Heel Pad Syndrome [Causes, Symptoms, Diagnosis & Treatment]
Do you have heel fat pad atrophy or heel pad syndrome? We review the best shoes for heel pad syndrome & heel fat pad pain!
Heel fat pad syndrome treatment & symptoms video:
How to treat heel pad syndrome & symptoms video summary:
🦶Do you have Bottom of the Foot Pain or Heel Pad Syndrome? This might be Foot Fat Pad Atrophy!🦶
Foot fat pad atrophy is when the disappearing cushion causes heel pad syndrome or ball of the foot pain and bottom of the foot pain.
0:00 Heel Pad Syndrome Treatment & Fat Pad Atrophy Treatment
0:55 What causes fat pad atrophy, fat pad syndrome, and heel pad syndrome
1:20 Fat pad atrophy ball of the foot
1:37 Heel Fat pad atrophy
1:50 Fat pad atrophy podiatrist
2:15 Can fat pad atrophy be reversed
2:42 Foot fat pad atrophy causes
3:00 Calcaneal fat pad atrophy
3:40 Best slippers for foot fat pad atrophy
4:10 Best shoes for fat pad atrophy
5:18 Best shoe inserts for fat pad atrophy
5:54 Foot fat pad exercises
6:15 Foot fat pad atrophy surgery
6:40 Fillers for foot fat pad atrophy
7:25 foot fat pad atrophy cure
7:35 Fat pad atrophy causes
8:03 Massage for the bottom of the foot pain
9:13 Stretches for the bottom of the foot pain
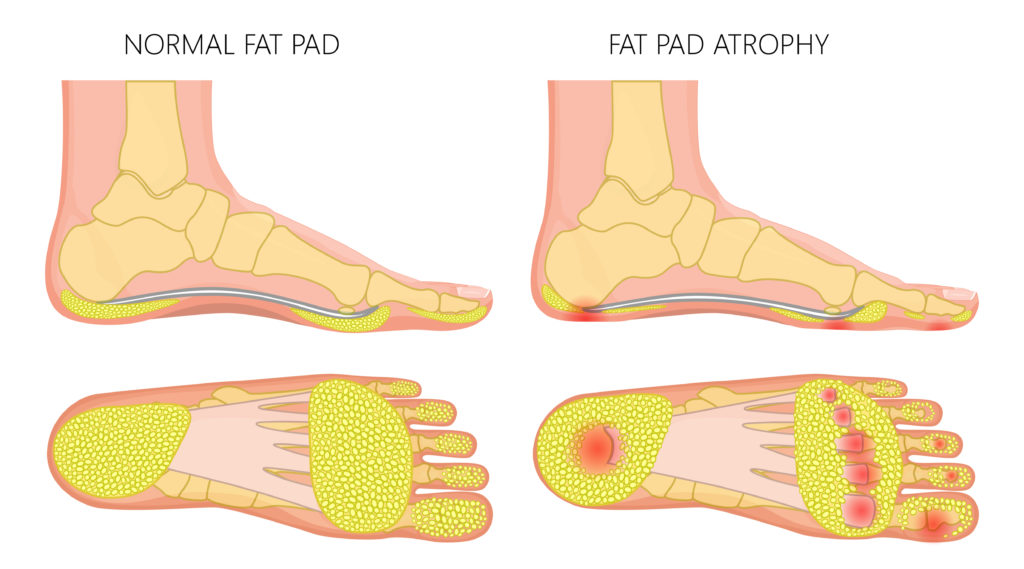
What is heel pad syndrome?
Heel pad syndrome is an ailment that can progress due to the changes in the overall elasticity and depth of the heel pad. It is characteristically progressed because of wear and tear in the muscle filaments and fatty tissue that cushioned the sole pad of your feet.
The most distal part of the human body is the feet. Mainly their role is balancing the body posture, transmitting body mass to the ground without putting too much pressure on the inner tissues, and helping the inaccurate movement. Heels are the point of the first contact between the body and the ground, made of calcaneus bone, cushioned with muscle layer and a covering of calcaneal fat. This fat layer is made with a thickness of 1-2 cm, and an average healthy body measures a width of 18 mm.
