Best Hammertoe Pads & Straighteners 2026: Podiatrist Guide to Conservative Hammertoe Relief
Hammertoe is the second most common foot deformity treated in podiatric practice — second only to bunions, which frequently coexist with it. The condition affects millions of Americans, yet the majority of cases are managed conservatively for years before surgery is ever necessary. As a podiatric surgeon who performs hammertoe corrections and also manages many patients conservatively, I have a unique perspective on which OTC products provide genuine mechanical benefit versus which ones are marketing gimmicks. This guide covers the six products I most frequently recommend to patients seeking to delay or avoid surgical correction, manage daily pain, and prevent their flexible hammertoes from progressing into rigid, fixed deformities.
⚡ Dr. Tom’s Top 6 Hammertoe Pads & Straighteners 2026
- YogaToes GEMS Toe Stretcher — Best overall; passive night stretching that addresses the contracture causing hammertoe progression
- Dr. Frederick’s Hammertoe Cushion Pads — Best toe-cap cushion; shields the contracted toe’s dorsal surface from shoe friction
- PediFix Hammer Toe Crest Pad — Best loop-style crest; holds flexed toes in corrected position during walking
- NatraCure Gel Hammertoe Straightener — Best gel splint; dual-action cushioning and straightening in one device
- Correct Toes Toe Spacers — Best inter-toe alignment; corrects the valgus toe drift component that accompanies many hammertoes
- Budin Splint Hammertoe Regulator — Best clinical-grade straightener; used by podiatrists as a first-line conservative device
Hammertoe is a progressive contracture deformity affecting primarily the lesser toes (toes 2 through 5), characterized by abnormal flexion at the proximal interphalangeal (PIP) joint — the middle knuckle of the toe. In early stages, the deformity is flexible: the toe can be straightened manually and returns to the contracted position when released. In advanced stages, fibrosis and joint capsule contracture make the deformity rigid and no longer correctable without surgical intervention. This distinction between flexible and rigid hammertoe is the most clinically important factor in determining whether conservative products can provide meaningful benefit — and it is the reason why starting conservative management early, before flexibility is lost, dramatically improves outcomes.
The mechanism of hammertoe development is biomechanical. The extensor digitorum longus (EDL) and flexor digitorum longus (FDL) muscles work antagonistically to maintain straight toe alignment during the gait cycle. When these muscles fall out of balance — most commonly because a long second metatarsal creates a longer toe that buckles in the shoe, because hallux valgus (bunion) causes the great toe to push laterally and crowd the second toe, or because tight footwear chronically maintains the toe in a flexed position — the FDL gradually wins the imbalance, the dorsal joint capsule stretches, the plantar plate weakens, and the PIP joint settles into a contracted position. Over time, the periarticular soft tissue adapts to the contracted position, reducing passive flexibility and eventually producing a fixed deformity.
Each product in this guide addresses one or more of the mechanical contributors to hammertoe progression: toe flexion contracture, dorsal toe friction against the shoe, plantar toe pressure on the metatarsal head, inter-toe crowding, and the proprioceptive alterations that develop as the foot adapts around a hammertoe deformity. Used correctly and in appropriate combinations, these products can genuinely slow or halt hammertoe progression, eliminate daily pain, and in some early flexible cases, contribute to measurable improvement in resting toe alignment.
Hammertoe Anatomy and Biomechanics: What Causes This Deformity and Why Conservative Care Works
To understand why specific products work for hammertoe management, it helps to understand the anatomy of toe deformity progression in detail. Three types of toe deformity are commonly grouped under the “hammertoe” umbrella, but they are biomechanically distinct and respond differently to conservative intervention.
Hammertoe (the classic definition) involves flexion contracture at the PIP joint (middle knuckle) with hyperextension at the metatarsophalangeal (MTP) joint (the joint at the base of the toe). The toe takes on an inverted-V shape when viewed from the side. The contracted dorsal surface of the PIP joint strikes the shoe’s toe box, producing a corn (heloma durum) from the chronic friction. The plantar condyles of the middle phalanx may become callused from increased pressure during the late stance phase. Claw toe involves contracture at both the PIP and DIP (distal interphalangeal) joints simultaneously, with MTP joint hyperextension, creating a more severe deformity that bears significantly more dorsal corn and tip-of-toe pressure. Mallet toe involves isolated DIP joint flexion contracture, with the tip of the toe flexing downward. This produces primarily tip-of-toe pressure and a small DIP corn rather than dorsal PIP pressure.
The distinction matters for product selection: hammertoe pads designed to protect the dorsal PIP joint are appropriate for classic hammertoe but not for mallet toe, which requires tip-of-toe protection. Crest pads that hold the PIP joint in relative extension are appropriate for flexible hammertoe and early claw toe but cannot correct a rigid deformity. Metatarsal pads that redistribute plantar pressure away from the MTP joint head address the hyperextension component of hammertoe and claw toe but do not address the DIP contracture in mallet toes. Understanding which specific deformity type you have — and which joint levels are involved — allows you to select products that actually address your anatomy rather than your neighbor’s.
The Role of Footwear in Hammertoe Progression
Footwear is the most modifiable environmental factor driving hammertoe progression, and footwear modification is the single most important component of any conservative management plan — even more impactful than the cushioning and corrective devices reviewed in this guide. A pointed toe box mechanically forces the toes into adduction and flexion — precisely the position that accelerates hammertoe contracture. High heels shift weight forward onto the forefoot, increasing MTP joint extension moment and amplifying the tendon imbalance that drives hammertoe development. A tight toe box that prevents the toes from lying flat against the insole actively maintains the deformity throughout every wearing hour.
