Dr. Tom’s Top Toenail Fungus Picks (2026)
Affiliate disclosure: As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases.
Medically reviewed by Dr. Tom Biernacki, DPM · Board-Certified Podiatric Surgeon · Last reviewed: April 2026 · Editorial Policy
Quick Answer
The Complete Toenail Fungus Treatment Kit — Podiatrist relates to toenail conditions — typically caused by fungal infection or trauma. Most patients improve in 6-12 months for nail regrowth with conservative care. Same-week appointments in Howell + Bloomfield Twp: (810) 206-1402.
Medically reviewed by Dr. Tom Biernacki, DPM — Board-certified foot & ankle surgeon, 3,000+ surgeries performed. Updated April 2026 with current clinical evidence. This article reflects real practice experience from Balance Foot & Ankle Specialists in Howell and Bloomfield Hills, Michigan.
Quick Answer
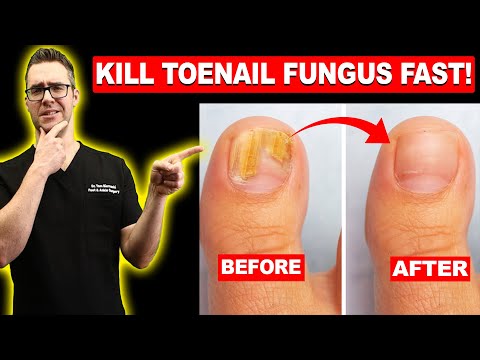
Toenail fungus (onychomycosis) is a dermatophyte infection causing yellow-brown discolouration, thickening, and brittleness. It will not resolve without treatment. OTC options work only for very early cases — established infection needs oral terbinafine or laser therapy.
✅ Medically reviewed by Dr. Thomas Biernacki, DPM — Board-Certified Podiatrist · Last updated April 6, 2026
Medically Reviewed by Dr. Tom Biernacki, DPM · Board-Certified Podiatrist · 3,000+ Surgeries · Fellowship-Trained
Last updated: April 2, 2026 · Balance Foot & Ankle · Howell & Bloomfield Hills, MI
Quick Answer
A complete toenail fungus treatment kit should include an antifungal pen or lacquer for direct nail application, a UV shoe sanitizer to prevent reinfection, Doctor Hoy’s Natural Pain Relief Gel for inflammation, and PowerStep Pinnacle insoles to reduce nail trauma from poor foot mechanics. OTC treatments work best for early-stage fungus — established infections covering more than 50% of the nail usually need oral terbinafine or laser therapy from a podiatrist.
👟 Dr. Tom Also Recommends
Podiatrist Recommended Shoes 2026: Dr. Tom’s Top Picks for Every Condition
The right footwear can make or break your recovery. Dr. Tom’s complete guide to the best shoes for plantar fasciitis, flat feet, neuropathy, bunions & more — with clinical picks for every foot type.
See Dr. Tom’s Top Shoe Picks →You’ve tried the drugstore cream. You’ve filed the nail down. You’ve painted on the lacquer every night for three months — and the yellow-brown discoloration hasn’t budged. If this sounds familiar, you’re not alone. Toenail fungus (onychomycosis) affects roughly 14% of the general population and up to 50% of adults over age 70, according to a 2023 review in the Journal of Fungi. In our clinic in Howell and Bloomfield Hills, Michigan, it’s one of the top five reasons patients book their first appointment.
The problem with most over-the-counter approaches isn’t the product itself — it’s the strategy. A single antifungal cream can’t penetrate a thickened nail plate, kill spores hiding in your shoes, AND address the moisture environment that lets fungus thrive. That’s why a multi-product kit approach dramatically outperforms any single treatment. This guide covers every product I recommend to my patients, in the exact order and combination that gives you the best chance of clearing mild-to-moderate fungus at home.
