Same-Week Appointments at Balance Foot & Ankle
Three board-certified podiatric surgeons. 950K+ YouTube subscribers. 1,123+ five-star reviews. Howell & Bloomfield Hills, Michigan.
Best Sesamoiditis Insoles & Forefoot Pads 2026: Podiatrist Guide to Ball-of-Foot Pain Under the Big Toe
👨⚕️ Reviewed by Dr. Tom Biernacki, DPM — Balance Foot & Ankle Specialists, Howell, Michigan
Sesamoiditis is one of the most frequently misdiagnosed forefoot pain conditions I encounter — patients come in having been told they have a stress fracture, Morton’s neuroma, or simply “ball of foot pain,” when the real culprit is inflammation of the sesamoid bones or their surrounding tendons beneath the first metatarsophalangeal joint. The two sesamoid bones — each about the size of a corn kernel — sit within the flexor hallucis brevis tendons beneath the first MTP joint and serve as a pulley system for the great toe, multiplying the mechanical force of toe-off during walking and running. When these bones or their surrounding soft tissue become inflamed through repetitive loading, acute trauma, or biomechanical overload, the result is a deep, aching or sharp pain directly under the big toe joint that worsens with activity and is dramatically aggravated by barefoot walking or any pressure on the ball of the foot. The cornerstone of conservative management is offloading — shifting weight away from the sesamoids with targeted pads, dancer’s cushions, and supportive insoles. The six products reviewed on this page are the best available options for doing exactly that. Amazon affiliate links are used; I earn a small commission at no extra cost to you. Clinical opinions are independent.
⚡ Quick Answer: Top 6 Sesamoiditis Products in 2026
- HAPAD Dancer’s Pads — Best Overall: the gold-standard J-shaped sesamoid offloading pad used in podiatry clinics
- Powerstep Pinnacle Arch Support Insoles — Best Full Insole: firm arch support + forefoot cushioning layer for comprehensive sesamoid offloading
- Tuli’s Gel Heel Cups — Best Shock Absorber: reduces peak impact at heel strike, indirectly reducing forefoot loading
- Spenco Total Support Max Insoles — Best for Flat Feet with Sesamoiditis: deep heel cup controls pronation that overloads the first MTP joint
- Biofreeze Pain Relief Spray — Best Topical: cold-activated menthol pain relief for post-activity sesamoid pain management
- Pedag Comfort Insole — Best Dress Shoe Option: slim-profile support that fits in lower-volume footwear
Full reviews, the science of sesamoid offloading, and Dr. Tom’s complete management protocol follow below.
Treatment at Balance Foot & Ankle: Morton's Neuroma Treatment →
Understanding what sesamoiditis is — and what it is not — is essential before selecting a treatment product. The sesamoids are not “floating” bones as commonly described; they are embedded within tendon tissue and bear up to three times body weight during the push-off phase of running. Sesamoiditis is an overuse injury caused by repetitive compressive and tensile forces exceeding the tissue’s adaptive capacity. It is most common in runners, dancers (particularly ballet), athletes who perform repeated jumping, and patients with a cavus (high-arched) foot type that increases plantar pressure under the first metatarsal head. It is frequently bilateral in patients with structural foot deformities but typically presents on the dominant foot or the foot of the dominant limb in athletes.
Before selecting any product on this page, it is important to confirm the diagnosis. Not all pain under the first MTP joint is sesamoiditis. Differential diagnosis includes: sesamoid stress fracture or avulsion fracture (requires weight-bearing X-ray and possibly MRI), first MTP joint arthritis or synovitis, turf toe (a sprain of the plantar plate), flexor hallucis longus tendinopathy, and a bipartite sesamoid (a normal anatomical variant where one sesamoid is in two segments, sometimes mistaken for a fracture). A podiatric evaluation including X-ray is strongly recommended before committing to a conservative management protocol — the appropriate product selection differs slightly depending on whether the primary pathology is bony stress, tendon irritation, or soft tissue inflammation.
That said — for confirmed sesamoiditis or for patients awaiting their appointment — the offloading products on this page represent the best-evidenced conservative measures currently available, and most clinically significant improvement in sesamoiditis occurs within 6–12 weeks of consistent offloading combined with activity modification. Let’s look at the products that do this best.
Sesamoiditis is one of the most underdiagnosed sources of ball-of-foot pain in active adults. Unlike most foot pain that originates from bone spurs, plantar fascia tears, or nerve compression, sesamoiditis targets two tiny floating bones buried beneath your big toe joint — bones so small they are rarely discussed in general medicine yet so critical that their malfunction can ground runners, dancers, and athletes for months. Understanding exactly what sesamoids do, why they become inflamed, and how the right orthotic device can dramatically accelerate recovery is the foundation of every successful conservative treatment plan.
The Biomechanics of Sesamoid Pain: Why These Two Tiny Bones Cause So Much Trouble
The medial and lateral sesamoids sit within the flexor hallucis brevis tendon beneath the first metatarsophalangeal (MTP) joint — the joint at the base of the big toe. Anatomically, they function like mini pulleys: they redirect the tendon force generated when you push off the ground, multiplying the mechanical advantage of the big toe flexors. Without sesamoids, the big toe would lose roughly 40% of its push-off power. With them, the forefoot delivers explosive force with every step, sprint, and jump.
The problem is that this load-bearing role is relentless. Each time your heel rises and your weight transfers onto the ball of the foot, the sesamoids absorb ground reaction forces that can reach two to three times body weight. In a 160-pound runner logging 30 miles per week, that translates to millions of high-force compression cycles per month. Add a rigid forefoot, a high-arched foot, dancing on hard floors, or a sudden spike in training volume, and the bones and surrounding soft tissue begin to break down faster than the body can repair them.
Sesamoiditis exists on a spectrum. Early-stage sesamoiditis is purely inflammatory — the periosteum and surrounding tendon sheath become irritated without structural damage. Moderate sesamoiditis involves micro-stress reactions within the bone itself, visible on MRI as bone marrow edema. Advanced cases can progress to stress fractures, avascular necrosis, or bipartite sesamoid fragmentation that requires surgical intervention. Catching the condition at stage one and providing proper mechanical offloading with the right insole or forefoot pad is what prevents the 3-month recovery from becoming a 12-month ordeal.
Who Gets Sesamoiditis Most Often?
While sesamoiditis can affect anyone who spends significant time on their feet, specific populations carry dramatically higher risk. Ballet dancers represent the highest-risk group — performing in pointe shoes shifts nearly all body weight through the sesamoids in a position of maximum plantarflexion. Distance runners, particularly those who run on their forefoot or mid-foot, apply repetitive high-force loading to the sesamoid complex with every stride. Baseball catchers spend long periods squatting with the forefoot loaded. Athletes who wear cleated footwear on artificial turf — where the forefoot cannot plantarflex naturally into the ground — experience elevated compressive forces at the first MTP joint.
Beyond athletic populations, high-heel wearers, individuals with cavus (high-arched) foot types, and people with hypermobile first rays (where the first metatarsal moves excessively during push-off) all face elevated baseline sesamoid stress. Interestingly, some patients with bipartite sesamoids — a congenital variant where one sesamoid forms in two segments — mistakenly receive a sesamoid fracture diagnosis, when in reality their anatomy has always been that way. An experienced podiatrist can differentiate through comparison X-rays and clinical history.
