✅ Medically reviewed by Dr. Thomas Biernacki, DPM — Board-Certified Podiatrist · Last updated April 7, 2026

Medically reviewed by Dr. Carl Jay, DPM
Board-Certified Podiatric Surgeon · Balance Foot & Ankle
Last reviewed: April 2026
Quick Answer: What Is Permanent Ingrown Toenail Removal?
Permanent ingrown toenail removal is an in-office procedure called a partial nail avulsion with matrixectomy. Under local anesthesia, the podiatrist removes the ingrown nail border and applies a chemical (phenol) to the nail matrix to permanently prevent that edge from regrowing. The procedure takes about 15 minutes, has a 95%+ success rate, and most patients return to normal shoes within 2–3 days. It’s the gold-standard treatment for recurrent ingrown toenails.
Table of Contents
- When Is Surgery Needed for an Ingrown Toenail?
- Types of Ingrown Toenail Surgery
- What Happens During the Procedure
- Recovery Timeline — Day by Day
- Post-Procedure Aftercare Protocol
- Best Products for Recovery
- Risks and Complications
- Home Treatment vs. Surgery — When to Choose What
- Warning Signs After Surgery
- Frequently Asked Questions
- The Bottom Line
You’ve tried soaking your toe, cutting the nail differently, stuffing cotton under the edge, and maybe even digging out the ingrown part yourself with tweezers. But the pain keeps coming back — every few weeks or months, the same corner of the same toenail digs into the same spot, gets red, swollen, and sometimes infected. You’re done dealing with it.
If this sounds familiar, you’re not alone. Ingrown toenails are one of the most common foot problems we treat at Balance Foot & Ankle — and permanent removal of the offending nail border is one of the most satisfying procedures we perform because the results are immediate and lasting. Patients walk in with a painful, infected toe and walk out with a permanently fixed problem. Here’s everything you need to know about the procedure.
When Is Surgery Needed for an Ingrown Toenail?
Not every ingrown toenail requires surgery. Mild, first-time ingrown nails often respond to warm soaks, proper trimming, and wider shoes. But surgery becomes the right choice when:
The ingrown nail keeps coming back. If you’ve had 2 or more episodes of the same nail border becoming ingrown, the nail matrix is producing a nail edge that’s genetically curved into the skin. Trimming will never fix this permanently — the nail regrows the same problematic shape every time. Matrixectomy addresses the root cause.
Infection is present or recurrent. A red, swollen toe with pus, granulation tissue (that red bumpy overgrowth), or spreading redness indicates bacterial infection. Infected ingrown nails need the offending nail border removed — antibiotics alone don’t fix the mechanical problem of a nail digging into skin.
You have diabetes or poor circulation. In patients with diabetes, peripheral neuropathy, or peripheral arterial disease, an ingrown toenail can quickly escalate to cellulitis, osteomyelitis (bone infection), or worse. We take these cases very seriously and recommend early intervention rather than conservative management.
The pain is affecting daily activities. If an ingrown nail is preventing you from wearing shoes comfortably, exercising, or walking without pain, the procedure provides definitive relief. There’s no reason to endure chronic pain from a problem that has a quick, highly effective fix.
Types of Ingrown Toenail Surgery
| Procedure | What It Involves | Permanent? | Best For |
|---|---|---|---|
| Partial nail avulsion (without matrixectomy) | Remove the ingrown nail border only | No — nail edge regrows in 2–4 months | First-time ingrown nail, mild cases, temporary relief |
| Partial nail avulsion with chemical matrixectomy | Remove nail border + apply phenol to destroy the nail matrix | Yes — 95%+ permanent cure rate | Recurrent ingrown nails, infected ingrown nails, permanent fix |
| Total nail avulsion with matrixectomy | Remove entire nail + destroy entire matrix | Yes — no nail regrows | Severe deformity, fungal nails with recurrent ingrown, both borders ingrown |
| Wedge excision (Winograd procedure) | Surgically cut out the nail border and matrix tissue | Yes — 97%+ success rate | Failed chemical matrixectomy, very wide nail borders |
At Balance Foot & Ankle, we perform partial nail avulsion with phenol matrixectomy in approximately 90% of our ingrown toenail surgeries. It offers the best balance of effectiveness, minimal tissue disruption, and fast recovery. The Winograd excision is reserved for cases where chemical matrixectomy has failed or the nail anatomy requires a wider resection.
