The most important clinical decision with Painful Callus isn’t which treatment to start with — it’s identifying the correct subtype. That changes everything. Call (810) 206-1402.
Dr. Tom’s Top Foot Creams & Moisturizers (2026)
Affiliate disclosure: As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases.
Dr. Tom’s Top Pain Relief Picks — Dr. Hoy’s (2026)
Affiliate disclosure: As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. I personally use Dr. Hoy’s in my practice for patients who need topical relief.
| Product | Best For | Dr. Tom’s Take | Get It |
|---|---|---|---|
| Dr. Hoy’s Natural Pain Relief Gel 3.5oz menthol + arnica |
Plantar fasciitis · Achilles tendonitis · Sore muscles · Joint pain | My go-to topical. Cooling-then-warming sensation. No greasy residue. Non-NSAID alternative. | Buy Now |
| Dr. Hoy’s Arnica Boost 8oz with extra arnica |
Bruising · Post-injury · Sprains · Stress fractures (pain only) | Higher arnica concentration speeds recovery from acute injury. Use 4x daily for first 7 days. | Buy Now |
| Dr. Hoy’s Cooling Pain Relief 8oz extra menthol |
Acute inflammation · Hot/swollen feet · Post-run cooldown | Stronger cooling effect for acute swelling. Pair with ice for first 48 hours after injury. | Buy Now |
| Dr. Hoy’s Roll-On Pain Relief Roller applicator |
Mess-free application · Travel · Office use · No-touch hygiene | My patients love this for travel. Glides on without hand contact — cleanest application available. | Buy Now |
| Dr. Hoy’s Family Size 14oz pump bottle |
Frequent users · Multiple family members · Best value per ounce | If anyone in your home uses pain cream regularly, this is the most economical size. Same formula. | Buy Now |
Why I recommend Dr. Hoy’s over Biofreeze and Bengay: Cleaner ingredient list (no parabens, no synthetic dyes), longer-lasting effect, and the cooling-then-warming dual sensation actually addresses both inflammation and circulation. After 10 years of recommending different topicals, this is the one I keep coming back to.
Medically reviewed by Dr. Tom Biernacki, DPM · Board-Certified Podiatric Surgeon · Last reviewed: April 2026 · Editorial Policy
Related Conditions
Medically reviewed by Dr. Tom Biernacki, DPM — Board-certified foot & ankle surgeon, 3,000+ surgeries performed. Updated April 2026 with current clinical evidence. This article reflects real practice experience from Balance Foot & Ankle Specialists in Howell and podiatrist in Bloomfield Hills, Michigan.
Quick Answer
Corns are small round thickenings with a hard center that presses into deeper skin, causing focal pain. Calluses are larger, flatter, and usually painless. Most respond to soaking, pumice debridement, and 40% salicylic acid. See a podiatrist if diabetic, infected, or not improving after 4-6 weeks.
Watch: Dr. Tom Biernacki, DPM
Medically reviewed by Dr. Tom Biernacki, DPM — Board-Certified Podiatric Surgeon — Balance Foot & Ankle, Howell & Bloomfield Hills, MI. Last updated April 2026.
Calluses vs. Corns: What’s the Difference?