The heel pad is made up of a thick layer of muscle tissue with dense pockets of fat. Muscle fibers surrounded these pockets of fat and made a tough but elastic and flexible covering that supports the heel sole. These heel pads help us during running, jumping, and walking, acting as a cushion with a distribution of body weight by absorbing a sudden shock wave and shielding the body frame of joints and bones. We may not feel it in our daily routine, but our heels bear a great to protect us from a sudden trauma or injury. Heel soles endure this wear and tear over a while, but too much work and burden on heel pads cause a shrinkage in the normal size of muscles with a loss of flexibility. This drop-in elasticity absorbs less shock, ultimately leading to a syndrome named heel pad syndrome. With this illness, the normal workout of heel pads is compromised in the sense of standing, running, and jumping, initiating inflammation, soreness, and discomfort of the whole body.
Heel pad syndrome is also termed heel fat pad syndrome (HFPS). This happens due to a change in pliability and thickness of fatty tissue in the heel pad due to an excessive workload for a long time. Fat thickness reduces in size or atrophy of the sole pad (Fat pad syndrome), and the sole cushion becomes less resistive to pressure and shock. This is ranked as second to the principal cause of plantar heel pain with a percentage of 14.8% afterward to plantar fasciitis, but it is quite different from it. Our feet tolerate a lifetime of irrational use. It is believed that human feet go for 100,000 miles approximately in a century. The pressure-bearing capacity of heels for the body’s bulk is 110 % and 200 % during walking and running. This excessive use and chronic intensification in pressure and weight forces cause thinness of the heel fat, progressing to a severe ache in the heel. In addition to this, the natural process of degeneration upsurges with multiple other factors affecting the fat layer in the heel, causing displacement compromised the protection of the heel bones resulting in the pain and disability known as heel pad syndrome.
Risk factors and important causes of heel pad syndrome
Various factors play an important role in the development of heel pad syndrome, and sometimes this illness is accredited to a combination of certain other factors. These factors include:
- Process of Aging: with the increase in age, many major systems of our body go through degeneration in which these systems become less active. This includes not only major systems of the body but also the soft tissues of our body. The aging process affects the heel pad’s soft tissues and fat layer, decreasing its elasticity and thickness. As we grow and with more use, mostly above age 40, the fatty covering in the underlying tissue starts to disrupt along with it, loss of collagen fibers and muscle tissues occurs. Lose in shock absorbency make us more susceptible to the bruising of the heel bone and pain.
- Injury or sudden trauma: Any injury or trauma in the heel pad may lead to heel pad syndrome. This injury might result from playing high-level sports and games or any accident that could damage directly to the heel pad.
- Obesity: The more the body weight, the more pressure it puts on the heels, decreasing the flexibility of the heel muscles and the heel fat pad.
- General problems with gait and structure of the body: Sometimes, the issues with gait and general frame of the feet, knees, hip joint, and ankle joint can change the pattern of walking due to unequal distribution of the weight across the feet, which ultimately results in serious injury or deformity of the heel pad leading to the heel pad syndrome.
- Inappropriate footwear: Wearing improper footwear that is not supportive to the feet, especially during the activities of weight bear or in strengthening exercises, can aggravate the losing of tensile strength of the heel pads.
- Tough/rigid surfaces: Heels prone to hard surfaces during walking or exercise may lead to the stiffening of the heel sole, decreasing the capacity of the shock absorbance and pain in the heel pad.
- Tiresome activities: Any repetitive activity of the body which makes the body feel tiresome, like standing, running, walking, jumping, and jogging, cause chronic changes in the heel muscles leading to the development of inflammation and loss of original strength of the heel pads.
- Plantar fasciitis: Due to the degeneration in the plantar fascia and impaired activity of absorbing shock and supporting the feet, it may result in more stress on the heels and eventually the heel pad syndrome.
- Injections of Corticosteroids: Corticosteroid injections may lead to the atrophy of the muscles of the heel instead of reducing pain and inflammation in the heel pad. This might be the side effect of the corticosteroid injections causing degeneration of the muscles.
- High arched feet: The individuals having high arched feet and involved in running and high activity games are probably more prone to the heel fat pad syndrome due to the displacement of the fay layer in the heel.
- Genetics or family history of heel pad syndrome: If there is any previous history of heel pad syndrome, it will strongly advocate the loss of heel fat and degeneration of the muscle fibers.
