Ball of the Foot Pain
Metatarsophalangeal Joint Pain [Causes, Symptoms & Best Treatment]
Metatarsarsophalangeal joint pain is also know as ball of the foot pain or metatarsalgia. 95% of the time this can be improved by offloading pressure.
Look:
- Ball of the foot pain & big toe joint pain can be improved with a few simple treatment changes.
- We are foot doctors & we see this problem get better almost every day.
- The goal is to solve this problem without medication or surgery if at all possible.
So, let’s GO!
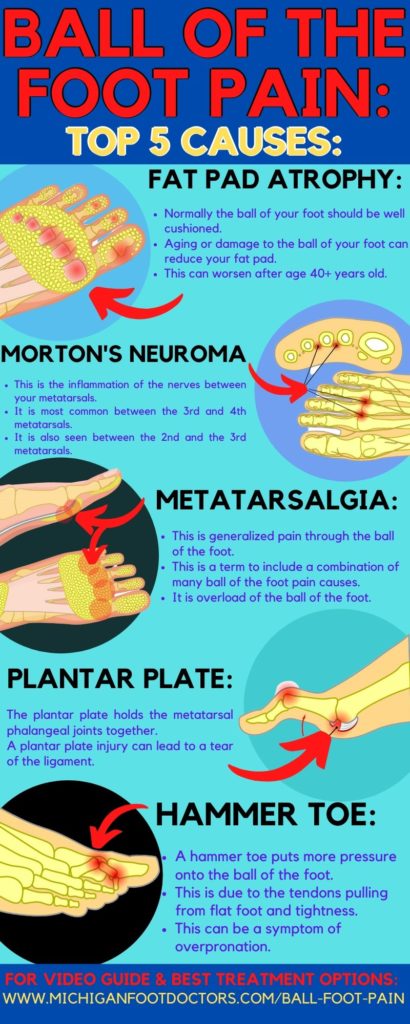
Table of Contents
Ball of the Foot Pain Pictures & Photo Gallery:
Look:
- Metatarsalgia: which means generalized foot pain without a specific cause.
- Second toe capsulitis: this is the inflammation of the second toe joint capsule.
- Capsulitis is related to hammertoe formation, and can lead to a plantar plate tear. There is some overlap between these three disorders. As they get worse tearing and ligament damage can occur.
- Morton’s neuroma: this is the damage and inflammation to the nerves between and underneath the metatarsal joints.
- Fat pad atrophy of the ball of the foot: this is the loss of cushioning in the ball the foot.
- Plantar Plate Tear: A plantar plate tear is ripping of the ligaments holding the toe together.
So, click on the photo gallery to see the specific causes of your ball of the foot pain!
Click on the photo gallery to see the specific causes of your ball of the foot pain!
Overview of Metatarsalgia & Ball of the Foot Pain:
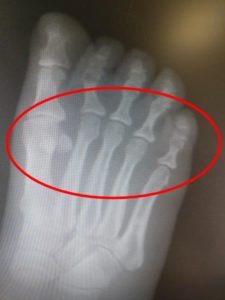
- Metatarsal joint pain usually occurs at the prominent part of the forefoot where the toes connect to the metatarsal bones.
- The most common site of metatarsal joint pain is the second metatarsal but it can spread over to the third, fourth and fifth toes as well.
- The most common causes of metatarsal joint pain are detailed below.
This is most common in people who have very tight hamstrings calf muscles are putting much more pressure on the ball the foot. This can lead to neuroma, metatarsal or even stress fracture pain.
Symptoms:
- Pain in the forefoot that is worse with weight bearing.
- Pain usually begins the longer you are on your feet vs some conditions that get better the more you walk.
- If you move the toe up and down to its extreme range of motion, it should usually hurt more.
- If you push on the foot from the bottom, see if a metatarsal is longer or somehow more prominent than the other metatarsal heads.
Risk Factors:
- A flat foot which spreads out the forefoot as well as putting more pressure on it
- Over pronation of the foot.
- A previously broken, bent or rigid big toe joint that then relies on the other four joints to carry a greater load.
- Tight footwear- make sure you use a brannock device to properly measure your shoe size.
- Capsulitis.
- Bursitis.
- Long 2nd toe.
- Short 1st toe.
- Previous fractures that may have healed improperly and lead to osteoarthritis.
- Morton’s neuroma or Morton’s Neuralgia.
Causes:
Metatarsalgia:
- Metatarsalgia is the generalized ball of the foot pain.
- This means that there is too much pressure on the front of your foot.
- The bones the tendons the nerves in the tissue surrounding the site could all get bruised up.
- This is one of the most common causes of ball of the foot pain that we see.
- Click on the link to see how to take care of this common problem!