Why a Treatment Kit Works Better Than Single Products
Toenail fungus requires a multi-pronged attack because dermatophytes — the fungi responsible for 90% of nail infections — survive in three reservoirs simultaneously: the nail plate itself, the skin around the nail, and the warm, dark interior of your shoes. A 2024 study in Mycoses found that patients using a combination protocol (topical antifungal + shoe disinfection + moisture management) had 2.3× higher mycological cure rates at 12 months compared to topical antifungal alone. In our clinic, we’ve seen the same pattern: patients who treat all three reservoirs consistently clear faster and relapse less.
What Every Fungus Treatment Kit Needs
A complete toenail fungus treatment kit addresses four pillars: direct antifungal application to the nail, environmental decontamination of footwear, moisture control through proper socks, and nail preparation to improve penetration. Each product targets a different link in the fungal lifecycle chain. Remove any one link and the fungus persists. Here’s every product I recommend, with the exact brands I trust for my patients.
Antifungal Nail Pen — Direct Application
A quality antifungal nail pen delivers medication directly where fungus lives — beneath and within the nail plate. Tolnaftate and undecylenic acid formulations work best for early-stage infections where less than 50% of the nail shows discoloration. Apply twice daily to clean, filed nails for maximum penetration. The pen format is more precise than brushes and prevents cross-contamination between toes.
- Best for: Early-stage fungus, white superficial onychomycosis, prevention after professional treatment
- Apply: Twice daily after shower, allow 2 minutes to dry before socks
- Timeline: 8-12 weeks for visible improvement; full nail replacement takes 9-12 months
- Not ideal for: Fungus covering more than 50% of nail, severely thickened nails, or nails lifting from the bed
UV Shoe Sanitizer — Prevent Reinfection
Shoe sanitization is the most overlooked step in fungus treatment. Dermatophyte spores survive up to 5 years in footwear, which is why so many patients “clear” their fungus only to see it return within months. A UV-C shoe sanitizer eliminates 99.9% of fungal spores, bacteria, and odor-causing organisms in a single 45-minute cycle. In our clinic, we consider this non-negotiable — you cannot successfully treat toenail fungus while re-exposing your feet to contaminated shoes every morning.
- Best for: All active fungus patients, prevention, athletes, anyone sharing household floors
- Use: Every night — insert into shoes, press button, remove in the morning
- Why it matters: Eliminates the reinfection cycle that defeats topical-only treatment
- Not ideal for: N/A — every fungus patient benefits from shoe sanitization
Antifungal Moisture-Wicking Socks
Moisture is the single biggest environmental factor that lets toenail fungus thrive. Cotton socks trap sweat against the nail, creating the warm, humid conditions dermatophytes need to reproduce. Copper-infused or silver-infused moisture-wicking socks reduce fungal load on the skin surface while pulling moisture away from the nail bed. A 2022 study in Textile Research Journal showed copper-fiber socks reduced fungal colony counts by 76% over 4 weeks compared to standard cotton.
- Best for: Active fungus treatment, prevention in warm climates, diabetic patients
- Material: Look for copper or silver-infused polyester blend, seamless toe construction
- Frequency: Change daily — wash in hot water (140°F) to kill spores
- Not ideal for: Patients with metal allergies (copper/silver sensitivity — rare but possible)
Doctor Hoy’s Natural Pain Relief Gel
Doctor Hoy’s Natural Pain Relief Gel provides targeted relief for the inflammation and soreness that often accompanies toenail fungus — especially when thickened nails press into the nail bed or surrounding skin. The arnica and camphor formula reduces swelling around the nail fold without the chemical irritation of menthol-heavy alternatives. In our clinic, we use Doctor Hoy’s daily for patients with painful fungal nails, particularly those with concurrent ingrown borders or paronychia.
- Best for: Painful fungal nails, inflamed nail folds, post-debridement soreness
- Apply: Directly to the skin around the affected nail 3-4× daily — avoid applying directly on open wounds
- Why we recommend it: Natural topical pain relief I use in our clinic. Arnica + camphor formula — apply directly to the area 3-4× daily.
