✅ Medically Reviewed by Dr. Tom Biernacki, DPM
Board-certified podiatric physician & surgeon | Balance Foot & Ankle | Updated April 2026
⚡ Quick Answer: What is Haglund’s deformity and how is it treated?
Haglund’s deformity is a bony bump on the back of the heel irritating the Achilles tendon. Treatment includes heel lifts, physical therapy, and surgery to remove the prominence.
Medically Reviewed by Dr. Tom Biernacki, DPM — Board-Certified Podiatrist, Balance Foot & Ankle | Howell & Bloomfield Hills, MI | 3,000+ surgeries performed
What Is Haglund’s Deformity (“Pump Bump”)?
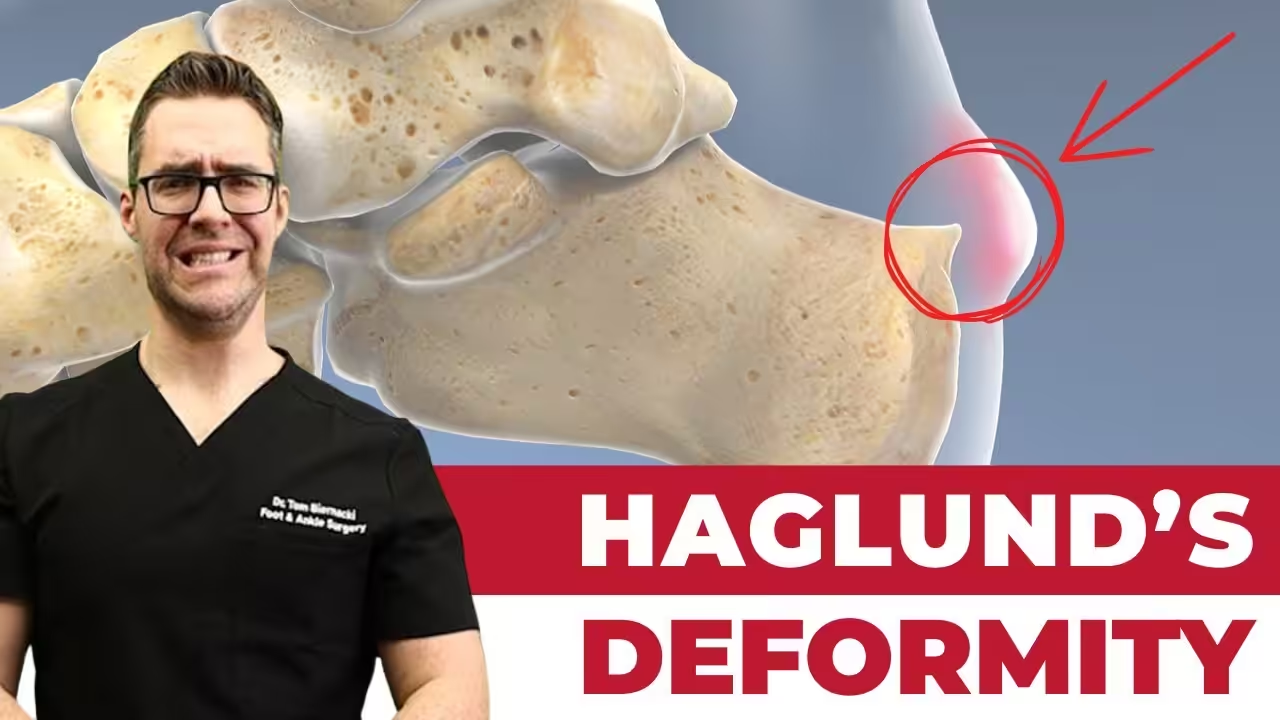
Haglund’s deformity is a bony enlargement at the back of the heel bone (calcaneus) where the Achilles tendon attaches. The bony prominence causes friction against footwear, creating a painful bursa (fluid-filled sac) between the bone and the Achilles tendon. It is commonly called “pump bump” because tight, rigid pump-style shoes aggravate it. Conservative treatment resolves most cases; surgery is reserved for refractory cases.