- Additional health conditions: Certain other health problems like lupus, rheumatoid arthritis, and Diabetes mellitus are also associated with the development of heel fat syndrome with a loss in adipose tissue and erosions in the collagen fibers in the heel area. Moreover, diabetic patients may suffer from peripheral neuropathy and lose peripheral nerves supply to the legs and feet. This tends to misplace some nerve sensations in the heel area with an inability to feel pain, putting more pressure on the heel, leading to the permanent loss of muscle tissue in the heel pads.
- Wearing inappropriate shoes: Wearing shoes that are not compatible with your feet may cause heel pain and inflammation.
Common symptoms of the heel fat pad syndrome: The individuals suffering from heel pad syndrome will likely observe some of these common symptoms:
- The heel feels deep pain, characteristically in the mid of the calcaneal bone, causing ache around the heel pad.
- The feeling of pain often seems like there was an internal injury or bruise in the sole, felt during walking, running, jumping, or standing.
- Sense of pain can be re-felt by tapping or pressing the heel sole.
- The intensity of the pain increases with a continued activity of walking, running, and jumping, particularly barefooted on hard surfaces.
- In chronic cases, the individuals cannot walk and run due to the severe pain in their heels.
Less commonly observed symptoms are prickly, burning, or cold sensation in the heel due to the neurological problem in the nearby nerves, located superficially after the muscle and fat atrophy in the heel pad.
Minor cases of the heel pad syndrome are non-symptomatic or rarely can be felt by pressing the heel sole or when the heel comes in contact with a hard object or surface like a concrete floor.
Diagnosis of heel pad syndrome
If you are suffering from heel pain, it is important to approach your physician for a proper diagnosis and specific treatment of your heel pad pain.
- A good physician always takes your medical history to reach a proper diagnosis and treatment. Other medical conditions like arthritis, lupus, diabetes mellitus, and nerve damage may also contribute to heel pad syndrome. Your physician will ask you in detail the type, duration, time, and intensity recurrence of pain, and you must give their proper detail of your medical condition.
- After taking your medical history, your health care professional will make a physical examination of your feet for any visible abnormality or deformity in the heel. With this, he will observe the exact location of the pain by moving the fingers from the bottom to the upper side. Sometimes, the heel bones are felt by pressing the skin to check any structural abnormality in the sole bones.
- To check the elasticity of the heel pad, another examination is performed, which measures the variation in the thickness of the heel sole during standing, sitting, and lying positions as ache heel pads do not bear more weight which will give a clue to your doctor about your heel condition. If your heel pads are stiff and hard, you can’t compress your heel, which gives the idea of little flexibility of your heel muscles, which will not support your body weight.
- An X-ray examination is also performed to eliminate other medical issues which have similarities in the presentation to heel pad syndromes like plantar fasciitis and heel bone fracture.
- The above-mentioned clinical diagnostic techniques are standard procedures. However, in case of ambiguity where these procedures do not give a conclusive remark, ultrasound (US) and MRI are performed as these are the advanced diagnostic tools.
Treatment of the heel pad syndrome
Heel pad syndrome can be treated through proper management and treatment therapy, and it is categorized into two methods:
Conservative therapy for heel pad syndrome
In the conservative approach, the primary goal is to manage the signs and symptoms by reducing the inflammation and ache in the heel and improving the quality of life. It does not include the replacement of lost fatty tissues in the heel. It attempts to preserve and protect the remaining fat and muscle tissues in the heel pad to prevent further damage and reduce inflammation, which allows the natural healing process in the heel sole.
Treatments under this category include:
- Proper rest: Whenever you feel this kind of pain in your heel, it is necessary to take proper rest, walk less, avoid heavy exercise and sports, do not carry a heavy load, reduce your walking and standing time.
- The icing of the feet: Icing of feet has a good impact in reducing the inflammation and pain in your heel pad. After every hectic activity that may cause heel pain, try to ice your feet for at least 20 minutes. This will soothe your heels. There are slippers available for ice therapy, convenient in use, and available. These footwears provide comfortable icing to feet minimizing heel pain and inflammation.
- Physical therapy of massage: Manual massage method includes restoration exercises for the leg, feet, and ankle joint. Massaging the soft tissue of the heel found an effective method in relieving the discomfort in the heel pad.