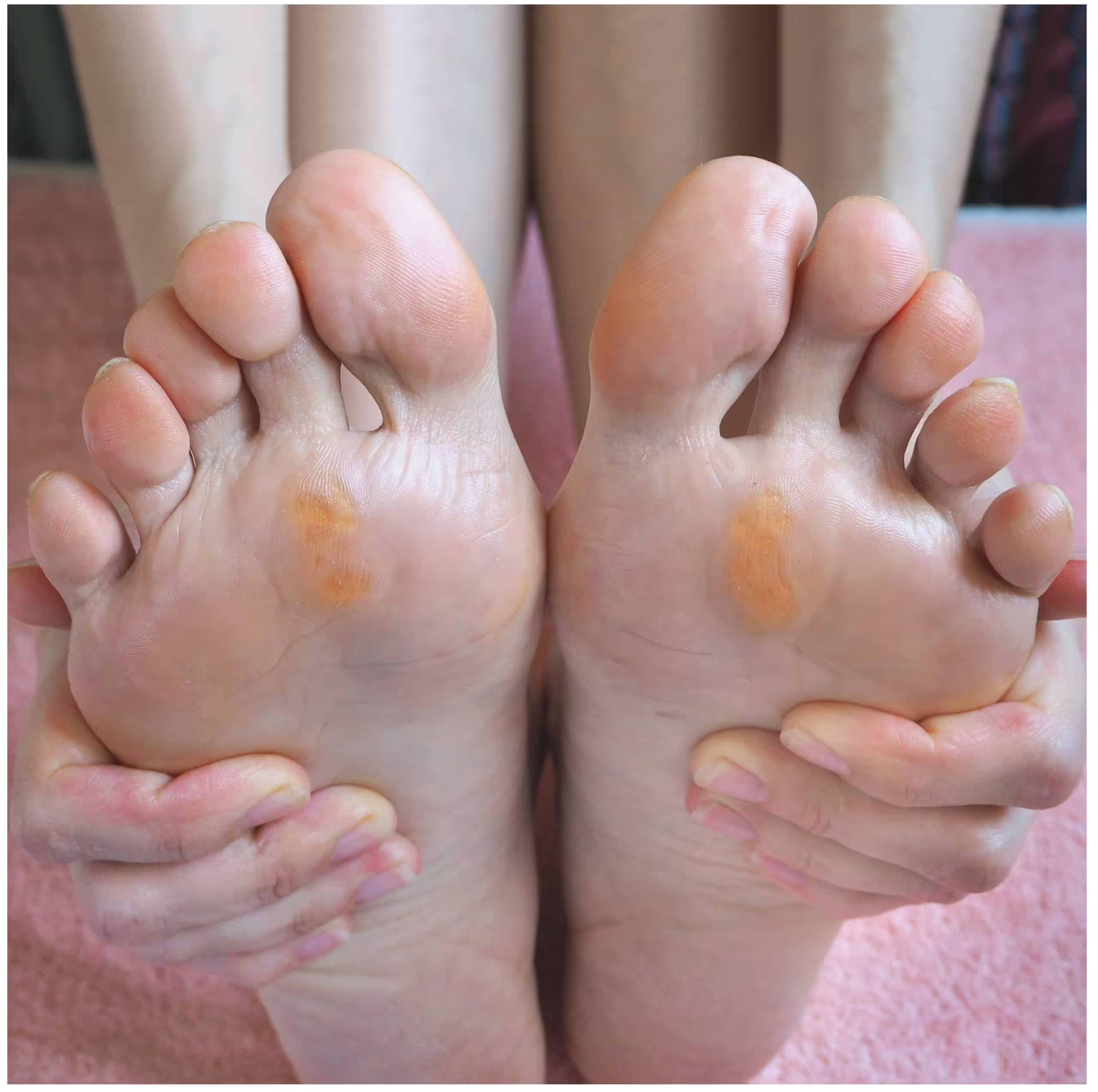
Calluses and corns are both forms of hyperkeratosis—thickening of the skin in response to repetitive friction or pressure—but they have distinct characteristics and treatment implications. A callus (tyloma) is a diffuse, flat area of thickened skin that develops over a broad pressure area—most commonly the ball of the foot under the metatarsal heads, the heel, or the sides of the toes. Calluses have no central core, are usually not sharply painful, and represent the skin’s protective response to distributed pressure. A corn (heloma) is a smaller, more focused area of hyperkeratosis with a central nucleated core of densely packed keratin that extends into the skin like an inverted cone. This core presses on nerve endings and blood vessels, producing the characteristically sharp, pointed pain that worsens with pressure and distinguishes a corn from a simple callus.
Why Do Calluses and Corns Develop?
