Ball of the Foot Pain
Second Metatarsal Overload Syndrome [Causes & Best Home Treatment]
Second Metatarsal Overload Syndrome results from excess stress placed onto the 2nd metatarsal. STOP crossover toes and bunion pain, FIX IT 100%!
Look:
- 2nd toe joint pain and metatarsal overload syndrome can be improved with a few simple treatment changes.
- We are foot doctors & we see this problem get better almost every day.
- The goal is to solve this problem without medication or surgery if at all possible.
So, let’s GO!
Ball of the Foot Pain Pictures & Photo Gallery:
Look:
- Metatarsalgia: which means generalized foot pain without a specific cause.
- Second toe capsulitis: this is the inflammation of the second toe joint capsule.
- Capsulitis is related to hammertoe formation, and can lead to a plantar plate tear. There is some overlap between these three disorders. As they get worse tearing and ligament damage can occur.
- Morton’s neuroma: this is the damage and inflammation to the nerves between and underneath the metatarsal joints.
- Fat pad atrophy of the ball of the foot: this is the loss of cushioning in the ball the foot.
- Plantar Plate Tear: A plantar plate tear is ripping of the ligaments holding the toe together.
So, click on the photo gallery to see the specific causes of your ball of the foot pain!
Causes:
- The cause of second metatarsal overload syndrome is simply that too much pressure is placed on the 2nd metatarsal.
- This can be for any of the following reasons, but it always comes down to one longer than the other. Eventually a callus will form under the 2nd metatarsal head.
- There will also be constant pain while standing on the ball of the foot.

Activities that aggravate 2nd metatarsal overload syndrome:
- The pain is typically aggravated while walking running.
- Athletes who participate in high impact running in sports, generally develop an inflammatory condition which causes irritation to the second third, fourth or fifth metatarsals.
- This is also referred to as a medic her cell just in some cases.
- The pain gradually appears over a period of several weeks or months, it does not happen with one bad fall or crack of the bone.
- This can frequently be associated with conditions such as Morton’s neuroma, capsulitis, or stress fractures.
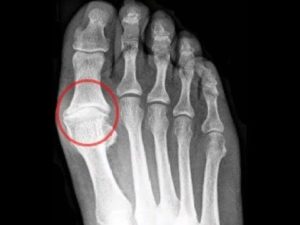
Specific Causes:
- Short 1st metatarsal – Morton’s Toe.
- Long 2nd metatarsal.
- Hypermobility of the 1st metatarsal.
- Prior broken foot.
- Tight calf muscles.
- Excessive wearing of heeled shoes.
- Bunion – that does not make proper contact with the ground for push-off.
- Flat foot due to another reason.
Symptoms:
- Sharp, aching or burning pain.
- Pain concentrated around the base of the 2nd toe.
- Pain that gets worse when you stand, walk or run.
- Pain that gets better when you are resting.
- Numbness in your toes.
- Pain that worsens when you bend your 2nd toe up and down to the extremes.
- Increased pain walking barefoot, especially on a hard floor.
This is most common in people who have very tight hamstrings calf muscles are putting much more pressure on the ball the foot. This can lead to neuroma, metatarsal or even stress fracture pain.
Diagnosis:
When to seek treatment:
- Not all 2nd toe pain requires seeing a doctor for treatment, especially if you’ve had a long day on your feet.
- It might be a good idea to try home treatment for a few days.
- If the pain does continue for an extended period of time and home treatment has not been effective, then it might be time to go seek professional care from your podiatrist.
Podiatrist In Office Evaluation:
- The first and most basic step is to get an x-ray. This only takes a few minutes and gives very valuable information.
- The first thing we are looking for is how long the metatarsal is, do you have a bunion, is there a broken bone, or is there any obvious deformities.
- It is almost impossible to tell if you have Morton’s neuroma based on an x-ray, this is based on clinical exam.
- Sometimes we may try to order an MRI, but most insurance plans these days don’t cover this right off the bat. As a result we can take an in office ultrasound to make sure that this is what’s going on.
- Through a physical exam, we will make sure that you do not have an aroma between your toes. We will make sure that none of the toes are dislocated or have a plantar plate rupture. We’ll make sure that you don’t have capsulitis at the site.
- By pressing with our fingertips along the metatarsal shaft, this would lead us to confirm that what you do have is a stress fracture through the site.
Our basic treatment algorithm includes:
- A foot x-ray as the first step.
- A full ultrasound in the office as the second step.
- An ultrasound as a backup, but insurance can sometimes be difficult in approving these at the beginning.
- Very rarely do we need to get a CT scan or a bone scan, especially for younger athletes, this can lead to a higher amount of radiation.
Metatarsalgia & Ball of the Foot Pain Treatment:
This long, long …. long in depth treatment guide will hopefully entertain you and show you everything you want to know about metatarsal joint pain!