- Relaxing low-dye taping method: This technique has been proven effective in treating the heel pad syndrome, commonly used in the treatment of plantar fasciitis than heel fat pad syndrome, but research reports have declared this a great tool in heel pain syndrome. The tapping approach produces an anti-pronation effect reducing the inflammation and pain in the heel with a dispersion of the pressure in the plantar region. This technique is a useful and convenient tool mainly indoors where orthotics and heel pads are less suitable, as it cushions the heel by increasing the thickness of the fat in the heel pad. There are modified versions of the taping method, most frequently used version that is found to be more active in heel pad syndrome is the addition of taping figure-8 type around the heel zone.
- Use of medicines: Certain medicines like analgesics (pain reliever) and anti-inflammatory drugs, Ibuprofen and Voltaren, help reduce heel ache.
- Use of orthotics and heel cups: One of the most operative conservative approaches used in treating heel pad syndrome is the use of heel cups and suitable shoe inserts. This approach lessens the load on the heel area and provides a cushion and support to the thin and stiff heel area. Heel seats use the fascia bar’s unique and groundbreaking idea by absorbing the stress and providing support during standing, walking, and running. Keraton stuffed dense heel cushions prevent moisture, bacteria, and shoe sliding during the walk. Furthermore, heel seats put mild therapeutic acupressure on the heel’s bones, which boosts the natural healing process. This is overall. A cheap and active treatment can be obtained online in custom sizes with or without a prescription by a physician. Additionally, gel treatment can also be used in reducing pain and inflammation in the heel pad.
Innovative/non-conventional methods of treatment:
Where the conventional methods do not give conclusive results or in the cases of heel fat atrophy, there, the advanced methods help the patients relieve heel fat pad syndrome. The physicians suggest replacing the thin heel fat pads to get more noticeable consequences and prevent future damage. Fat replacement techniques have many degrees of success and are categorized under the term of augmentation of the heel pad, which is further divided into three classes:
- Injectable therapy: various materials are used as injectables that thicken the shrunken parts of the heel fat pad. These filled out the dermis and underlying tissues with fat and are known as dermal fillers. Dermal fillers are both natural and synthetic and are infused into the skin, where they increase the volume of that specific area of the heel. The practice of dermal fillers comprising poly-L-lactic acid and hyaluronic acid for handling heel pad syndrome is one of the most popular techniques used worldwide by physicians. It provides a quick and easy intermediate solution to heel pain. Dermal fillers have almost no side effects, with minimal bruising, stiffness, and a little inflammation in the heel area. The recovery period is quick in this case as the person can resume walking on their feet instantly after the procedure, wearing suitable footwear, and avoiding advanced exercises. The efficiency of the results depends on the material of the filler, stage and weight of the patient, activity, and lifestyle, and the degree of deformity in the fat layer. Some dermal fillers like silicone have negative impacts on the body, too, as it moves from one part to the other, causing adverse effects on the body. Moreover, it might cause a foreign body reaction having negative effects.
- Fat transplantation or auto lipo-transplantation: This is also known as grafting of the fat or fat augmentation as it involves displacement of fatty tissues from one part of the body where it is present in high concentration to another part, i.e., heel where it is in low concentration (the site of graft). This procedure needs a small volume of fat tissue, just a few cubic centimeters, with local anesthesia at the harvesting and grafting sites to avoid the sensation of pain and bruising during the practice. Auto lip-transplantation or autografting techniques of heel pad do not need hospitalization as they are quick and can easily be performed at the doctor’s clinic with the discharge of the patient on the same day. The recovery period takes time. The bandage must be done for 24hrs, approximately three weeks are required for a quick recovery with great care during walking and other activities. This technique has a success rate of 98 %, which is much more than the other techniques discussed. Results are long-lasting as compared to the derma fillers. But care in wearing suitable cushioned shoes with reduced weight-bearing actions is the primary key to success.
- Allografting: This is the third method, similar to autografting, but here the source of fat is another individual. The fat is obtained from the donor and grafted into the heel of the patient (recipient). The fat cells of the donor are not living to certify that the recipient’s body will not reject it. This technique is more complex and requires a proper surgical atmosphere, with six to eight weeks taken for recovery purposes, as the graft takes time to unite with the receiver’s tissue. Still, once it joins with the patient’s tissue, it gives remarkable results with relief of heel fat pad syndrome.