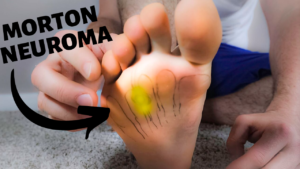
Morton’s neuroma:
- A Morton’s neuroma is the irritation of nerves in the ball of the foot.
- This can result in sharp, shooting and tingling pain.
- This is also a very common condition, it can feel as though if your foot is clicking and popping by the third and fourth toe.
- You can also feel like you have a bunched up sock and the ball of the foot.
Capsulitis:
- Capsulitis in the ball the foot is due to the ligaments and tendons getting irritated in the foot.
- This is very common around the second and the third toe joints.
- These are the longest metatarsal bones in your foot, and if there is tightness through the ankle and increase pressure on the foot, these tendons can very easily get agitated.
- Click on the above link to find out how to treat this very common condition.

Ball of the foot bruising:
- Ball of the foot pressure can frequently result in bruising.
- This can result in calluses corns and pressure buildup.
- This is a very common injury, click on the above link to see how to take care of this very important problem.

This is most common in people who have very tight hamstrings calf muscles are putting much more pressure on the ball the foot. This can lead to neuroma, metatarsal or even stress fracture pain.
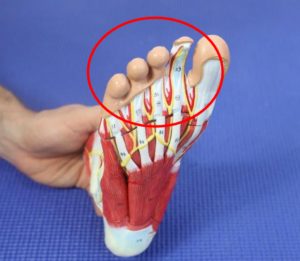
Plantar plate injury:
- The planter plate is a ligament that holds the metatarsal phalangeal joints together.
- This is a very important ligament as it has to support your body weight prevent your toes from coming apart.
- If this starts to tear, become inflamed or injured, it can cause you significant pain.
- This is a very common problem with solutions available.

Non-Surgical Best Treatment:
- Taping: Low Dye Taping is a taping technique that can recreate the foot arch and can be attempted to maintain supination rather than pronation.
- Splinting: An offloading pad can be made for your forefoot that has a second toe cutout that is amazing for relieving pain.
- Ice: This is not just about pain! It will decrease the inflammation and the time needed to heal the forefoot. Put ice in a bag (wrapped with cloth) and apply it for 15-20 minutes until the area starts to become numb. This decreases the effect of inflammatory cells and at the same time boosts the rebound blood flow to the area after the ice is removed.
- Elevation: Recline in a chair and elevate our foot while watching tv. Like the Ice principle, it flushes the inflammatory cells out of the area and is very important immediately after running or standing for a long time.
- Pain medication: Ibuprofen or other anti-inflammatories. The goal is to continue it regularly for 1-2 weeks not for pain but to raise anti-inflammation enzyme levels in your blood so that the area has a chance to heal. This is not just for pain!
- Tight Calf Muscles – Stretching your calves is essential and the cheapest possible cure. This may be the single most important component of reducing pain due to overpronation!
- Use a Brannock device to properly measure your shoe size: It is essential to measure the foot length, the arch length and the foot width. It is possible that you have longer toes or longer metarsals that require a wider Toe box than you think you need.
- Combine icing, elevation, non-weight bearing and pain medication gives you the best chance at healing as quickly as possible.
- Corticosteroid injection at the podiatrist office is highly recommended as it is shown to slightly decrease pain, but greatly increase motion and time of recovery.
What can a podiatrist do for Metatarsophalangeal Joint Pain?
- X-rays, MRI’s or Ultrasound scans can be used to look inside the foot to view any damage.
- Blood tests may be taken to diagnose any underlying medical causes such as diabetes or gout.
- A podiatrist may assess your foot position and gait (walking pattern).
- If necessary custom orthotics (insoles) can be made.
- A doctor may inject a corticosteroid injection into the foot.
For more on Metatarsophalangeal Joint Pain.
Ball of the Foot Pain Treatment Infographic:
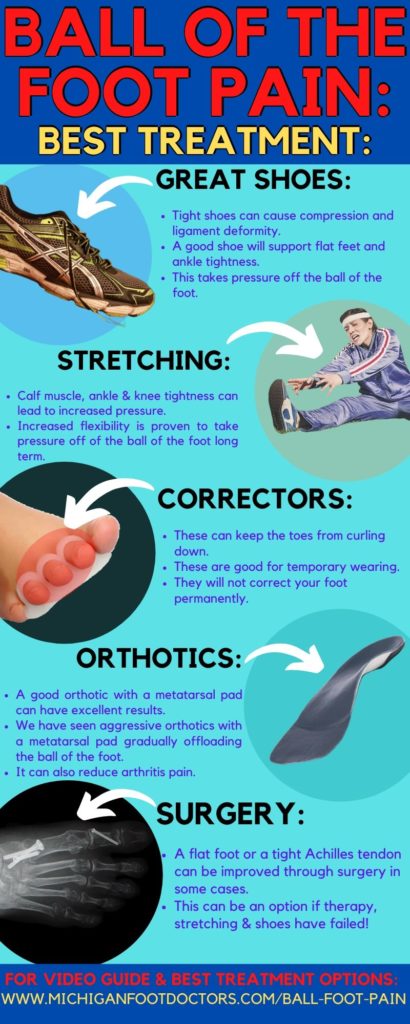
Ball of the Foot Home Treatment:
- Consider taping, orthotics, and great shoes as a combination to fix your foot problem.
- Products are not always necessary to fix your problem.
- The key is correcting the biomechanical problems that are leading to forefoot overload.
- Foot overload means too much pressure in the ball of the foot.
- Generally, something called ankle joint equinus can lead to too much pressure in the ball of your foot. This means your ankle is not flexible enough to move up and down.
- Ball of the foot pain treatment consists of two phases, first is control inflammation, next is to control bio-mechanics.
Remove Control Inflammation:
Massage & Ice Products:
- The metal ball is one of my personal favorites.
- This works great for your arch, less for the ball of the foot.
- These can help relax the arch or heel ligaments, leading to less pressure in the ball of the foot.
- Pills, creams, and ice will never completely fix your problem alone. What they will do is reduce the pressure on the area.
Best Foot & Ankle Manual Massage Devices:
Best Premium Massage Roller
Most Cost Effective Massage Roller.
Cost Effective Freezable Massage Roller.