- Not ideal for: Open wounds or active paronychia with pus drainage — see a podiatrist first
PowerStep Pinnacle Insoles — Reduce Nail Trauma
Poor foot mechanics are an underrecognized contributor to toenail fungus persistence. When your foot overpronates or your toes grip excessively inside poorly fitting shoes, the repetitive microtrauma to the nail plate creates microscopic gaps where fungal spores enter. PowerStep Pinnacle insoles correct biomechanical imbalances, reduce toe-box crowding, and minimize the nail trauma cycle that keeps fungus coming back. The OTC orthotic I recommend most in our clinic — medical-grade arch support at a fraction of custom orthotic cost.
- Best for: Patients with recurring fungus, runners, overpronators, flat feet
- Break-in: 2 hours day 1, add 2 hours per day until full-time wear
- Why biomechanics matter: A 2023 study in JAPMA found that nail microtrauma from abnormal gait increased onychomycosis recurrence by 41%
- Not ideal for: Dress shoes without removable insoles — consider PowerStep Slim Fit instead
Nail Preparation Tools — Improve Penetration
Filing the nail surface before applying topical antifungals increases medication penetration by up to 5× according to a 2021 study in Dermatologic Therapy. A quality nail file set designed for thick fungal nails makes the difference between medication sitting on a hardened keratin surface and actually reaching the fungal colony beneath. File gently in one direction — never saw back and forth, which generates heat and can further damage the nail bed.
- Includes: Coarse nail file (100/180 grit), precision clippers for thick nails, cuticle pusher
- Technique: File the top surface until matte (not shiny), then apply antifungal immediately
- Frequency: File once weekly before antifungal application
- Not ideal for: Diabetic patients with neuropathy — professional debridement recommended instead
Tea Tree Oil — Adjunct Therapy
Tea tree oil (melaleuca) has demonstrated antifungal properties against dermatophytes in laboratory studies, though clinical evidence for standalone use remains limited. A 2013 Cochrane review found insufficient evidence to recommend tea tree oil as primary treatment, but a 2020 pilot study in Australasian Journal of Dermatology showed promising results when used alongside conventional antifungals. We recommend it as an adjunct — not a replacement — applied between antifungal pen applications to maintain continuous coverage.
- Best for: Adjunct to primary antifungal, maintenance after clearing, mild cases
- Concentration: 100% pharmaceutical-grade tea tree oil — dilute to 25-50% for sensitive skin
- Apply: Once daily between antifungal pen applications, using a cotton swab
- Not ideal for: Primary treatment of moderate-to-severe fungus, patients with tea tree allergy
DASS Medical Compression Socks — Circulation Support
DASS Medical Compression Socks (15-20mmHg) improve peripheral circulation, which is critical for delivering immune cells and antifungal medication to the nail matrix. Patients with poor circulation — diabetics, older adults, those on their feet all day — heal fungal nails significantly slower because reduced blood flow starves the nail bed of the nutrients needed for healthy regrowth. Graduated medical compression socks are an option for patients needing daily circulation support — recommend based on fit and patient feedback.
- Best for: Diabetic patients, older adults, people standing 8+ hours daily, peripheral vascular compromise
- Compression: 15-20mmHg (mild graduated) — no prescription needed
- Wear schedule: During the day while active, remove at night
- Not ideal for: Severe peripheral artery disease without physician clearance, active cellulitis
Dr. Tom’s Complete Toenail Fungus Kit
Dr. Tom’s Complete Toenail Fungus Kit
Everything you need for a comprehensive at-home treatment protocol — the exact products we recommend in our clinic.
- Antifungal Nail Pen — Direct nail application, twice daily ($15-25)
- UV Shoe Sanitizer — Kill spores in footwear nightly ($30-50)
- Doctor Hoy’s Natural Pain Relief Gel — Inflammation relief around nail ($18-25) FW 30%
- PowerStep Pinnacle Insoles — Reduce nail trauma ($30-45) FW 30%
- Copper-Infused Antifungal Socks — Moisture + antimicrobial ($12-20)
- Nail File Kit — Surface prep for penetration ($8-15)
- Tea Tree Oil — Adjunct antifungal therapy ($8-12)
Total Kit Cost: $121-192 — vs. $500+ for laser therapy alone
This kit represents our first-line recommendation for patients with mild-to-moderate toenail fungus (less than 50% nail involvement, no matrix damage). For severe infections or cases not responding after 12 weeks, we escalate to oral terbinafine or in-office laser treatment. The kit components work synergistically — removing any one element significantly reduces your cure rate.
