What a Podiatrist Can Do For YOU!
Diabetic Foot Treatment [Podiatrist or Foot Doctor Diabetic Foot Care]
Diabetic foot management with a podiatrist is one of the most proven ways to avoid hospitalization, infection, and even amputation as a person with diabetes.
Look:
- Podiatrists are vital team members in caring for diabetes and the diabetic foot.
- We are trained to cure diabetic ulcers, diabetic foot infections and prevent hospitalizations.
- We welcome patients with ingrown toenails, toenail fungus, corns, and calluses, as well as wounds.
So don’t wait! Let us help you with your diabetic foot care.
Table of Contents
Balance Foot & Ankle Specialists Brighton Michigan
Balance Foot & Ankle Specialists Livingston County
Balance Home Care & Wound Care
11 Reasons To Choose US!
- 🥇 We work hard for YOUR Satisfaction. (If you’re not 100% satisfied with your appointment, we WILL do everything we can to FIX IT for you.) Terms & Conditions.
- 🦶The BEST Podiatrists: Board Certified in Foot Surgery & Board Certified in Podiatric Medicine for all of your foot & ankle needs!
- 💻Telehealth appointment from the comfort of your own home!
- 🚗 You Can Park 100% for Free Right Outside The Door.
- 📲 You Can Book Online 24/7 Right From Your Phone.
- 🌙 You Can Get A Late Appointment Or Seen Outside of Regular Hours……No Need To Take Time Off Work.
- 🏠 If you cannot come to see us due to health issues or immobility… We can come to see YOU!
- 💉 The BEST Tools: In-office X-ray, In-office fluoroscopy, In-office ultrasound, injections, skin treatment, and in-office surgical suite. We are trained to use the NEWEST equipment.
- 📞 You Can Take Up Our Offer for a Phone or Telehealth Consult With Our Podiatry Team before you arrive if you are unsure if we can help you.
- 🏥 A professional cutting edge surgical suite staffed by residency trained Board Certified Foot & Ankle Surgeons: Minimally Invasive Surgery!
- 👣You Get Treated By Podiatrists Who Specialize In the Foot & Ankle, So They KNOW What’s Needed To Get You Back On Your Feet.
Google Rating
Prime Foot & Ankle Specialists - Podiatrists & Foot Doctors
4.9 308 reviews
-
Joseph Russo
★★★★★
a month ago
I'm 54 years old, and I'm always enlighten by the info I get from this channel. We can never stop learning to better … More our health.
-
Nancy
★★★★★
in the last week
Information provided is sooo useful. Everything is explained clearly making it so easy to understand. Its also a guide and … More you understand supplements better. I also like his recommendations.
-
Amy Corbett
★★★★★
2 months ago
This channel is so informative! Thank you for being quick but thorough! And I love hearing the OTC stuff & what works … More for many of your patients! Thank you! 🙏🥰
Free BOOK to solve foot pain:
STOP wasting TIME & MONEY on your foot & ankle pain!
“11 SIMPLE Ways to STOP Foot PAIN. “
Learn 11 simple step-by-step tips to get rid of foot & ankle pain… even if you’ve suffered for months or years and your doctor told you nothing could be done to help!

Frustrated With Your Foot Pain? Let Us Help!
Not sure what to do?
Not sure who to ask?
- If you live in Michigan, we can HELP!
Fill in the form, and one of our highly qualified team will be in touch to discuss your specific problem.
What a Podiatrist Can Do For YOU!
Daily Diabetic Foot Management:
- The true keys to diabetic foot management are inspecting your feet every day and seeking early podiatrist care for your foot injury.
- Make sure your podiatrist checks your fee at least once per year. Some people need to be checked twice per year, and some people need to be checked even every three months, depending on certain risk factors.
- If you have excellent blood flow and excellent sensation through the bottom of your feet, then you can probably get away with just been checked once per year.
- If you have either poor blood flow or a poor sensation through the bottom of your feet, you may benefit from a more frequent visit, like twice per year.