Price:
Price not available
$8.99
$11.99
Overview:
Premium freezable metal ball that stays cold for up to 6 hours. Great for plantar fascia, neck, shoulders and calf muscles.
Amazing Price, Great Reviews – Non-Freezable Massage Rolling Stick
Great price and it is freezable. Budget friendly freezable massage roller.
Pros:
Great reviews – near 5 star. Stays cold for a long time with deep penetrating plantar fascia massage. Used by professional athletes. Stays cold for HOURS!
Great for what it does. You roll it back and forth along your plantar fascia massaging the swelling and irritation out. Decreases pain. Thousands of 5 star reviews on Amazon.
Excellent reviews. It massages and ices, so it is a step up over the massage rollers. Near 5 star reviews with >500 reviews.
Cons:
More expensive than some of the other options, but near perfect reviews.
Is not freezable like the other two options. Massaging a sore muscle without the cold sensation can be very painful and render it useless to you if really sore.
It does a great job doing what it is supposed to do. Main downside is that it does not stay cold as long as the premium metal ball.
Important Tips:
Use it with a sock to start (could be too cold). Massaging and icing definitely loosens you up and makes you feel better, but you still have to prevent the pain in the first place. You still need stretching, orthotics and good shoes to prevent the initial damage.
Two things: Without the freezing component, it may be really painful for a very sore arch (So make sure to use ICE also). Also this only reduces pain, it does not stop the cause! You still need good orthotics, shoes and stretching to stop the pain in the first place!
Start with socks at first, especially if you have peripheral neuropathy => don’t freeze your foot! Remember that you still need good orthotics, good shoes and inserts as well as temporary activity reduction.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Manual Massage Devices:
Best Premium Massage Roller

Price:
Price not available
Overview:
Premium freezable metal ball that stays cold for up to 6 hours. Great for plantar fascia, neck, shoulders and calf muscles.
Pros:
Great reviews – near 5 star. Stays cold for a long time with deep penetrating plantar fascia massage. Used by professional athletes. Stays cold for HOURS!
Cons:
More expensive than some of the other options, but near perfect reviews.
Important Tips:
Use it with a sock to start (could be too cold). Massaging and icing definitely loosens you up and makes you feel better, but you still have to prevent the pain in the first place. You still need stretching, orthotics and good shoes to prevent the initial damage.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Manual Massage Devices:
Most Cost Effective Massage Roller.

Price:
$8.99
Overview:
Amazing Price, Great Reviews – Non-Freezable Massage Rolling Stick
Pros:
Great for what it does. You roll it back and forth along your plantar fascia massaging the swelling and irritation out. Decreases pain. Thousands of 5 star reviews on Amazon.
Cons:
Is not freezable like the other two options. Massaging a sore muscle without the cold sensation can be very painful and render it useless to you if really sore.
Important Tips:
Two things: Without the freezing component, it may be really painful for a very sore arch (So make sure to use ICE also). Also this only reduces pain, it does not stop the cause! You still need good orthotics, shoes and stretching to stop the pain in the first place!
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Manual Massage Devices:
Cost Effective Freezable Massage Roller.

