foot and ankle procedures and prioritize minimally-invasive techniques whenever appropriate. We discuss recovery timelines, return-to-activity milestones, and realistic outcome expectations before any procedure is scheduled.
Recovery timeline and prevention
Recovery from diabetic foot varies based on severity and chosen treatment path. Conservative cases often improve within 4-8 weeks with consistent adherence to the protocol. Post-procedural recovery may range from a few days (in-office procedures) to several months (reconstructive surgery). Long-term prevention involves footwear assessment, activity modification, structured strengthening, and regular check-ins with your podiatrist if you have a history of recurrence. We provide written home-exercise plans and digital follow-up support.
Ready to feel better?
Same-week appointments available in Howell and Bloomfield Hills, Michigan.
Book Your VisitDr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.










![Diabetes Peripheral Neuropathy Treatment [Diabetic Nerve Pain Remedy]](https://www.michiganfootdoctors.com/wp-content/cache/flying-press/83886306c119511909f4e50d00e25908.jpg)