Treatment of underlying deformity or abnormality: If heel pad syndrome is due to an underlying deformity that puts too much weight and stress on the heel, it is central to address this abnormality by treating it. Individuals with diabetes mellitus often develop claw toe deformities, other people with ankle and knee joint deformity issues, the treatment for this kind of individuals is either conservative or surgical depending upon the physician’s choice.
Prevention of the heel fat pad syndrome:
As we have discussed above, many factors are contributing to the development of heel pad syndrome. Some of these factors cannot be sidestepped, such as the age and genetics of the patients. However, others can be negated with proper measures and a healthy lifestyle.
- Wearing proper footwear that is tightly cushioned and provides support to the heel pad all the time.
- During the high-impact activity, wearing of supports shoes.
- Reducing the intensity and period of advanced exercises and heavy activities, such as running, jogging, prolonged standing, and jumping, guarantee the quick recovery of the heel pad after an activity.
- Wearing high heels, especially pointed heels, must be avoided, as these heels distribute the body weight unevenly and put too much pressure on the feet.
- Barefooted walking should be avoided, particularly on hard surfaces.
- Check the durability and condition of your athletic shoes regularly and try to change when you observe any reduction in their cushion.
- Sustain a healthy body weight to avoid heel pad syndrome
Heel fat pad syndrome vs. Plantar Fasciitis:
Heel fat pad syndrome is usually misdiagnosed with plantar fasciitis. Although both are associated with heel pain, the causes, risk factors, symptoms, and treatment may vary for these two. The location of the plantar fascia is mainly the part of the mistake, as a part of plantar fascia lies inside the heel with an overlap in the heel fat pad and plantar fascia. The other part runs from the bottom of the feet and forms an arch on the medial side. This arch is functional in the absorbance of dynamic shock withstanding support during movement.
Plantar fasciitis is a disorder that happens due to the prolonged degeneration in the plantar fascia, affecting the blood supply to the plantar fascia, and finally, the failure in self-repair and healing. This degeneration is attributed to the microtrauma occurring in the plantar fascia due to heavy workload, increased standing and running period, structural deformity in the muscle, bone, and joint. This prone the plantar fascia to chronic destruction.
The symptoms in the case of plantar fascia vary from heel pad syndrome. As in this case, the pain starts from the inner front portion of the heel extending towards the foot arch, causing swelling in this region. This pain is not as deep as in the fat pad syndrome but dull and throbbing. Plantar fasciitis sometimes feels tight and stretches, ensuring its occurrence in the feet. In addition, the most important sign of it is that sensation of pain generally happens during the first step after a long period of rest, such as the first step in the morning; the intensity of pain reduces after few steps but can return if a person continues to walk for a long period.
In the case of heel pad syndrome, the sensation of pain is deep and long-lasting. The pain is usually localized in the center of the heel and starts during walking, jumping, and prolonged standing. Moreover, the pain is in both the heels. While in plantar fasciitis, the pain might be present in one foot or both and commonly felt in the early morning coming out of the bed.
In some cases, the person might suffer from plantar fasciitis and heel pad syndrome, making the clinical diagnosis more challenging and complicated. Advanced diagnostic tools like Ultrasound and MRI are being used to ensure the underlying ailment with the best treatment accordingly to combat this challenge.
The final piece of advice to the patients:
In case of heel pain, promptly consult with your health care professional, take proper advice from him, and determine the possible risk factors and causes of your heel pain. The clinical diagnosis, treatment, and pain management on an earlier basis are signs of a good prognosis with less damage to the heel structure. Always ensure compatible footwear, supporting and padding to your heels and feet sole, and cushioning your feet during high-impact exercise and weight-bearing activities, lowering pressure on your heels and joints of lower limbs.
References:
https://www.aafp.org/afp/2011/1015/p909.html
https://lermagazine.com/article/management-of-painful-plantar-fat-pad-atrophy
https://www.sydneyheelpain.com.au/heel-pad-pain/
https://footeducation.com/overload-heel-pain-syndrome/
https://www.physio-pedia.com/Heel_Fat_Pad_Syndrome
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3309235/
https://www.mayoclinic.org/diseases-conditions/plantar-fasciitis/symptoms-causes/syc-20354846