Price:
$11.99
Overview:
Great price and it is freezable. Budget friendly freezable massage roller.
Pros:
Excellent reviews. It massages and ices, so it is a step up over the massage rollers. Near 5 star reviews with >500 reviews.
Cons:
It does a great job doing what it is supposed to do. Main downside is that it does not stay cold as long as the premium metal ball.
Important Tips:
Start with socks at first, especially if you have peripheral neuropathy => don’t freeze your foot! Remember that you still need good orthotics, good shoes and inserts as well as temporary activity reduction.
Affiliate Link (Buying through these links will connect you to Amazon):
Menthol Based Gels:
- Biofreeze is one of our favorites.
- These gels have been studied to work 2x as long as ice.
- This works great for the ball of the foot.
- Consider using these as options when resting on the couch or going to sleep at night.
Best Foot & Ankle Muscle/Ligament Pain Relief Products
Best & Proven Pain Relieving Gel.
Roll On Version of Biofreeze Gel.
A giant container of value size biofreeze.
Menthol Based Ointment with Hemp Extract




Price:
$34.95
$28.60
$175.00
$19.99
Overview:
The Proven and Scientifically Published Menthol Based Gel
Same as biofreeze gel, but the roll-on is prefered by some people for their feet, less messy.
8.1 lbs(3.67 kg) of Value Sized Biofreeze!
This is an alternative cream: Basically Biofreeze + hemp extract.
Pros:
Scientifically proven to loosen up and relief pain up to 2x longer than Ice. Less effort than ice and great reviews. 900+ 5 star reviews on Amazon.
The roll-on application of this biofreeze can be easier to apply. Less overall mess.
If you know you already love it and trust the reviews. This is a great value that lasts a long time.
It has great reviews, loved by the all natural crowd. 100s of 5 star reviews with a near perfect rating.
Cons:
Don’t put this on open sores or mucous membranes, it will burn! It can run out quick and doesn’t prevent pain, just helps it.
Not as easy to spread in other areas, main difference is the roll on applicator, same solution.
A gigantic bottle that could fall over and injure you! Seriously this could be too big in some situations.
Basically looks like menthol(active Biofreeze ingredient), but with hemp extract SKYROCKETING the price.
Important Tips:
Menthol is the active ingredient in this and other hemp based creams. It works similar to ice, but once you apply it you can just move on rather than waiting 20 minutes. **Works great to get your through the night if you have pain sleeping**
Roll-on method is best for the bottom of the feet. No other real advantage. Most patients like it prior to bed for easy sleeping without foot pain.
If you know you love it, this stuff works all over the sore areas in your body not just your foot. I have had many people get me to order this for them in the past and LOVED IT!
The hemp extract is almost nothing and likely a marketing gimmick. It’s basically Biofreeze with some hemp extract raising the price.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Muscle/Ligament Pain Relief Products
Best & Proven Pain Relieving Gel.

Price:
$34.95
Overview:
The Proven and Scientifically Published Menthol Based Gel
Pros:
Scientifically proven to loosen up and relief pain up to 2x longer than Ice. Less effort than ice and great reviews. 900+ 5 star reviews on Amazon.
Cons:
Don’t put this on open sores or mucous membranes, it will burn! It can run out quick and doesn’t prevent pain, just helps it.
Important Tips:
Menthol is the active ingredient in this and other hemp based creams. It works similar to ice, but once you apply it you can just move on rather than waiting 20 minutes. **Works great to get your through the night if you have pain sleeping**
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Muscle/Ligament Pain Relief Products
Roll On Version of Biofreeze Gel.

Price:
$28.60
Overview:
Same as biofreeze gel, but the roll-on is prefered by some people for their feet, less messy.
Pros:
The roll-on application of this biofreeze can be easier to apply. Less overall mess.
Cons:
Not as easy to spread in other areas, main difference is the roll on applicator, same solution.
Important Tips:
Roll-on method is best for the bottom of the feet. No other real advantage. Most patients like it prior to bed for easy sleeping without foot pain.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Muscle/Ligament Pain Relief Products
A giant container of value size biofreeze.

Price:
$175.00
Overview:
8.1 lbs(3.67 kg) of Value Sized Biofreeze!
Pros:
If you know you already love it and trust the reviews. This is a great value that lasts a long time.
Cons:
A gigantic bottle that could fall over and injure you! Seriously this could be too big in some situations.
Important Tips:
If you know you love it, this stuff works all over the sore areas in your body not just your foot. I have had many people get me to order this for them in the past and LOVED IT!
Affiliate Link (Buying through these links will connect you to Amazon):
Best Foot & Ankle Muscle/Ligament Pain Relief Products
Menthol Based Ointment with Hemp Extract

Price:
$19.99
Overview:
This is an alternative cream: Basically Biofreeze + hemp extract.
Pros:
It has great reviews, loved by the all natural crowd. 100s of 5 star reviews with a near perfect rating.
Cons:
Basically looks like menthol(active Biofreeze ingredient), but with hemp extract SKYROCKETING the price.
Important Tips:
The hemp extract is almost nothing and likely a marketing gimmick. It’s basically Biofreeze with some hemp extract raising the price.
Affiliate Link (Buying through these links will connect you to Amazon):
Massage Sticks:
- These can work great for loosening your muscles.
- This is means for your hamstring and calf muscles. This can loosen the ankle tightness, putting pressure on the ball of your foot.
- This allows less tightness and pressure on the ball of your foot.
Leg & Calf Muscle Massage Roller Sticks:
Best Overall Muscle Massage Stick
Best Cost Effective Massage Roller.
Best & Most Affordable Foot Massage Unit