Second Metatarsal Overload Syndrome Treatment:
What kind of rehabilitation can I do?:
- The most important thing you could do is switch up to different forms of exercises.
- What we usually prefer is stop running, and switch to cycling and swimming if at all possible.
- You can still do upper body exercises weightlifting rolling. You can do many things that raise your heart rate without damaging your foot further.
- The key is to accept that you have done some damage, and you must let it heal rather than getting worse.
What kind of stretching can I do?
- The most common reason people get pressure on the front of their foot is very tight Achilles tendons and hamstrings.
- Focus on stretching your calf muscles and hamstrings.
- If these are starting to loosen up, you can even start looking at your lower back and stretching this.
What are the best stretching devices to help me get more flexible?
- Second Metatarsal Overload Syndrome Treatment should be treated by identifying the cause.
- If you have a bunion for example: correct the flat foot causing the bunion and the bunion itself.
- If you wear heels: get a good running shoe with inserts.
- If you have tight calf muscles: perform continuous calf stretches.
How long does it take to heal from second metatarsal overload syndrome?:
- Doing all the right things, such as where good supportive orthotics, great shoes, resting the foot, and stretching your calf muscles and hamstrings: they can still take 6 to 8 weeks to fully heal this.
- Some people get better quicker, but you need to keep doing these things for many many weeks.
- The biggest mistake people do is think that they can do the right stuff for one to two weeks, no! It has to be longer, you have to treat this almost like a broken bone.
- The biggest key to this is to accept that you have an injury, and you must do all the right stuff to give it time to heal. Have confidence that this is your diagnosis and let it heal up. Don’t turn what should be a 1 to 2 month injury into a 2 to 3 year injury or longer!
For more on 2nd metatarsal overload syndrome: 2nd metatarsal overload procedures.
Ball of the Foot Pain Treatment Infographic

Ball of the Foot Home Treatment:
- Consider taping, orthotics, and great shoes as a combination to fix your foot problem.
- Products are not always necessary to fix your problem.
- The key is correcting the biomechanical problems that are leading to forefoot overload.
- Foot overload means too much pressure in the ball of the foot.
- Generally, something called ankle joint equinus can lead to too much pressure in the ball of your foot. This means your ankle is not flexible enough to move up and down.
- Ball of the foot pain treatment consists of two phases, first is control inflammation, next is to control bio-mechanics.
Remove Control Inflammation:
Massage & Ice Products:
- The metal ball is one of my personal favorites.
- This works great for your arch, less for the ball of the foot.
- These can help relax the arch or heel ligaments, leading to less pressure in the ball of the foot.
- Pills, creams, and ice will never completely fix your problem alone. What they will do is reduce the pressure on the area.






Menthol Based Gels:
- Biofreeze is one of our favorites.
- These gels have been studied to work 2x as long as ice.
- This works great for the ball of the foot.
- Consider using these as options when resting on the couch or going to sleep at night.








Massage Sticks:
- These can work great for loosening your muscles.
- This is means for your hamstring and calf muscles. This can loosen the ankle tightness, putting pressure on the ball of your foot.
- This allows less tightness and pressure on the ball of your foot.






Ball of the Foot Stress Relief.
- The key is to prevent future pain.
- If you can get rid of the pain and swelling, this will let you start walking normally.
- If you can walk normally, the vast majority of your pain should gradually start to go away.
- This means proper cushion, proper stability, and pressure relief from the front of your foot.
- This will relieve pressure from your big toe, your 2nd toe, your Morton’s neuroma, your plantar plate, hammertoes and joint capsules.
Best Metatarsalgia Shoes:
- Getting a great supportive pair of shoes will make sure that there is pressure removed from the ball of your foot.
- This is especially important if you have metatarsalgia, Morton’s neuroma, 2nd metatarsal overload syndrome, and capsulitis!
- Consider shoes combined with a good supportive orthotic for the best pain relief!
- The following link will show you what our favorites are.
Best Ball of the Foot Insoles:
- These are our recommended orthotics & insoles.
- There are different types of different shoes.
- Women’s shoes usually need a less bulky orthotic but allow for less correction.
- A full-length orthotic requires a running shoe, boot, or comfortable walking/dress shoe.
Best Full-Length Orthotics:
- Full-length orthotics are the most recommended type for the ball of the foot pain.
- Be aware that if they are too uncomfortable, it might be worth starting with a less corrective pair.
- Eventually, you can then work your way up to these.








Best Dress Shoe Orthotics:
- These are a stronger option for shoes with tight dress shoes.
- Just be aware that less corrective orthotics & tight shoes are usually not a good combination.






Best 3/4 Length Orthotics:
- These may be a good option for the ball of the foot if the full-length orthotics are too tight or too uncomfortable.


Get A Great Dynamic Stretch:
- It is possible to stretch on your own, but these products can also really help!
- Personally, I have the stationary block set up in my kitchen to stretch every day multiple times while getting my coffee!
- This will take pressure off of the ball of your foot.








Ball of the Foot Pain