Haglund’s deformity is one of those conditions where patients often come in after months or years of assuming the lump at the back of their heel is “just how my heel is built” — not realizing it’s a specific, treatable pathology. In our Howell and Bloomfield Hills clinics, we see it frequently in women who wear pumps and high heels, but also in runners and anyone with a high-arched (cavus) foot type. The condition is named after Swedish surgeon Patrik Haglund, who first described it in 1928. What we now understand is that the bony spur itself is only part of the problem — the associated retrocalcaneal bursitis is usually what produces the majority of the pain.
What Is Haglund’s Deformity
The calcaneus (heel bone) has a posterior superior prominence — a naturally rounded bony bump at its top-back corner where the Achilles tendon inserts. In Haglund’s deformity, this normal prominence becomes excessively enlarged, either due to genetic bone shape or repetitive mechanical stress. As the enlarged bony prominence presses against the rigid counter (back) of a shoe, it creates chronic friction on the retrocalcaneal bursa — a fluid-filled sac that normally cushions the Achilles tendon from the bone. This bursa becomes inflamed and thickened (retrocalcaneal bursitis), producing the painful swelling at the back of the heel that patients notice and feel.
Simultaneously, the Achilles tendon itself, particularly the insertional portion, can develop tendinopathy from the same mechanical irritation. This triad — bony enlargement + retrocalcaneal bursitis + insertional Achilles tendinopathy — is what podiatrists call the “painful heel syndrome” of Haglund’s deformity. Understanding all three components matters because treatment must address all three to succeed.
Symptoms and What It Feels Like
The hallmark presentation of Haglund’s deformity is a painful, visible bony bump at the back of the heel, typically at the top-back corner of the calcaneus — just above where most shoe counters press. The bump is hard (it’s bone), often with a soft, spongy overlay (the inflamed bursa) and red, irritated skin from shoe friction. Pain is typically worst when wearing shoes with a rigid back and better in open-backed shoes, sandals, or barefoot. Running and walking on inclines worsens pain, as does any activity that engages the Achilles tendon under tension.
Causes and Risk Factors
Haglund’s deformity has both structural and environmental causes. Structurally, a high-arched (cavus) foot type tilts the heel into inversion, which causes the superior-posterior calcaneus to protrude more prominently against footwear. A tight Achilles tendon further increases the mechanical load at the insertion site. Environmentally, the most significant factor is footwear — specifically shoes with rigid backs (pumps, dress shoes, skates) that directly compress the posterior heel. The combination of bone shape + tight Achilles + rigid footwear creates a perfect storm for this condition.
| Risk Factor | Mechanism |
|---|---|
| High-arched (cavus) foot | Heel inversion increases posterior calcaneal prominence |
| Tight Achilles tendon | Increases tension at Achilles insertion, compresses bursa |
| Rigid-backed footwear (pumps, dress shoes) | Direct friction on posterior calcaneal bump |
| Female sex | Higher prevalence of pump-style footwear |
| Running (particularly hill running) | Repetitive Achilles loading at insertion |
Diagnosis: How We Identify It
Diagnosis of Haglund’s deformity is primarily clinical — the combination of posterior heel pain, visible bony prominence, and shoe-related aggravation is characteristic. We confirm with weight-bearing X-rays, which show the enlarged posterior-superior calcaneal prominence and allow measurement of the parallel pitch lines (PPL) angle — a radiographic measure of the posterior calcaneal protrusion. An angle greater than 44 degrees on the PPL measurement is considered diagnostic. MRI or diagnostic ultrasound is used when we need to assess the Achilles tendon for insertional tendinopathy, the retrocalcaneal bursa for thickness, or when surgical planning requires detailed soft tissue information.
Treatment Options
The vast majority of Haglund’s deformity cases (approximately 90%) respond to conservative treatment over 3–6 months. The guiding principle is to simultaneously offload the Achilles insertion and reduce friction on the bony prominence. This requires addressing footwear, Achilles flexibility, and local inflammation — all three simultaneously. Treating only one component is why many patients plateau with partial improvement and return to us having tried “everything” without success.