What Happens During the Procedure — Step by Step
Understanding exactly what happens removes the anxiety. Here’s the procedure from start to finish:
Step 1: Numbing the Toe (2–3 minutes)
We inject local anesthetic (lidocaine) at the base of the toe using a digital block. This numbs the entire toe. You’ll feel a brief sting from the injection — this is the most uncomfortable part of the entire procedure. Within 2–3 minutes, the toe is completely numb and you won’t feel anything for the rest of the procedure.
Step 2: Preparing the Toe (1 minute)
We clean the toe with antiseptic solution and apply a tourniquet (a small rubber band around the base of the toe) to minimize bleeding and allow clear visualization of the nail matrix.
Step 3: Removing the Nail Border (2–3 minutes)
Using a specialized nail splitter, we separate the ingrown edge from the rest of the nail plate — typically removing a 2–4mm strip along the affected border. The strip is cut all the way back to the base of the nail (the matrix area under the cuticle). The remaining nail plate stays intact and continues to grow normally.
Step 4: Chemical Matrixectomy — The Permanent Part (3–4 minutes)
This is what makes the procedure permanent. We apply phenol (89% concentration) to the exposed nail matrix — the growth center where the removed nail border originated. Phenol cauterizes the matrix cells, permanently preventing that strip of nail from regrowing. We apply phenol in 3 separate 30-second applications, flushing with alcohol between each application to neutralize the chemical and control the depth of tissue destruction. This precision is what achieves the 95%+ success rate.
Step 5: Bandaging (2 minutes)
The tourniquet is removed, we clean the area, apply antibiotic ointment, and wrap the toe in a sterile bandage. You’re done. The entire procedure from injection to bandage takes about 15 minutes. You walk out of the office on your own feet — no crutches, no special shoes, no wheelchair.
Recovery Timeline — Day by Day
| Timeframe | What to Expect |
|---|---|
| Day 0 (procedure day) | Toe is numb for 2–4 hours. Mild aching as anesthesia wears off. Take OTC ibuprofen or acetaminophen. Keep foot elevated when possible. No soaking. |
| Days 1–3 | Mild soreness (most patients rate 2–3/10). Change bandage daily. Can wear loose, open-toed shoes. Most patients return to desk work the next day. |
| Days 4–7 | Begin daily warm water soaks (plain warm water, 10 minutes). Apply antibiotic ointment after each soak. Soreness is minimal. Can wear regular shoes if comfortable. |
| Weeks 2–3 | Drainage decreases. The site where phenol was applied produces clear/yellow drainage — this is normal healing, not infection. Continue daily soaks and bandaging. |
| Weeks 3–6 | Site fully heals. Drainage stops. The nail border where the strip was removed fills in with smooth skin. No more bandaging needed. |
| Months 2–4 | Final result visible. The remaining nail has grown out fully. The narrow strip where the border was removed is now covered by normal skin. The nail looks slightly narrower but cosmetically excellent. |
Post-Procedure Aftercare Protocol
Proper aftercare is the difference between a smooth 3-week recovery and a complicated 6-week one. Follow this protocol exactly:
Days 1–3: Keep the initial bandage dry. Change it daily using sterile gauze and antibiotic ointment. No soaking, no submerging in water. Wear open-toed shoes or a loose sneaker. Avoid strenuous exercise.
Days 4–21: Begin daily warm water soaks (plain warm water, 10 minutes). After soaking, dry the toe, apply antibiotic ointment, and rebandage with sterile gauze. You’ll notice clear or slightly yellow drainage from the phenol application site — this is normal wound healing fluid, not infection. The drainage is the most common source of patient concern, but it’s expected and resolves within 2–3 weeks.
Weeks 3–6: Continue soaks if drainage persists. Most patients can stop bandaging by week 3. Keep the area clean and dry. Resume all normal activities including exercise. Avoid tight shoes that compress the healing toe.
Best Products for Recovery
These products support healing after ingrown toenail surgery and help prevent recurrence:
🏆 #1 Pick: Brooks Ghost (Wide Toe Box)
Best for: Protecting the healing toe and preventing recurrence
Why we recommend it: Tight shoes are the most common contributing factor to ingrown toenails. The Brooks Ghost has the widest toe box among major running shoes, giving your recovering toe space to heal without compression. We recommend switching to wide toe box shoes permanently after ingrown toenail surgery — it’s the single most effective prevention measure. Wear these during the recovery period and consider making them your everyday shoe going forward.