Price:
$39.95
Price not available
Price not available
Overview:
This is a great option because hair or skin never gets pinched between the wheels. Softer interface.
Great option for an amazing cost. Not as sturdy and comfortable as the tiger tail.
A well reviewed foot massage unit.
Pros:
Best reviews. Hair and skin cannot get pinched. Almost instantly makes you less tender and more flexible. This is a professional grade massage roller.
Amazing reviews for the price point. It essentially does the same job. Muscles feel great afterward. Same overall benefit.
Amazing reviews averaging almost 5 stars. Reasonable price compared to most other units. Relieves swelling and inflammation in your feet naturally.
Cons:
If truly injured (break or tear) this won’t fix your pain. But no real downsides as far as what a massage roller does. Reviews are near perfect.
Wheels and handles can come loose. As a result it can gap and pinch skin and leg hairs. Not as durable as the other roller recommended here.
A more expensive version of manual and ice massage. The extra $ is basically to remove the manual labor yourself if you are OK with that!
Important Tips:
Studies show how effective massage rollers are: Use for 30-60 seconds to loosen up tight muscles, and then you can stretch further short term(1-2 hrs). Great for calf, hamstring, thight and IT band muscle stretching.
Same as for the more expensive one. Studies show the real benefits appear in 30-60 seconds per muscle => less sore and more flexible. That is the time to take advantage and play sports/stay loose. Very proven results.
This can actually help loosen up your calf muscles and foot muscles for a better stretch. So take advantage! You will be less sore and more flexible, but the results disappear after 1-2 hours or so!
Affiliate Link (Buying through these links will connect you to Amazon):
Leg & Calf Muscle Massage Roller Sticks:
Best Overall Muscle Massage Stick

Price:
$39.95
Overview:
This is a great option because hair or skin never gets pinched between the wheels. Softer interface.
Pros:
Best reviews. Hair and skin cannot get pinched. Almost instantly makes you less tender and more flexible. This is a professional grade massage roller.
Cons:
If truly injured (break or tear) this won’t fix your pain. But no real downsides as far as what a massage roller does. Reviews are near perfect.
Important Tips:
Studies show how effective massage rollers are: Use for 30-60 seconds to loosen up tight muscles, and then you can stretch further short term(1-2 hrs). Great for calf, hamstring, thight and IT band muscle stretching.
Affiliate Link (Buying through these links will connect you to Amazon):
Leg & Calf Muscle Massage Roller Sticks:
Best Cost Effective Massage Roller.

Price:
Price not available
Overview:
Great option for an amazing cost. Not as sturdy and comfortable as the tiger tail.
Pros:
Amazing reviews for the price point. It essentially does the same job. Muscles feel great afterward. Same overall benefit.
Cons:
Wheels and handles can come loose. As a result it can gap and pinch skin and leg hairs. Not as durable as the other roller recommended here.
Important Tips:
Same as for the more expensive one. Studies show the real benefits appear in 30-60 seconds per muscle => less sore and more flexible. That is the time to take advantage and play sports/stay loose. Very proven results.
Affiliate Link (Buying through these links will connect you to Amazon):
Leg & Calf Muscle Massage Roller Sticks:
Best & Most Affordable Foot Massage Unit

Price:
Price not available
Overview:
A well reviewed foot massage unit.
Pros:
Amazing reviews averaging almost 5 stars. Reasonable price compared to most other units. Relieves swelling and inflammation in your feet naturally.
Cons:
A more expensive version of manual and ice massage. The extra $ is basically to remove the manual labor yourself if you are OK with that!
Important Tips:
This can actually help loosen up your calf muscles and foot muscles for a better stretch. So take advantage! You will be less sore and more flexible, but the results disappear after 1-2 hours or so!
Affiliate Link (Buying through these links will connect you to Amazon):
Ball of the Foot Stress Relief.
- The key is to prevent future pain.
- If you can get rid of the pain and swelling, this will let you start walking normally.
- If you can walk normally, the vast majority of your pain should gradually start to go away.
- This means proper cushion, proper stability, and pressure relief from the front of your foot.
- This will relieve pressure from your big toe, your 2nd toe, your Morton’s neuroma, your plantar plate, hammertoes and joint capsules.
Best Metatarsalgia Shoes:
- Getting a great supportive pair of shoes will make sure that there is pressure removed from the ball of your foot.
- This is especially important if you have metatarsalgia, Morton’s neuroma, 2nd metatarsal overload syndrome, and capsulitis!
- Consider shoes combined with a good supportive orthotic for the best pain relief!
- The following link will show you what our favorites are.
Best Ball of the Foot Insoles:
- These are our recommended orthotics & insoles.
- There are different types of different shoes.
- Women’s shoes usually need a less bulky orthotic but allow for less correction.
- A full-length orthotic requires a running shoe, boot, or comfortable walking/dress shoe.
Best Full-Length Orthotics:
- Full-length orthotics are the most recommended type for the ball of the foot pain.
- Be aware that if they are too uncomfortable, it might be worth starting with a less corrective pair.
- Eventually, you can then work your way up to these.
Best Medium to Heavy Duty Heel Pain Orthotics:
Best Overall Orthotic For Everything (Medium Thick Fit)
Best Heavy Duty Orthotic (Thickest Fit)
Best SOFTER Choice For Sensitive Feet (Medium Thick Fit)
Best Women’s Orthotics