Watch: Sesamoiditis Explained by Dr. Tom Biernacki
Before we review the specific products, watch Dr. Tom’s comprehensive video on sesamoiditis — covering anatomy, diagnosis, taping techniques, offloading strategies, and when conservative care is enough versus when imaging is needed.
The Podiatrist’s Framework for Selecting a Sesamoid Offloading Device
Not every forefoot pad or insole is appropriate for sesamoiditis. The primary mechanical goal is to reduce compressive and shear forces at the first MTP joint while preserving normal gait mechanics. This requires understanding four design principles that separate therapeutic sesamoid products from generic cushioning.
Principle 1 — Metatarsal Offloading, Not Metatarsal Compression. A metatarsal pad placed directly under the sesamoids will worsen pain. The pad must sit just proximal (behind) to the metatarsal heads, creating a gentle “dome” that redistributes forefoot pressure across the second through fourth metatarsals while creating a protected valley beneath the first metatarsal and sesamoids. Pad placement is everything. A 3mm mismatch in positioning can mean the difference between significant relief and increased pain.
Principle 2 — Appropriate Shore Hardness. Extremely soft materials (silicone gels below 15 Shore A) initially feel comfortable but bottom out under load, providing minimal true mechanical offloading. Materials in the 20–40 Shore A range — like EVA foam composites, high-density felt, and medical-grade polyurethane foam — provide sustained pressure distribution throughout the gait cycle without collapsing under body weight.
Principle 3 — First Ray Stabilization. Many sesamoiditis patients have a hypermobile first ray — the first metatarsal drops and rises excessively with each step, creating abnormal sesamoid shear. An insole with a medial arch support component stabilizes the first ray, preventing excessive motion that aggravates the sesamoid tendon interface.
Principle 4 — Appropriate Stiffness in the Toe Box Region. A rigid or semi-rigid toe plate (Morton’s extension concept applied inversely) limits first MTP dorsiflexion during push-off, dramatically reducing the compressive load on the sesamoids. Shoes with rocker soles or carbon fiber plates built into athletic footwear achieve this at the shoe level; insoles with a stiff forefoot section achieve it at the insole level.
With these four principles as our guide, here are the six sesamoiditis-specific products Dr. Tom most frequently recommends to patients — ranked by clinical scenario and use case.
Product Reviews: Best Sesamoiditis Insoles & Forefoot Pads 2026
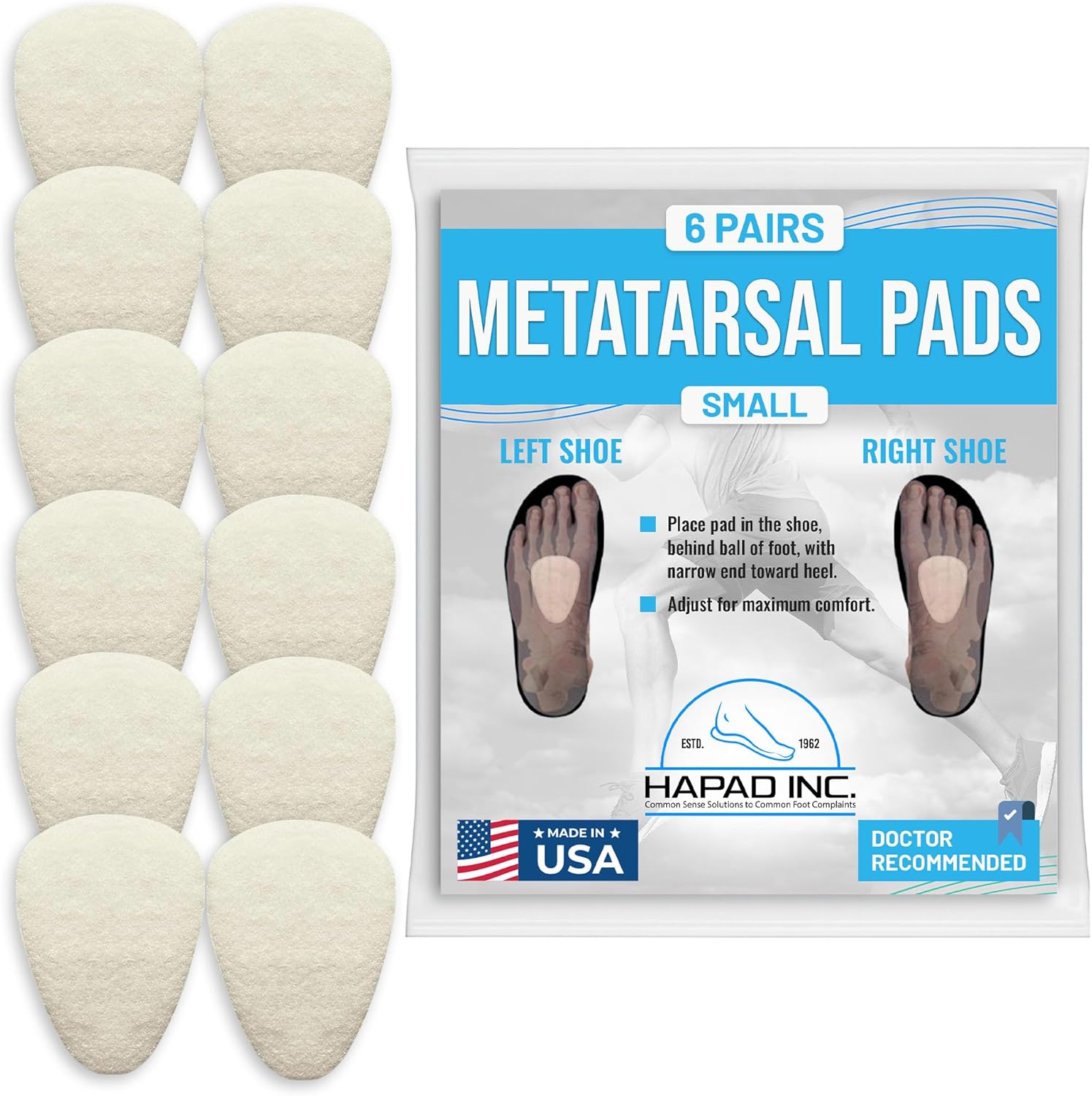
HAPAD Dancer’s Pads — The Gold Standard for Sesamoid Offloading
Best for: Dancers, runners with acute sesamoiditis, post-cortisone injection recovery, patients who need precise pad placement under clinical supervision
HAPAD Dancer’s Pads have been in podiatric practice for decades for a very specific reason: they work. These are not generic moleskin or silicone gel dots. HAPAD uses a coiled, spring-like wool fiber construction (their proprietary Coiled Spring Fiber technology) that provides consistent, graduated compression resistance throughout the gait cycle. Unlike foam pads that flatten after a few uses, the coiled fiber structure maintains its mechanical properties across hundreds of use cycles, making these pads genuinely therapeutic rather than simply cushioning.
The “dancer’s pad” cut is the critical feature here. The horseshoe-shaped design has a specific notch that wraps around the sesamoids rather than sitting under them — exactly the offloading geometry described in Principle 1 above. When properly positioned just proximal to the first metatarsal head, the pad creates a protected valley that allows the sesamoid complex to function without bearing direct ground reaction force. This is the same pad design used in professional ballet companies and by most sports medicine podiatrists treating high-level athletes.