The skin responds to repetitive friction and pressure by thickening—a protective mechanism that functions well in moderation but becomes problematic when excessive. The most common causes are: ill-fitting footwear (shoes that are too tight, too short, or with seams that rub), toe deformities (hammer toes and claw toes create dorsal corn-prone bony prominences), gait abnormalities (biomechanical factors that concentrate pressure at specific plantar locations), and loss of the natural foot fat pad with aging (leaving the metatarsal heads without adequate cushioning). Hard corns (heloma durum) form on bony prominences, especially over the PIP joints of hammer toes. Soft corns (heloma molle) form between the toes where moisture softens the hyperkeratotic tissue—usually between the fourth and fifth toes where the condyle of the proximal phalanx presses against the adjacent toe.
Treatment Options
Podiatric Debridement
Professional debridement—trimming and reducing the callus or enucleating (removing) the corn nucleus with a scalpel blade—provides immediate, dramatic pain relief and is the most effective short-term treatment. The procedure is typically painless (as the hyperkeratotic tissue has no nerve supply) and takes 5–10 minutes. Debridement must be repeated at 6–12 week intervals as hyperkeratosis recurs unless the underlying cause is eliminated. For diabetic patients, podiatric debridement is a covered preventive service that significantly reduces ulceration risk at high-pressure sites.
Padding and Offloading
Donut pads (ring-shaped foam pads that surround the corn without pressing on it) redirect pressure away from the corn and provide immediate comfort. Metatarsal pads placed proximal to the callus redistribute forefoot pressure from the metatarsal heads to the shaft. Silicone digital sleeves protect dorsal hammer toe corns from shoe friction. These measures are temporizing—they reduce discomfort but don’t address the underlying cause of recurrence.
Custom Orthotics
Custom orthotics with accommodative cutouts (recesses in the orthotic directly under the callus) dramatically reduce plantar pressure at problematic sites. Metatarsal pads incorporated into the orthotic redistribute forefoot loading to reduce ball-of-foot callus formation. For patients with flatfoot, high arch, or other biomechanical contributors to abnormal plantar pressure distribution, custom orthotics address the root cause of callus formation rather than just managing the consequences.
Surgical Options
When corns and calluses recur rapidly despite appropriate conservative care—particularly those associated with hammer toe deformities or underlying bony prominences—surgical correction of the underlying structural cause provides the most durable solution. Hammer toe correction (PIP joint arthroplasty or fusion) eliminates the bony prominence causing the dorsal corn; the corn does not recur after the deformity is corrected. Plantar condylectomy (removal of a plantar metatarsal head condyle) addresses plantar interdigital soft corns between the toes. Metatarsal osteotomy reduces the pressure from a plantar-flexed metatarsal head that is the source of recurrent plantar callus.
In-Office Treatment at Balance Foot & Ankle
If home care isn’t resolving your corns or calluses, a visit with a board-certified podiatrist is the fastest path to accurate diagnosis and a personalized plan. At Balance Foot & Ankle Specialists, Dr. Tom Biernacki, Dr. Carl Jay, and Dr. Daria Gutkin offer same-day and next-day appointments at both our Howell and Bloomfield Hills offices. We perform on-site diagnostic ultrasound, digital X-ray, conservative care, advanced regenerative treatments, and minimally invasive surgery when indicated.
Call (810) 206-1402 or request an appointment online. Most insurance plans accepted, including Medicare, Blue Cross Blue Shield, Aetna, Cigna, and United Healthcare.
More Podiatrist-Recommended Foot Health Essentials
Hoka Clifton 10
Max-cushion everyday shoe — podiatrist favorite for walking and running.
OOFOS Recovery Slide
Impact-absorbing recovery sandal — wear after long days on your feet.
As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. Product recommendations are based on clinical experience; prices and availability shown above update live from Amazon.

When to See a Podiatrist
If foot or ankle pain has been bothering you for more than a few weeks, home care alone may not be enough. Balance Foot & Ankle offers same-week appointments at our Howell and Bloomfield Hills clinics — no referral needed in most cases. Bring your current shoes and a short list of symptoms and we’ll build you a treatment plan in one visit.