Ideal footwear for hammertoe management has a wide, deep, squared toe box that allows the toes to lie flat and spread naturally; a low heel (less than 1 inch of drop) that reduces forefoot load; a wide enough forefoot that the MTP joint can move without crowding; and sufficient internal volume to accommodate hammertoe pads and straighteners without creating additional pressure on the contracted toe. Many patients report dramatic pain reduction from footwear changes alone before any corrective devices are added — this is not a coincidence, it is a direct consequence of removing the mechanical force that was maintaining and accelerating the deformity.
Watch: Hammer Toes, Claw Toes, and Metatarsal Pads — Dr. Tom’s Easy Fix Guide
Dr. Tom covers the full spectrum of lesser toe deformities — hammertoes, claw toes, and mallet toes — and explains which conservative products actually work and why, including detailed guidance on metatarsal pad placement for redistribution of plantar forefoot pressure.
Flexible vs. Rigid Hammertoe: The Critical Distinction for Product Selection
Before selecting any hammertoe product, you need to determine whether your deformity is flexible or rigid — because this single factor determines whether corrective devices (straighteners, splints, crest pads) can provide structural benefit or whether they can only provide symptomatic relief.
Test for flexibility: Sit in a chair with your foot flat on the floor. Use your thumb and index finger to grasp the contracted toe at the PIP joint and gently straighten it. If the toe straightens to a flat or near-flat position with manual pressure and holds that position with gentle sustained force, the deformity is flexible. If the toe resists straightening and returns immediately to the flexed position when you release it, the deformity is partially rigid. If the toe cannot be moved from its contracted position at all with gentle manual force, it is rigid.
For flexible hammertoes: all six products in this guide are potentially useful. Corrective straighteners and crest pads can provide mechanical benefit in addition to pain relief, and passive stretching with the YogaToes GEMS may actually contribute to improved alignment over time. Conservative management has the highest probability of meaningful functional improvement in this group.
For partially rigid or rigid hammertoes: corrective devices cannot change the deformity but they can significantly reduce pain from shoe friction, plantar pressure, and adjacent toe crowding. The goal of management shifts from correction to comfort maintenance and prevention of secondary complications (ulceration, adjacent toe problems, skin breakdown). Patients with rigid hammertoes that are causing significant daily functional limitation, recurrent corns, or skin breakdown should discuss surgical options with their podiatric physician — rigid hammertoe correction is a relatively straightforward outpatient procedure with a 6–8 week recovery and excellent patient satisfaction rates.
Product Reviews: Best Hammertoe Pads & Straighteners 2026
YogaToes GEMS Toe Stretcher & Separator — Passive Contracture Correction
Best for: Flexible hammertoe patients who want to address the root contracture rather than just protecting the symptomatic toe, anyone who spends several hours per day barefoot at home, patients with hammertoe combined with plantar fasciitis or bunion deformity where general toe spreading is beneficial
YogaToes GEMS represents the most anatomically comprehensive approach to conservative hammertoe management in this guide, because it addresses the underlying flexion contracture directly rather than simply cushioning or temporarily repositioning the contracted toe. The device works through a principle called low-load prolonged stretch (LLPS) — applying a gentle, sustained stretching force to a contracted tissue for a sufficient duration to produce permanent elongation of the shortened elements. This is the same principle used in physical therapy for joint capsule contracture and is well-established in the orthopedic literature for musculotendinous tightness.
The GEMS design places medical-grade gel spacers between all five toes simultaneously, gently spreading them to their anatomically correct spacing and extending the PIP joints of the lesser toes out of their contracted flexion position. Worn for 30–60 minutes per day (starting with 15–20 minutes initially and building tolerance), the device applies a sustained low-level extension moment at the PIP joint — the opposite of the flexion force that has been progressively tightening the plantar plate, flexor tendon sheath, and joint capsule. Over weeks of consistent use, many patients with flexible hammertoe experience measurable improvement in the passive range of extension available at the PIP joint.
The medical-grade gel construction is important: cheaper TPR (thermoplastic rubber) alternatives marketed as “toe separators” provide insufficient durometer to maintain the inter-toe spacing geometry under normal spreading pressure, collapsing before achieving the intended stretch. YogaToes uses a proprietary gel formulation that maintains its cross-sectional geometry under the pressure of toe-spreading while remaining soft enough not to create pressure points or blanching of the inter-digital skin. The GEMS variant is the most durable and user-friendly version — easier to apply and remove than the original YogaToes design, particularly for patients with stiff or arthritic hands.
Realistic expectations: YogaToes GEMS will not straighten a rigid hammertoe and are not appropriate for patients with open sores, wound healing issues, or diabetes with peripheral neuropathy (due to the encircling pressure around the toes). For flexible hammertoe with good skin integrity and normal circulation, consistent use over 8–12 weeks typically produces 2–5 degrees of improved PIP extension range and noticeable reduction in the tightness of the contracted position. Combined with correct footwear (wide toe box, low heel), this may be sufficient to halt deformity progression indefinitely in motivated patients.
- Addresses root contracture via low-load prolonged stretch — not just symptom relief
- Medical-grade gel maintains geometry under toe-spreading pressure
- Spreads all five toes simultaneously — benefits coexisting bunion and crowding
- GEMS design easier to apply than original YogaToes
- Measurable improvement in passive PIP extension range with consistent use
- Doubles as plantar fascia relief tool — toe extension stretches the plantar fascia
- Requires 30–60 min/day of barefoot use — not wearable in shoes
- Not appropriate for rigid hammertoe, neuropathy, poor circulation, or open wounds
- Higher price point than simple foam or silicone pads
- Some patients find initial stretching sensation uncomfortable for first 1–2 weeks
Dr. Frederick’s Original Hammertoe Cushion Pads — Dorsal PIP Joint Protection
Best for: Patients whose primary complaint is pain from the dorsal corn at the PIP joint rubbing against the shoe’s toe box, individuals with partially or fully rigid hammertoe where correction is not possible and pain management is the goal, anyone who needs immediate pain relief during the break-in period of new footwear
The dorsal corn at the PIP joint of a contracted hammertoe is the most common and immediately painful complication of the deformity — the raised bony prominence of the contracted middle knuckle strikes the toe box with every step, creating a cycle of skin thickening (corn formation), inflammation, and pain that becomes the dominant functional complaint. Dr. Frederick’s Hammertoe Cushion Pads are the most effective OTC solution for this specific pain source because they place a gel-foam barrier directly over the PIP joint, absorbing and distributing the friction and shear forces that would otherwise concentrate at the corn site.