Price:
$44.95
$47.66
Price not available
$59.95
Overview:
These work best in shoes with laces and running shoes. Not good for dress shoes or women’s cute shoes.
Biggest and most corrective option. Only use for running shoes or work boots. Not cute shoes.
These are full length inserts, but softer. Great if you can’t tolerate the firmer ones. Best for very sore and sensitive feet.
Great Support & Better Fit
Pros:
Pretty much guaranteed to help you if it fits in your shoes and you give it 2 weeks to get used to. 5,000+ amazon reviews, great track record.
My personal favorite, but not for everyone. Amazing reviews over 3,500. But not for everyone. Only for bigger shoes that can fit them
They are softer and the initial break in time is AMAZING. But longer term benefits are less. >500 Almost 5 star amazon rating.
Sleek, supportive and have a better fit than the orthotics above.
Cons:
Do not wear these in cute or dress shoes!
Bigger and bulkier than all the other ones. You will be dissappointed if you have a cute women’s shoe or dress shoe. This is meant for running shoes and boots.
Great to start with, but don’t correct long term as much as the other ones.
A little bit more expensive.
Crucial Tips:
Ease in to these, 1-2hrs a day. They are like braces for your teeth, they suck at the beginning! But they will make your feet pain free as 1-2 weeks go by. Don’t give up on them after 1 or 2 days. Everyone feels off at the beginning!
This has the most correction, but hardest break in time! IF SENSITIVE, USE A SOFTER PAIR FIRST! But if you get these, you must break them in. Give it 1-2 hours a day, but then you will start to have excellent results. The bad reviews are all people who couldn’t fit it into their shoes and gave up too quickly. You have been WARNED!
If you are very sore, TRY THESE FIRST! These are easiest to break in with initially. If you are very sore and rigid, don’t use the heavy duty ones to start with.
These will have a harder time fitting in flats and pointed shoes.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Medium to Heavy Duty Heel Pain Orthotics:
Best Overall Orthotic For Everything (Medium Thick Fit)

Price:
$44.95
Overview:
These work best in shoes with laces and running shoes. Not good for dress shoes or women’s cute shoes.
Pros:
Pretty much guaranteed to help you if it fits in your shoes and you give it 2 weeks to get used to. 5,000+ amazon reviews, great track record.
Cons:
Do not wear these in cute or dress shoes!
Crucial Tips:
Ease in to these, 1-2hrs a day. They are like braces for your teeth, they suck at the beginning! But they will make your feet pain free as 1-2 weeks go by. Don’t give up on them after 1 or 2 days. Everyone feels off at the beginning!
Affiliate Link (Buying through these links will connect you to Amazon):
Best Medium to Heavy Duty Heel Pain Orthotics:
Best Heavy Duty Orthotic (Thickest Fit)

Price:
$47.66
Overview:
Biggest and most corrective option. Only use for running shoes or work boots. Not cute shoes.
Pros:
My personal favorite, but not for everyone. Amazing reviews over 3,500. But not for everyone. Only for bigger shoes that can fit them
Cons:
Bigger and bulkier than all the other ones. You will be dissappointed if you have a cute women’s shoe or dress shoe. This is meant for running shoes and boots.
Crucial Tips:
This has the most correction, but hardest break in time! IF SENSITIVE, USE A SOFTER PAIR FIRST! But if you get these, you must break them in. Give it 1-2 hours a day, but then you will start to have excellent results. The bad reviews are all people who couldn’t fit it into their shoes and gave up too quickly. You have been WARNED!
Affiliate Link (Buying through these links will connect you to Amazon):
Best Medium to Heavy Duty Heel Pain Orthotics:
Best SOFTER Choice For Sensitive Feet (Medium Thick Fit)

Price:
Price not available
Overview:
These are full length inserts, but softer. Great if you can’t tolerate the firmer ones. Best for very sore and sensitive feet.
Pros:
They are softer and the initial break in time is AMAZING. But longer term benefits are less. >500 Almost 5 star amazon rating.
Cons:
Great to start with, but don’t correct long term as much as the other ones.
Crucial Tips:
If you are very sore, TRY THESE FIRST! These are easiest to break in with initially. If you are very sore and rigid, don’t use the heavy duty ones to start with.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Medium to Heavy Duty Heel Pain Orthotics:
Best Women’s Orthotics