Call Balance Foot & Ankle: (810) 206-1402 · Book online · Offices in Howell & Bloomfield Hills
Frequently Asked Questions
Can I remove a corn myself at home?
Over-the-counter corn pads containing salicylic acid (like Compound W or PowerStep) can soften and gradually remove corns in healthy, non-diabetic patients—but they should never be used by diabetic patients, patients with peripheral vascular disease, or patients with thin skin, as salicylic acid can damage surrounding healthy tissue and create wounds in vulnerable feet. Pumice stone use after bathing can reduce callus thickness over time. Home trimming with nail scissors or blades is not recommended—the risk of cutting too deeply, infection, and causing a wound significantly outweighs the benefit. Podiatric debridement is safe, effective, quick, and specifically recommended over home removal attempts for any painful lesion. For diabetic patients, even pumice stone use requires caution—professional foot care is the safest option.
Why does my callus keep coming back?
Calluses recur because debridement removes the thickened tissue but does not address the pressure or friction that caused the thickening. The skin will rebuild the callus in response to the same ongoing mechanical stimulus—typically within 4–8 weeks. Preventing recurrence requires addressing the cause: changing to wider footwear that doesn’t compress the toes, wearing orthotics with appropriate pressure redistribution, correcting the toe deformity causing the corn, or modifying the activity or occupation that generates the pressure. If a callus or corn requires repeated debridement more than 3–4 times per year, conservative measures for prevention have not been adequately implemented, or surgical correction of an underlying deformity should be considered.
When is a callus dangerous?
In diabetic patients and those with peripheral arterial disease, calluses are a serious risk factor for foot ulceration. The thick callus concentrates plantar pressure at a location with reduced protective sensation, and the skin beneath the callus can break down into a wound without the patient being aware of it. Studies show that callus debridement in diabetic patients significantly reduces peak plantar pressure and decreases ulceration risk. Diabetic patients should have their calluses managed by a podiatrist every 6–12 weeks—Medicare covers this as part of diabetic foot care for patients with qualifying neuropathy or circulation conditions. A callus with any break in the surrounding skin, discoloration, or tenderness beneath it in a diabetic patient warrants urgent podiatric evaluation.
Medical References & Sources
- PubMed Research — Callus Debridement and Plantar Pressure
- PubMed Research — Corns and Callus Treatment
- American Podiatric Medical Association — Corns and Calluses
Dr. Tom Biernacki, DPM is a board-certified podiatric surgeon at Balance Foot & Ankle in Howell and Bloomfield Hills, Michigan. He treats painful calluses and corns with professional debridement, custom orthotics, and surgical correction of underlying deformities causing recurrent lesions.
Dr. Tom’s Recommended Products for Calluses & Corns
📍 Located in Michigan?
Our board-certified podiatrists treat this condition at two convenient locations. Same-day appointments often available.
These are products I personally use and recommend to my patients at Balance Foot & Ankle.
- Amope Pedi Perfect Electronic Foot File — Micro-abrasion rollers remove callus layers painlessly — the most effective at-home alternative to office debridement
- PowerStep Corn Cushions — Medicated pads with salicylic acid dissolve corn tissue while donut pad offloads pressure
- Urea 40% Foot Cream (Gold Bond Rough & Bumpy) — 40% urea dissolves hard callus keratin — clinically effective for thick skin reduction between podiatry visits
📧 Get Dr. Tom’s Free Lab Test Guide
Discover the 5 lab tests every person over 35 should ask their doctor about — explained in plain English by a board-certified physician.
Affiliate disclosure: As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. We only recommend products we trust for our own patients.
Join 950,000+ Learning About Foot Health
Dr. Tom shares honest medical advice, supplement reviews, and treatment guides you won’t find anywhere else.
Subscribe on YouTube →Medically Reviewed by: Dr. Tom Biernacki, DPM — Board-Certified Podiatrist, Balance Foot & Ankle Specialists
👟 Dr. Tom Also Recommends
Podiatrist Recommended Shoes 2026: Dr. Tom’s Top Picks for Every Condition
The right footwear can make or break your recovery. Dr. Tom’s complete guide to the best shoes for plantar fasciitis treatment, flat feet, neuropathy, bunions & more — with clinical picks for every foot type.