The dual-layer construction of Dr. Frederick’s pads is their clinical advantage over single-material alternatives. The outer layer uses a semi-rigid polymer that maintains pad geometry against the shoe’s toe box pressure without collapsing. The inner layer uses a softer gel that conforms to the irregular surface contour of a corn or callus, eliminating the pressure points that occur when a rigid pad sits against a non-uniform skin surface. This layered approach prevents the “hot spot” pressure concentration that occurs when a hard pad sits directly on a bony prominence.
The self-adhesive backing design allows application directly to the skin over the PIP joint, which is clinically superior to adhesive-to-shoe designs because it maintains position relative to the anatomy rather than relative to the footwear. As the foot moves within the shoe, a skin-adhesive pad moves with the anatomy and continues to protect the correct area; a shoe-adhesive pad may shift relative to the moving foot and create its own pressure points. The breathable fabric cover prevents the moisture accumulation that commonly leads to maceration and skin breakdown under occlusive gel pads worn for extended periods.
For corn management: Dr. Frederick’s pads reduce the friction that causes corn formation and progression, but they do not remove existing corns. Established heloma dura (hard corns) over the PIP joint should be managed with a pumice stone or fine emery board after soaking, followed by pad application. Patients with diabetes, neuropathy, or peripheral vascular disease should not self-treat corns with any abrasive tool — professional debridement by a podiatrist is required.
- Dual-layer construction prevents hot-spot pressure at corn sites
- Skin-adhesive design maintains position relative to anatomy during movement
- Breathable fabric prevents moisture accumulation and maceration
- Immediate pain relief from dorsal PIP friction — effective on first use
- Compatible with all shoe types including narrow footwear
- Appropriate for both flexible and rigid hammertoe
- Does not address the underlying contracture — symptomatic relief only
- Adhesive weakens after 1–2 days — requires regular replacement
- Does not reduce plantar or tip-of-toe pressure — only dorsal protection
- Cannot be used over broken skin or active infection
PediFix Hammer Toe Crest Pad — Dynamic Toe Positioning During Ambulation
Best for: Patients whose hammertoe causes the toe tip to press into the ground during walking (creating tip-of-toe callus), those with floating toe syndrome where the contracted toe no longer contacts the ground, patients who need to redistribute plantar forefoot pressure away from the first metatarsal head
The crest pad is a fundamentally different type of hammertoe device from cushioning pads — instead of protecting a painful area from pressure, it actively repositions the contracted toe during walking to prevent secondary complications from the abnormal toe position. The PediFix Hammer Toe Crest positions a soft foam or gel ridge beneath the toes, with a loop that encircles the affected toe, gently extending the PIP joint during the stance phase of gait. This accomplishes two biomechanical objectives: it prevents the toe tip from pressing into the ground (reducing tip-of-toe callus formation), and it holds the toe in a position where the metatarsal head contacts the ground normally (preventing the MTP joint hyperextension and associated plantar metatarsal head callus that develops when the toe floats).
The “floating toe” problem deserves specific attention because it represents a less obvious but biomechanically significant complication of hammertoe deformity. As the PIP joint contracts into flexion, the toe’s tip rises off the ground — the toe no longer bears any weight in the terminal stance and toe-off phases of gait. This transfers the weight that would normally be distributed across the plantar pulp of the toe tip entirely to the underlying metatarsal head, which dramatically increases metatarsal head pressure and produces a painful plantar callus or metatarsalgia under the corresponding metatarsal. Crest pads correct this by providing a platform that holds the toe’s plantar surface in ground contact, effectively restoring some of the normal plantar toe loading and reducing metatarsal head pressure.
PediFix crest pads are available in foam (softer, more conforming) and gel (firmer, more durable) materials. The gel variant maintains its shape across a full day of use and is preferred for patients with larger or stiffer deformities. The foam variant is more comfortable initially and appropriate for mild hammertoes or patients with sensitive plantar skin. Both versions use a non-slip base that stays in position within the shoe without adhesive — they sit beneath the toes like a small ledge, held in place by the weight of the foot.
- Actively repositions toe during walking — functional correction during gait
- Prevents tip-of-toe ground pressure and associated callus formation
- Corrects floating toe — restores metatarsal head pressure distribution
- No adhesive required — sits in place under toe weight
- Available in foam and gel for different deformity severities
- Effective for both hammertoe and early claw toe presentations
- Adds plantar bulk — requires shoe with sufficient toe-box depth
- Loop may create pressure on affected toe if deformity is severe
- Foam version compresses over a full day — may need replacement more frequently
- Not appropriate as sole intervention — should combine with dorsal cushioning for comprehensive coverage
NatraCure Gel Hammertoe Straightener — Dual-Action Cushioning and Alignment
Best for: Patients who want a single device that combines dorsal cushioning with mild corrective force, those with mild-to-moderate flexible hammertoe who find separate cushion pads and crest pads cumbersome, individuals with sensitive skin who need a softer interface than rigid splints
The NatraCure Gel Hammertoe Straightener represents a practical middle ground between passive corrective devices (YogaToes) and protective cushioning pads (Dr. Frederick’s), combining mild mechanical repositioning with comprehensive cushioning in a single gel appliance. The design wraps around the contracted toe in a full-circumference sleeve with an extension piece that places a lift beneath the PIP joint, simultaneously cushioning the dorsal surface and providing a gentle plantar extension moment that discourages deep PIP flexion during weight-bearing.