- If you have numerous foot problems, have poor blood flow, and have a poor sensation at the bottom of your feet.
- This would necessitate visits about every three months for toenail callous care to make sure blisters don’t turn into infected wounds.
- Most patients are generally covered for diabetic shoes and other products that can help prevent any wounds from forming.
- So don’t feel guilty. This isn’t a cosmetic pedicure! This is a life-saving treatment that can save your life and your foot.
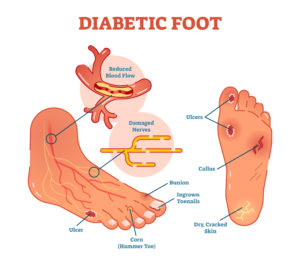
Podiatrist Diabetic Foot Management:
It would help if you visited your podiatrist at least once per year to have a diabetic foot exam. We admit the vast majority of the time this should be an unremarkable exam, where you ask yourself why did I even come in here? And if that’s all that’s happening, you are doing an excellent job.
On the other hand, our clinic is filled with patients who don’t think anything is wrong, that they have a callous that is turning dark, that they simply are developing thick toenails. And they are absolutely shocked to learn that as we trim these down, there is blood pouring out of these, with a large wound, with dry blood trapped underneath these.
Nobody actually knows that they have a huge ulcer that is obviously infected. What usually happens is a callous start turning red, and people shop to the hospital not thinking anything is wrong. At that point, it may be too late! We personally see this over 10 times a week at the hospitals we cover. Most people are always shocked that something like this could happen to them, they thought something was hurting more and more, but they always put it off until seeing a podiatrist.
So, don’t use this as an excuse! This is a covered medical benefit, and it is proven repeatedly to be beneficial and even cost-effective for you to see a podiatrist.
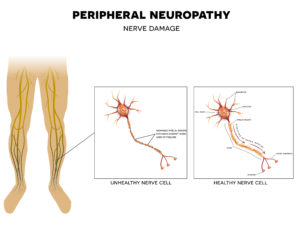
The keys to diabetic foot management:
Improve your diabetes as much as possible: work with your primary care doctor in your podiatrist to keep a close eye on your blood sugar and keep it in the target range. If your blood sugar is well-controlled, it’s almost like you don’t even have diabetes!
Sometimes we have a foot problem. It doesn’t make sense to go on walks or runs. But things like water aerobics and riding a stationary bike make a lot of sense for you. These types of exercise can even burn more calories than simply going for a walk which barely burns any calories at all. Be as healthy as possible: talk to your podiatrist and your primary care doctor about how to exercise.
Look into your insurance and Medicare plan: most versions of Medicare plans do cover special diabetic shoes. You have to qualify for some criteria, but your podiatrist can work with you in making these available.
Wash your feet daily: be careful to look between your toes. I can build up a lot of crust and dry skin here. This is a common site for infection to develop.
Keep your skin moisturized: this is especially important after taking a bath and going to bed at night. The biggest mistake you can make is buying something expensive. Don’t do that. Even something like petroleum jelly or Vaseline can be a couple of dollars for a gigantic tub. Applying this daily will solve the vast majority of your skin issues.
Maintain your toenails and calluses: this is something your podiatrist can do for you. This is not cosmetic! This is the biggest mistake people make. There have been thousands of times where I see the patient in the hospital, and they said they were not ready or felt guilty getting their nails checked. Don’t let this happen to you, don’t let yourself have a large infection because you are embarrassed or are worried about some coverage issue. If you have a medical problem, any insurance would be glad to have you get it taken care of outside the hospital!
Wear good shoes and socks: Don’t fall for the “peripheral neuropathy” trap where people think that purple neuropathy is causing your foot pain. Peripheral neuropathy generally makes your foot numb, but then your foot throbs at night because you did damage to it without feeling. Don’t fall for the pharmaceutical marketing gimmicks where you feel you need some nerve-numbing medication. This is not a disease that you can’t do anything about. You can do something about your foot pain and your numbness. Almost every patient you have that wears good shoes, good inserts, and good socks has much less pain at night if not completely resolved than nighttime pain.