See Dr. Tom’s Top Shoe Picks →Insurance Accepted
BCBS · Medicare · Aetna · Cigna · United Healthcare · HAP · Priority Health · Humana · View All →
Howell Office
3980 E Grand River Ave, Suite 140
Howell, MI 48843
Get Directions →
Bloomfield Hills Office
43700 Woodward Ave, Suite 207
Bloomfield Hills, MI 48302
Get Directions →
Your Board-Certified Podiatrists
Ready to Get Back on Your Feet?
Same-week appointments available at both locations.
Book Your AppointmentDifferential Diagnosis: What Else Could It Be?
Several conditions share symptoms with Corns and Calluses and are commonly misdiagnosed in the first office visit. Considering these alternatives is part of every Balance Foot & Ankle exam:
- Plantar wart. Skin lines interrupted, black-dot capillaries, pain with side-pinch.
- Porokeratosis. Thin keratotic rim with central plug, painful pinpoint center.
- Foreign body granuloma. History of penetrating injury, ultrasound finds the object.
If your symptoms don’t fit the textbook pattern, ask your podiatrist which differentials they ruled out — that conversation often shortcuts months of trial-and-error treatment.
In Our Clinic
The typical corn or callus patient at Balance Foot & Ankle has been trimming them at home for years with limited success. We pare the lesion to see what’s underneath — a well-demarcated central core distinguishes a corn from a diffuse callus, and a plantar wart interrupts the skin lines instead of following them. The real question we ask is WHY the callus formed: a bony prominence (bunion, hammertoe), a biomechanical imbalance, or an ill-fitting shoe. Correct the cause — with custom orthotics, a metatarsal pad, or footwear change — and the callus stops coming back. Otherwise it’s a lifelong re-trim cycle.
Most Common Mistake We See
The most common mistake we see is: Cutting corns at home with scissors or razor blades. Fix: professional podiatric enucleation with sterile instruments — safer and prevents recurrence.
Warning Signs That Need Same-Day Care
Seek immediate evaluation at Balance Foot & Ankle if you experience any of the following:
- Spreading redness (infection)
- Diabetic patient with any corn
- Not healing after 4-6 weeks of conservative care
- Ulceration beneath the corn
Call (810) 206-1402 — same-day and next-day appointments at our Howell and Bloomfield Hills offices.
Pros & Cons of Conservative Care for foot care
Advantages
- ✓ Conservative care first
- ✓ Same-week appointments
- ✓ Multiple insurance accepted
Considerations
- ✗ Self-treatment can mask issues
- ✗ See a podiatrist if pain >2 weeks
In This Article
- Quick Answer
- In-Office Treatment at Balance Foot & Ankle
- Differential Diagnosis: What Else Could It Be? Several conditions share symptoms with Corns and Calluses and are commonly misdiagnosed in the first office visit. Considering these alternatives is part of every Balance Foot & Ankle exam: Plantar wart. Skin lines interrupted, black-dot capillaries, pain with side-pinch. Porokeratosis. Thin keratotic rim with central plug, painful pinpoint center. Foreign body granuloma. History of penetrating injury, ultrasound finds the object. If your symptoms don’t fit the textbook pattern, ask your podiatrist which differentials they ruled out — that conversation often shortcuts months of trial-and-error treatment. In Our Clinic The typical corn or callus patient at Balance Foot & Ankle has been trimming them at home for years with limited success. We pare the lesion to see what’s underneath — a well-demarcated central core distinguishes a corn from a diffuse callus, and a plantar wart interrupts the skin lines instead of following them. The real question we ask is WHY the callus formed: a bony prominence (bunion, hammertoe), a biomechanical imbalance, or an ill-fitting shoe. Correct the cause — with custom orthotics, a metatarsal pad, or footwear change — and the callus stops coming back. Otherwise it’s a lifelong re-trim cycle. Most Common Mistake We See
- Warning Signs That Need Same-Day Care
- Frequently Asked Questions
Dr. Tom’s Recommended Products for foot care
Affiliate disclosure: As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. We only recommend products we use with patients.