Application is straightforward: clean and dry the ball of the foot, peel the self-adhesive backing, position the notch so it sits behind the first metatarsal head (you will feel the pad making contact just proximal to the sore area), and press firmly for 30 seconds. Apply directly to the foot for maximum precision, or to the insole of your shoe if you prefer to move the pad between footwear. One package provides multiple pads, which is important because the adhesive weakens after 3–5 days of regular use and pads should be replaced to maintain optimal positioning.
In clinical experience, HAPAD Dancer’s Pads produce noticeable pain reduction within the first 48–72 hours of consistent use in acute sesamoiditis cases. For stress fractures or advanced bone marrow edema, they remain part of the conservative protocol but work alongside immobilization and activity restriction rather than replacing it.
- Precise horseshoe cut designed specifically for sesamoid offloading geometry
- Coiled spring fiber maintains mechanical properties across many use cycles
- Self-adhesive — applies directly to foot or insole
- Used by professional dancers and sports medicine podiatrists worldwide
- Available in multiple sizes (small, medium, large)
- Appropriate for most shoe types including athletic, dress, and dance footwear
- Adhesive weakens after 3–5 days — pads must be replaced regularly
- Requires correct placement to work — misapplication reduces effectiveness
- Higher cost per-pad than generic foam alternatives
- Wool fiber may irritate very sensitive skin in rare cases
Powerstep Pinnacle — Full Orthotic Support with Forefoot Cushion Platform
Best for: Runners and active adults who need full foot support beyond just forefoot padding, patients with sesamoiditis combined with plantar fasciitis or arch strain, those who want an all-day insole that addresses multiple forefoot load drivers simultaneously
When sesamoiditis coexists with arch fatigue, plantar fascia irritation, or a dropped medial longitudinal arch — which is more common than isolated sesamoid involvement — a targeted forefoot pad alone will not address the full mechanical picture. The Powerstep Pinnacle is the full-length insole that most frequently earns a place in the treatment protocol because it combines three clinically relevant features: a semi-rigid polypropylene shell that controls first-ray hypermobility, a dual-layer EVA foam forefoot platform with metatarsal ridge positioning, and a deep heel cup that corrects the rearfoot pronation that often drives excessive forefoot load.
The Pinnacle’s metatarsal ridge is positioned just behind the metatarsal heads — proximal enough to genuinely offload the ball-of-foot region rather than compress it. The dual-layer foam uses a firmer base layer (40 Shore A) topped by a softer comfort layer (25 Shore A), creating the progressive compression resistance that maintains offloading integrity throughout the stance phase. For runners, this means the insole continues to protect the sesamoid area at the moment of peak forefoot load — toe-off — rather than bottoming out when protection matters most.
Compatibility is excellent — the Pinnacle fits most athletic shoes and most low-profile casual footwear with a removable factory insole. Remove the factory insole before inserting the Powerstep to avoid stacking two insoles (which raises the foot inside the shoe and creates a different set of problems). The heel cup depth (approximately 14mm) provides enough motion control to meaningfully reduce first-ray hypermobility in most patients without requiring a custom prescription orthotic as a first-line intervention.
Clinical expectations: most patients with early-to-moderate sesamoiditis and arch involvement notice measurable improvement in ball-of-foot pain within 2–3 weeks of consistent use in appropriate footwear. The Pinnacle does not replace dancer’s pads for precise first-MTP offloading, but it addresses the full-foot mechanical context that dancer’s pads alone cannot.
- Semi-rigid shell controls first-ray hypermobility — a key sesamoiditis driver
- Dual-layer EVA maintains offloading integrity at peak load (toe-off)
- Metatarsal ridge positioned correctly proximal to metatarsal heads
- Deep heel cup addresses rearfoot pronation component
- Fits most athletic and casual footwear
- More affordable than custom orthotics; highly effective for early/moderate cases
- Does not fit narrow dress shoes, heels, or some fashion footwear
- Semi-rigid shell may feel firm initially — requires 1–2 week break-in period
- Does not provide the precise horseshoe cutout of HAPAD dancer’s pads
- Not recommended as sole intervention for severe sesamoiditis or stress fractures
Tuli’s Gel Heel Cups — Forefoot Shock Absorption for High-Impact Recovery
Best for: Patients who need maximum forefoot shock absorption during the return-to-activity phase, those with sesamoiditis triggered by hard-surface training (concrete, asphalt, tile), individuals who find rigid orthotics uncomfortable and prefer a softer cushioning approach
Tuli’s Waffle Gel pads deserve their own section in this guide even though their name suggests heel focus — the same waffle-grid gel technology performs exceptionally well as a forefoot cushion platform when used as a full-length or three-quarter-length pad beneath the forefoot. The medical-grade silicone used in Tuli’s products has a durometer rating in the sweet spot for forefoot protection: firm enough to resist compression bottoming under body weight, soft enough to attenuate the high-frequency vibration and impact forces that aggravate inflamed sesamoid periosteum during early recovery.
The waffle grid geometry is functionally significant. Rather than a flat silicone sheet, the grid creates alternating columns and channels that allow the material to deform locally in response to bony prominences (like the sesamoid complex) while the surrounding grid columns maintain structural support. The net effect is a dynamic cushioning system that conforms to foot anatomy rather than imposing a uniform pressure across the entire plantar surface — which is precisely what sesamoiditis patients need during the return-to-walking phase when every step must minimize first MTP joint compression.
Tuli’s gel products are machine washable and reusable across many months of use, making them significantly more economical than adhesive foam pads for patients who need ongoing protection during a gradual return to training. They are thin enough to fit inside most athletic and casual shoes alongside the factory insole, and their grippy silicone surface prevents migration within the shoe — a critical practical feature for patients who cannot afford the distraction of shifting insole hardware mid-stride.
Note for clinical use: Tuli’s gel pads provide excellent shock attenuation but do not provide the proximal-to-metatarsal-head positioning geometry of HAPAD dancer’s pads. For acute sesamoiditis requiring precise offloading, pair Tuli’s forefoot gel with a HAPAD dancer’s pad for both shock attenuation and precise mechanical offloading. For return-to-activity phases where pain has largely resolved and the goal is prevention of recurrence, Tuli’s gel alone is often sufficient.
- Medical-grade silicone with waffle-grid geometry for dynamic forefoot cushioning
- Machine washable and reusable — economical for long-term protection
- Thin profile fits inside most athletic and casual footwear
- Non-slip surface prevents migration during activity
- Excellent shock attenuation on hard surfaces (concrete, tile, asphalt)
- Available in multiple sizes and configurations
- Does not provide the targeted horseshoe cutout geometry for acute offloading
- Heavier than foam alternatives — may feel bulky in slim footwear
- Silicone can feel warm during prolonged use in hot conditions
- Best used in return-to-activity phase; pair with dancer’s pads for acute cases
Spenco Total Support Max — Maximum Motion Control for Hypermobile First Ray
Best for: Patients with significant overpronation and hypermobile first ray contributing to sesamoiditis, those who have tried softer insoles without adequate relief, individuals who need prescription-grade motion control in an over-the-counter product
The Spenco Total Support Max occupies a distinct clinical position in sesamoiditis management: it is the highest-rigidity, maximum-motion-control over-the-counter insole available without a custom prescription. For patients in whom sesamoid pain is directly driven by first-ray hypermobility — where the first metatarsal drops significantly into pronation during the midstance phase, creating abnormal sesamoid shear — a softer, cushion-focused insole may actually fail to provide meaningful relief because it does not address the underlying mechanical cause.