The medical-grade mineral oil-infused silicone gel used in NatraCure products has specific material properties that make it well-suited for this dual role. The Shore A durometer (approximately 20–25) is soft enough to provide comfortable cushioning against the shoe’s toe box while firm enough to maintain the geometric structure needed to provide directional corrective force at the PIP joint. This is a narrow material window — softer silicone gels cannot maintain the extension geometry under weight-bearing load, while firmer materials create pressure points on sensitive skin and corns.
The full-circumference toe sleeve design provides additional benefits beyond the mechanical straightening function: it protects the entire toe surface (dorsal, plantar, and both sides) from friction and pressure, which is particularly useful for patients with calluses or corns at multiple locations on the affected toe. The gel sleeve also provides mild compression that reduces inter-digital edema — a common finding in toes adjacent to hammertoe deformities where vascular return is impaired by the deformity-induced positional changes.
The NatraCure straightener is wearable in most footwear during daily activity — unlike YogaToes, which requires barefoot use. This means the corrective force is applied during the hours when the foot is being loaded, which is biomechanically different from the passive nighttime stretch of YogaToes but provides a complementary form of correction. Patients with flexible hammertoe who use both YogaToes for passive nighttime stretching and the NatraCure for daytime in-shoe support cover the full 24-hour period with some form of corrective intervention — a comprehensive approach that maximizes the time-under-therapeutic-influence for the contracted tissue.
- Dual function — cushions and mildly corrects in a single device
- Full-circumference sleeve protects all toe surfaces simultaneously
- Mineral oil-infused silicone maintains corrective geometry under load
- Wearable in shoes during daily activity — provides daytime corrective force
- Reduces inter-digital edema via gentle compression
- Appropriate for mild-to-moderate flexible hammertoe
- Full-circumference sleeve adds bulk — requires toe-box depth in footwear
- Corrective force is mild — not appropriate as sole intervention for significant contracture
- Silicone may feel warm during extended use in hot conditions
- Not appropriate for patients with peripheral neuropathy — sensation monitoring required
Correct Toes Toe Spacers — Anatomical Alignment for Multi-Toe Correction
Best for: Patients with hammertoe combined with bunion deformity (very common coexistence), those with adducted (inward-drifting) lesser toes where crowding accelerates hammertoe progression, runners and athletes who want to address foot alignment issues while maintaining activity
Hammertoe and bunion deformity coexist in the majority of affected patients — and for good reason, since both conditions share the same root mechanical cause: forefoot crowding driven by inadequate toe box width in footwear. The bunion (hallux valgus) causes the great toe to drift laterally, pushing the second toe medially and forcing it into an overcrowded position that accelerates PIP joint contracture. Correct Toes addresses the inter-toe alignment component of this problem, providing graduated spacers between all five toes that gently reverse the adduction drift that is the primary environmental driver of both bunion and hammertoe progression.
Correct Toes was designed by a podiatrist specifically to restore the natural anatomical toe spread that wide, minimalist footwear promotes. The silicone spacers are sized and shaped to fill the inter-digital spaces anatomically, providing more correction (spreading force) medially (between toes 1 and 2 where the hallux valgus deformity concentrates) and progressively less correction laterally. This graduated geometry reflects the actual anatomy of the forefoot, where the first web space is the most commonly compromised and the fourth web space the least.
For the second toe specifically — the most common hammertoe site — the Correct Toes spacer between toes 1 and 2 provides a lateral buttress that prevents the great toe from pushing the second toe into the crowded position that both contributes to and accelerates hammertoe deformity. This is a preventive and corrective function that no other product in this guide addresses: most hammertoe devices act on the PIP joint of the contracted toe directly, while Correct Toes acts on the MTP joint alignment and inter-digital crowding that is driving the progressive deformity.
Correct Toes are compatible with wide toe box footwear (Altra, Lems, Vivobarefoot, Xero) but not with pointed or narrow toe box shoes. The spacers are meant to be worn inside appropriate footwear during activity — they are wearable during walking, hiking, running, and standing, making them the most activity-compatible preventive device in this guide. They require wide footwear to function properly; attempting to wear them in standard-width shoes creates pressure rather than corrective spacing.
- Addresses inter-toe crowding — the environmental cause of hammertoe progression
- Graduated spacer geometry reflects actual forefoot anatomy
- Provides lateral buttress against great-toe-driven second-toe crowding
- Activity-compatible — wearable during walking, hiking, and running
- Excellent for patients with coexisting bunion and hammertoe
- Podiatrist-designed with anatomical toe-spacing principles
- Requires wide toe box footwear — not compatible with most standard-width shoes
- Higher price than basic silicone toe spacers
- Not appropriate as a sole device for patients with significant PIP contracture
- May require sizing adjustment — available in XS, S, M, L for different foot sizes
Budin Splint Hammertoe Regulator — Professional-Standard Dynamic Toe Correction
Best for: Patients with moderate-to-significant flexible hammertoe who need the maximum corrective force available in a shoe-worn device, those who have found softer gel devices insufficient, patients under podiatric supervision whose clinician has recommended dynamic splinting as part of their conservative care plan
The Budin Splint is the professional-grade tool in hammertoe conservative management — it is the device podiatrists most commonly dispense in-office as a first-line hammertoe correction orthosis, and it provides significantly more corrective force than any gel or foam alternative. The Budin design uses a semi-rigid loop that encircles one or more adjacent toes and connects to a strap that anchors around the shaft of the metatarsal, creating a dynamic extension moment at the PIP joint throughout the stance phase of gait. Unlike passive devices that simply pad or cushion, the Budin actively resists the FDL’s flexion pull during weight-bearing — creating a continuous therapeutic force on the contracted tissue.