Oofos OOahh Recovery Sandals
Best for: Immediate post-procedure footwear (days 1–7)
Why we recommend it: During the first week after surgery, you want zero pressure on the healing toe. Oofos recovery sandals have an open toe design that eliminates contact with the surgical site and proprietary OOfoam cushioning that absorbs 37% more impact than standard EVA foam. Ideal for around the house and short errands during the bandaging phase. Many of our patients keep wearing them for general recovery and relaxation long after their toe has healed.
Tea Tree Oil (100% Pure)
Best for: Natural antimicrobial support during healing
Why we recommend it: After the first week of healing, adding 2–3 drops of tea tree oil to your warm soaking water provides mild antibacterial and antifungal benefits. Tea tree oil has demonstrated activity against Staphylococcus aureus — the most common bacteria in post-operative nail infections. It’s a gentle, natural way to support clean healing alongside your antibiotic ointment protocol.
Correct Toes Toe Spacers
Best for: Long-term prevention of ingrown toenail recurrence
Why we recommend it: Correct Toes are medical-grade silicone toe spacers that gently realign the big toe and prevent it from being compressed against the second toe. This compression is a major contributor to ingrown nails on the medial (inner) border of the big toe. Worn inside wide shoes, they maintain proper toe alignment and reduce the mechanical forces that push the nail into the skin. Start wearing them 3–4 weeks post-surgery once the site is fully healed.
Disclosure: Some links above are affiliate links. We only recommend products we use in our practice or have vetted for our patients. Affiliate commissions help support our free educational content. Your price is not affected.
Risks and Complications
Partial nail avulsion with matrixectomy is one of the safest procedures in podiatric surgery. But like all procedures, it carries potential risks:
Regrowth of the nail border (5% chance): In approximately 1 in 20 cases, a small spicule of nail regrows from surviving matrix cells. If this happens, a second matrixectomy (or surgical excision) resolves it permanently. The 5% failure rate is typically related to inadequate phenol contact time during the initial procedure.
Post-operative infection (uncommon): With proper aftercare, infection rates are very low (less than 5%). Signs include increasing redness, pus, and worsening pain after the first 48 hours. A short course of oral antibiotics clears most post-operative infections quickly.
Prolonged drainage (common but normal): The phenol application creates a controlled chemical burn to the matrix tissue. This area weeps clear-to-yellow drainage for 2–3 weeks as it heals. This is not infection — it’s normal wound healing. It’s the most common source of patient concern, but it’s expected.
Cosmetic narrowing of the nail: The nail will be 2–4mm narrower on the treated side. Most patients consider this a cosmetic improvement over the chronically inflamed, red, swollen appearance of the recurrent ingrown nail. The narrowing is subtle and the remaining nail looks healthy and normal.
Home Treatment vs. Surgery — When to Choose What
| Scenario | Recommended Approach |
|---|---|
| First-time ingrown nail, mild redness, no pus | Home treatment: warm soaks, proper trimming, wider shoes |
| First-time ingrown nail with pus or infection | Office visit: possible temporary nail border removal + antibiotics |
| Second or third recurrence of same ingrown nail | Permanent surgery: partial avulsion with matrixectomy |
| Ingrown nail in a patient with diabetes | Office visit for ANY severity: do not self-treat |
| Both borders of the nail are ingrown | Bilateral partial avulsion or total avulsion with matrixectomy |
| Severely deformed nail from fungus + ingrown | Total nail avulsion with matrixectomy |
Warning Signs After Surgery
⚠️ Contact Your Podiatrist If You Experience:
- Red streaks extending from the toe toward the foot — indicates spreading infection (lymphangitis) that requires prompt antibiotic treatment.
- Thick, opaque pus (not clear drainage) after the first week — clear/yellow drainage is normal; thick white or green pus suggests bacterial infection.
- Increasing pain after the first 48 hours — post-procedure pain should steadily decrease. Worsening pain after 2 days suggests infection or hematoma.
- Fever or chills — systemic symptoms combined with a surgical site indicate the infection needs systemic antibiotic treatment.