The Spenco Max uses a polyethylene foam frame with an embedded polypropylene stabilizer that is stiffer than most OTC options but still significantly more flexible than custom orthotics. The medial arch is high and firm, providing aggressive subtalar joint control that limits first-ray plantarflexion during gait. The metatarsal support ridge is positioned to transfer load proximal to the metatarsal heads. The forefoot platform layer is a Spenco polysorb material — a proprietary closed-cell foam that provides consistent density even after extended use, avoiding the flattening issue common in standard EVA insoles.
Patient selection for this insole is important: the Spenco Max works best in patients with moderate-to-severe overpronation (visible arch collapse during standing) and documented first-ray hypermobility. Patients with cavus (high-arched, rigid) foot types, neutral arches, or supination tendencies should not use maximum motion-control insoles, as these will overcorrect gait and create new mechanical stress. When in doubt, a brief in-office gait evaluation with your podiatrist before purchasing will clarify whether the Max is appropriate for your foot type.
The Total Support Max fits most athletic footwear with a roomy toe box and a removable factory insole. Its stiffer frame makes it less compatible with low-volume shoes, cycling shoes, or dress footwear. Expect a meaningful break-in period of 7–10 days as the foot and musculature adapt to the increased motion control — mild arch fatigue in the first week is normal and typically resolves as the foot adjusts to the corrected alignment.
- Highest OTC motion control — addresses first-ray hypermobility directly
- Embedded polypropylene stabilizer provides prescription-grade arch support
- Polysorb forefoot material maintains density after extended use
- Metatarsal ridge positioned proximal to metatarsal heads
- Excellent for patients where pronation is the primary sesamoiditis driver
- Available in full range of sizes
- Not appropriate for high-arched or neutral foot types — may overcorrect
- 7–10 day break-in period required; initial arch fatigue is common
- Stiffer frame does not fit narrow or low-volume footwear
- Heavier than foam-only alternatives
Biofreeze Professional Pain Relief Spray — Targeted Cryotherapy for Acute Sesamoid Inflammation
Best for: Acute sesamoiditis pain management, post-activity inflammation control, patients who cannot tolerate oral NSAIDs, athletes managing pain between training sessions during a structured return-to-sport protocol
Mechanical offloading through insoles and pads addresses the structural cause of sesamoiditis, but it does not immediately eliminate the inflammatory pain response that has already been established. Biofreeze Professional Spray fills this gap as the most widely used topical analgesic in sports medicine and podiatric practices — and the spray format is specifically advantageous for the sesamoid region because it allows precise delivery to the plantar surface of the forefoot without requiring direct finger pressure on an already painful area.
Biofreeze’s active mechanism is TRPM8 receptor activation — the same cold-sensing pathway that menthol triggers in skin. This activates a counter-irritation response (gate control theory of pain) that reduces nociceptive signal transmission from the inflamed sesamoid periosteum and surrounding soft tissue. The clinical benefit is meaningful but temporary: most patients experience 2–4 hours of significant pain reduction per application, creating a window for gentle range-of-motion exercises, physical therapy interventions, or low-intensity activity without the dose-dependent risks associated with oral NSAIDs.
Application protocol for sesamoiditis: apply 2–3 sprays to the plantar forefoot surface directly overlying the first metatarsal head and allow to air dry for 30 seconds. Do not cover immediately with socks — allow the menthol to penetrate and activate the cooling response. Apply before morning activity (when sesamoiditis pain is typically worst after the first steps), after any activity that has loaded the forefoot, and before physical therapy sessions when range-of-motion work will be performed on the first MTP joint. Do not apply under heat or compression immediately following, as this intensifies the cold sensation to an uncomfortable level.
Biofreeze is not a substitute for mechanical offloading — it manages symptoms while the structural interventions do the heavy lifting of reducing the underlying mechanical cause. Used together (insole for offloading, Biofreeze for pain control), most early-stage sesamoiditis patients can maintain a meaningful level of daily activity while the periosteal inflammation resolves over the 6–8 week conservative treatment window.
- Spray format allows contactless application to painful plantar surface
- 2–4 hours of significant pain relief per application
- TRPM8 receptor mechanism — no absorption risk like topical NSAIDs
- Professional-grade formulation used in sports medicine and podiatry practices
- Safe to use alongside oral medications (no systemic interaction)
- Menthol scent dissipates quickly — practical for daytime use
- Temporary relief only — does not address structural cause
- Strong menthol sensation may be intense for first-time users
- Should not be applied under heat or compression immediately after
- Some patients find the cold sensation uncomfortable on the plantar surface
Pedag Comfort Insole — European-Engineered Leather & Foam for Dress & Fashion Footwear
Best for: Patients who need sesamoid protection in dress shoes, loafers, Oxford shoes, or fashion footwear where bulkier athletic insoles will not fit, professionals who cannot switch to athletic footwear during recovery, those who prioritize breathability and natural materials
One of the most overlooked challenges in sesamoiditis management is footwear compliance. Patients who work in professional environments — where dress shoes, heels, or fashion footwear are expected — often cannot simply switch to running shoes during their 6–8 week recovery period. Standard athletic insoles are too thick and structurally incompatible with low-volume dress footwear. This is where Pedag’s slim-profile leather and foam construction fills a genuine clinical gap.
Pedag Comfort Insoles from Germany use a combination of vegetable-tanned leather on the top surface and layered EVA foam with a latex metatarsal support pad to create an insole thin enough (typically 4–6mm total depth) to fit inside most dress shoes, Oxford shoes, ballet flats, and loafers without raising the foot significantly within the shoe. The metatarsal support pad — a small raised dome positioned just proximal to the metatarsal heads — provides the same load redistribution principle as the Powerstep Pinnacle’s metatarsal ridge but in a format compatible with professional footwear.
The leather surface provides natural moisture management superior to synthetic materials, which is relevant for patients who wear dress footwear for 8+ hours per day. The natural leather molds gently to the plantar foot anatomy over the first week of use, creating a semi-custom fit without the cost of custom orthotics. The latex metatarsal support maintains its shape well across months of daily use without the compression fatigue common in purely foam-based pads of similar thickness.
Clinical expectation: the Pedag Comfort provides meaningful but not maximum sesamoid offloading — it is an appropriate protective insole for mild-to-moderate sesamoiditis in dress footwear, or as a maintenance insole during the late recovery phase when pain has largely resolved and the goal is prevention of recurrence. For acute sesamoiditis or stress fractures, mechanical offloading in a rigid-soled athletic shoe with a dancer’s pad remains the primary intervention, and the Pedag serves a complementary role for unavoidable dress shoe occasions.