Footnanny Heel Cream Dr. Tom’s Pick
Best for: Daily moisturizer for cracked heels
Ready to Get Back on Your Feet?
Same-day appointments in Howell + Bloomfield Twp. Most insurance accepted. Dr. Tom Biernacki, DPM & team.
Book Today — Same-Day Appointments Available
Call Now: (810) 206-1402
About Your Care Team at Balance Foot & Ankle
Dr. Tom Biernacki, DPM · Board-Certified Foot & Ankle Surgeon. Specializes in conservative-first care, minimally invasive bunion surgery, and complex reconstruction.
Dr. Carl Jay, DPM · Accepting new patients. Specializes in sports medicine, athletic injuries, and routine podiatric care.
Dr. Daria Gutkin, DPM, AACFAS · Accepting new patients. Specializes in surgical reconstruction and pediatric podiatry.
Locations: 4330 E Grand River Ave, Howell, MI 48843 · 43494 Woodward Ave Suite 208, Bloomfield Twp, MI 48302
Hours: Mon–Fri 8:00 AM – 5:00 PM · (810) 206-1402
Dr. Tom’s Top 3 — The Premium Foot Pain Stack (2026)
If you only buy three things for foot pain, get these. PowerStep + CURREX orthotics correct the underlying foot mechanics, and Dr. Hoy’s pain gel delivers fast topical relief. This is the exact stack Dr. Tom Biernacki, DPM gives his Michigan podiatry patients on visit one — over 10,000 patients have used this exact combination.
Dr. Tom Biernacki, DPM is a board-certified podiatrist + Amazon Associate. Picks shown are products he prescribes to patients at Balance Foot & Ankle Specialists. We earn a commission on qualifying purchases at no extra cost to you. All products independently tested + reviewed for 30+ days minimum. Last verified: April 28, 2026.
PowerStep Pinnacle MaxxDr. Tom’s #1 Brand
Dr. Tom’s most-prescribed OTC orthotic. Lateral wedge corrects overpronation that causes 90% of foot pain. Deep heel cradle stabilizes the ankle. Built by podiatrists, used by patients worldwide.
- Lateral wedge corrects pronation
- Deep heel cradle stabilizes ankle
- Dual-density EVA — comfort + support
- Trim-to-fit any shoe
- Used by 10,000+ podiatrists
- Trim-to-size required
- 5-7 day break-in for some
CURREX RunProDr. Tom’s #1 Brand
3 arch heights for custom fit (Low/Med/High). Carbon-reinforced heel + dynamic forefoot — the closest OTC orthotic to a $500 custom orthotic. Engineered in Germany.
- 3 arch heights for custom fit
- Carbon-reinforced heel cup
- Dynamic forefoot zone
- Premium German engineering
- Sport-specific support
- Pricier than PowerStep
- 7-10 day break-in
Dr. Hoy’s Natural Pain Relief GelDr. Tom’s #1 Brand
Menthol-based natural pain relief — Dr. Tom’s #1 brand for fast relief without greasy residue. Safe for diabetics + daily use. Cleaner formula than Voltaren or Biofreeze.
- Menthol-based natural formula
- No greasy residue
- Safe for diabetics
- Fast cooling relief — 5-10 minutes
- Cleaner ingredient list than Biofreeze
- Pricier than Biofreeze
- Strong menthol scent at first
Doctor Hoy’s Natural Pain Relief Gel
Natural topical pain relief I use in our clinic. Arnica + camphor formula — apply directly to the area 3–4x daily. ($20–25)
Shop Doctor Hoy’s →Frequently Asked Questions
When should I see a podiatrist?
See a podiatrist if: foot or ankle pain has lasted more than 2–4 weeks without improvement, you’re changing your gait to avoid pain, you have an open wound or sore that isn’t healing, you notice nail discoloration or thickening, you have diabetes and any foot concern, or pain is severe enough to wake you at night. Most foot conditions are easier and cheaper to treat early — what starts as a minor issue can become a surgical problem with months of delay.