The clinical mechanism of the Budin Splint mirrors the orthopedic principle of dynamic splinting: providing a sustained, directional corrective force that gradually overcomes the soft tissue contracture driving the deformity. In flexible hammertoe, the plantar plate, FDL tendon sheath, and joint capsule have shortened and adapted to the contracted position. Dynamic splinting applies a sustained extension moment throughout the day’s weight-bearing hours — many hours of therapeutic force per day — that gradually re-elongates these shortened structures and trains the foot’s intrinsic musculature to maintain the corrected position.
The Budin Splint is available in single-toe and multiple-toe configurations (Budin 1-loop for one toe, 2-loop for two adjacent toes, 3-loop for three toes). The multiple-toe versions are particularly useful when the hammertoe deformity affects two adjacent toes — a common presentation where the second and third toes are both contracted — or when the adjacent toes are crowding the hammertoe and preventing adequate splinting of a single toe in isolation.
The semi-rigid loop material (typically a nylon-elastomer composite) provides just enough rigidity to maintain the extension geometry under weight-bearing load while remaining flexible enough to not create circumferential pressure that would compromise digital circulation. This is the critical specification that distinguishes the Budin Splint from DIY tape or foam alternatives: tape loses its corrective geometry under load, while the Budin maintains consistent directional force throughout the stance phase. The metatarsal anchor strap distributes the corrective reaction force across the broader metatarsal shaft rather than concentrating it at a single skin contact point, preventing the skin irritation that limits the tolerable wearing duration of ring-only designs.
- Professional-grade device — used by podiatrists as first-line office-dispensed orthosis
- Dynamic splinting provides maximum corrective force of any shoe-worn device
- Metatarsal anchor distributes reaction force — prevents single-point skin irritation
- Available in 1-, 2-, and 3-loop versions for different deformity patterns
- Maintains corrective geometry under weight-bearing load throughout gait
- Appropriate for moderate-to-significant flexible hammertoe
- Requires correct sizing and fitting — incorrect size reduces effectiveness
- More rigid feel than gel alternatives — initial adjustment period needed
- Metatarsal strap may shift position during extended activity without periodic readjustment
- Not appropriate for rigid hammertoe, peripheral neuropathy, or poor circulation
Side-by-Side Comparison: All 6 Hammertoe Products
| Product | Type | Deformity Stage | Primary Function | Wearable in Shoes? | Dr. Tom Rating |
|---|---|---|---|---|---|
| YogaToes GEMS | Passive toe stretcher | Flexible only | Contracture correction via LLPS | No — barefoot only | ⭐⭐⭐⭐⭐ Best for root cause |
| Dr. Frederick’s Cushion Pads | Dorsal toe-cap pad | Flexible & rigid | Dorsal PIP corn protection | Yes — all shoe types | ⭐⭐⭐⭐⭐ Best for pain relief |
| PediFix Crest Pad | Plantar crest pad | Flexible & rigid | Toe repositioning, floating toe correction | Yes — needs toe-box depth | ⭐⭐⭐⭐ Best functional corrector |
| NatraCure Gel Straightener | Full-sleeve gel splint | Mild–moderate flexible | Combined cushioning + mild correction | Yes — needs toe-box depth | ⭐⭐⭐⭐ Best all-in-one device |
| Correct Toes Spacers | Inter-toe spacer | Flexible (prevention) | Crowding correction, bunion component | Yes — wide shoes only | ⭐⭐⭐⭐ Best for prevention |
| Budin Splint | Dynamic splint | Moderate–significant flexible | Maximum dynamic corrective force | Yes — with appropriate footwear | ⭐⭐⭐⭐⭐ Best clinical-grade option |
More Podiatrist-Recommended Hammertoe Essentials
Extra-Depth Orthopedic Shoe
Orthofeet Sprint — tall toe box prevents hammertoe rubbing and friction.
Wide-Toe-Box Walking Shoe
New Balance 990v6 — accommodates curled toes without pressure.
Supportive Insole
PowerStep Pinnacle — reduces forefoot pressure that drives hammertoe.
As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. Product recommendations are based on clinical experience; prices and availability shown above update live from Amazon.