- 4–6mm slim profile fits dress shoes, loafers, Oxford shoes, ballet flats
- Vegetable-tanned leather top surface — superior breathability and moisture management
- Latex metatarsal support maintains shape over months of use
- Molds to plantar foot anatomy over first week of wear
- Allows sesamoid protection in professional/fashion footwear contexts
- European medical-grade manufacturing standards
- Not appropriate as sole intervention for acute or severe sesamoiditis
- Thin profile means less cushion than full-depth athletic insoles
- Leather surface requires conditioning periodically to prevent cracking
- Higher price point than basic foam alternatives
Side-by-Side Comparison: All 6 Sesamoiditis Products
| Product | Type | Best Use Stage | Shoe Compatibility | Offloading Mechanism | Dr. Tom Rating |
|---|---|---|---|---|---|
| HAPAD Dancer’s Pads | Adhesive forefoot pad | Acute / Active flare | All types (applies to foot) | Horseshoe cutout — proximal metatarsal offloading | ⭐⭐⭐⭐⭐ Clinical gold standard |
| Powerstep Pinnacle | Full-length insole | Subacute / Return to activity | Athletic & casual with removable insole | Semi-rigid shell + metatarsal ridge | ⭐⭐⭐⭐⭐ Best full insole |
| Tuli’s Gel | Gel forefoot pad / insole | Return to activity / Prevention | Most athletic and casual | Waffle-grid shock attenuation | ⭐⭐⭐⭐ Excellent shock absorber |
| Spenco Total Support Max | Full-length insole (max control) | Subacute — high pronation cases | Athletic with roomy toe box | Polypropylene shell + first-ray stabilization | ⭐⭐⭐⭐ Best for overpronators |
| Biofreeze Spray | Topical analgesic | All stages (adjunct only) | N/A (topical) | TRPM8 counter-irritation — symptom control | ⭐⭐⭐⭐ Essential adjunct |
| Pedag Comfort Insole | Slim-profile full insole | Subacute / Maintenance | Dress shoes, loafers, flats | Latex metatarsal dome + leather contouring | ⭐⭐⭐⭐ Best for dress footwear |
More Podiatrist-Recommended Orthotics Essentials
PowerStep Pinnacle
The podiatrist-recommended OTC orthotic — arch support + heel cup.
CURREX RunPro Insole
Performance insole for runners — reduces fatigue and prevents injuries.
Tuli’s Heel Cups
Shock-absorbing heel cushion — adds lift and relief under painful heels.
As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. Product recommendations are based on clinical experience; prices and availability shown above update live from Amazon.
When to See a Podiatrist
Off-the-shelf inserts help 70% of patients — but if you’ve tried several without relief, custom orthotics molded to your specific foot mechanics are usually the next step. Balance Foot & Ankle makes custom orthotics in-office and most major insurance plans cover them. We’ll cast or scan your feet and have them ready in about 2 weeks.
Call Balance Foot & Ankle: (810) 206-1402 · Book online · Offices in Howell & Bloomfield Hills
Frequently Asked Questions: Sesamoiditis Treatment & Products
Early-stage sesamoiditis (pure inflammation, no stress reaction) typically resolves in 4–6 weeks with consistent offloading, activity modification, and anti-inflammatory measures. Moderate sesamoiditis with bone marrow edema on MRI generally requires 8–12 weeks. Sesamoid stress fractures — depending on whether the blood supply to the bone is intact — may take 3–6 months to fully heal and occasionally require surgical intervention if avascular necrosis develops. Starting treatment early, before the condition progresses from inflammatory to structural damage, is the most important factor in reducing recovery time. Most patients who present within the first 2–3 weeks of symptoms resolve fully with conservative care. Those who wait 3+ months and continue loading the forefoot through the inflammatory phase often face more complex, prolonged recoveries.
This is the most common application error and the reason many patients report that “insoles didn’t help” — the pad was placed in the wrong location. For sesamoiditis specifically, the pad must be positioned just proximal (behind) to the first metatarsal head — not under it, not under the sesamoids themselves. The horseshoe cutout of a HAPAD dancer’s pad should open toward the toes, with the U-shaped notch creating a valley beneath the sesamoid complex while the pad’s body sits approximately 5–10mm behind the first metatarsal head. When you press the padded foot against the floor and walk, you should feel the pad making contact on the ball of your foot but not directly under the sore spot. The sore area should feel slightly suspended or unweighted. If pressure increases over the painful area, the pad is too far forward and needs to be moved 3–5mm proximally (toward the heel).
This depends entirely on the severity of your sesamoiditis. With early-stage inflammatory sesamoiditis, modified running — on soft surfaces, at reduced intensity and volume, with a HAPAD dancer’s pad and a rigid-plate shoe (such as a carbon fiber plated racing shoe or a rocker-bottom shoe that limits first MTP dorsiflexion) — may be possible without worsening the condition. Ground reaction forces at push-off in running reach 2.5–3× body weight compared to approximately 1.2× for walking, so the reduction in force per step is significant when transitioning to walking during the recovery period. For moderate sesamoiditis with bone marrow edema or any stress fracture involvement, continued running directly delays healing and significantly increases the risk of progression to avascular necrosis. A 4–6 week running pause is far better than a 12-month recovery from a failed sesamoid. When in doubt, get an MRI — it is the only imaging modality that definitively characterizes whether bone marrow changes are present.
Sesamoiditis is an overuse inflammatory syndrome affecting the sesamoid bones and the surrounding periosteum, tendons, and joint capsule — without structural disruption of the bone itself. On X-ray, the sesamoids appear normal or show only minor sclerosis. On MRI, there may be mild edema in the sesamoid but no fracture line. A sesamoid stress fracture involves actual disruption of the cortical bone, visible on MRI as a fracture plane and associated bone marrow edema — though often not visible on plain X-ray until later stages. Treatment differences are meaningful: sesamoiditis is managed with activity modification, offloading, and anti-inflammatory measures while remaining ambulatory. A true sesamoid stress fracture typically requires a period of non-weight-bearing in a boot or cast (4–6 weeks), followed by a gradual return to activity. Continuing to run or walk heavily on a stress fracture extends healing significantly and risks progressing to avascular necrosis (bone death) — a situation that may ultimately require surgical sesamoid excision. Getting an MRI within 2–3 weeks of symptom onset if pain is significant and not improving is strongly recommended for any athlete or active individual.
For mild ball-of-foot pain that has been present for less than 2 weeks and is not severe, a trial of OTC offloading products is reasonable. Begin with HAPAD dancer’s pads applied correctly just proximal to the first metatarsal head, switch to supportive footwear with a stiff sole and roomy toe box, and reduce forefoot-loading activities. If pain is not improving after 2 weeks of consistent conservative measures, or if pain is severe enough to significantly alter your gait, or if there is visible swelling, bruising, or warmth at the ball of the foot — schedule a podiatry appointment promptly. An X-ray is the minimum imaging needed to rule out a bipartite sesamoid misdiagnosed as a fracture, and MRI is needed to rule out stress fracture and avascular necrosis in athletes who have continued training through significant pain. The OTC products on this list are appropriate adjuncts to professional care, not substitutes for it in moderate-to-severe cases.
- Severe pain that prevents normal walking — may indicate stress fracture requiring imaging and possible immobilization
- Visible swelling, warmth, or redness at the ball of the foot — rule out infection, gout, or bursitis before self-treating
- Pain in a child or teenager — growth plate involvement must be excluded before any loading is allowed
- Pain that has been present for more than 4–6 weeks without improvement — stress fracture and early avascular necrosis must be ruled out with MRI
- Numbness, tingling, or burning in the ball of the foot or toes — may indicate nerve involvement (Morton’s neuroma, digital nerve compression) requiring separate evaluation
- History of diabetes, peripheral neuropathy, or vascular disease — self-treatment of foot pain carries significantly elevated risk; all foot pain in this population warrants professional evaluation
The Complete Sesamoiditis Offloading Protocol: A Step-by-Step Guide
Product selection is only one component of effective sesamoiditis management. How and when you use these products — and in what combination — determines whether you achieve the 6–8 week recovery typical of well-managed early-stage sesamoiditis or the prolonged 4–6 month ordeal common in poorly managed cases. This protocol represents the conservative management framework used in our clinic at Balance Foot & Ankle Specialists in Howell, Michigan, adapted for self-management with OTC products.