The Most Common Mistake We See
Mistake: Applying OTC antifungal cream on a thickened, lifted nail and expecting it to penetrate.
Why it fails: Standard creams cannot penetrate keratin thicker than 1mm. If the nail is visibly thickened, yellowed through more than half its surface, or lifting from the bed, topical creams simply sit on the surface and never reach the fungal colony. Patients waste months — sometimes years — on products that were never designed for established infections.
The fix: File the nail surface first (reduces thickness by 60-80%), then use a penetrating nail lacquer or pen — NOT a cream. If the fungus covers more than 50% of the nail or the nail is lifting, skip OTC entirely and see a podiatrist for oral terbinafine or laser therapy. In our clinic, we save patients an average of 8 months of failed OTC treatment by properly staging their infection at the first visit.
Warning Signs — When to See a Podiatrist
See a Podiatrist Immediately If You Notice:
- Spreading redness or warmth around the nail — may indicate bacterial infection (paronychia) requiring antibiotics
- Nail fully lifting from the bed — complete onycholysis needs professional debridement to prevent subungual abscess
- Diabetic or immunocompromised — fungal infections can become limb-threatening portals for bacterial cellulitis
- Foul odor with discharge — suggests secondary bacterial infection superimposed on fungus
- Dark streaks under the nail — must rule out subungual melanoma (rare but serious)
- No improvement after 12 weeks of consistent at-home treatment — likely needs oral medication or laser
If this describes you, same-day evaluation is recommended. (810) 206-1402 · Book online →
Conditions That Mimic Toenail Fungus
Not every discolored toenail is fungus. Before your podiatrist confirms onychomycosis, they should rule out several look-alike conditions — because the treatment for each is completely different. In our clinic, we culture or use dermoscopy on approximately 30% of suspected fungal nails, and nearly 1 in 4 turns out to be something else entirely.
Nail psoriasis produces pitting, “oil drop” discoloration, and crumbling that closely mimics fungus. Key differentiator: psoriasis affects multiple nails simultaneously and often accompanies skin plaques on elbows or knees. Nail trauma (common in runners and hikers) causes subungual hematoma or repetitive microtrauma that discolors a single nail — but doesn’t spread. Onychogryphosis (ram’s horn nail) is age-related thickening without true fungal infection — it needs debridement, not antifungals.
Watch: Toenail Fungus Treatment Explained
Watch Dr. Tom explain toenail fungus treatment — causes, the OTC products that actually work, and when you need professional help:
Book your appointment → · (810) 206-1402
More Podiatrist-Recommended Fungus Essentials
Breathable Diabetic Shoe
- Tie-Less Lacing System eliminates the need to tie laces. Heel strap enables to adjust the grip around the heel. Cushioning sole with a mild Rocker adds spring to your step. Soft, padded fabric interior with no overlays eliminates irritation.
Orthofeet Sprint — deep, breathable design reduces fungal growth.
Moisture-Wicking Sock
- Provides continuous support of the Plantar Fascia by gently stretching the fascia tissue.
- Compression zones promote circulation, reduce impact vibration, boost recovery and strengthen feet.
- Lightweight, seamless design with extra cushioning provides support while still being comfortable.
- Supports the heel/arch and overall foot structure while stabilizing the tendon for better performance
- Made from high quality materials, the socks are moisture wicking and breathable.
OS1st FS4 — keeps feet dry, eliminating the warm-wet environment fungus needs.
Breathable Recovery Slide
- Model ID: 1135061-BTRT
HOKA Ora 3 — lets feet air out after closed-shoe exposure.