Price:
$59.95
Overview:
Great Support & Better Fit
Pros:
Sleek, supportive and have a better fit than the orthotics above.
Cons:
A little bit more expensive.
Crucial Tips:
These will have a harder time fitting in flats and pointed shoes.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Dress Shoe Orthotics:
- These are a stronger option for shoes with tight dress shoes.
- Just be aware that less corrective orthotics & tight shoes are usually not a good combination.
Best Dress Shoe Orthotics:
Best Fitting Dress Shoe Orthotic (3/4″)
Best Full Length Dress Orthotic.
Great Heavy Duty Insole for Men



Price:
Price not available
Price not available
$34.95
Overview:
This is my top choice due to best fit. It is a little less supportive than full length, but fit is the key in dress shoes!
Best option if you can fit a full length orthotic. This does give you most control.
Great price and heavy duty insole for Oxford shoes.
Pros:
Excellent overall fit. This will fit in almost every dress shoe. Excellent reviews and reasonable cost overall. Can’t go wrong in most cases.
Great color dress option. Not the most corrective, but very color and dress appropriate. Great Reviews. Better correction and relief than the 3/4″ length.
These fit in most shoes and have really good predictable results
Cons:
Less correction than full length and heavy duty orthotics.
These can have a poor fit in in some shoes. If you have tight shoes, DO NOT BUY the full length orthotic! You have been warned.
They are not full length and thus do not provide as much support
Crucial Tips:
If you haven’t used dress orthotics before, get this one and avoid poor fit. If you wear dress shoes every day with room, the full length might give you more support.
This is will work great in most men’s shoes that are not pointy. If you have a rounded toe box, this will probably work well. If a tight shoe go with the 3/4″ length.
Get these for Oxford and pointed shoes. This will provide best results.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Dress Shoe Orthotics:
Best Fitting Dress Shoe Orthotic (3/4″)

Price:
Price not available
Overview:
This is my top choice due to best fit. It is a little less supportive than full length, but fit is the key in dress shoes!
Pros:
Excellent overall fit. This will fit in almost every dress shoe. Excellent reviews and reasonable cost overall. Can’t go wrong in most cases.
Cons:
Less correction than full length and heavy duty orthotics.
Crucial Tips:
If you haven’t used dress orthotics before, get this one and avoid poor fit. If you wear dress shoes every day with room, the full length might give you more support.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Dress Shoe Orthotics:
Best Full Length Dress Orthotic.

Price:
Price not available
Overview:
Best option if you can fit a full length orthotic. This does give you most control.
Pros:
Great color dress option. Not the most corrective, but very color and dress appropriate. Great Reviews. Better correction and relief than the 3/4″ length.
Cons:
These can have a poor fit in in some shoes. If you have tight shoes, DO NOT BUY the full length orthotic! You have been warned.
Crucial Tips:
This is will work great in most men’s shoes that are not pointy. If you have a rounded toe box, this will probably work well. If a tight shoe go with the 3/4″ length.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Dress Shoe Orthotics:
Great Heavy Duty Insole for Men

Price:
$34.95
Overview:
Great price and heavy duty insole for Oxford shoes.
Pros:
These fit in most shoes and have really good predictable results
Cons:
They are not full length and thus do not provide as much support
Crucial Tips:
Get these for Oxford and pointed shoes. This will provide best results.
Affiliate Link (Buying through these links will connect you to Amazon):
Best 3/4 Length Orthotics:
- These may be a good option for the ball of the foot if the full-length orthotics are too tight or too uncomfortable.
Best Flat Shoe (Non-Lace Up) Orthotics:
Best Choice For Tight Women’s Shoes or High Heels..

Price:
Price not available
Overview:
These are the best fitting for the most narrow shoes. Some but not great correction.
Pros:
They will fit in even the tightest shoes! Guaranteed to make you feel better, but you know what you are getting in a tight shoes. Great reviews and price.
Cons:
At the end of the day high heels and slender orthotics help, but never cure all your pain. Make the best of a painful shoe!
Crucial Tips:
**WARNING***: If your shoe almost just barely fits onto your foot, this WILL NOT FIT! Be aware, it still needs a small amount of space to fit.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Flat Shoe (Non-Lace Up) Orthotics:
Best Choice For Tight Women’s Shoes or High Heels..

Price:
Price not available
Overview:
These are the best fitting for the most narrow shoes. Some but not great correction.
Pros:
They will fit in even the tightest shoes! Guaranteed to make you feel better, but you know what you are getting in a tight shoes. Great reviews and price.
Cons:
At the end of the day high heels and slender orthotics help, but never cure all your pain. Make the best of a painful shoe!
Crucial Tips:
**WARNING***: If your shoe almost just barely fits onto your foot, this WILL NOT FIT! Be aware, it still needs a small amount of space to fit.
Affiliate Link (Buying through these links will connect you to Amazon):
Get A Great Dynamic Stretch:
- It is possible to stretch on your own, but these products can also really help!
- Personally, I have the stationary block set up in my kitchen to stretch every day multiple times while getting my coffee!
- This will take pressure off of the ball of your foot.
Best Standing Foot & Ankle Stretching Devices:
Best Premium Plantar Fascia Stretching Device.
Best Budget Plantar Fascia Stretching Stretch Device.
Best Stationary Calf Stretching Device.
Best Hamstring Stretching Device