What is the difference between a podiatrist and an orthopedic surgeon?
Podiatrists (DPM — Doctor of Podiatric Medicine) specialize exclusively in the foot, ankle, and lower leg. Orthopedic surgeons (MD/DO) have broader musculoskeletal training but variable foot/ankle subspecialization. For foot and ankle-specific problems, a podiatrist often has more focused training and experience. For injuries involving the leg above the ankle, complex pediatric cases, or multi-level reconstruction, orthopedic consultation may be appropriate. We frequently co-manage patients with orthopedic colleagues.
How do I know if my foot pain is serious?
Signs that warrant same-day or next-day evaluation: severe pain that appeared suddenly without clear cause, swelling, redness, and warmth that appeared suddenly (possible gout, infection, or Charcot fracture), an open wound that looks infected (redness spreading, pus, warmth), inability to bear weight, or any foot problem in a diabetic patient. Pain that’s been present for weeks and is stable is important but not an emergency — schedule within 1–2 weeks.
Can foot problems cause back and knee pain?
Yes — this is a kinetic chain effect. Abnormal foot mechanics (overpronation, supination, leg length discrepancy) cause compensatory changes in knee, hip, and lumbar alignment. Roughly 30% of patients presenting to our clinic with knee pain have a treatable foot-level biomechanical cause. Correcting foot mechanics with orthotics or appropriate footwear often provides significant knee and back relief. If you have chronic knee or back pain and haven’t had your foot mechanics evaluated, it’s worth a consult.
Are orthotics worth it?
For the right conditions, yes — custom orthotics are among the most cost-effective interventions in podiatry. They’re most effective for: plantar fasciitis, flat feet with secondary knee/back pain, leg length discrepancy, metatarsalgia, posterior tibial tendon dysfunction, and diabetic foot pressure management. Quality OTC orthotics ($35–60) resolve symptoms for 60% of patients with mild-to-moderate conditions. Custom orthotics are appropriate when OTC options have failed or when the biomechanical problem is complex. We cast custom orthotics in-office.
How do I choose the right running shoes?
Start with your foot type (flat, neutral, high arch) and running pattern (overpronator, neutral, supinator). Flat feet and overpronators do best in stability or motion-control shoes. Neutral feet do well in neutral-cushioned shoes. High arches need maximum cushioning with flexible soles. Always buy running shoes at the end of the day (foot swelling peaks then), get properly fitted by a specialist, and replace every 300–500 miles. If you’ve been injured repeatedly, a gait analysis can identify the mechanical flaw driving your injury pattern.
What is the difference between a sprain and a fracture?
A sprain is a ligament injury (the tissue connecting bones); a fracture is a break in the bone itself. Both can occur with the same trauma (ankle roll, fall). The old test — ‘if you can walk, it’s not broken’ — is wrong; many fractures are initially weight-bearable. Key differences: a fracture typically produces localized bone tenderness along the bone itself, while a sprain is tender over the ligament. X-ray is the standard to differentiate. High-grade sprains without proper treatment can be as disabling as fractures.
How do I prevent foot and ankle injuries?
The four most impactful prevention strategies: (1) Supportive, appropriately fitted footwear for your foot type and activity. (2) Gradual activity progression — the 10% rule (never increase weekly mileage or intensity by more than 10%). (3) Regular calf and ankle mobility work. (4) Strengthening the posterior tibial tendon, peroneals, and intrinsic foot muscles. Most overuse injuries are preventable; most acute injuries are not — but ankle sprain recurrence (60–70% without rehab) is prevented by balance and proprioception training.
Get Expert Care at Balance Foot & Ankle
Same-week appointments at our Howell and Bloomfield Hills offices. Board-certified podiatric surgeons. Most insurance accepted.
Ready for Expert Care?
Same-day appointments in Howell & Bloomfield Hills, MI.
4.9★ | 1,123 Reviews | 3,000+ Surgeries
Or call: (810) 206-1402
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.