Phase 1: Acute Management (Weeks 1–2)
The primary goal in Phase 1 is halting the inflammatory cascade while maintaining some mobility. Complete rest is rarely appropriate or necessary for early-stage sesamoiditis — immobility creates its own problems including stiffness, muscle atrophy, and gait compensations that produce secondary problems in the knee and hip. Instead, focus on controlled activity reduction combined with aggressive mechanical offloading.
Daily protocol for Phase 1: Apply a fresh HAPAD dancer’s pad to the plantar surface of the forefoot just proximal to the first metatarsal head each morning before the first steps of the day. Apply Biofreeze spray to the painful forefoot 15–20 minutes before any walking activity. Wear footwear with a rigid, rockered sole — running shoes with embedded carbon fiber plates or rocker-bottom walking shoes are ideal. Eliminate barefoot walking on hard floors entirely. Ice the ball of the foot for 15–20 minutes after any activity that has loaded the forefoot. Completely eliminate running, jumping, dancing, and activities requiring forefoot push-off. Walking for essential daily activities is acceptable; plan routes that minimize incline and stair climbing, which increase forefoot load significantly.
Footwear for Phase 1: The shoe matters as much as the insole. Choose footwear with these characteristics: rocker-bottom sole that promotes heel-to-toe rollover without a prominent toe-off phase; a toe box wide enough to accommodate the forefoot without any lateral compression at the first MTP joint; a firm midsole that does not collapse into a V-shape at the forefoot during loading; and a low-to-moderate heel drop (8–12mm is ideal, reducing ankle equinus that increases forefoot loading). Avoid completely flat shoes, ballet flats, or minimalist footwear during Phase 1 — even with insoles, these shoe types do not provide adequate mechanical protection during the inflammatory phase.
Phase 2: Subacute Recovery (Weeks 3–6)
Phase 2 begins when pain at the first MTP joint with normal walking has reduced by at least 50% from peak severity. Transition from HAPAD dancer’s pads as the primary insole to either the Powerstep Pinnacle (for patients with arch involvement or pronation) or continue dancer’s pads combined with Tuli’s gel forefoot cushioning for patients with primarily high-impact forefoot loading as their sesamoiditis driver.
Return-to-activity progression for Phase 2: Begin with flat-ground walking at comfortable pace — 15–20 minutes without pain is the benchmark before advancing. Add inclined walking when flat-ground walking is pain-free. Introduce very light cycling (stationary bike) which largely spares the sesamoids compared to weight-bearing activity. Aqua jogging or pool walking allows cardiovascular maintenance with minimal forefoot load. Do not advance to impact activity (running) until you can complete 45 minutes of brisk walking without any forefoot pain during or after activity. Rushing the Phase 2 progression is the most common cause of sesamoiditis recurrence.
Physical therapy during Phase 2: Begin gentle first MTP joint mobilization to prevent joint stiffness from the activity restriction of Phase 1. Intrinsic foot muscle strengthening — particularly exercises targeting the abductor hallucis and flexor digitorum brevis — helps rebuild the soft tissue support around the sesamoid complex. Calf stretching reduces ankle equinus and indirectly reduces the forefoot loading moment during gait. These exercises should not produce pain at the first MTP joint; if they do, reduce intensity and reconfirm pain has adequately resolved before continuing.
Phase 3: Return to Full Activity (Weeks 7–12)
Phase 3 begins when walking is completely pain-free and the sesamoid complex is non-tender to firm palpation. For most patients with early-stage sesamoiditis, this occurs around weeks 6–8. For athletes with stress fracture history or bone marrow edema on MRI, this phase is delayed until imaging confirms resolution of edema — typically at the 10–12 week mark.
Return-to-run protocol: Begin with a 10-minute run/walk interval program — one minute of easy running alternated with two minutes of walking, totaling 10 minutes. Perform every other day. Advance by 10% total volume per week if pain-free. Continue wearing dancer’s pads or the Powerstep Pinnacle insole for the first 4 weeks of return-to-run regardless of symptoms, as the sesamoid complex remains mechanically vulnerable during this period. If any forefoot pain returns during Phase 3, drop back to the previous volume level for one week before attempting to advance again. Full return to pre-injury training volume typically occurs at weeks 10–14 for runners who managed Phase 1 and 2 correctly.
Sesamoiditis Taping: The Adjunct Technique That Accelerates Recovery
Athletic taping of the big toe — specifically, taping the first MTP joint in slight plantarflexion to limit dorsiflexion during the push-off phase — is a powerful adjunct to insole therapy for sesamoiditis. When the first MTP joint cannot dorsiflex as far during toe-off, the compressive and shear forces on the sesamoid complex are significantly reduced, allowing earlier return to activity than insoles alone provide.
The taping technique for sesamoiditis is straightforward: use 1.5-inch athletic tape or kinesiology tape. Begin with an anchor strip on the dorsum (top) of the foot just proximal to the toes. Apply a series of 2–3 “J-strips” that start on the dorsal anchor, pass beneath the big toe, and pull the toe into slight plantarflexion before securing to the anchor. The toe should be in approximately neutral position or 5–10 degrees of plantarflexion — not forced into flexion, just gently unloaded. A final lock-down strip over the anchor completes the application. Properly applied, the tape should immediately reduce pain with push-off. Tape typically remains effective for one day of activity before losing tension and requiring reapplication.
Kinesiology tape (KT Tape, RockTape) applied in a Y-strip configuration beneath the ball of the foot provides proprioceptive feedback and mild mechanical decompression that some patients find helpful between taping sessions. This is a different mechanism from the functional limitation tape described above and provides less mechanical offloading, but it is easier to apply independently and can be worn for 3–5 days continuously.
Shoe Selection for Sesamoiditis: The Foundation of Every Treatment Plan
The best insole in the world cannot compensate for a biomechanically inappropriate shoe. The shoe is the structural environment that determines how load is distributed across the forefoot — and for sesamoiditis management, shoe selection is arguably more impactful than insole selection. Here are the footwear characteristics that either protect or aggravate the sesamoid complex.
Shoes that protect the sesamoids: Carbon fiber plated running shoes (Nike Vaporfly, Adidas Adizero Adios Pro, Saucony Endorphin Pro) have a rigid carbon plate that prevents first MTP dorsiflexion during toe-off — the gold standard for sesamoiditis-friendly athletic footwear, though not appropriate for everyday casual wear. Rocker-bottom therapeutic shoes (Hoka Clifton, Brooks Glycerin, ASICS Gel-Nimbus) achieve similar protection through sole geometry rather than a rigid plate. Maximalist cushioned shoes absorb ground reaction forces before they reach the forefoot. Wide toe box shoes (New Balance wide widths, Altra footwear) prevent lateral compression of the first MTP joint.
Shoes that aggravate sesamoiditis: High heels shift body weight forward onto the sesamoid complex — even a 2-inch heel increases forefoot loading by approximately 70% compared to flat footwear. Pointed toe boxes compress the first and fifth metatarsal heads toward each other, increasing sesamoid stress. Barefoot and minimalist shoes (Vibram FiveFingers, Xero Shoes) eliminate cushion and motion control, maximizing ground reaction forces at the sesamoids. Cleated athletic shoes on artificial turf surfaces create an inflexible interface that prevents normal forefoot roll, compressing the sesamoids. Worn-out athletic shoes with collapsed midsoles lose their mechanical benefit and may actually worsen forefoot loading compared to well-cushioned alternatives.