- A nail spicule regrowing from the treated border — if you feel a sharp point or see a thin nail strip emerging 2–3 months after surgery, the matrix wasn’t fully ablated and may need re-treatment.
- Significant bleeding that soaks through multiple bandages — mild spotting is normal; heavy bleeding may indicate a blood vessel issue and needs evaluation.
More Podiatrist-Recommended Ingrown Essentials
Roomy Walking Shoe
New Balance 990v6 — wide toe box prevents toe jamming that causes ingrowns.
Extra-Depth Diabetic Shoe
Orthofeet Sprint — no pressure on nail edges, seamless lining.
Moisture-Wicking Compression Sock
OS1st FS4 — dry environment reduces ingrown infection risk.
As an Amazon Associate, Balance Foot & Ankle earns from qualifying purchases. Product recommendations are based on clinical experience; prices and availability shown above update live from Amazon.
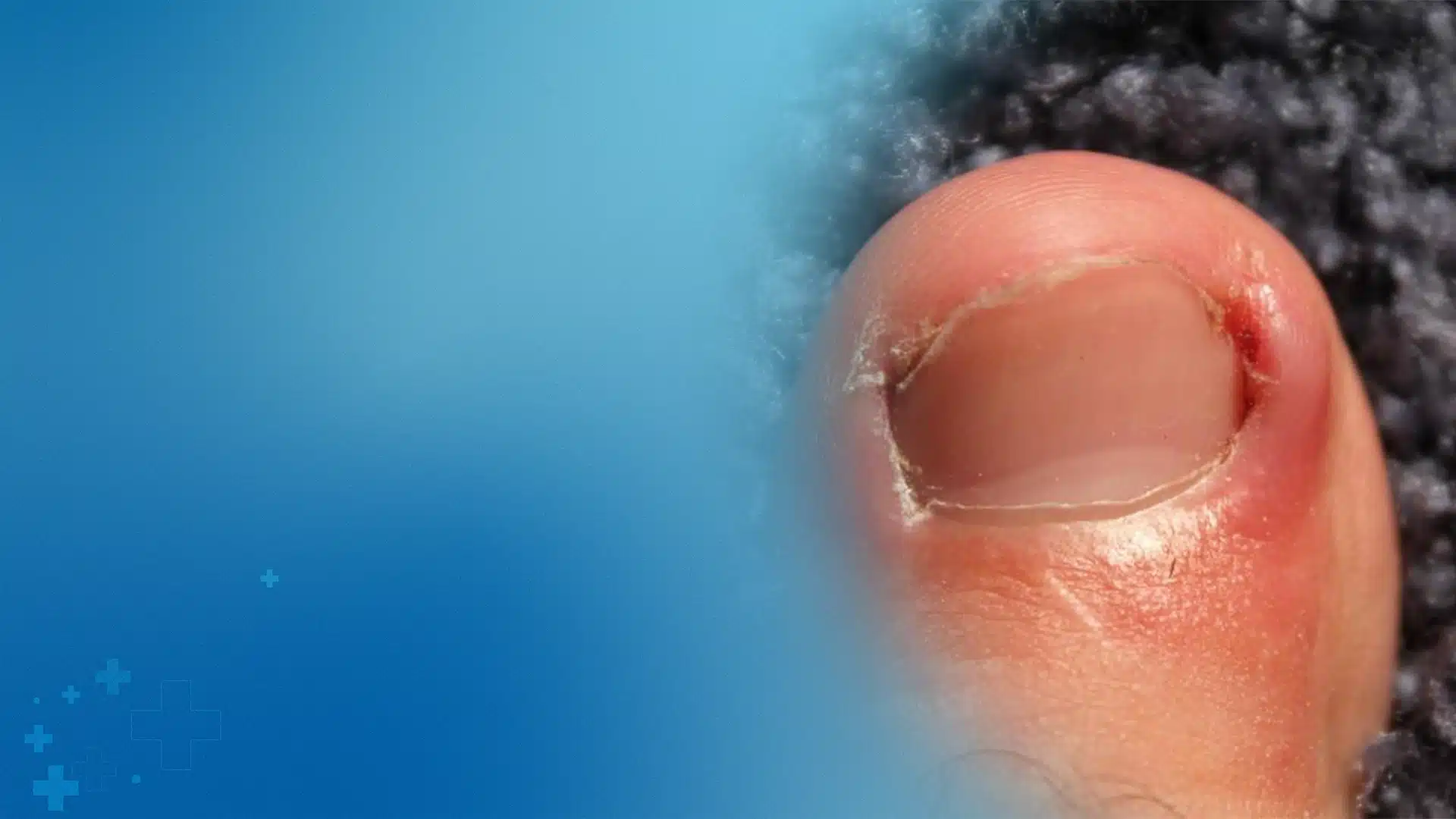
When to See a Podiatrist
Home care works for early ingrowns — but if redness, drainage, or granulation tissue has developed, the nail edge needs professional removal. At Balance Foot & Ankle, matrixectomy (permanent corner removal) is a 15-minute in-office procedure that prevents recurrence. Most patients walk out the same day and return to normal shoes within 48 hours.