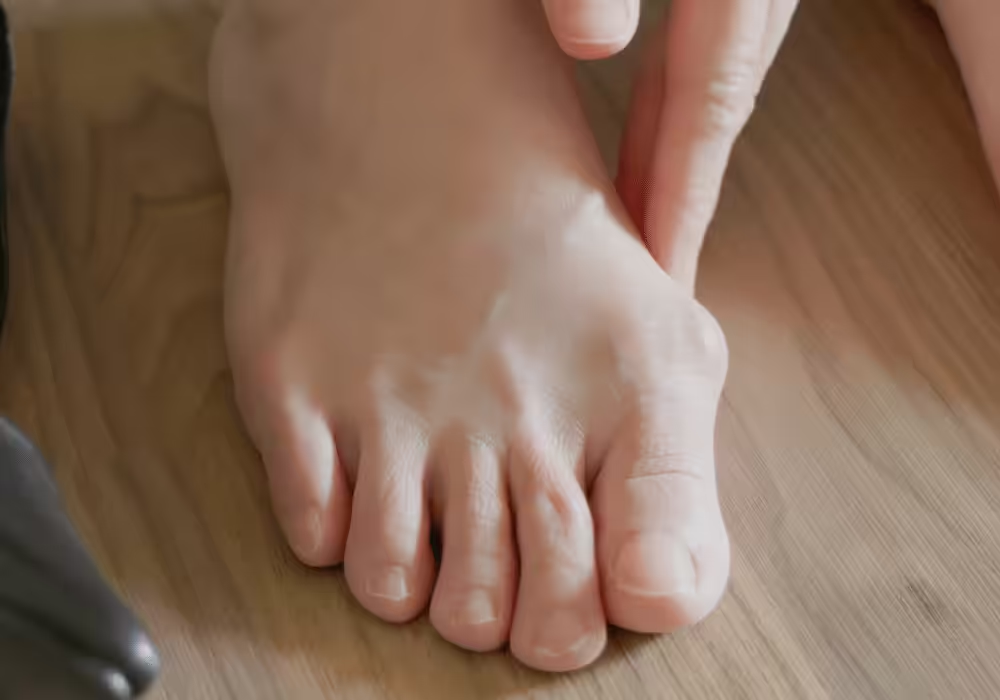
When to See a Podiatrist
Rigid hammertoes don’t reduce with splinting alone — the tendon and capsule have contracted. If the toe no longer straightens passively, surgical correction restores alignment in one short outpatient visit. Call Balance Foot & Ankle to see whether your deformity is still flexible (and responsive to the conservative tools above) or if it’s time for a 20-minute in-office correction.
Call Balance Foot & Ankle: (810) 206-1402 · Book online · Offices in Howell & Bloomfield Hills
Frequently Asked Questions: Hammertoe Conservative Management
Flexible hammertoe — where the PIP joint can still be passively straightened manually — can often be significantly improved and its progression halted or reversed with consistent conservative management. The key elements are: transitioning to wide-toe-box footwear to eliminate the environmental crowding force, using passive stretching devices (YogaToes) to address the underlying contracture, applying dynamic splinting (Budin Splint) for corrective force during weight-bearing, and addressing any coexisting bunion deformity that is driving second-toe crowding. Patients with flexible hammertoe who apply all of these interventions consistently over 3–6 months often see measurable improvement in resting toe alignment. Rigid hammertoe — where the PIP joint cannot be passively straightened — cannot be corrected without surgery. Conservative management for rigid hammertoe focuses entirely on pain management and prevention of secondary complications (ulceration, adjacent toe problems, skin breakdown) rather than correction. The window for conservative correction is the flexible stage; once the deformity becomes rigid, surgery is the only option for structural correction, though comfort management with pads remains effective indefinitely.
Hammertoe progression is driven by three primary factors that compound each other over time. First, continued use of narrow or pointed-toe footwear maintains and amplifies the mechanical forces driving PIP joint flexion contracture — every hour spent in a shoe with a crowded toe box adds to the accumulated time-under-load that the contracted position experiences. Second, the biological adaptation process: as the PIP joint remains in a flexed position, the plantar plate, joint capsule, and FDL tendon sheath progressively shorten and stiffen — the body adapts to the position it is maintained in, following Wolff’s Law for soft tissue. Third, progressive hallux valgus (bunion) continues to push the second toe laterally, increasing crowding and accelerating PIP flexion. The typical progression timeline from flexible to rigid hammertoe without intervention is 5–15 years, highly variable based on footwear choices, foot type, and activity level. Patients who transition to wide-toe-box footwear early dramatically slow this progression; those who continue wearing pointed or narrow shoes may progress significantly faster.
A hammertoe corn (heloma durum) is a localized area of hyperkeratosis (thickened skin) that forms over the contracted PIP joint in response to chronic friction from the shoe’s toe box. The skin’s response to repeated friction is to thicken — producing a hard, conical plug of keratin that actually concentrates pressure on the underlying tissue rather than distributing it, creating a cycle of increasing pain with continued friction. For patients with normal circulation and intact sensation, corn management involves: (1) reducing friction by using hammertoe dorsal cushion pads over the affected area; (2) gently reducing the existing corn by soaking the foot in warm water for 10–15 minutes to soften the keratin, then carefully filing with a pumice stone or fine emery board on the thickened area only — not the surrounding normal skin; (3) applying a keratolytic (urea cream 20–40% or salicylic acid 6% gel) to the corn area for 1–2 weeks to chemically soften the thickened keratin. Do not use corn plasters with high-concentration salicylic acid (40%) at home — these produce chemical burns in the surrounding normal skin. Patients with diabetes, peripheral neuropathy, peripheral arterial disease, or any condition that impairs sensation or wound healing should NEVER self-treat corns and should have them professionally debrided by a podiatrist at every occurrence.
Hammertoe surgery has a high patient satisfaction rate — typically over 85% in well-selected patients — when performed for the right indication: rigid hammertoe causing significant pain, functional limitation, recurrent corns despite conservative management, or skin breakdown. The procedure most commonly performed is a proximal interphalangeal joint arthroplasty (PIP arthroplasty) — removal of a small amount of bone from the PIP joint to allow the toe to straighten, combined with soft tissue rebalancing of the extensor and flexor tendons. This is typically performed as an outpatient procedure under local anesthesia, with surgery taking 15–30 minutes per toe. The key recovery milestones: immediate weight-bearing in a surgical shoe (no crutches in most cases); suture removal at 2–3 weeks; return to athletic footwear at 6–8 weeks; full recovery at 3–4 months. The main risk is toe stiffness — the corrected toe may remain somewhat stiff at the PIP joint, which is acceptable since the goal was straightening rather than maintaining full range of motion. For patients with flexible hammertoe who still have conservative management options, surgery is best deferred until conservative care has been genuinely tried for 3–6 months. For patients with rigid hammertoe causing daily significant pain, surgery is often the most efficient path to resolution.