Price:
$37.97
$24.36
$39.99
$69.95
Overview:
Great Stretching Device While Standing. (4.9 Amazon Rating)
Plastic and Lighter Plantar Fascia & Achilles Stretching Device.
Premium Best Rated Wood Ankle Stretch Device.
Uses gravity to stretch your hamstring for you. Great reviews and track record.
Pros:
Very sturdy and durable. Great bottom grip and weight so it won’t slide on you. Perfect 5 star review on Amazon.
Amazing cost, still works and 1,300+ 5 star reviews. Works great overall and gives you the same stretch.
Near perfect 4.8 star review on Amazon. Great sturdy device that stretches your calf and hamstring. All you have to do is lean forward. Can be very effective.
Reviews on Amazon are >4.5 overall with hundreds of reviews. It uses gravity to stretch for you, allows you to also use your hips. Gets great results.
Cons:
More expensive and built like a tank = more weight. If you can’t balance well or support yourself it could be dangerous.
The plastic and less bulk/grip makes it more dangerous to slip. Less premium feel to it.
Nothing wrong with the product, as the reviews suggest, but at the end of the day you can do this stuff yourself (just a little bit harder).
These are stretches that you realistically can do on your own. If budget is tight, this is not worth it. If you need help with hamstring stretching, it can make all the difference.
Important Tips:
Make sure you can balance yourself well against a counter/railing. Do only one foot at a time to prevent falling. Uses your body weight to stretch for you.
Even more important to balance yourself well with this device, make sure you don’t injure yourself with this thing! Still gives you a great stretch to the area.
Make sure you balance yourself on a counter/railing. You need to keep up with this daily at least 15-30 second x 3 or so per morning. It doesn’t stretch for you!
Need to do 3-5 stretches per day 15-30 seconds. You should notice a massive difference to knee and hamstring tightness. You can massage roll ahead to time for better results for 30-60 seconds.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Standing Foot & Ankle Stretching Devices:
Best Premium Plantar Fascia Stretching Device.

Price:
$37.97
Overview:
Great Stretching Device While Standing. (4.9 Amazon Rating)
Pros:
Very sturdy and durable. Great bottom grip and weight so it won’t slide on you. Perfect 5 star review on Amazon.
Cons:
More expensive and built like a tank = more weight. If you can’t balance well or support yourself it could be dangerous.
Important Tips:
Make sure you can balance yourself well against a counter/railing. Do only one foot at a time to prevent falling. Uses your body weight to stretch for you.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Standing Foot & Ankle Stretching Devices:
Best Budget Plantar Fascia Stretching Stretch Device.

Price:
$24.36
Overview:
Plastic and Lighter Plantar Fascia & Achilles Stretching Device.
Pros:
Amazing cost, still works and 1,300+ 5 star reviews. Works great overall and gives you the same stretch.
Cons:
The plastic and less bulk/grip makes it more dangerous to slip. Less premium feel to it.
Important Tips:
Even more important to balance yourself well with this device, make sure you don’t injure yourself with this thing! Still gives you a great stretch to the area.
Affiliate Link (Buying through these links will connect you to Amazon):
Best Standing Foot & Ankle Stretching Devices:
Best Stationary Calf Stretching Device.

Price:
$39.99
Overview:
Premium Best Rated Wood Ankle Stretch Device.
Pros:
Near perfect 4.8 star review on Amazon. Great sturdy device that stretches your calf and hamstring. All you have to do is lean forward. Can be very effective.
Cons:
Nothing wrong with the product, as the reviews suggest, but at the end of the day you can do this stuff yourself (just a little bit harder).
Important Tips:
Make sure you balance yourself on a counter/railing. You need to keep up with this daily at least 15-30 second x 3 or so per morning. It doesn’t stretch for you!
Affiliate Link (Buying through these links will connect you to Amazon):
Best Standing Foot & Ankle Stretching Devices:
Best Hamstring Stretching Device

Price:
$69.95
Overview:
Uses gravity to stretch your hamstring for you. Great reviews and track record.
Pros:
Reviews on Amazon are >4.5 overall with hundreds of reviews. It uses gravity to stretch for you, allows you to also use your hips. Gets great results.
Cons:
These are stretches that you realistically can do on your own. If budget is tight, this is not worth it. If you need help with hamstring stretching, it can make all the difference.
Important Tips:
Need to do 3-5 stretches per day 15-30 seconds. You should notice a massive difference to knee and hamstring tightness. You can massage roll ahead to time for better results for 30-60 seconds.
Affiliate Link (Buying through these links will connect you to Amazon):
Ball of the Foot Pain