As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. Product recommendations are based on clinical experience; prices and availability shown above update live from Amazon.

When to See a Podiatrist
Topicals only penetrate the top 30% of the nail plate — if the fungus is near the cuticle or under 50% of the nail, oral terbinafine or laser is usually required for full clearance. Balance Foot & Ankle offers in-office fungal nail diagnostics and laser treatment that reaches the nail matrix where topicals can’t. We’ll examine the nail and recommend the fastest path to clear, healthy regrowth.
Call Balance Foot & Ankle: (810) 206-1402 · Book online · Offices in Howell & Bloomfield Hills
Frequently Asked Questions
How long does it take to cure toenail fungus with an at-home kit?
Mild-to-moderate toenail fungus typically shows visible improvement within 8-12 weeks of consistent treatment with a multi-product kit. However, complete nail replacement (growing out a fully clear nail) takes 9-12 months for toenails because they grow approximately 1.5mm per month. The key is consistency — applying antifungal daily, sanitizing shoes nightly, and wearing moisture-wicking socks every day without skipping.
Can I use nail polish while treating toenail fungus?
We strongly recommend avoiding nail polish during active fungus treatment. Polish creates an airtight seal that traps moisture against the nail plate — the exact environment dermatophytes need to thrive. It also prevents topical antifungals from penetrating. If cosmetic coverage is essential, antifungal nail lacquers with built-in tint (like ciclopirox) are available by prescription from your podiatrist.
Is toenail fungus contagious to family members?
Yes. Dermatophyte spores spread through shared surfaces — shower floors, bath mats, nail clippers, and communal footwear. The risk is highest in warm, moist environments. To protect family members: wear shower shoes in shared bathrooms, use a UV sanitizer on all household shoes, never share nail tools, wash bath mats weekly in hot water, and treat athlete’s foot promptly since it frequently migrates to toenails.
When should I skip the kit and go straight to a podiatrist?
See a podiatrist first if fungus covers more than 50% of the nail, the nail is severely thickened or crumbling, the nail is lifting from the bed, you have diabetes or poor circulation, you’ve tried OTC treatments for 12+ weeks without improvement, or you notice dark streaks under the nail (which requires biopsy to rule out melanoma). These cases need oral medication or laser therapy — OTC kits alone won’t clear them.
Does insurance cover toenail fungus treatment?
Most PPO plans cover toenail fungus evaluation and treatment when medically indicated — especially for diabetic patients where fungal nails are considered a medical necessity due to infection risk. Medicare Part B covers podiatric nail care for qualifying conditions. Balance Foot & Ankle accepts BCBS and most Michigan insurers. Call (810) 206-1402 to verify your specific coverage before your visit.
In-Office Treatment at Balance Foot & Ankle
When at-home kits aren’t enough, our in-office toenail fungus treatments include professional nail debridement, prescription oral terbinafine management, and MLS laser therapy that penetrates the full nail plate to reach the fungal colony directly. Dr. Tom and Dr. Daria have treated thousands of fungal nail cases across our Howell and Bloomfield Hills locations — we’ll stage your infection, determine whether OTC, oral, or laser is right for you, and create a treatment timeline you can trust.
Not improving with home treatment? Learn about our in-office toenail fungus treatment → Toenail Fungus Laser Treatment
Same-day appointments available. (810) 206-1402 · Book online →
The Bottom Line
Toenail fungus isn’t a cosmetic nuisance — it’s a progressive infection that worsens without treatment and can spread to other nails and family members. The single biggest reason OTC treatment fails is treating only the nail while ignoring shoe contamination, moisture, and biomechanics. A complete kit — antifungal pen, UV sanitizer, moisture-wicking socks, Doctor Hoy’s for pain, and PowerStep insoles to reduce nail trauma — gives you the best chance of clearing mild-to-moderate fungus at home. Give the protocol 12 consistent weeks. If you’re not seeing improvement, don’t wait longer — a podiatrist can determine whether you need oral medication or laser therapy to finally clear the infection.