Watch out for hot and cold: with diabetes, your foot can have a harder time telling hot from the cold. This means if you stepped on something really cold or something hot, you could be doing damage to your foot. Just be aware, especially when it’s icy outside, that your floor may be called, and this is why your toes are turning purple or red. Also, when you’re filling up a tub, make sure that the water is not too hot. Use the elbow rule. If you can touch it with your elbow, that is the true temperature.
See your podiatrist today: it has been proven repeatedly that a podiatrist is the foot specialist that is best suited to look after your feet. If you have diabetes, it has been proven that the cost savings and the overall improvements are amazing with even one to two trips. So don’t keep holding off and end up in the hospital. It’s covered by insurance. What have you got to lose except for a few moments of your time?
Don’t wait until we see you in the hospital:
- This is not a cosmetic problem. This is something that any reasonable insurance will cover!
- The biggest mistake we see is patients feel guilty about seeking foot care because they think it’s a cosmetic effect, and they end up in the hospital with a traumatic life-altering infection.
Is Diabetic Foot Management a Covered Benefit?
- Absolutely, this is a covered benefit by almost every single insurance.
- This is proven to help reduce hospitalization and infections.
- Most insurances can cover diabetic shoes and inserts to prevent further infection and deformity.
Diabetic Foot Management by a Podiatrist:
- A podiatrist is a physician who has performed a minimum of 4 years undergraduate degree, 4 years of medical training, 3 years of surgical and medical hospital-based residency training, possibly a fellowship training period, and is board certified in foot & ankle surgery!
- We have extensive training in diabetes and diabetic management.
- We are extremely proud of the training our physicians have accomplished.
What is Diabetic Foot Care?
- Diabetes can damage nerves in your feet and cause “peripheral neuropathy,” a condition that causes numbness, pain, or loss of sensitivity in your extremities. Diabetes can also affect your body’s ability to heal properly from cuts or blisters because of changes in blood flow to your feet.
- Initial risk stratification and regular checkups with your podiatrist will protect your feet and keep them healthy.
- If you notice any problems such as redness, blisters, cracks, or breaks in your skin, keep the area clean and schedule an appointment. Stop these problems before they get worse!
- An infection causes fungal toenails underneath the surface of the nail.
- The fungus can turn the nail yellow or brown in color while making it thicker. Debris can also collect beneath the nail plate and may make it painful to walk or run. (Fungal toenails may or may not be painful while they are still an active infection).
- We can perform a test to identify the type(s) of infection and determine the best treatment option for your case.
- Treatments may include prescription topical medication, prescription oral medication, and trimming of the toenails.
- It is important to seek treatment for this condition to avoid complications from an infection and spread the fungus to other nails on your hands or feet.
Diabetic Shoes:
- Most major insurances cover diabetic shoes and inserts.
- See a podiatrist today to see if you are eligible.
- This is an essential benefit that can decrease your chances of ulcer formation and infection.
Podiatrist Diabetic Foot Care In Berkley Mi
Areas we service:
The podiatrists & foot doctors of Prime Foot & Ankle Specialists are available for in office visits, home care and telehealth for the following locations:
- Berkley Michigan
- Oakland County Michigan
- Royal Oak Michigan
- Oak Park Michigan
- Huntington Woods Michigan
- Clawson Michigan
- Ferndale Michigan
- Birmingham Michigan
- Madison Heights Michigan
- Franklin Michigan
- Hazel Park Michigan
- Southfield Michigan
- Troy Michigan
- Bloomfield Hills Michigan
- Lathrup Village Michigan
- Novi Michigan Area
- Bloomfield Michigan Area
- West Bloomfield Michigan Area
- South Lyon Michigan Area
- Northville Michigan Area
- But anyone in the state of Michigan.
Contact us if you need to be seen in Michigan or Oakland County Michigan!