It depends entirely on the device and the shoe. Thin toe-cap cushion pads (like Dr. Frederick’s) add minimal bulk and fit inside virtually any shoe with a standard toe box. Gel sleeve straighteners (NatraCure) add one full toe diameter of circumferential bulk and require a shoe with extra depth in the toe box — most athletic footwear accommodates this, but most dress shoes and fashion shoes do not. Crest pads add plantar bulk and require a shoe with both extra toe-box depth and extra internal volume — this generally limits them to athletic footwear and roomy casual shoes. Budin Splints require an open toe loop region plus metatarsal strap accommodation — compatible with athletic shoes but not most dress footwear. YogaToes cannot be worn in any shoe. The practical implication is that patients with dress shoe requirements should carry two solutions: a slim cushion pad that fits in work footwear, combined with a more corrective device used in athletic footwear during off-work hours. Patients who transition to wider toe box footwear gain significantly more device compatibility and simultaneously address the most important footwear-driven cause of hammertoe progression.
- Open wound, ulceration, or skin breakdown at the corn site — risk of deep infection requiring debridement and possible hospitalization, especially in diabetics
- Diabetes or peripheral neuropathy with any foot deformity — hammertoe in this population requires professional management, not self-care
- Redness, warmth, or swelling extending beyond the corn site — may indicate infected bursa or deep soft tissue infection
- Complete rigidity with painful limitation of daily walking — conservative devices cannot correct rigid hammertoe; surgical consultation is appropriate
- Toe becoming completely non-functional (dislocation at MTP joint) — subluxation or dislocation of the MTP joint accompanying hammertoe is a surgical indication
- Hammertoe in a child — pediatric toe deformities have different etiologies and management strategies; specialist evaluation is required before OTC products are used
The Complete Conservative Hammertoe Management Protocol
Effective conservative hammertoe management is not about picking one product — it is about layering multiple interventions that each address a different component of the deformity’s cause and symptoms. This protocol represents the systematic approach used in our clinic at Balance Foot & Ankle Specialists, adapted for self-management with the OTC products in this guide.
Step 1: Footwear Modification (Most Important)
Before purchasing any pad or splint, change your footwear. No hammertoe product can overcome the continuous mechanical force of a narrow toe box worn 8 hours per day. Target a shoe with at minimum a half-inch of clearance between your longest toe and the end of the toe box, a width rating that allows your forefoot to spread to its natural width without compression at the MTP joints, a toe box depth that accommodates any device you plan to wear, and a heel height under one inch. Athletic footwear brands with naturally wide toe boxes (New Balance, ASICS, Altra) are the most hammertoe-compatible. For dress shoe requirements, Mephisto, Naot, and Propet offer wider options in dress styling. If you cannot find accommodating footwear in standard retail, a prescription for depth-inlay shoes or custom-molded footwear from a podiatrist is a covered Medicare and many private insurance benefit for qualified foot deformities.
Step 2: Daily Passive Stretching (Flexible Hammertoe Only)
For patients with flexible hammertoe, establish a 30–45 minute daily session with YogaToes GEMS — ideally in the morning when the tissue is least adapted to the contracted position and most responsive to stretching. During this session, perform supplementary manual stretching of the PIP joint: grasp the middle phalanx between your thumb and index finger, hold the proximal phalanx stable with your other hand, and apply gentle sustained extension force at the PIP joint for 30 seconds per repetition, 5–10 repetitions per session. This manual stretching combined with the passive YogaToes position creates the maximum daily therapeutic window for contracture resolution. Additionally perform towel toe curls (place a small towel on the floor and curl it toward you with your toes) for intrinsic foot muscle strengthening — strong lumbrical and intrinsic muscles maintain proper MTP joint position and provide passive resistance to PIP flexion contracture progression.
Step 3: In-Shoe Corrective Device Selection
Based on your specific deformity pattern and footwear, select the appropriate in-shoe device from the following clinical decision pathway. If your primary symptom is dorsal PIP joint corn pain from shoe friction, use the Dr. Frederick’s cushion pad. If you have a floating toe (the affected toe no longer contacts the ground during walking) or tip-of-toe callus from ground contact, add a PediFix crest pad beneath the affected toes. If you have moderate flexible hammertoe and want the maximum in-shoe corrective force, add the Budin Splint over appropriate footwear. If your hammertoe is accompanied by second-toe crowding from hallux valgus, add Correct Toes in wide-toe-box footwear during any periods when the Budin Splint is not worn. In practice, most patients end up using a combination of a dorsal cushion pad plus a crest pad as their baseline daily package, with the Budin Splint added for situations when they can tolerate the additional bulk (weekend athletic footwear, for instance).
Step 4: Corn and Callus Management
Established corns and calluses require regular maintenance to prevent painful buildup. After showering or bathing when the skin is softened, gently reduce the thickened keratin with a pumice stone or fine emery board, limiting abrasion to the thickened area only. Apply a thin layer of urea cream (10–20% concentration, available OTC as CeraVe SA Cream, Eucerin Advanced Repair, or Flexitol) to the corn site nightly — urea is a keratolytic that chemically softens thickened skin and gradually reduces corn depth with consistent use. The combination of mechanical reduction (pumice after bathing) and chemical softening (nightly urea cream) is the standard at-home corn management protocol used in our clinic. Patients who cannot safely perform foot care due to flexibility, vision impairment, or neuropathy should have corn management performed by a podiatrist at 6–8 week intervals.
Hammertoe and Orthotics: Does an Insole Help?