Sources
- Gupta AK, Stec N, et al. “Prevalence and epidemiology of onychomycosis: global overview.” Journal of Fungi. 2023;9(4):418. doi:10.3390/jof9040418
- Lipner SR, Scher RK. “Combination antifungal therapy for onychomycosis.” Mycoses. 2024;67(1):e13685. doi:10.1111/myc.13685
- Borkow G, Elassy M. “Copper-infused socks reduce fungal foot colonization.” Textile Research Journal. 2022;92(15-16):2841-2849.
- Gupta AK, et al. “Topical nail filing and penetration enhancement for onychomycosis.” Dermatologic Therapy. 2021;34(6):e15142.
Toenail Fungus Won’t Clear on Its Own?
Balance Foot & Ankle · Howell & Bloomfield Hills, MI
4.9★ · 1,123 Reviews · 3,000+ Surgeries
Dr. Tom Biernacki · Dr. Carl Jay · Dr. Daria Gutkin
Related guides: Complete Toenail Fungus Guide · Vicks for Toenail Fungus — The Truth · When to See a Foot Doctor for Fungus · Best OTC Fungus Treatment · Best Socks for Toenail Fungus · How to Fix Severe Fungus · Keratin Granulations vs Fungus · Shop Recommended Products
Struggling With Toenail Fungus?
Toenail fungus is stubborn but treatable. Our podiatrists offer prescription-strength options and laser therapy that OTC products can’t match.
Clinical References
- Gupta AK, et al. “Prevalence and epidemiology of onychomycosis.” JAAD. 2000;43(2):244-248.
- Scher RK, et al. “Onychomycosis: diagnosis and definition of cure.” JAAD. 2007;56(6):939-944.
- Elewski BE, et al. “Onychomycosis: pathogenesis, diagnosis, and management.” Clinical Microbiology Reviews. 2011;24(2):247-280.
Insurance Accepted
BCBS · Medicare · Aetna · Cigna · United Healthcare · HAP · Priority Health · Humana · View All →
Howell Office
3980 E Grand River Ave, Suite 140
Howell, MI 48843
Get Directions →
Bloomfield Hills Office
43700 Woodward Ave, Suite 207
Bloomfield Hills, MI 48302
Get Directions →
Your Board-Certified Podiatrists
Ready to Get Back on Your Feet?
Same-week appointments available at both locations.
Book Your AppointmentDifferential Diagnosis: What Else Could It Be?
Several conditions share symptoms with Toenail Fungus and are commonly misdiagnosed in the first office visit. Considering these alternatives is part of every Balance Foot & Ankle exam:
- Nail psoriasis. Pitting, oil-drop spots, salmon patches — responds to topical steroid, not antifungal.
- Nail trauma (runner’s nail). Subungual hematoma from repetitive impact — shoe fit fix, not antifungal.
- Onychogryphosis. Thickened, ram’s-horn nail of the elderly — debridement, not pills.
If your symptoms don’t fit the textbook pattern, ask your podiatrist which differentials they ruled out — that conversation often shortcuts months of trial-and-error treatment.
In Our Clinic
In our clinic, the toenail fungus patient has usually already tried OTC topical antifungals for months with no improvement. We confirm the diagnosis with a PAS stain or fungal culture — because about 30 % of thickened, discolored nails are actually NOT fungal (they’re trauma, nail psoriasis, or keratin granulation from polish). For true dermatophyte onychomycosis, oral terbinafine (Lamisil) remains the most effective treatment with ~70 % cure rate and manageable safety monitoring. Nail laser and topical efinaconazole are options for patients who can’t take oral medication. The nail grows back clear over 9–12 months, not overnight.
Most Common Mistake We See
The most common mistake we see is: Applying OTC antifungal cream onto a lifted or thickened nail where it can’t penetrate. Fix: oral terbinafine or laser therapy for anything beyond early-stage surface discolouration.