Call Balance Foot & Ankle: (810) 206-1402 · Book online · Offices in Howell & Bloomfield Hills
Frequently Asked Questions
Does permanent ingrown toenail removal hurt?
The injection to numb the toe is the only uncomfortable part — it feels like a brief pinch that lasts 5–10 seconds. Once the toe is numb, you won’t feel the procedure at all. After the anesthesia wears off (2–4 hours), most patients describe mild aching that’s easily controlled with over-the-counter ibuprofen. The vast majority of patients say it was much less painful than they expected.
How long does it take to walk normally after ingrown toenail surgery?
Most patients walk normally within 24–48 hours. The toe is sore but weight-bearing is safe immediately. We recommend wearing open-toed shoes or a loose sneaker for the first week. Patients can typically return to desk work the next day and to moderate physical activity within a week. Running and high-impact exercise can resume at 2–3 weeks.
Can an ingrown toenail grow back after permanent removal?
The success rate for phenol matrixectomy is approximately 95–97%. In about 3–5% of cases, a small nail spicule regrows from surviving matrix cells. If this happens, a second procedure (either repeat phenol application or surgical excision) has an even higher success rate. After two procedures, the permanent cure rate is essentially 100%.
Will my nail look normal after the procedure?
The remaining nail looks slightly narrower (by 2–4mm on the treated side) but otherwise grows normally and looks healthy. Most patients and their families can’t tell which toe had the procedure unless they look very closely. The cosmetic result is far better than the chronically red, swollen, infected appearance of a recurring ingrown nail.
The Bottom Line
Permanent ingrown toenail removal is a quick, safe, in-office procedure with a 95%+ success rate. It’s the gold-standard treatment for ingrown toenails that keep coming back. The procedure takes about 15 minutes, most patients return to normal shoes within 2–3 days, and the results are permanent. If you’re tired of dealing with recurring ingrown nails, this is the fix — and it’s far simpler than most people expect.
In-Office Treatment at Balance Foot & Ankle
When conservative care isn’t enough, Dr. Tom Biernacki and the team at Balance Foot & Ankle offer advanced, same-day options — including Ingrown Toenail Treatment Michigan at our Howell and Bloomfield Hills clinics.
Same-day appointments available. Call (810) 206-1402 or book online.
Sources
- Bos AMC, van Tilburg MWA, van Sorge AA,”; Klaassen AM. “Randomized clinical trial of surgical technique and local antibiotics for ingrowing toenail.” Br J Surg. 2007;94(3):292-296.
- Felton PM, Weaver TD. “Phenol and alcohol chemical matrixectomy in diabetic versus nondiabetic patients.” J Am Podiatr Med Assoc. 2012;102(4):287-292.
- Karaca N, Dereli T. “Treatment of ingrown toenail with proximal nail matrix excision.” Ann Fam Med. 2012;10(6):556-558.
- Eekhof JAH, Van Wijk B, Knuistingh Neven A, van der Wouden JC. “Interventions for ingrowing toenails.” Cochrane Database Syst Rev. 2012;(4):CD001541.
Ready to Fix Your Ingrown Toenail for Good?
15-minute in-office procedure · 95%+ success rate · Howell & Bloomfield Hills, MI
⭐ 4.9 Stars · 1,123 Reviews · 3,000+ Surgeries
Need Permanent Ingrown Toenail Relief?
Permanent ingrown toenail removal surgery eliminates the problem at the root. Our podiatrists perform this quick, in-office procedure with minimal downtime and excellent long-term results.