When Conservative Care Isn’t Enough: Understanding Surgical Options
The vast majority of sesamoiditis cases — over 80% in most clinical series — resolve with consistent conservative management. Surgery is reserved for cases where conservative care has been applied correctly for 3–6 months without adequate improvement, or where imaging reveals avascular necrosis (bone death) that prevents natural healing. Understanding what surgical options exist helps patients make informed decisions when the conversation with their podiatrist reaches that point.
Sesamoidectomy — partial or complete removal of one or both sesamoid bones — is the most commonly performed procedure for refractory sesamoiditis and sesamoid avascular necrosis. Medial sesamoidectomy (removal of the larger, more commonly affected medial sesamoid) generally has more favorable outcomes than lateral sesamoidectomy, as the medial sesamoid is more accessible and its removal has fewer biomechanical consequences. Complete medial sesamoidectomy does slightly reduce big toe push-off power (typically by 10–15%), which is clinically significant for high-level athletes but acceptable for most recreational patients.
Recovery from sesamoidectomy involves 6–8 weeks of protected weight-bearing, followed by gradual rehabilitation. Most patients return to non-impact activity at 3 months and full athletic activity at 4–6 months. Outcomes are generally good for pain relief — over 85% of patients report significant or complete resolution of sesamoid pain post-operatively — though a small percentage develop adjacent metatarsal overload as the first metatarsal adjusts to the changed sesamoid complex. This is another reason why exhausting conservative care before considering surgery is important: once the sesamoid is removed, the biomechanical consequences are permanent.
Related Foot & Ankle Resources from Balance Foot & Ankle Specialists
Sesamoiditis often occurs alongside or is confused with other forefoot conditions. Explore these related resources for comprehensive information:
- Sesamoiditis Treatment Guide — Balance Foot & Ankle
- Best Metatarsal Pads 2026: Podiatrist Guide
- Best Morton’s Neuroma Insoles & Pads 2026
- Podiatrist Recommended Orthotics 2026: Dr. Tom’s Top 10 Insoles
- Best Kinesiology Tape for Foot Pain 2026
- Best Running Shoes for Foot Pain 2026
- Plantar Fasciitis: Complete Treatment Guide
Ready to Resolve Your Sesamoid Pain? See Dr. Tom in Howell, Michigan
Sesamoiditis responds well to conservative treatment — but only when the correct mechanical cause is identified and addressed. Dr. Tom Biernacki provides comprehensive sesamoiditis evaluation including gait analysis, X-ray, and MRI interpretation at our Howell clinic. Most patients leave their first appointment with a clear understanding of their condition severity, a personalized offloading strategy, and a realistic recovery timeline.
Balance Foot & Ankle Specialists
Howell, Michigan | (517) 545-0100
Schedule Your Sesamoiditis Consultation →
Differential Diagnosis: What Else Could It Be?
Not every case of sesamoiditis is straightforward. In our clinic we routinely rule out three look-alike conditions before confirming the diagnosis. If your symptoms don’t match the classic presentation, one of these may explain the pain — which is why physical exam matters more than self-diagnosis.
| Condition | How It Differs |
|---|---|
| Sesamoid stress fracture | Acute or gradually worsening sharp pain, tender directly over one sesamoid, positive findings on MRI. |
| Hallux rigidus | Stiff, painful big toe joint with limited dorsiflexion — pain is AT the joint, not UNDER the ball. |
| Turf toe (plantar plate injury) | Acute hyperextension mechanism, diffuse swelling of the 1st MTP, positive 1st MTP drawer test. |
Red Flags — When to See a Podiatrist Now
Seek same-day evaluation at Balance Foot & Ankle if you notice any of the following:
- Sudden sharp onset (possible fracture)
- Bruising or swelling under the big toe
- Pain at rest or at night
- Inability to push off during gait
Call (810) 206-1402 or request an appointment. Our Howell and Bloomfield Hills offices reserve same-day slots for urgent foot and ankle issues.
In Our Clinic: What We See
Clinical perspective from Dr. Tom Biernacki, DPM — Balance Foot & Ankle, Howell & Bloomfield Hills, MI:
In our Balance Foot & Ankle clinic, sesamoiditis patients are usually dancers, runners, or women who have spent significant time in heels. They describe pain directly UNDER the big toe joint — not at the joint (that’s hallux rigidus) — which worsens with push-off. On exam we palpate each sesamoid separately (tibial and fibular) and assess for sensitivity. We always get X-rays to look for sesamoid fracture or bipartite sesamoid (a normal variant). Treatment uses a dancer’s pad to offload the sesamoid, stiff-soled footwear to reduce push-off stress, and activity modification.
When Shoes Aren’t Enough — Dr. Tom’s Top 9 Orthotics
About 30% of patients I see for foot pain need MORE than a great shoe — they need a structured insole. Below: my complete 2026 orthotic ranking with pros, cons, and the specific patient I’d give each one to.
★ DR. TOM’S COMPLETE 2026 ORTHOTIC RANKING
9 Best Prefab Orthotics by Use Case
PowerStep, Currex, Spenco, Vionic, and PowerStep Pinnacle — every orthotic I’ve fitted to thousands of patients across both Michigan offices. Each card includes pros, cons, and the specific patient I’d give it to. Real Amazon ratings, review counts, and prices below.
Best All-Purpose Orthotic for Most Patients
Semi-rigid arch shell + dual-layer cushion + deep heel cup. The orthotic I’ve fitted to more patients than any other for 15 years. APMA-accepted. Trim-to-fit design works in athletic shoes, casual shoes, and most work boots.
✓ Pros
- Semi-rigid arch shell provides true biomechanical correction
- Deep heel cup centers the heel and reduces lateral instability
- Dual-layer cushion (top + bottom) lasts 9-12 months daily wear
- Available in 8 sizes for precise fit
- APMA-accepted and clinically validated
- Lower price than PowerStep Pinnacle for equivalent function
✗ Cons
- Too thick for most dress shoes (use ProTech Slim instead)
- Some break-in period required (3-7 days for arch tolerance)
- Not enough correction for severe pes planus or rigid pes cavus
Dr. Tom’s Recommendation: If a patient has run-of-the-mill plantar fasciitis, mild flat feet, or arch fatigue, this is the first orthotic I try. Better value than PowerStep Pinnacle for 90% of patients, which is why I swapped it into our clinic kits three years ago. Sub-$50 typically.
Maximum Motion Control · Flat Feet & Severe Over-Pronation
PowerStep’s most aggressive stability orthotic. Adds a 2°-7° medial heel post on top of the standard PowerStep platform — designed specifically for flat-footed patients and severe pronators who need real corrective force.
✓ Pros
- 2°-7° medial heel post adds aggressive pronation control
- Same trusted PowerStep arch shell, more correction
- Built specifically for flat-foot biomechanics
- Excellent for posterior tibial tendon dysfunction (PTTD)
- Removable top cover for cleaning
✗ Cons
- Too aggressive for neutral-arch patients
- Needs longer break-in (10-14 days) due to stronger correction
- Adds 2-3 mm of stack height — won’t fit slim dress shoes
Dr. Tom’s Recommendation: When a patient comes in with significant flat feet AND symptoms (heel pain, arch pain, knee pain), the Original PowerStep isn’t aggressive enough. The Maxx is what gets prescribed. About 25% of my flat-footed patients end up here.