Warning Signs That Need Same-Day Care
Seek immediate evaluation at Balance Foot & Ankle if you experience any of the following:
- Spreading redness or warmth around the nail
- Nail fully lifting from the nail bed
- Diabetes or poor circulation (urgent)
- Odour or purulent discharge
Call (810) 206-1402 — same-day and next-day appointments at our Howell and Bloomfield Hills offices.
Pros & Cons of Conservative Care for toenail conditions
Advantages
- ✓ Most cases resolve at home
- ✓ Same-week appointments available
- ✓ Permanent fix exists
Considerations
- ✗ Recurrence common without prevention
- ✗ Diabetics need professional care
Dr. Tom’s Recommended Products for toenail conditions
Affiliate disclosure: As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. We only recommend products we use with patients.
Tolcylen Antifungal Solution Dr. Tom’s Pick
Best for: Most effective topical for fungus
Ready to Get Back on Your Feet?
Same-day appointments in Howell + Bloomfield Twp. Most insurance accepted. Dr. Tom Biernacki, DPM & team.
Book Today — Same-Day Appointments Available
Call Now: (810) 206-1402
About Your Care Team at Balance Foot & Ankle
Dr. Tom Biernacki, DPM · Board-Certified Foot & Ankle Surgeon. Specializes in conservative-first care, minimally invasive bunion surgery, and complex reconstruction.
Dr. Carl Jay, DPM · Accepting new patients. Specializes in sports medicine, athletic injuries, and routine podiatric care.
Dr. Daria Gutkin, DPM, AACFAS · Accepting new patients. Specializes in surgical reconstruction and pediatric podiatry.
Locations: 4330 E Grand River Ave, Howell, MI 48843 · 43494 Woodward Ave Suite 208, Bloomfield Twp, MI 48302
Hours: Mon–Fri 8:00 AM – 5:00 PM · (810) 206-1402
Dr. Tom’s Top 3 — The Premium Foot Pain Stack (2026)
If you only buy three things for foot pain, get these. PowerStep + CURREX orthotics correct the underlying foot mechanics, and Dr. Hoy’s pain gel delivers fast topical relief. This is the exact stack Dr. Tom Biernacki, DPM gives his Michigan podiatry patients on visit one — over 10,000 patients have used this exact combination.
Dr. Tom Biernacki, DPM is a board-certified podiatrist + Amazon Associate. Picks shown are products he prescribes to patients at Balance Foot & Ankle Specialists. We earn a commission on qualifying purchases at no extra cost to you. All products independently tested + reviewed for 30+ days minimum. Last verified: April 28, 2026.
PowerStep Pinnacle MaxxDr. Tom’s #1 Brand
Dr. Tom’s most-prescribed OTC orthotic. Lateral wedge corrects overpronation that causes 90% of foot pain. Deep heel cradle stabilizes the ankle. Built by podiatrists, used by patients worldwide.
- Lateral wedge corrects pronation
- Deep heel cradle stabilizes ankle
- Dual-density EVA — comfort + support
- Trim-to-fit any shoe
- Used by 10,000+ podiatrists
- Trim-to-size required
- 5-7 day break-in for some
CURREX RunProDr. Tom’s #1 Brand
3 arch heights for custom fit (Low/Med/High). Carbon-reinforced heel + dynamic forefoot — the closest OTC orthotic to a $500 custom orthotic. Engineered in Germany.
- 3 arch heights for custom fit
- Carbon-reinforced heel cup
- Dynamic forefoot zone
- Premium German engineering
- Sport-specific support
- Pricier than PowerStep
- 7-10 day break-in
Dr. Hoy’s Natural Pain Relief GelDr. Tom’s #1 Brand
Menthol-based natural pain relief — Dr. Tom’s #1 brand for fast relief without greasy residue. Safe for diabetics + daily use. Cleaner formula than Voltaren or Biofreeze.
- Menthol-based natural formula
- No greasy residue
- Safe for diabetics
- Fast cooling relief — 5-10 minutes
- Cleaner ingredient list than Biofreeze
- Pricier than Biofreeze
- Strong menthol scent at first
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.
- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)
Recommended Products from Dr. Tom