📞 Or call us directly: (810) 206-1402
Clinical References
- Eekhof JA, et al. Interventions for ingrowing toenails. Cochrane Database of Systematic Reviews. 2012;(4):CD001541.
- Bos AM, et al. Partial matrix excision or orthonyxia for ingrowing toenails. Journal of the American Podiatric Medical Association. 2007;97(5):369-375.
- Heidelbaugh JJ, Lee H. Management of the ingrown toenail. American Family Physician. 2009;79(4):303-308.
Insurance Accepted
BCBS · Medicare · Aetna · Cigna · United Healthcare · HAP · Priority Health · Humana · View All →
👟 Dr. Tom Also Recommends
Podiatrist Recommended Shoes 2026: Dr. Tom’s Top Picks for Every Condition
The right footwear can make or break your recovery. Dr. Tom’s complete guide to the best shoes for plantar fasciitis, flat feet, neuropathy, bunions & more — with clinical picks for every foot type.
See Dr. Tom’s Top Shoe Picks →Howell Office
3980 E Grand River Ave, Suite 140
Howell, MI 48843
Get Directions →
Bloomfield Hills Office
43700 Woodward Ave, Suite 207
Bloomfield Hills, MI 48302
Get Directions →
Your Board-Certified Podiatrists
Ready to Get Back on Your Feet?
Same-week appointments available at both locations.
Book Your AppointmentDr. Tom’s Top 3 — The Premium Foot Pain Stack (2026)
If you only buy three things for foot pain, get these. PowerStep + CURREX orthotics correct the underlying foot mechanics, and Dr. Hoy’s pain gel delivers fast topical relief. This is the exact stack Dr. Tom Biernacki, DPM gives his Michigan podiatry patients on visit one — over 10,000 patients have used this exact combination.
Dr. Tom Biernacki, DPM is a board-certified podiatrist + Amazon Associate. Picks shown are products he prescribes to patients at Balance Foot & Ankle Specialists. We earn a commission on qualifying purchases at no extra cost to you. All products independently tested + reviewed for 30+ days minimum. Last verified: April 28, 2026.
PowerStep Pinnacle MaxxDr. Tom’s #1 Brand
Dr. Tom’s most-prescribed OTC orthotic. Lateral wedge corrects overpronation that causes 90% of foot pain. Deep heel cradle stabilizes the ankle. Built by podiatrists, used by patients worldwide.
- Lateral wedge corrects pronation
- Deep heel cradle stabilizes ankle
- Dual-density EVA — comfort + support
- Trim-to-fit any shoe
- Used by 10,000+ podiatrists
- Trim-to-size required
- 5-7 day break-in for some
CURREX RunProDr. Tom’s #1 Brand
3 arch heights for custom fit (Low/Med/High). Carbon-reinforced heel + dynamic forefoot — the closest OTC orthotic to a $500 custom orthotic. Engineered in Germany.
- 3 arch heights for custom fit
- Carbon-reinforced heel cup
- Dynamic forefoot zone
- Premium German engineering
- Sport-specific support
- Pricier than PowerStep
- 7-10 day break-in
Dr. Hoy’s Natural Pain Relief GelDr. Tom’s #1 Brand
Menthol-based natural pain relief — Dr. Tom’s #1 brand for fast relief without greasy residue. Safe for diabetics + daily use. Cleaner formula than Voltaren or Biofreeze.
- Menthol-based natural formula
- No greasy residue
- Safe for diabetics
- Fast cooling relief — 5-10 minutes
- Cleaner ingredient list than Biofreeze
- Pricier than Biofreeze
- Strong menthol scent at first
Dr. Tom Biernacki, DPM is a double board-certified podiatrist and foot & ankle surgeon at Balance Foot & Ankle Specialists in Southeast Michigan. With over a decade of clinical experience, he specializes in heel pain, bunions, diabetic foot care, sports injuries, and minimally invasive surgery. Dr. Biernacki is a member of the APMA and ACFAS, and his patient education content on MichiganFootDoctors.com and YouTube has reached over one million views.
- Plantar Fasciitis: Diagnosis and Conservative Management (PubMed)
- Plantar Fasciitis (APMA)
- Diagnosis and Treatment of Plantar Fasciitis (PubMed / AAFP)
- Heel Pain (APMA)
Recommended Products from Dr. Tom