Low-Profile · Fits Dress Shoes & Narrow Casuals
3 mm slim profile with podiatrist-designed tri-planar arch technology. Engineered specifically to fit inside dress shoes, oxfords, loafers, and women’s flats without crowding the toe box. Vionic was founded by an Australian podiatrist.
✓ Pros
- 3 mm slim profile (vs 7-10 mm for standard orthotics)
- Tri-planar arch technology adds support without bulk
- Built-in deep heel cup despite slim design
- Fits dress shoes WITHOUT having to remove the factory insole
- Trim-to-fit · APMA-accepted
✗ Cons
- Less arch support than full-volume orthotics
- Top cover wears faster than thicker alternatives
- Not enough correction for severe foot deformities
Dr. Tom’s Recommendation: My default when a patient says ‘I need orthotics but I have to wear dress shoes for work.’ Slim enough to fit in oxfords and pumps without the heel sliding out. The single highest-impact change you can make for office workers with foot pain.
Built-In Metatarsal Pad · Morton’s Neuroma · Ball-of-Foot Pain
Standard Pinnacle orthotic with a built-in metatarsal pad positioned proximal to the metatarsal heads — the exact location that offloads neuromas and metatarsalgia. No need for separate met pads or pad placement guesswork.
✓ Pros
- Built-in met pad eliminates DIY pad placement errors
- Specifically designed for Morton’s neuroma + metatarsalgia
- Same trusted PowerStep arch + heel cup platform
- Top cover protects sensitive forefoot skin
- Faster relief than orthotics + add-on met pads
✗ Cons
- Met pad position is fixed (can’t fine-tune individual placement)
- Some patients with very small or very large feet need custom
- Slightly thicker than the standard Pinnacle
Dr. Tom’s Recommendation: If a patient has Morton’s neuroma, sesamoiditis, or generalized ball-of-foot pain (metatarsalgia), this saves a clinic visit and a prescription. The built-in pad placement is anatomically correct for 80% of feet. Way better than DIY met pads.
Adaptive Dynamic Arch · Athletic & Daily Wear
Currex’s flagship adaptive arch technology — the orthotic flexes with your gait instead of fighting it. Different stiffness zones along the length give you targeted support at the heel, midfoot, and forefoot. Available in three arch heights (low/medium/high).
✓ Pros
- Dynamic flex zones adapt to natural gait cycle
- Three arch heights ensure precise fit
- Lighter than rigid orthotics (no ‘heavy foot’ feel)
- Excellent for runners and athletic walkers
- European podiatric design (German engineering)
✗ Cons
- More expensive than PowerStep Original ($55-65 typically)
- Less aggressive correction than Pinnacle Maxx for severe cases
- Three arch heights means you must self-select correctly
Dr. Tom’s Recommendation: I started recommending Currex three years ago for runners who said PowerStep felt ‘too rigid.’ The dynamic flex zones respect natural gait. Best for active patients who walk 8K+ steps daily and don’t need maximum motion control.
Running-Specific · Heel Strike + Forefoot Strike Compatible
Currex’s purpose-built running orthotic. The midfoot flex zone is positioned for runner’s gait mechanics, with a flared heel cushion for heel strikers and a forefoot rocker for midfoot/forefoot strikers. Tested on 1000+ runners during product development.
✓ Pros
- Designed by German biomechanics lab specifically for runners
- Dynamic arch flexes with running gait (not static like PowerStep)
- Three arch heights (low/medium/high)
- Reduces overuse injury risk in mid-distance runners
- Lightweight (no impact on cadence)
✗ Cons
- Premium price ($60-75)
- Not aggressive enough for severe over-pronators (use Pinnacle Maxx)
- Runner-specific design = less ideal for daily walking shoes
Dr. Tom’s Recommendation: If a patient runs 20+ miles per week and has plantar fasciitis or shin splints, this is the orthotic I prescribe. The dynamic flex zones respect running biomechanics in a way that no rigid PowerStep can match. Pricier but worth it for serious runners.
Cavus Foot & High-Arch Patients
Polyurethane base with a deeper heel cup and higher arch profile than PowerStep — built for cavus (high-arched) feet that need maximum cushion and support. The 5-zone cushioning system addresses the unique pressure points of high-arch feet.
✓ Pros
- Deeper heel cup centers the heel for cavus foot stability
- Higher arch profile fills the void under high arches
- 5-zone cushioning addresses cavus foot pressure points
- Polyurethane base lasts 12+ months
- Available in Wide width
✗ Cons
- Too tall/aggressive for normal or low arches
- Won’t fit slim dress shoes
- Pricier than PowerStep Original
- Some patients find the arch height uncomfortable initially
Dr. Tom’s Recommendation: Cavus foot patients are often misdiagnosed and given low-arch orthotics — that makes everything worse. Spenco’s Total Support has the arch profile that high-arch feet actually need. About 15% of my patients have cavus feet; this is what they wear.
Cushion Layer · Standing All Day · Gel Pressure Relief
NOT a true biomechanical orthotic — this is a cushion insole. But for patients who want gel pressure relief instead of arch correction (or to add ON TOP of factory insoles in work boots), this is the best gel option on Amazon.
✓ Pros
- Genuine gel cushioning (not foam pretending to be gel)
- Targeted gel waves under heel and ball of foot
- Trim-to-fit · works in most shoe types
- Sub-$15 price (most affordable option in this list)
- Massaging texture is genuinely soothing
✗ Cons
- ZERO arch support — this is cushion only
- Won’t fix plantar fasciitis or flat-foot issues
- Compresses faster than PowerStep (4-6 months)
- Top cover wears through in high-mileage applications
Dr. Tom’s Recommendation: I recommend these to patients who tell me ‘I just want my feet to stop hurting at the end of my shift’ and who don’t have a biomechanical issue. Construction workers, factory workers, retail. Pure cushion does the job for them.
Tight-Fitting Shoes · Cycling Shoes · Hockey Skates
PowerStep Pinnacle’s slim version of their famous Green insole. The trademark stabilizer cap is preserved but the overall thickness is reduced — works in cycling shoes, hockey skates, ski boots, and other tight-fitting footwear that the standard PowerStep Pinnacle can’t fit into.
✓ Pros
- Stabilizer cap centers the heel (PowerStep Pinnacle’s signature feature)
- Slim profile fits tight athletic footwear
- Lasts 12+ months daily wear
- Excellent for cycling shoes specifically
- Built-in odor-control treatment
✗ Cons
- Premium price ($45-55)
- Less cushion than PowerStep equivalents
- Not as aggressive correction as Pinnacle Maxx for flat feet
- The signature ‘heel cup feel’ takes 1-2 weeks to adapt to
Dr. Tom’s Recommendation: If you’re a cyclist with foot numbness, hot spots, or knee pain — this is the orthotic. The stabilizer cap solves cycling-specific biomechanical issues that no other orthotic addresses. Worth the premium for athletes.
None of these solving your foot pain?
Some patients (about 30%) need custom-molded prescription orthotics. We make 3D-scanned custom orthotics in our Howell and Bloomfield Hills offices — specifically built for your foot mechanics.
Schedule a Custom Orthotic Fitting →FSA/HSA eligible · Most insurance accepted · (810) 206-1402
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.
Related reading: Plantar Fasciitis Secrets — our complete heel pain guide: what works and what to avoid.
- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)
Recommended Products from Dr. Tom