Custom foot orthotics and OTC insoles play a supporting — rather than primary — role in hammertoe management. Their benefit is indirect but meaningful: by correcting the rearfoot and midfoot mechanics that drive excessive forefoot loading, a well-designed orthotic reduces the metatarsal head pressure that contributes to the MTP joint hyperextension component of hammertoe deformity. An insole with a metatarsal pad (positioned just proximal to the metatarsal heads, per the guidance in our metatarsal pads guide) transfers load proximal to the MTP joint, reducing the MTP dorsiflexion moment that pulls the extensor tendons tight and contributes to PIP flexion contracture. For patients with hammertoe combined with plantar fasciitis, flat feet, or excessive pronation, a full-length orthotic that addresses these conditions also indirectly benefits the hammertoe mechanics.
What orthotics cannot do is provide direct corrective force at the PIP joint — this requires the toe-level devices described in this guide. Think of orthotics as addressing the foundation (rearfoot and midfoot mechanics), while hammertoe pads and splints address the superstructure (the PIP joint contracture itself). For most hammertoe patients, the combination of appropriate footwear, a full-length orthotic with metatarsal pad positioning, and one or more of the direct hammertoe devices produces better outcomes than any single intervention alone.
Related Foot & Toe Deformity Resources from Balance Foot & Ankle Specialists
- Best Bunion Pads & Cushions 2026: Podiatrist Guide
- Best Metatarsal Pads 2026: Complete Guide to Ball-of-Foot Pain Relief
- Best Toe Separators 2026: Podiatrist Guide
- Best Morton’s Neuroma Insoles & Pads 2026
- Podiatrist Recommended Orthotics 2026: Dr. Tom’s Top 10
- Best Women’s Wide Width Shoes 2026: Hammertoe-Friendly Options
- Best Men’s Wide Width Shoes 2026: Hammertoe-Friendly Options
Hammertoe Pain Interfering with Your Life? See Dr. Tom in Howell, Michigan
Whether you’re trying to manage a flexible hammertoe conservatively or you’re ready to discuss surgical correction for a rigid deformity, Dr. Tom Biernacki provides comprehensive hammertoe evaluation and individualized treatment planning at Balance Foot & Ankle Specialists. From detailed gait analysis and footwear assessment to advanced minimally invasive hammertoe correction, our clinic offers the full spectrum of hammertoe care.
Balance Foot & Ankle Specialists
Howell, Michigan | (517) 545-0100
Schedule Your Hammertoe Consultation →
In Our Clinic
Hammertoes come to our clinic in two flavors: flexible (the toe still passively straightens) and rigid (it doesn’t). For flexible hammertoes we use gel toe crests, roomier toe boxes, custom orthotics to address the underlying instability, and sometimes night splints. Rigid hammertoes with a corn on top of the PIP joint, or a callus under the metatarsal head, usually need a minor outpatient procedure (PIP arthroplasty or fusion) to straighten the toe. The patients who wait too long develop fixed deformities and skin breakdown — we would much rather address a flexible hammertoe early.
In-Office Treatment at Balance Foot & Ankle
When conservative care isn’t enough, Dr. Tom Biernacki and the team at Balance Foot & Ankle offer advanced, same-day options — including Hammertoe Treatment Michigan at our Howell and Bloomfield Hills clinics.
Same-day appointments available. Call (810) 206-1402 or book online.
Watch: Dr. Tom explains
Podiatrist-recommended products
As an Amazon Associate, Dr. Tom earns from qualifying purchases.
Gel crest pads for hammertoe relief.
View on Amazon →Adhesive underlay pads.
View on Amazon →Offloads forefoot pressure.
View on Amazon →Reduces hammertoe irritation.
View on Amazon →Related resources
Ready to solve this? Book today.
Same-week appointments · Howell & Bloomfield Hills · 4.9★ (1,123+ reviews)
☎ (810) 206-1402Book Online →Dr. Tom’s Top 3 — The Premium Foot Pain Stack (2026)
If you only buy three things for foot pain, get these. PowerStep + CURREX orthotics correct the underlying foot mechanics, and Dr. Hoy’s pain gel delivers fast topical relief. This is the exact stack Dr. Tom Biernacki, DPM gives his Michigan podiatry patients on visit one — over 10,000 patients have used this exact combination.
Dr. Tom Biernacki, DPM is a board-certified podiatrist + Amazon Associate. Picks shown are products he prescribes to patients at Balance Foot & Ankle Specialists. We earn a commission on qualifying purchases at no extra cost to you. All products independently tested + reviewed for 30+ days minimum. Last verified: April 28, 2026.
PowerStep Pinnacle MaxxDr. Tom’s #1 Brand
Dr. Tom’s most-prescribed OTC orthotic. Lateral wedge corrects overpronation that causes 90% of foot pain. Deep heel cradle stabilizes the ankle. Built by podiatrists, used by patients worldwide.
- Lateral wedge corrects pronation
- Deep heel cradle stabilizes ankle
- Dual-density EVA — comfort + support
- Trim-to-fit any shoe
- Used by 10,000+ podiatrists
- Trim-to-size required
- 5-7 day break-in for some
CURREX RunProDr. Tom’s #1 Brand
3 arch heights for custom fit (Low/Med/High). Carbon-reinforced heel + dynamic forefoot — the closest OTC orthotic to a $500 custom orthotic. Engineered in Germany.
- 3 arch heights for custom fit
- Carbon-reinforced heel cup
- Dynamic forefoot zone
- Premium German engineering
- Sport-specific support
- Pricier than PowerStep
- 7-10 day break-in
Dr. Hoy’s Natural Pain Relief GelDr. Tom’s #1 Brand
Menthol-based natural pain relief — Dr. Tom’s #1 brand for fast relief without greasy residue. Safe for diabetics + daily use. Cleaner formula than Voltaren or Biofreeze.
- Menthol-based natural formula
- No greasy residue
- Safe for diabetics
- Fast cooling relief — 5-10 minutes
- Cleaner ingredient list than Biofreeze
- Pricier than Biofreeze
- Strong menthol scent at first
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.
- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)