Conservative Treatment Protocol
Step 1 — Footwear Modification (immediate)
- Eliminate or minimize all rigid-backed shoes — the #1 intervention
- Heel lifts (5–10mm) in all footwear to reduce Achilles tendon tension at insertion
- Open-backed shoes or clogs allow complete symptom relief during the healing phase
- Silicone heel cups protect the prominence from shoe friction
Step 2 — Achilles Stretching (daily)
- Gastrocnemius stretch: straight knee, 30 seconds × 3, 3× daily
- Soleus stretch: bent knee, 30 seconds × 3, 3× daily
- Night splint if morning Achilles tightness is significant
Step 3 — Anti-inflammatory Measures
- Ice pack to the bursa area after activity: 15 minutes
- Doctor Hoy’s Natural Pain Relief Gel applied to the posterior heel — reduces bursitis inflammation
- Corticosteroid injection into the retrocalcaneal bursa (not into the Achilles tendon) — performed in-office
Step 4 — Orthotics
- PowerStep Pinnacle provides heel cup that cushions the prominence and mild heel lift
- Custom orthotics for significant cavus foot deformity — redistributes ground forces away from Achilles insertion
When Surgery Is Needed
Surgical treatment is considered when conservative management over 4–6 months fails to provide adequate relief, when MRI shows significant insertional Achilles tendinopathy alongside the Haglund’s prominence, or when the bone deformity is severe enough that footwear modification cannot sufficiently offload it. The procedure — calcaneal osteotomy for Haglund’s deformity — involves removing the posterior-superior prominence of the calcaneus under general or regional anesthesia. Recovery requires a walking boot for 4–6 weeks, followed by physical therapy for 8–12 weeks. Full return to sport typically takes 4–6 months. In our practice, we perform this procedure endoscopically when possible (2 small incisions) which significantly reduces recovery time compared to open surgery.
Differential Diagnosis
Several conditions produce pain at the posterior heel and must be distinguished from Haglund’s deformity, as they require different treatments. The most important is insertional Achilles tendinopathy without bony deformity — this has identical symptoms but no palpable hard bump. Posterior calcaneal apophysitis (Sever’s disease in children) produces heel pain at the Achilles insertion in skeletally immature patients. Calcaneal stress fractures from overuse can be mistaken for posterior heel bursitis. Septic bursitis (infected retrocalcaneal bursa) is rare but urgent — it requires immediate drainage and antibiotics.
| Condition | Distinguishing Feature |
|---|---|
| Insertional Achilles tendinopathy (no Haglund’s) | Tendon pain at insertion, no bony prominence on X-ray |
| Retrocalcaneal bursitis (isolated) | Soft spongy swelling, no hard bony bump |
| Calcaneal stress fracture | Diffuse heel pain, positive squeeze test, MRI confirms |
| Sever’s disease (apophysitis) | In children only (8–14 years), bilateral often |
| Septic bursitis | Warmth, erythema spreading, fever — urgent evaluation |
The Most Common Mistake with Haglund’s Deformity
The most common mistake we see is patients continuing to wear the offending footwear while trying every other conservative treatment. They’ll come in having tried stretching, orthotics, ice, topical gels — but they haven’t changed their shoes because “those are my work shoes.” Conservative treatment for Haglund’s deformity cannot succeed while the bony prominence is under daily mechanical friction from rigid footwear. Shoe modification is not optional — it is the foundation of every other treatment. Without it, the bursa remains chronically inflamed, the Achilles tendon remains irritated, and patients predictably fail conservative care and end up in surgery that could have been avoided.
Warning Signs Requiring Immediate Evaluation
🚨 Red Flags — These Need Same-Day Evaluation
- Sudden “pop” at the back of the heel — possible Achilles tendon rupture (urgent evaluation)
- Warmth, spreading redness, fever — possible septic bursitis (ER or urgent care)
- Complete inability to rise on toes — Achilles integrity compromised
- Rapidly enlarging lump — rule out soft tissue mass (lipoma, ganglion, rare tumor)
- No improvement after 6 months conservative care — surgical consultation indicated
Recommended Products for Haglund’s Deformity
Dr. Tom’s Haglund’s Relief Kit
Doctor Hoy’s Natural Pain Relief Gel — Bursitis Inflammation Control
Arnica + camphor topical formula. Apply directly over the posterior heel bursa area 2–3× daily. Reduces retrocalcaneal bursitis swelling and provides local pain relief. Preferred over Biofreeze for posterior heel application — better skin tolerance with daily use.
Not Ideal For: Broken or blistered skin at the heel; camphor-sensitive patients.
PowerStep Pinnacle Insoles — Heel Cup Cushioning + Lift
The built-in heel cup provides padding between the calcaneal prominence and shoe counter, while the mild heel elevation reduces Achilles tendon tension at the insertion. A practical first-line orthotic for Haglund’s before custom orthotics are considered.
Not Ideal For: Open-backed shoes (use heel pad alone); very narrow dress shoes.
In-Office Treatment at Balance Foot & Ankle
If you have a painful bump at the back of your heel, an in-office evaluation will determine whether it’s Haglund’s deformity, isolated bursitis, or insertional Achilles tendinopathy — three conditions that look similar but have different optimal treatments. We take weight-bearing X-rays, measure the PPL angle, and perform diagnostic ultrasound to assess both the bursa and Achilles tendon integrity. From there, we create a personalized treatment plan ranging from footwear modifications and orthotics all the way to endoscopic calcaneal surgery when indicated. View our heel pain treatment options or call (810) 206-1402 for same-day appointments.
Painful Bump on the Back of Your Heel? We Can Help.
Dr. Tom Biernacki, DPM · 4.9 stars · 1,123 reviews · Howell & Bloomfield Hills, MI
Book an Appointment →Or call: (810) 206-1402
Frequently Asked Questions
Can Haglund’s deformity go away on its own?
The bony prominence itself does not resolve without surgery — bone does not reabsorb on its own. However, the associated retrocalcaneal bursitis and Achilles irritation that cause most of the pain can resolve with conservative treatment over 3–6 months. Many patients achieve excellent pain control with footwear changes, orthotics, and stretching, even though the bony bump remains visible.
Is Haglund’s deformity the same as a heel spur?
No — they are different conditions. A plantar heel spur is a bony growth on the bottom (plantar) surface of the heel, associated with plantar fasciitis. Haglund’s deformity is an enlargement of the posterior-superior (top-back) calcaneus at the Achilles insertion. Different locations, different causes, different treatments — though both cause heel pain.
What shoes are best for Haglund’s deformity?
Open-backed shoes, clogs, sandals, and soft-backed athletic shoes are best. Avoid rigid dress shoes, pumps, ice skates, ski boots, and any footwear where a firm counter presses against the posterior heel. When closed-back shoes are required (work, formal occasions), add a silicone heel cup to cushion the prominence and a heel lift to reduce Achilles tension.
How long does Haglund’s deformity take to heal?
Conservative treatment takes 3–6 months to achieve maximal improvement. Footwear changes provide relief within days to weeks. Stretching and anti-inflammatory measures reduce bursitis swelling over 4–8 weeks. If surgery is needed, full recovery takes 4–6 months after the procedure.
When should I see a podiatrist for heel pain?
See a podiatrist if you have a visible bony bump at the back of the heel, if posterior heel pain persists beyond 2 weeks of home care, if you suspect Achilles tendon involvement, or if pain is limiting your daily activity. Same-day appointments: Balance Foot & Ankle (810) 206-1402.
Does insurance cover Haglund’s deformity treatment?
Yes. Haglund’s deformity evaluation and treatment — including X-rays, custom orthotics (with documentation), corticosteroid injections, and surgery — is covered by most health insurance plans including Medicare and Medicaid. Prior authorization may be required for surgery and custom orthotics. Call (810) 206-1402 to verify your coverage.
Sources
- Haglund P. “Beitrag zur Klinik der Achillessehne.” Z Orthop Chir. 1928;49:49-58.
- Pavlov H, Heneghan MA, et al. “The Haglund syndrome: initial and differential diagnosis.” Radiology. 1982;144(1):83-88.
- Leitze Z, Sella EJ, Aversa JM. “Endoscopic decompression of the retrocalcaneal space.” J Bone Joint Surg Am. 2003;85(8):1488-1496.
- Vaishya R, Agarwal AK, et al. “Haglund’s Syndrome: A Commonly Seen Mysterious Condition.” Cureus. 2016;8(10):e820.
- Moroney PJ, et al. “Conservative treatment of Haglund’s deformity.” Foot Ankle Int. 2008;29(12):1188-93.
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.
- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)